 Case Report
Case Report
A Rare Association of Marfan Syndrome with Papillary Carcinoma of Thyroid
Lendoye W*, Moujrid S, Radhi H, Abada R and Mahtar M
ENT Head and Neck Surgery department, Ibn Rochd University Hospital, Morocco
Dr. Wilfrid Lendoye, ENT Head and Neck Surgery department, Ibn Rochd University Hospital17, Rue Sebta, Quartier des hopitaux, Casablanca, Morocco.
Received Date:March 07, 2022; Published Date: June 07, 2022
Abstract
Marfan syndrome is a common genetic disorder involving a defciency of the structural extracellular matrix component fbrillin-1 and overactivation of the transforming growth factor-β signalling pathway. The growth factor-β signalling pathway also actively participates in malignant transformation. The aim of this work is to present a rare association observed in a 18-years-old patient treated in the ENT tertiary referral center of Casablanca, Morocco for a voluminous goiter and Marfan syndrome.
Keywords: papillary carcinoma; Marfan syndrome; Thyroid; Growth factor-β
Introduction
Marfan syndrome is a fairly common genetic disorder that affects the connective tissue in different parts of the body, with an incidence of approximately 1 in 5,000 worldwide [1,2]. The connective tissue holds the body parts together and provides its structures with strength and flexibility [1]. Marfan syndrome is the manifestation of the body’s failure to control the production of a protein known as fibrillin-1 as a result of the genetic mutation. The deficiency in fibrillin-1 causes an overproduction of the transforming growth factor-β (TGF)-β [3]. Studies have revealed that (TGF)-β perturbations promote tumor emergence and are synonymous with underling inflammatory diseases [4]. People with Marfan syndrome typically exhibit skeletal manifestations, they are usually tall and slender, have elongated arms, legs and fingers, a long and narrow face, crowded teeth [1,5]. It can also compromise the normal development of the ribs, which can result in protruding or sunken breastbone. Marfan syndrome complications may range from mild to severe to life threatening if left without proper treatment [1]. It most commonly affects the heart, eyes, blood vessels and skeleton. The condition is often associated with degenerative non-inflammatory structural cardiovascular diseases, including aortic root dilatation and aortic dissection.
Case Report
We present a case of an 18-years-old man, he was admitted to our service of otolaryngology with complaints of a mediansided neck swelling that started a year ago. The swelling gradually increased in size over time, without any signs or symptoms of dyspnea, dysphagia, or dysphonia. He didn’t report that he had a dysthyroid symptom. Most notable is that our patient hadn’t any medical history. On his admission clinical examination showed that he had Marfan syndrome symptoms. He has tall and slender build, disproportionately long arms, legs and fingers and a breastbone that dips inward. He presented a large, hard, painless to the touch, and movable thyroid goiter, with a major axis of 4 cm. B-mode ultrasound examination revealed a bulky goiter, pseudo-nodular, sinking in the chest. CT-scan showed a voluminous goiter, sinking in chest, reaching in contact with aortic arch. Heart Doppler-ultrasound revealed no anomaly. Thyroid function tests were normal. The patient underwent total thyroidectomy and suspect adenopathy of central territory was also extracted. Final Histological examination showed a papillary carcinoma measuring 17 cm, with extra thyroid extensions, associated to carcinomatous nodule. The patient was addressed to nuclear medicine where he received iratherapy as complement of treatment. His CT-scan revealed a large thyroid goiter (Figure 1-5).

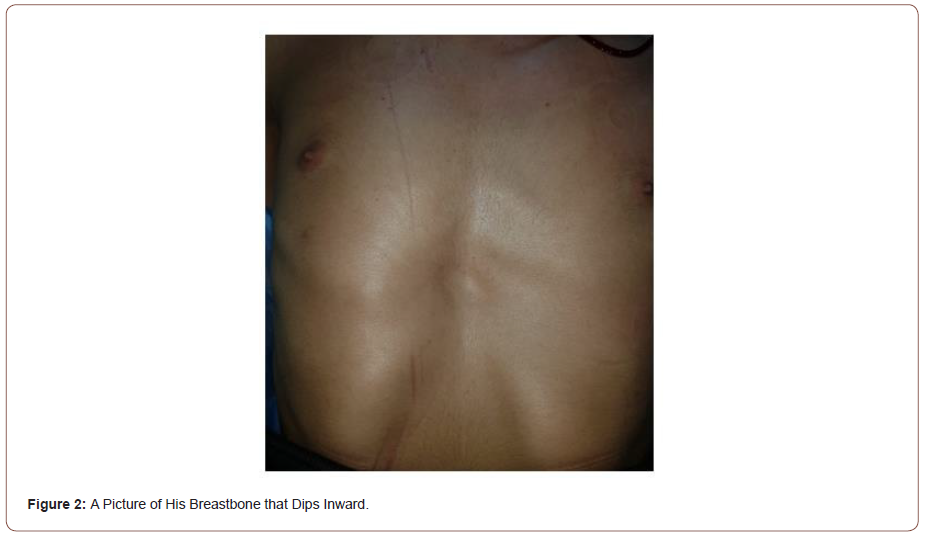
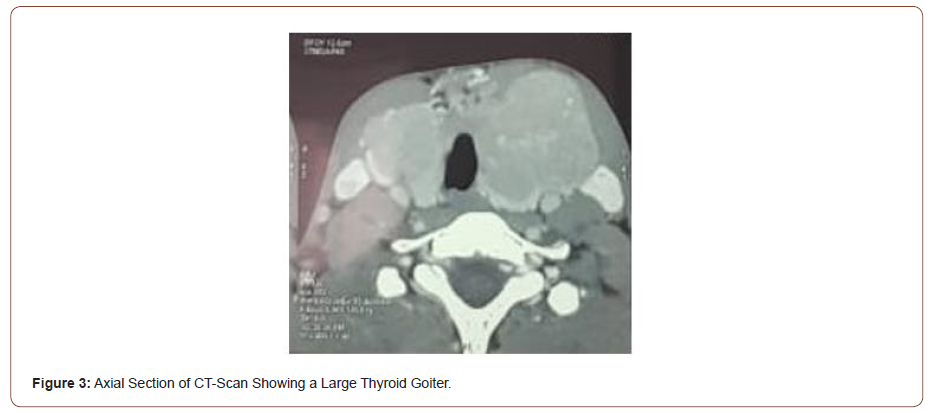
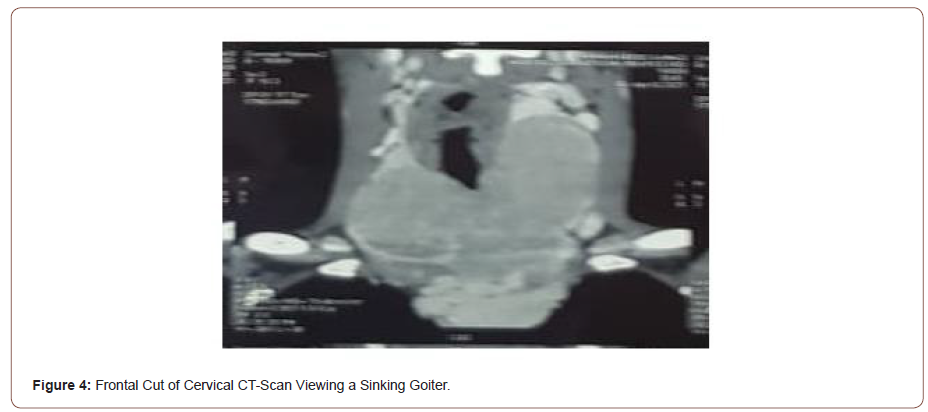
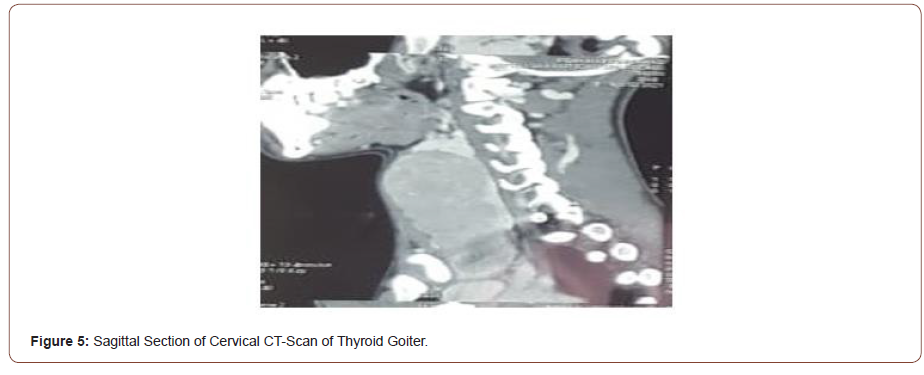
Discussion
A nationwide and population-based study conducted in Taiwan and published in 2017, has demonstrated for the first time that Marfan syndrome is associated with the development of certain malignancies. Several case reports throughout the literature have also suggested that MFS patients might be at a higher risk of developing various types of malignancies including thyroid cancer, esophageal cancer, angiosarcoma and testicular cancer. The study also reports a higher incidence rate of head and neck malignant tumors in individuals with MFS. Fibrillins, especially Fibrillin-1 (FBN-1) and fibrillin-2 (FBN-1), play a vital role by contributing to the formation of the connective tissue and by sequestering and controlling transforming growth factor β (TGFβ) and maintaining it in its inactive and latent form [3,6]. Genetic mutations in FBN- 1 result in MFS and seem to be involved in cancer emergence and development [3,6].
Research has shown that an overproduction of TGF-β, resulting from FBN-1 deficiency, leads to larger aortic root diameters and faster aortic root growth. More importantly, high levels of TGF-β actively contribute to malignant transformation and progression as it was associated with various solid malignancies, including head and neck, bladder and prostate [3]. When TGF-β primary function is compromised it loses its ability to inhibit epithelial cell proliferation and starts contributing to tumor promoting effects, increasing tumor invasiveness and disseminating malignant cells. Another strong indicator of the link between Marfan syndrome and cancer is that patients with MFS developed malignancies at a much younger age than those without MFS [3,7,8].
Conclusion
Individuals with Marfan syndrome are obviously at a higher risk of developing various malignancies. Thus, these patients may require additional monitoring and screening tests for cancer.
Acknowledgement
None.
Conflict of Interest
No conflict of interest.
References
- https://medlineplus.gov/genetics/
- https://my.clevelandclinic.org/search
- Chin-Wang Hsu, Jen-Chun Wang, Wen-I Liao, Wu-Chien Chien, Chi-Hsiang Chung, et al. (2017) Association between malignancies and Marfan syndrome: a population-based. nested case–control study in Taiwan BMJ Open7: e017243.
- Eduard Batlle, Joan Massagué (2019) Transforming Growth Factor-β Signaling in Immunity and Cancer Immunity. 50(4): 924-940.
- Daniel A Winer, Shawn Winer, Lorne Rotstein, Sylvia L Asa, Ozgur Mete (2012) Villous Papillary Thyroid Carcinoma: a Variant Associated with Marfan Syndrome. Endocr Pathol 23(4):254-259.
- Francesco Ramirez, Sakai LY (2010) Biogenesis and function of fibrillin assemblies. Cell Tissue Res 339(1): 71-82.
- https://teach.genetics.utah.edu/
- José Manuel Cameselle-Teijeiro, Catarina Eloy, Manuel Sobrinho-Simões (2020) Pitfalls in Challenging Thyroid Tumors: Emphasis on Differential Diagnosis and Ancillary Biomarkers. Endocr Pathol 31(3): 197-217.
-
Lendoye W, Moujrid S, Radhi H, Abada R, Mahtar M. A Rare Association of Marfan Syndrome with Papillary Carcinoma of Thyroid. Open J Pathol Toxicol Res. 1(2): 2021. OJPTR.MS.ID.000507.
-
Voluminous goiter, Dysthyroid symptom, Neck swelling, Aortic dissection, Cardiovascular diseases, Fibrillin-1
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






