 Review Article
Review Article
Functional Outcomes in Endoscopic Endonasal Surgery of the Skull Base, A rising challenge
David Bedoya1, Joaquim Enseñat2, Isam Alobid1,3 and Cristobal Langdon1,3*
1Department of Otorhinolaryngology, University of Barcelona, Spain
2Department of Neurosurgery, University of Barcelona, Spain
3Department of Clinical and Experimental Respiratory Immunology, University Barcelona, Spain
Cristobal Langdon, Department of Otorhinolaryngology, University of Barcelona, Spain.
Received Date: June 05, 2019; Published Date: July 09, 2019
Abstract
Since the introduction of endonasal endoscopic skull base surgery in the management of skull base neoplasms the exclusive purpose has been to increase survival rates. Recently, given the improved of the survival rates, more attention has been focused on other aspects such as nasal symptoms and quality of life. The purpose of this review is to assess the current evidence of functional outcomes after endoscopic skull base surgery.
Keywords: Endoscopic surgery, Skull base, Quality of life, Nasal symptoms
Introduction
Extended endonasal endoscopic approaches (EEEA) for skull base lesions have been increasing over the last decade. Determinants for this development are the enhanced understanding of the endoscopic anatomy, improvement of imaging systems and specific instruments, and the use of vascularized flaps for reconstruction [1]. This EEEA can cause postoperative morbidity related to the reconstruction, like crusting and posterior rhinorrhea, especially in those cases requiring an endonasal flap [2,3]. The healing process start the first week with a reepithelization by stratified epithelium, then hair cells appear in the third week and complete recovery of the sinus epithelium occurs within 6-8 weeks [4]. Given this, [5] conclude that one must wait at least three months to assess the clinical and postoperative symptoms. Regarding quality of life (QOL) after EEEA evidence have shown that the morbidity is related to the extension of the approach. [6] reported a negative impact in QOL after the use of nasoseptal flap which is commonly associated to extended approaches. The latter was mainly due to an increased tendency to headaches and reduced smell; however, recovery occurs over time especially in those patients with secreting pituitary tumors.
Since the use of endoscopic skull base surgery, there have been great efforts to develop specific QOL questionnaires for EEEA and pituitary surgery (Table 1) Until now, the following tests have been applied in English literature; Quality of Life-Assessment of Growth Hormone Deficiency in Adults [7], Hypopituitarism Quality of Life Satisfaction (QLS-H) [8], Previous Skull Base Quality of Life (ASB-QOL) [9], Hormone Deficiency-Dependent Quality of Life ( HDQOL) [10], Acromegaly Quality of Life (ACROQOL) [11], Pituitary Adenoma Quality of Life (PA-QOL) [12], Cushing Quality of Life [13], Addison Quality of Life (AddiQOL) [14], or ASK nasal inventory [15]. Handicaps for these tests are that they do not include specific areas about quality of life and cancer, visual defects, hormonal deficiency or sinonasal symptoms. Here, we will discuss the impact of EEEA regarding the following topics:
1. Sinonasal symptoms.
2. Mucociliary clearance.
3. Quality of life.
4. Imaging findings.
Table 1: Publications about Quality of Life and Nasal Symptoms in Surgery ESBC.
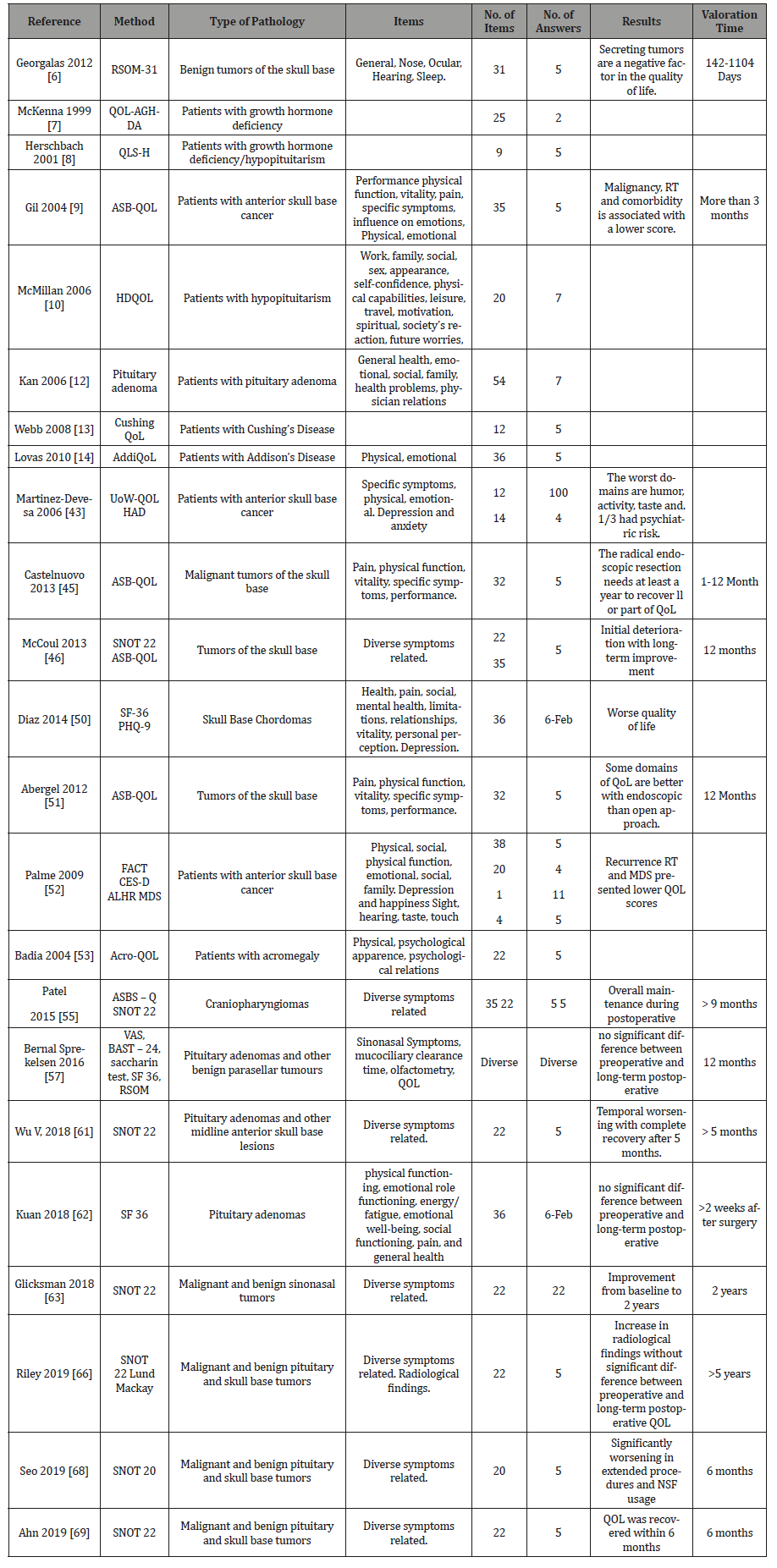
Sinonasal symptoms
In the last decade, endoscopic skull base surgery has had a massive development in terms of surgical experience and technological advancement. Nowadays is it possible to address larger and more complex tumors, as so, patients suffer large anatomical and functional changes of the sinonasal cavity postoperatively. It is in the first postoperative period (2-4 weeks) when nasal symptoms are more evident, usually patients refer thick anterior and posterior rhinorrhea, nasal congestion, facial pain and headaches [16]. Currently nasal symptoms are measured according to the visual analogue scale and/or by different questionnaires such us the Sinonasal Outcome Test 22 (SNOT-22), Rhinosinusitis outcome measure (RSOM-31) and the Rhinosinusitis Disability Index (ISDN).
In one of the first studies about posterior nasal symptoms in skull base surgery, [3] observed that the most frequent finding were nasal crusts (98%) one month postoperative and at least half of the patients continue with nasal crusts for 3 months postsurgery. The time of disappearance of the crusts was related to the complexity of the surgery but not to the reconstruction of the defect [2] reported that in the postoperative period 28% of patients undergoing transsphenoidal and 64% undergoing extended surgery had posterior rhinorrhea. Interestingly [17] compared the nasal symptoms in patients undergoing endoscopic versus open surgery, they observed that the endoscopic surgery group had a lower score of nasal symptoms compared to the open approaches [18,19] showed that the SNOT-22 total score and the nasal symptoms score increased moderately in the immediate postoperative period but subsequently returned to their preoperative values. The same was reported by [16] who found that nasal symptoms significantly improved over time, although posterior rhinorrhea persisted during the first year after surgery.
Normal sense of smell requires the integrity of the olfactory epithelium for proper functioning. Usually in cases of lateral or anterior skull base surgery (without affecting cribriform plate) is possible to preserve the olfactory mucosa. In cases where the cribriform plate (with or without olfactory bulb resection) must be resected or an EEEA is performed, the integrity of the olfactory mucosa is affected almost entirely with the subsequent olfactory dysfunction for the patient. To almost all the studies regarding olfactory dysfunction after EEEA are made with olfactometry test [20]. used the olfactometry test of the University of Pennsylvania (UPSIT), before and after endoscopic endonasal hypophysectomy in 45 patients. They observed that patients had a lower ability to smell a month after surgery but after three months there were no significant differences compare to preoperative scores [21] did a prospective study with 36 patients and found no significant differences between pre- and post-operative SNOT 20 scores and visual analogue scale scores for nasal obstruction, actually they showed a significant improvement of symptoms [2]. studied olfaction in 50 patients (36 with transsphenoidal and 14 with extended surgery), they observed that patients undergoing extended approach with nasoseptal flap reconstruction had higher rate of olfactory dysfunction at 3 months compared to patients undergoing transesphenoidal surgery. The same group reported in a prospective study [22] that the smell impairment and the increased posterior nasal discharge is present up to twelve months after surgery. They also reported that the mucociliary clearance time was prolonged after EEEA [23] assessed the longterm olfactory outcomes between cold knife upper septal incision technique compared to monopolar cautery in nasoseptal flap for skull base reconstruction. They found no significant difference in short-term or long-term, assessed by the UPSIT scores 1 year after transnasal skull-base approaches [24], found in a systematic review that endoscopic approach appears to be superior regarding preservation of olfactory outcome when compared with the microscopic approach, especially when the endoscopic approach was performed without harvesting of the nasoseptal flap. Another nasal complaint has been studied [25] in 41 patients undergoing skull base surgery found nasal fossa synechia in 19.5%, internal nasal valve failure in 14.6% and complaints of worsening of the sense of smell in 39%.
Mucociliary clearance
Disruption of the mucociliary clearance (MCC), an important mechanism of the innate immunity of the upper and lower airways, predisposes to airway diseases [26].
The MCC could be altered for two reasons:
1. Misfunction in the movements of the cilia.
2. Dehydration of the mucus, which leads to increased viscosity and therefore the ciliary clearance becomes ineffective.
In the first group we have primary (genetic) and secondary (infection or inflammation) ciliary dyskinesia, while in the second group we found cystic fibrosis, asthma among others. Many factors influence the MCC, some can be derived from the environment, like temperature and humidity, while others are specific to the patient, e.g, trauma, smoking, viral infections, chronic sinusitis, allergic rhinitis, deviated septum, sinus surgery, and cystic fibrosis and asma [27]. At present, there is no gold standard test for MCC analysis, although there are a variety of investigational methods and techniques available.
The most commonly used method is the saccharine test [28]. Although it depends on a subjective factor, it gives a well-defined time of MCC, since subjects clearly described the perception of sweet taste. There are some who criticize the use of saccharin particles as a measure of mucosal transport [29,30] but there are studies that show a good correlation between the time of MCC measured by saccharine test and ciliary beat frequency determined by photometry [31,32] as well as, a significant negative correlation with the transport speed measured by resin particles labeled with 99Tc [33]. The saccharine test is performed at ambient temperature, where the patient is requested not to perform forced inspiration. A 1 mm saccharin particle is applied in the 1 cm of the anterior portion of the inferior turbinate. Patients are asked to report any change in taste without advising them that they will receive a sweet flavor. The time required by the patient to perceive sweetness is the defining time of the test.
Few studies have assessed the impact of EEEA in the MCC [2] studied the MCC in patients undergoing EEEA, they found that patients had a prolonged MCC time until three months after surgery. They also showed that the more extended the approached was the MCC time was higher. On the other hand, several studies have evaluated the effect of nasal surgery in MCC [34] showed that the MCC improved in patients who had a septoplasty, with no significant difference between the blocked nasal cavity and the opposite side [35] evaluated MCC by saccharin test in three groups of patients (septoplasty, endoscopic polypectomy and turbinectomy) and observed that patients with preoperative mucociliary dysfunction didn’t improve its function after surgery [36] studied the improvement of MCC in 43 patients undergoing endonasal endoscopic surgery for chronic rhinosinusitis with or without polyposis, they noted that the MCC measured by the saccharin test improved following endoscopic sinus surgery.
Quality of life
QOL is a multidimensional concept that measures the relationship of a series of physical and psychosocial factors. It describes the ability of an individual to make his life and get satisfaction from it. As so, QOL assessments provide a patientreported estimate of well-being and show their degree of comfort and satisfaction [37]. The analysis of QOL is based on the patient’s opinion about different aspects of his life that may have been modified after the treatment. These dimensions or domains include physical activity, psychological state, social interaction and somatic perception [38,39]. The advantages and limitations of endoscopic skull base surgery have been extensively studied [40,41]. Based on the latter results often the surgical success is defined as the balance between of maximal tumor resection and minimal functional impact. In 2013, [42] developed and validated the Anterior Skull Base Nasal Inventory-12 (ASK Nasal-12), a sitespecific nasal morbidity instrument to assess patient-reported outcomes following endonasal skull base surgery [43] designed a multidimensional, disease-specific instrument, the Endoscopic Endonasal Sinus and Skull Base Surgery Questionnaire (EES-Q), they proved the importance of a multidimensional health related QOL assessment in a prospective cohort study with 100 patients showing how inconveniences in social functioning had the greatest negative impact on postoperative health status rating 64.
Few studies have evaluated the organ specific functional impairment and QOL; this is mainly due to the low prevalence of the disease, high variability of localization of the tumors, and the different surgical approaches and reconstruction methods [44] were the first that used a generic questionnaire of QOL to study patients undergoing endoscopic pituitary surgery and showed no difference in QOL when compared with patients who underwent mastoidectomy [45] compared patients with pituitary pathology with the healthy population. They found that patients with acromegaly had impaired physical function while patients with Cushing syndrome showed deterioration in all the evaluated parameters except for one domain. Patients with prolactinoma had mental deterioration, but patients with a non-functioning adenoma presented impairments in the physical and mental spheres [45,46] studied the QOL in patients undergoing pituitary adenoma resection by endonasal endoscopic surgery; they showed that these patients had mild postoperative deterioration on the SF-36 [6] observed that patients with hormone-secreting tumors had greater postsurgical impairment of QOL [2] observed similar results to those previously mentioned; however, they did not find differences between functioning and non-functioning adenomas. Consistent with the latter study, [47] used the Rhinosinusitis Disability Index and observed no differences between preoperative and postoperative scores in patients with or without functioning pituitary pathology [48] found lower QOL in six of eight domains of SF 36 preoperatively but improved to baseline values on the long run after surgery in seven of eight domains [47] used ASBS-Q and SNOT 22 for evaluating the impact of ESBS for craniopharyngiomas resection and shows an overall maintenance of postoperative compared with preoperative QOL, better in patients with grosstotal resection and radiation therapy, and worse in patients with visual or endocrine deficits. Nevertheless, patients with craniopharyngiomas still had worse QOL than those undergoing similar surgery for pituitary macroadenomas.
Patients with extended endonasal approaches are a challenge, since they are usually oncological patients with a significant physical, cognitive, emotional or social deterioration [49]. It is possible that these findings correlate more closely with adjuvant treatments and oncological disease than the surgery itself. A metaanalysis confirmed that patients undergoing oncologic disease have a lower QOL compared to patients with benign tumors independent of the type of surgical technique [42,50]. Assessed the QOL in patients with sinonasal carcinomas after surgery and observed that they had a significant deterioration in the domains of anxiety, physical activity and emotional state [51] studied a cohort of 153 patients who received adjunctive therapy and found that they had a worsening of their QOL which was more related to the adjuvant therapy. Regarding the last point, [2] compared the impact of nasal symptoms and QOL using the sinonasal symptoms test RSOM-31 and QOL test SF-36. They found that patients undergoing extended endoscopic skull base surgery showed higher sinonasal symptoms that patients undergoing pituitary surgery, and both had mild impairment QOL assessed by the SF-36 questionnaire [52] showed a temporary worsening during the first year of postoperative ESBS, after which QOL recovers and returns almost to normal [53] in a single-center prospective cohort study of patients with endoscopic transsphenoidal skull base surgery conclude that sinonasal quality of life worsened after 1 month postoperatively but returned to preoperative levels after the second month and remained stable after 5 months of follow up [54] also reported a recovery of QOL after 6 months of ESBS [55] in a prospective cohort study with 145 patients with both malignant and benign sinonasal tumors, found a statistically significant improvement in SNOT-22 score from baseline to 2 years [56] observed that extended procedures and NSF usage was significantly associated with poor outcomes.
Radiological findings
Postoperative imaging evaluation is one of the keystones studies for monitoring patients undergoing skull base pathology. In order to detect residual lesions, recurrence and/or complications, the use of postoperative MRI is one of the fundamental pillars for following patients undergoing skull base pathology.
Correct interpretation of radiological findings implies to know how the healing process occurs in the sinonasal cavity, especially the radiological differentiation of the nasoseptal flap healing process and the differentiation between inflamed mucosa and mucosa infiltrated by tumor. In general, MRI distinguishes normal and inflamed soft tissues, and differentiates between these tissues and tumor. The latter is primarily based on the fact that inflamed mucosa is associated with increased submucosal oedema and increased mucus secretions [57] used MRI to evaluate the viability of the nasoseptal flap in the postoperative setting, they found that flap is healthy when is hypo intense on both T1 and T2. Regarding inflammatory tissue differentiation from tumor recurrence [58] observed that the inflamed sinus mucosa is characterized by hypo intensity on T1 and hyper intensity on T2. In contrast, the tumor tissue is characterized by hypo intensity on both T1 and T2, but to assess tumor tissue/recurrence, is better to assess images on T2 sequence [59,60], found Increased sinus opacification between the mean overall pre and [61-63]postoperative SNOT-22 scores after 67.4 months. Regarding other imaging tests such as PET-CT, one must keep in mind that inflamed cells also show increased glycolytic activity [64-67], consequently inflamed areas cannot be distinguishing with tumor tissue.
Conclusion
The endoscopic endonasal skull base surgery has evolved dramatically, emerging as the treatments of choice in addressing skull base pathology. While the main objective is tumor resection, there is a growing interest on studying the functional outcome in relation to the in QOL and nasal symptoms. Unfortunately, there are still few studies to perform a standardization of methods that measure functional outcomes after endoscopic skull base surgery. In a future, longitudinal studies are needed to standardize the measurement instruments of quality of life, nasal symptoms and general symptoms suffered by these patients after surgery.
Acknowledgements
None.
Conflict of interest
No conflict of interest.
References
- Kassam A, Mintz A, Gardner P, Horowitz M, Carrau R, et al. (2006) The expanded endonasal approach for an endoscopic transnasal clipping and aneurysmorrhaphy of a large vertebral artery aneurysm: technical case report. Neurosurgery 59: 162-165.
- Alobid I, Ensenat J, Marino Sanchez F, De Notaris M, Centellas S, et al. (2013) Impairment of olfaction and mucociliary clearance after expanded endonasal approach using vascularized septal flap reconstruction for skull base tumors. Neurosurgery 72(4): 540-546.
- De Almeida JR, Snyderman CH, Gardner PA, Carrau RL, Vescan AD (2011) Nasal morbidity following endoscopic skull base surgery: a prospective cohort study. Head Neck 33(4): 547-551.
- Beule AG (2010) Physiology and pathophysiology of respiratory mucosa of the nose and the paranasal sinuses. GMS Curr Top Otorhinolaryngol Head Neck Surg 89: S15-34.
- Ginzel A, Illum P (1980) Nasal mucoliliary clearance in patients with septal deviation. Rhinology 18(4): 177-181.
- Georgalas C, Badloe R, van Furth W (2012) Quality of life in extended endonasal approaches for skull base tumours. Rhinology 50(3): 255- 261.
- Mc Kenna SP, Doward LC, Alonso J (1999) The QoL-AGHDA: an instrument for the assessment of quality of life in adults with growth hormone deficiency. Qual Life Res 8(4): 373-383.
- Herschbach P, Henrich G, Strasburger CJ (2001) Development and psychometric properties of a disease-specific quality of life questionnaire for adult patients with growth hormone deficiency. Eur J Endocrinol 145: 255-265.
- Gil Z, Abergel A, Spektor S (2004) Development of a cancer-specific anterior skull base quality of life questionnaire. J Neurosurg 100: 813- 819.
- Mc Millan CV, Bradley C, Gibney J (2006) Preliminary development of the new individualized HD QoL questionnaire measuring quality of life in adult hypopituitarism. J Eval Clin Pract 12(5): 501-514.
- Webb SM, Badia X, Surinach NL (2006) Validity and clinical applicability of the acromegaly quality of life questionnaire, AcroQol: a 6-month prospective study. Eur J Endocrinol 155(2): 269-77.
- Kan P, Cusimano M (2006) Validation of a quality-of-life questionnaire for patients with pituitary adenoma. Can J Neurol Sci 33(1): 80-85.
- Webb SM, Badia X, Barahona MJ (2008) Evaluation of health-related quality of life in patients with Cushing’s syndrome with a new questionnaire. Eur J Endocrinol 158: 623-630.
- Lovas K, Curran S, Oksnes M (2010) Development of a disease-specific quality of life questionnaire in Addison’s disease. J Clin Endocrinol Metab 95(2): 545-551.
- Little AS, Jahnke H, Nakaji P (2012) The anterior skull base nasal inventory (ASK nasal inventory): a clinical tool for evaluating rhinological outcomes after endonasal surgery for pituitary and cranial base lesions. Pituitary 15(4):513-517.
- Balaker A, Bergsneider M, Martin N, Wang M (2010) Evolution of sinonasal symptoms following endoscopic anterior skull base surgery. Skull Base 4: 254-251.
- Graham SM, Iseli TA, Karnell LH (2009) Endoscopic approach for pituitary surgery improves rhinologic outcomes. Ann Otol Rhinol Laryngol 118(9): 630-635.
- Pant H, Bhatki AM, Snyderman CH (2010) Quality of life following endonasal skull base surgery. Skull Base20(1): 35-40.
- Mc Coul ED, Anand VK, Schwartz TH (2012) Improvements in sitespecific quality of life 6 months after endoscopic anterior skull base surgery: a prospective study. J Neurosurg 117(3): 498-506.
- Hart CK, Theodosopoulos PV, Zimmer LA (2010) Olfactory changes after endoscopic pituitary tumor resection. Otolaryngol Head Neck Surg 142(1): 95-97.
- Hanson M, Patel PM, Betz C, Olson S, Panizza B, et al. (2015) Sinonasal outcomes following endoscopic anterior skull base surgery with nasoseptal flap reconstruction: a prospective study. J Laryngol Otol 3: S41-46
- Rioja E, Bernal Sprekelsen M, Enriquez K, Enseñat J, Valero R, de Notaris M (2016) Long-term outcomes of endoscopic endonasal approach for skull base surgery: a prospective study. Eur Arch Otorhinolaryngol 273(7): 1809-1817.
- Puccinelli CL, Yin LX, O Brien EK, Van Gompel JJ, Choby GW, et al. (2019) Long-term olfaction outcomes in transnasal endoscopic skull-base surgery: a prospective cohort study comparing electrocautery and cold knife upper septal limb incision techniques. Int Forum Allergy Rhinol 9(5): 493-500.
- Majovsky M, Astl J, Kovar D, Masopust V, Benes V, et al. (2019) Olfactory function in patients after transsphenoidal surgery for pituitary adenomas-a short review. Neurosurg Rev 42(2): 395-401.
- Dolci RLL, Miyake MM, Tateno DA, Cançado NA, Campos CAC, et al. (2017) Postoperative otorhinolaryngologic complications intransnasal endoscopic surgery to access the skull base. Braz J Otorhinolaryngol 83(3): 349-355.
- Guilemany JM, Mullol J, Picado C (2006) Relation between rhinosinusitis and bronchiectasis. Arch Bronconeumol 42(3): 135-140.
- Karaman M, Tek A (2009) Deleterious effect of smoking and nasal septal deviation on mucociliary clearance and improvement after septoplasty. Am J Rhinol Allergy 23(1): 2-7.
- Andersen IB, Camner P, Jensen Pl, Philipson K, Proctor DF (1974) A comparison of nasal and tracheobronchial clearance. Arch Environ Health 29: 290-293.
- Armengot Carceller M, Carda Batalla C, Escribano A, Juan Samper G (2005) Study of mucociliary transport and nasal cytosolic ultrastructure in patients with Kartagener syndrome. Arch Bronconeumol 41: 11-15.
- Passali D, Bellusi L, Blanchini M, De Seta E (1984) Experiences in the determination of nasal mucociliary transport time. Acta Otolaryngol 97: 319-323.
- Ducheteau GS, Gramans K, Ludera J, Merkus S (1985) Correlations between nasal ciliary beat frequency and mucous transport rate in volunteers. Laryngoscope 95: 854-859.
- Stanley P, Mac Williams L, Greenstone M, Mackay I, Cole P (1984) Efficacy of saccharin test for screening to detect abnormal mucociliary clearance. Br J Dis Chest 78: 62-65.
- Puchelle E, Aug F, Pham QT, Bertrand A (1981) Comparison of three methods for measuring nasal mucociliary clearance in man. Acta Otolaryngol 91:297-303.
- David B (1987) The nasal septum. In: Alan GK, (edt.), Scott-Brown’s Otolaryngology’de. Oxford: Butterworth-Heinemann, USA, pp: 157-158.
- Shone GR, Yardley MP, Knight LC (1990) Mucociliary function in the early weeks after nasal surgery. Rhinology 28(4): 265-268.
- Singh M, Chandra M, Gupta SC, Sharma D (2010) Role of measurement of nasal mucociliary clearance by saccharine test as a yard stick of success of functional endoscopic sinus surgery. Indian J Otolaryngol Head Neck Surg 62(3): 289-295.
- Morton RP (1995) Life satisfaction in patients with head and neck cancer. Clin Otolaryngol 20: 499-503.
- Ware JE (1984) Conceptualizing disease impact and treatment outcomes. Cancer 53: 2316-2323.
- Schipper H (1990) Quality of life: principles of the clinical paradigm. J Psychosoc Oncol 8: 171-184.
- Eloy JA, Vivero RJ, Hoang K, Civantos FJ, Weed DT, et al. (2009) Comparison of transnasal endoscopic and open craniofacial resection for malignant tumors of the anterior skull base. Laryngoscope 119: 834- 840.
- Hanna E, De Monte F, Ibrahim S, Roberts D, Levine N, et al. (2009) Endoscopic resection of sinonasal cancers with and without craniotomy: oncologic results. Arch Otolaryngol Head Neck Surg 135: 1219-1224.
- Martinez Devesa P, Barnes ML, Alcock CJ, Kerr RS, Milford CA (2006) Evaluation of quality of life and psychiatric morbidity in patients with malignant tumours of the skull base. J Laryngol Otol 120(12): 1049- 1054.
- Ten Dam E, Feijen RA, van den Berge MJC, Hoving EW, Kuijlen JM, et al. (2017) Development of the Endoscopic Endonasal Sinus and Skull Base Surgery Questionnaire. Int Forum Allergy Rhinol 7(11): 1076-1084.
- Page RC, Hammersley MS, Burke CW (1997) An account of the quality of life of patients after treatment for non-functioning pituitary tumours. Clin Endocrinol (Oxf) 46(4): 401-406.
- Johnson MD, Woodburn CJ, Vance ML (2003) Quality of life in patients with pituitary adenoma. Pituitary 63: 81-87.
- Karabatsou K, O Kelly C, Ganna A (2008) Outcomes and quality of life assessment in patients undergoing endoscopic surgery for pituitary adenomas. Br J Neurosurg 22(5): 630-635.
- Suberman TA, Zanation AM, Ewend MG (2011) Sinonasal quality-of-life before and after endoscopic, endonasal, minimally invasive pituitary surgery. Int Forum Allergy Rhinol 1(3): 161-166.
- Kuan EC, Yoo F, Chyu J, Oh A, Bergsneider M, Wang MB (2018) Quality of Life before and after Endoscopic Pituitary Surgery as Measured by the Short-Form-36. J Neurol Surg B Skull Base 79(3): 314-318.
- Hanh CA, Dunn RH, Logue PE, King JH, Edwards CL, Halperin EC (2003) Prospective study of neuropsychologic testing and quality-of-life assessment of adults with primary malignant brain tumors. Int J Radiat Oncol Biol Phys 55(4): 992-999.
- Amit M, Abergel A, Fliss DM, Gil Z (2012) The clinical importance of quality-of-life scores in patients with skull base tumors: a meta-analysis and review of the literature. Curr Oncol Rep 14: 175-181.
- Castelnuovo P, Lepera D, Turri Zanoni M, Battaglia P, Bolzoni Villaret A, et al. (2013) Quality of life following endoscopic endonasal resection of anterior skull base cancers. J Neurosurg 119: 1401-1409.
- Mc Coul ED, Anand VK, Bedrosian JC, Schwartz TH (2012) Endoscopic skull base surgery and its impact on sinonasal-related quality of life. Int Forum Allergy Rhinol 2(2): 174-181.
- Wu V, Cusimano MD, Lee JM (2018) Extent of surgery in endoscopic transsphenoidal skull base approaches and the effects on sinonasal morbidity. Am J Rhinol Allergy 32(1): 52-56.
- Ahn JC, Cho SW, Kim DK, Han DH, Kim DY, et al. (2019) Recovery period of sinonasal quality of life and its associated factors after endoscopic endonasal approach for anterior skull base tumors. Acta Otolaryngol 139(5): 461-466.
- Glicksman JT, Parasher AK, Brooks SG, Workman AD, Lambert JL, et al. (2018) Sinonasal quality of life after endoscopic resection of malignant sinonasal and skull base tumors. Laryngoscope 128(4): 789-793.
- Seo MY, Nam DH, Kong DS, Lee JJ, Ryu G, et al. (2019) Quality of life after extended versus transsellar endoscopic skull base surgery from 767 patients. Laryngoscope 129(6): 1318-1324.
- Kang MD, Escott E, Thomas AJ, Carrau RL, Snyderman CH, Kassam AB, Rothfus W (2009) The MR imaging appearance of the vascular pedicle nasoseptal flap. AJNR Am J Neuroradiol 30(4):781-786.
- Som PM, Dillon WP, Curtin HD, Fullerton GD, Lidov M (1990) Hypointense paranasal sinus foci. Differential diagnosis with MR imaging and relation to CT findings. Radiology 176: 777-781.
- Loevner LA, Sonners AI (2004) Imaging of neoplasms of the paranasal sinuses. Neuroimaging Clin N Am 14: 625-646.
- Riley CA, Tabaee A, Conley L, Amine M, Soneru CP, Anand VK, Schwartz TH (2019) Long-term sinonasal outcomes after endoscopic skull base surgery with nasoseptal flap reconstruction. Laryngoscope 129(5): 1035-1040.
- Rotenberg BW, Saunders S, Duggal N (2011) Olfactory outcomes after endoscopic transsphenoidal pituitary surgery. Laryngoscope 121(8): 1611-1613.
- Diaz RJ, Maggacis N, Zhang S, Cusimano MD (2014) Determinants of quality of life in patients with skull base chordoma. J Neurosurg 120(2): 528-537.
- Badia X, Webb SM, Prieto L (2004) Acromegaly quality of life questionnaire (Acro-QOL). Health Qual Life Outcomes p: 2-13.
- Little AS, Kelly D, Milligan J, Griffiths C, Rosseau G, et al. (2013) Prospective validation of a patient-reported nasal quality-of-life tool for endonasal skull base surgery: The Anterior Skull Base Nasal Inventory-12. J Neurosurg 119(4): 1068-1074.
- Patel KS, Raza SM, Mc Coul ED, Patrona A, Greenfield JP, et al. (2015) Long-term quality of life after endonasal endoscopic resection of adult craniopharyngiomas. J Neurosurg 123(3): 571-580.
- Jones SH, Iannone AF, Patel KS, Anchouche K, Raza SM, et al. (2016) The Impact of Age on Long-Term Quality of Life After Endonasal Endoscopic Resection of Skull Base Meningiomas. Neurosurgery 79(5): 736-745.
- Ten Dam E, Korsten Meijer AGW, Hoving EW, Kuijlen JM, van der Laan BFAM, et al. (2019) Evaluation of the psychometric properties of the endoscopic endonasal sinus and skull base surgery questionnaire (EES-Q) in a prospective cohort study. Clin Otolaryngol 44(4): 565-571.
-
David Bedoya, Joaquim Enseñat, Isam Alobid, Cristobal Langdon. Functional Outcomes in Endoscopic Endonasal Surgery of the Skull Base, A rising challenge. On J Otolaryngol & Rhinol. 1(4): 2019. OJOR.MS.ID.000520.
-
Rhinorrhea, Sinonasal symptoms, Hypophysectomy, Chronic sinusitis, Allergic rhinitis, Septoplasty, Endoscopic polypectomy, Turbinectomy
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






