 Research Article
Research Article
Retropharyngeal Abscesses in Adult Patients: A Single Center Case Series of Risk Factors, Diagnostic Modalities, and Management
Michael Nicolette BA1*, Yekaterina Shapiro MD1,2, Bailey Balouch MD2, Mary Penckofer BA1, Marta Majewski BS1 and Donald Solomon MD1,2
1 Cooper Medical School of Rowan University, Camden NJ, USA
2 Division of Otolaryngology-Head and Neck Surgery, Department of Surgery, Cooper University Hospital, Camden NJ, USA
Michael Nicolette, Cooper Medical School of Rowan University, Camden NJ, USA.
Received Date: June 02, 2025; Published Date: June 13, 2025
Abstract
Background: Retropharyngeal abscess is a potentially life-threatening condition that is rare in the adult population. The present study sought
to identify risk factors, diagnostic modalities, management strategies and treatment outcomes of retropharyngeal abscesses in adult patients.
Methods: This was a single-institution retrospective series of adult patients with retropharyngeal abscess.
Results: Fifty adult patients were included. Risk factors included obesity, history of smoking, intravenous drug use, diabetes, and dental
infection. Presenting symptoms included dysphagia, odynophagia, cervical pain, decreased range of motion of the neck, and neck swelling. The
predominant causative organism was Streptococcal species, most commonly Viridans groups Streptococci, and ampicillin-sulbactam was the
most utilized antimicrobial agent. Incision and drainage was performed in 46% of cases. There was 1 recurrence of retropharyngeal abscess. No
mortalities were observed in this study.
Conclusion: Retropharyngeal abscess must be considered in patients presenting with dysphagia, odynophagia, and neck swelling. Appropriate
antibiotic initiation, and often incision and drainage, is critical to avoid complications such as mediastinitis and sepsis.
Keywords: Retropharyngeal abscess; Deep neck space infection; Infections of the head and neck; Incision and drainage, Adult retropharyngeal abscess
Introduction
Retropharyngeal abscess (RPA) is defined as suppurative infection of the deep spaces of the retropharynx [1, 2]. RPAs commonly occur in children, due to the presence of retropharyngeal space lymph nodes-nodes of Rouviere-however, these retropharyngeal lymph nodes typically involute by late childhood, making infection of the retropharyngeal space much less common in adult patients [3]. Infection of the retropharyngeal space in adults is often asso ciated with a traumatic injury-commonly foreign body ingestion in up to 60% of adult cases [3]. When no trauma is present, it has been previously shown that factors associated with the development of RPAs in adults include immunosuppression, cervical spine osteomyelitis, history of intravenous (IV) drug use, obesity, and cancer [4]. Common presenting symptoms in RPA are dysphagia, neck swelling, and sore throat [5]. RPAs are commonly diagnosed via a combination of history, physical exam, computed tomography or MRI and are most often treated with antibiotics and surgical drainage. Treatment typically begins with a trial of antibiotics followed by incision and drainage if symptoms worsen or fail to improve in 24-48 hours [6]. Causative organisms include species of Staphylococcus, Streptococcus, and Fusobacterium [2, 4, 5, 7].
In this study we sought to further elucidate the most common risk factors for RPA as well as to evaluate imaging modalities, treatment options, clinical course, and outcomes in the adult patient population. To our knowledge this is the largest reported single-institution series evaluating adult RPA.
Methods
Patient population
This was a single-institution retrospective case series evaluating adult patients with RPA treated at our tertiary care medical center. Only patients above the age of 18 years old were included. There were 72 patients with a diagnosis of RPA in their medical record. However, 22 of these patients were found to not have an RPA on further evaluation of imaging. The remaining 50 patients were included in this study.
Statistics
Statical analysis was performed using SPSS version 29 (IBM, Armonk NY). Descriptive statistics were used to determine mean age, gender breakdown, incidence of risk factors, diagnostic modalities, causative organisms, and complications. The Fisher’s exact test was used to analyze categorical variables and are reported as odds ratio (OR) with 95% confidence interval. Independent samples t-test was used to analyze continuous variables and reported at mean ± standard deviation. A p value < 0.05 was considered statistically significant. All tests were run two-tailed.
Ethics
This study was approved by the local institutional review board with waiver of informed consent.
Results
Demographics and presenting characteristics
A total of 50 adult patients were included in this case series as described in table 1. 50% were male and 50% were female. The average patient age was 50.9 ± 17.4 (range = 20-83). The average BMI was 30.3 ± 9.3 (range = 17.4-70.4). The majority (64.0%) of patients were white. Pertinent past medical history can be seen in table 2 and included obesity (42.0%), tobacco use (24.0%), diabetes (18.0%), dental infection (10.0%), and intravenous drug use (8.0%). Eight patients (16.0%) had a history of cancer, and 4 (8.0%) had a tumor in the head or neck. Only 1 patient (2.0%) in this series had a recent history of trauma.
Table 1:Patient demographics.
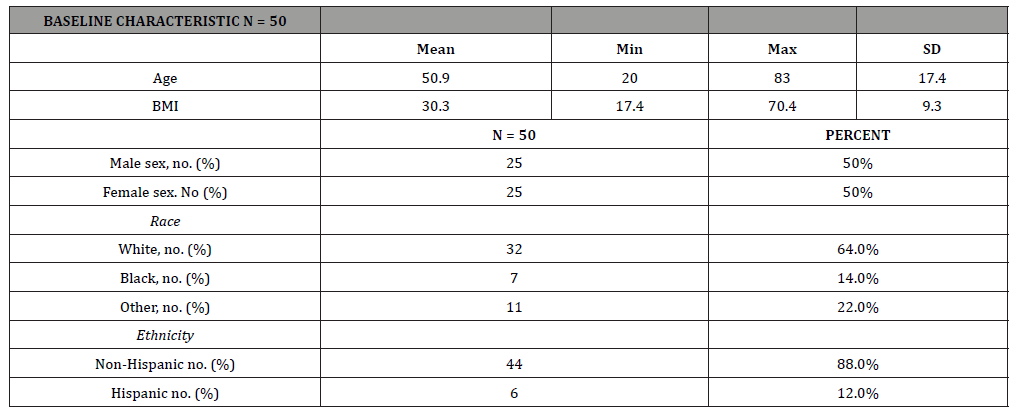
Table 2:Descriptive statistics.
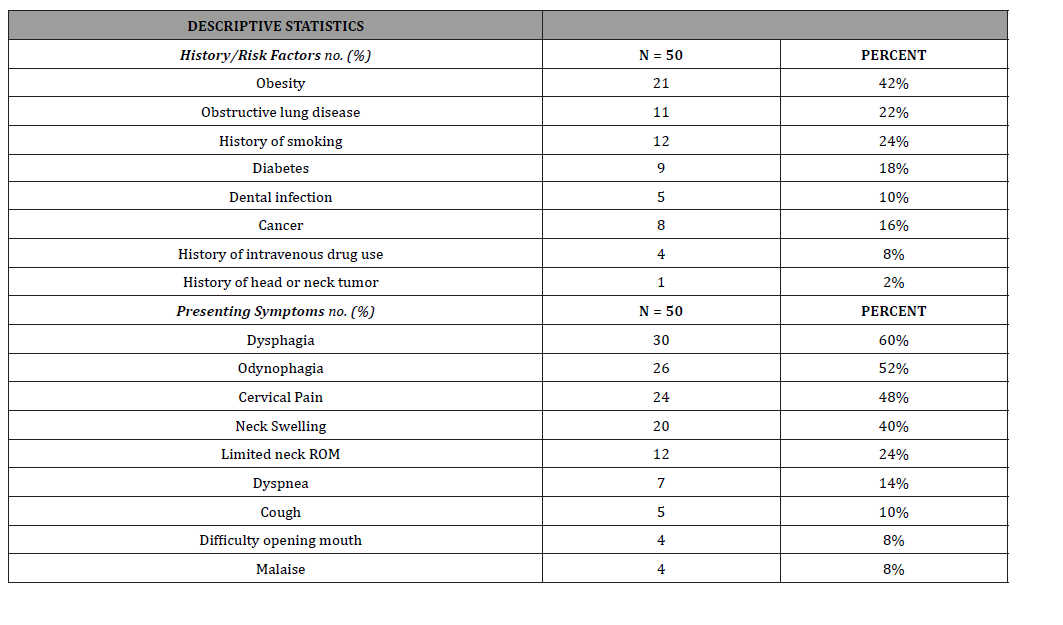
Dysphagia was the most common presenting symptom, noted in 60.0% of patients. This was followed by odynophagia (52.0%), cervical pain (48.0%), neck swelling (40.0%), dyspnea (14.0%), and cough (10.0%). Trismus and malaise were only present in 8.0% of patients and retrosternal pain was not present in any patients. Limited range of motion of the cervical spine was only seen in 24.0% of cases. Computed tomography was used in nearly all cases (96.0%) to make a diagnosis and MRI was used in 20.0% of cases. Average RPA size was 4.6 ± 2.8 cm in largest dimension on imaging.
Airway management and enteral access
36.0% of patients were monitored in an ICU setting during their admission for RPA. Enteral access via nasogastric feeding tube was required in 22.0% of cases, and 1 patient (2.0%) ultimately required gastrostomy tube placement. No patients received total or peripheral parenteral nutrition during their hospitalization. Flexible fiberoptic nasopharyngolaryngoscopy was performed in 60.0% of patients to evaluate for airway obstruction. 24.0% of patients required intubation for airway protection and remained intubated for an average of 3.8 ± 2.6 days. Four patients (8.0%) were intubated via awake fiberoptic intubation. Four patients (8.0%) ultimately required tracheostomy. Of those, 2 were decannulated (at 23 and at 30 days post-tracheostomy) and 2 were not decannulated before being lost to follow up.
Microbiology
Cultures were obtained in 50.0% of patients, of these cultures 92.0% evidenced bacterial growth. Cultures most commonly grew streptococcal (60.0%) or staphylococcal (44.0%) species, as seen in table 3. Viridans group Streptococci were the most common organisms identified (52.0%). Other organisms included Staphylococcus Aureus (24.00%), Rothia Mucilaginosa (12.0%), and Neisseria species (8.0%). Candida species was identified in 12.0% of cases.
Table 3:Microbiology and Antibiotics.
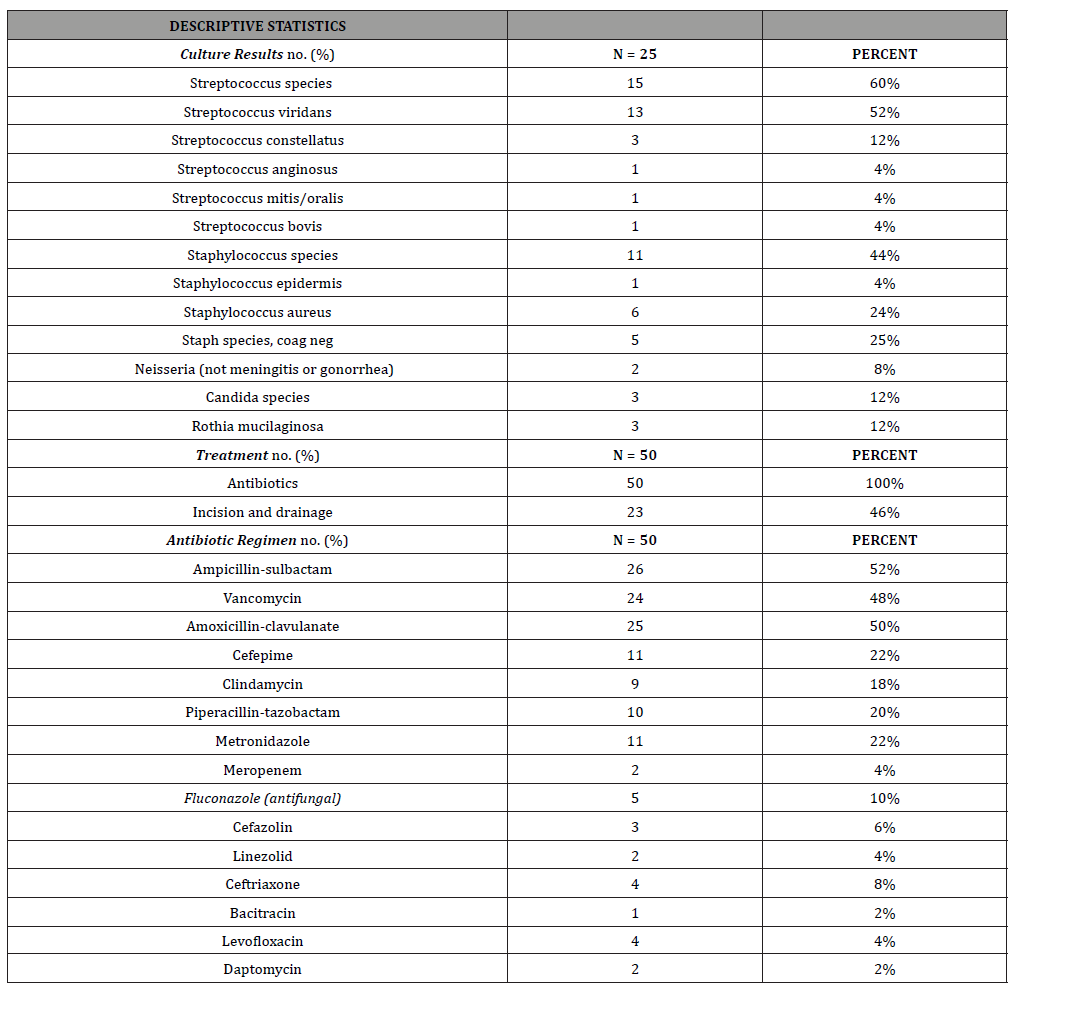
Management
Management for RPA included antibiotics in all cases, most commonly ampicillin-sulbactam (52.0%), usually followed by amoxicillin-clavulanate (50.0%). Vancomycin was used in 48.0% of cases. Less commonly used antibiotics included cefepime (22.0%), metronidazole (22.0%), piperacillin-tazobactam (20.0%), and clindamycin (18.0%). Fluconazole was also administered in 10.0% of cases. In addition to antimicrobial therapy, 46.0% of patients underwent incision and drainage of their RPA. Patients requiring ICU admission (OR = 5.720 [1.600-20.445]), intubation (OR = 9.615 [1829-50.546]), tracheostomy (OR = 1.211 [1.004-1.460]), or nasogastric feeding tube placement (OR = 20.000 [2.305-173.553]) were significantly more likely to undergo incision and drainage.
Outcomes
No mortalities were observed in this study. The average hospital length of stay was 8.8 ± 7.9 days (range = 0-31 days). Patients who required incision and drainage of their RPA had a significantly longer hospital length of stay compared to those who were treated with antibiotics alone (13.0 ± 8.6 days versus 5.2 ± 5.0 days, p <0.001). One patient (2.0%) had recurrence of their RPA after discharge.
Discussion
From this single center case series of adult patients with retropharyngeal abscess, several points of insight were gleaned. The first being that risk factors for RPA in our study included obesity, smoking tobacco, IV drug use, diabetes, dental infection and cancer. Contrary to what has previously been reported in the literature, only 1 of our 50 patients had a trauma preceding development of an RPA.
With regard to presenting symptoms, our findings aligned with previous reports. We noted that dysphagia, odynophagia, neck swelling, cervical pain, limited range of motion of the neck, dyspnea and cough were the most common complaints associated with RPA. Only 4 patients experienced trismus and malaise while no patients presented with retrosternal pain. History, physical exam and computed tomography were most useful in making the diagnosis of RPA, followed by X-ray and MRI.
Airway evaluation and management is a major consideration in adult patients with RPA, and may include flexible fiberoptic evaluation, monitoring in an intensive care unit setting, intubation, and in select cases tracheostomy. In this series, a quarter of patients required intubation for airway protection and approximately one third were admitted to the intensive care unit.
The most common treatment modalities utilized in our adult RPA population were intravenous antibiotics, with ampicillin-sulbactam being utilized most frequently. Vancomycin was commonly utilized as second line coverage. Just under half of our patients underwent operative incision and drainage. Predisposing characteristics of adult RPA patients likely to undergo incision and drainage were requiring ICU admission, intubation, tracheostomy, or NG tube feeding. Conservative management with antibiotics alone was utilized for clinically stable patients with no initial indication for operative management. Incision and drainage was reserved for patients with potential airway compromise or for those who are not improving clinically while on antibiotic treatment which was in keeping with what is described in the literature [8, 9, 10]. Additional indications for incision and drainage described in prior studies includes signs of mediastinitis and meningitis, however no patient in our series evidenced these complications of RPA [11, 12]. Prior studies have also suggested that larger size of abscess, limited neck range of motion, bulging pharyngeal walls, or multiple abscesses are clinical signs that may warrant operative management [12, 13].
Patients that underwent incision and drainage in our series notably had longer hospital courses than those who did not. These patients more frequently underwent intubation, tracheostomy and ICU placement, which led to prolonged hospitalization compared to those patients managed more conservatively by antibiotics alone.
The most common causative organisms noted in our series were species of Streptococcus or Staphylococcus which is consistent with prior literature. The most common causative organisms reported previously were groups A and B streptococcus along with Staphylococcus aureus [14].
Only 1 of our patients (2%) experienced recurrence of RPA, which is similar to prior reports which found recurrence rates of approximately 5% [15]. Common reported complications of retropharyngeal abscess are airway obstruction, respiratory distress, acute hypoxemic respiratory failure and sepsis [16]. In our series these complications were noted in X, Y and Z%s respectively. Finally, the mortality rate for retropharyngeal abscesses in adults has been reported to be approximately 2% and mortality has been associated with preexisting comorbidities [17, 18]. There were no deaths reported in our case series.
Our study, while larger than prior series reporting on adult RPA, was limited by relative small sample size. An additional limitation of our finding was that cultures were typically only obtained from patients who underwent operative drainage, limiting the number of patients on whom the determination of causative organisms could be ascertained.
Conclusion
While rare in adult patients, retropharyngeal abscess is a cannot miss diagnosis due to its potential for airway compromise and serious complications. It is imperative to consider the diagnosis of RPA in patients presenting with dysphagia, odynophagia, cervical pain, limited range of motion of the neck, and neck swelling. This is particularly true in patients with past medical history of obesity, smoking, IV drug use, diabetes, dental infection, or cancer. Retropharyngeal abscess may be readily diagnosed with contrasted computed tomography of the neck. Treatment should be started promptly and is heralded by intravenous antibiotics followed by intubation, tracheostomy and surgical incision and drainage in select cases.
Acknowledgment
None.
Conflict of Interest
No conflict of interest.
Sources of Funding
None.
References
- Harkani A, Hassani R, Ziad T (2011) Retropharyngeal abscess in adults: five case reports and review of the literature. Scientific World Journal 11: 1623-1629.
- Benmansour N, Benali A, Poirrier AL, Cherkaoui A, Oudidi A, et al. (2012) Retropharyngeal abscess in adults. Rev Laryngol Otol Rhinol (Bord). 133(3): 137-139.
- Sideris G, Nikolopoulos T, Papadimitriou N (2020) Spontaneous, Non-Traumatic Retropharyngeal Abscess Complicated by Spinal Osteomyelitis and Epidural Abscess in Immunocompetent Adult: Management and Proposal Pathophysiological Mechanism. Cureus 12(7): e9028.
- Sanz Sánchez CI, Morales Angulo C (2021) Retropharyngeal Abscess. Clinical Review of Twenty-five Years. Acta Otorrinolaringol Esp (Engl Ed). 72(2): 71-79.
- Hajare PS, Bellad SA, Anand A, Narahari S, Jadhav AV (2022) Disparate Presentations of Retropharyngeal Abscess: An Experience from a Tertiary Care Centre. Indian J Otolaryngol Head Neck Surg 74(Suppl 3): 5984-5989.
- Sudhir BS, Shawn L, Chan K, Samridh S (2023) Retropharyngeal Abscess - When to Drain? Clinics in Surgery.
- Schott CK, Counselman FL, Ashe AR (2013) A pain in the neck: non-traumatic adult retropharyngeal abscess. J Emerg Med 44(2): 329-331.
- Brook I (2004) Microbiology and management of peritonsillar, retropharyngeal, and parapharyngeal abscesses. J Oral Maxillofac Surg 62(12): 1545-1550.
- Akhavan M (2021) Ear, Nose, Throat: Beyond Pharyngitis: Retropharyngeal Abscess, Peritonsillar Abscess, Epiglottitis, Bacterial Tracheitis, and Postoperative Tonsillectomy. Emerg Med Clin North Am 39(3): 661-675.
- Elishar R, Sichel J, Gomori JM, Saah D, Elidan J (1999) Role of computed tomography scan in the diagnosis and treatment of deep neck infections in children. Laryngoscope109: 844.
- Page NC, Bauer EM, Lieu JE (2008) Clinical features and treatment of retropharyngeal abscess in children. Otolaryngol Head and Neck Surg 138(3): 300-306.
- Grisaru Soen G, Komisar O, Aizenstein O, Soudack M, Schwartz D, et al. (2010) Retropharyngeal and parapharyngeal abscess in children—epidemiology, clinical features and treatment. Int J Pediatr Otorhinolaryngol 74(9): 1016-1020.
- Wong DK, Brown C, Mills N, Spielmann P, Neeff M (2012) To drain or not to drain–Management of pediatric deep neck abscesses: A case–control study Int J Pediatr Otorhinolaryngol 76(12): 1810-1813.
- Sánchez CIS, Angulo CM (2021) Retropharyngeal abscess. clinical review of twenty-five years. Acta Otorrinolaringol (Engl Ed) 72(2): 71-79.
- Goldenberg D, Golz A, Joachims H (1997) Retropharyngeal abscess: a clinical review. J Laryngol Otol 111(6): 546-550.
- Jain H, Hohman MH, Sinha V (2024) Retropharyngeal Abscess. In: StatPearls [Internet].
- Yang TH, Xirasagar S, Cheng YF, Wu CS, Kao YW, et al. (2021) A nationwide population-based study on the incidence of parapharyngeal and retropharyngeal abscess—a 10-year study. Int J Environ Res Public Health 18(3): 1049.
- Ridder GJ, Technau Ihling K, Sander A, Boedeker CC (2005) Spectrum and management of deep neck space infections: an 8-year experience of 234 cases. Otolaryngol Head and Neck Surg 133(5): 709-714.
-
Michael Nicolette BA*, Yekaterina Shapiro MD, Bailey Balouch MD, Mary Penckofer BA, Marta Majewski BS and Donald Solomon MD. Retropharyngeal Abscesses in Adult Patients: A Single Center Case Series of Risk Factors, Diagnostic Modalities, and Management. On J Otolaryngol & Rhinol. 7(5): 2025. OJOR.MS.ID.000671
-
Retropharyngeal abscesses, Neck swelling, Dysphagia, Odynophagia, Cervical pain, Lymph nodes, Sore throat, Nasopharyngolaryngoscopy, Retrosternal pain, Tracheostomy
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






