 Research Article
Research Article
Prevalence of Immunodeficiency in Children with Trisomy 21 Requiring Frequent ENT Intervention
Chang A1*, Pitts M2, Eidson N3, Downs E3, White DR4 and Williams KW5
1B.A., Medical University of South Carolina (MUSC), College of Medicine, USA
2B.S., MUSC, College of Medicine, USA
3M.D., MUSC, Department of Pediatrics, USA
4M.D., MUSC, Professor, Department of Pediatric Otolaryngology, USA
5M.D., M.P.H., MUSC, Associate Professor, Department of Pediatrics, Division of Pediatric Pulmonology, Allergy & Immunology, USA
Prior Presentations: This work was presented as a poster at the Triological Society combined sections meeting in Orlando, Florida in January 23-25, 2025
Anna Grace Chang, B.A., 171 Ashley Ave., Charleston, SC, 29425, USA.
Received Date: January 21, 2026; Published Date:January 30, 2026
Abstract
Objective: To assess whether immunodeficiency in children with Trisomy 21 (T21) is associated with an increased need for otolaryngologic
procedures.
Study Design: Retrospective chart review.
Setting: Quaternary care academic center.
Methods: Patients ≤ 18 years of age with T21 were identified in the electronic medical record (EMR). Data were collected from the EMR
from August 2023 to July 2025, including demographics, referrals to otolaryngology and immunology, number and type of otolaryngologic (ENT)
procedures done, immunodeficiency diagnosis, and treatment status. Descriptive statistics were calculated, and student’s t-test was used to assess
variables with significance set at p < 0.05.
Results: 396 patients with T21 were included. Of these, 245 patients (61%) had at least one ENT procedure. The three most common procedures
were tympanostomy tube placement, airway endoscopies, and tonsillectomies/adenoidectomies. 57 (14.4%) patients were referred to Allergy and
Immunology, 24 patients completed immune evaluation, and 15 patients were diagnosed with an immunodeficiency (3.9%). The average number
of ENT procedures for patients with confirmed immunodeficiency was 9.6 vs. 2.4 in those who did not have a lab-confirmed immunodeficiency
(p<0.001).
Keywords: Trisomy 21, Down syndrome; Immunology; Immunodeficiency; Tympanostomy tubes; Tonsillectomy and adenoidectomy
Abbreviations: T21 - Trisomy 21; Ear, Nose, and Throat - ENT
Introduction
Trisomy 21 (T21), or Down Syndrome, is estimated to affect 14.47 per 10,000 live births in the United States [1]. T21 is often associated with pathologies of the ears, nose, and throat such as obstructive sleep apnea, chronic otitis media, hearing loss, and chronic rhinosinusitis. The increased burden of disease amongst individuals with T21 is, in part, related to anatomic factors. For example, the midface hypoplasia phenotype of many patients may contribute to abnormal insertion of the eustachian tube into the nasopharynx and subsequent increased risk of otitis [2]. Diminished immune function also plays a role in development of ear, nose, and throat pathologies (i.e. a predisposition to recurrent upper airway tract infections may lead to more episodes of otitis media) [2]. While not all T21 patients will have immunologic abnormalities, according to Lagan et al., T21 is the most common genetic disorder associated with immune dysregulation. This encompasses both immunodeficiency and a predisposition to autoimmunity [3]. Multiple factors contribute to immunologic dysfunction in T21 patients, namely: T and B cell lymphopenia, reduced neutrophil chemotaxis, diminished specific antibody responses to immunization, and impaired T cell proliferation in response to mitogens [4]. As a result, children with T21 can be at increased risk of infection, which can lead to recurrent and prolonged hospitalization -- approximately twice as long as that of children without T21. Patients with T21 also experience a greater than 30% mortality from sepsis [3, 5].
Early referral to immunology specialists may reduce infection-related morbidity and mortality in patients with T21. Potential interventions include the use of prophylactic antibiotics or immunoglobulin replacement therapy for patients with immunodeficiency, additional vaccinations, or alterations in antibiotic dosing [6, 7]. One challenge that remains is encouraging early contact between patients with T21 and immunology specialists. Patients with T21 are already tasked with seeing subspecialists in cardiology, gastroenterology, otolaryngology, and more – a process which may be overwhelming and time-consuming for families. As such, it would be beneficial to recommend T21 patients for immunologic evaluation from pre-existing points of contact. This paper investigates one potential proxy measurement for immunodeficiency in T21 patients: number of otolaryngologic procedures. It has been demonstrated that patients with T21 require more otolaryngologic interventions than the general population. In this paper, we hypothesize that patients with T21 who require a larger number of otolaryngologic procedures are more likely to have an underlying immunodeficiency. Patients with many procedures may benefit from early referral to immunology specialists for workup of potential immunodeficiency.
Materials and Methods
A retrospective chart review was conducted on 400 patients with Trisomy 21 ages 18 and under at our quaternary care center. All patients with a diagnosis of Trisomy 21 listed in their medical record were included in the initial data collection. Using the electronic medical record (EMR), data were collected between August 2023- July 2025 regarding demographics, number and types of procedure, referrals to otolaryngology and immunology, immunodeficiency diagnosis, and treatment status. Immunodeficiency was defined as intrinsic defects in immune function, proven by laboratory analyses such as immunoglobulin levels, response to the S. pneumoniae vaccine, and lymphocyte subtype analyses. Following data collection, descriptive statistics, student’s T test, and calculations of test characteristics were performed. Patients who had undergone open airway surgery for congenital malformations (i.e. complete tracheal rings requiring laryngoplasty) were excluded from data collection. Further, in order to mitigate possible misclassification bias due to the fact that only a small percentage of the patients actually completed an immunologic workup, we performed a subgroup analysis including only the children definitively tested for immunodeficiency.
This project was reviewed and approved by IRB-I – Medical University of South Carolina. In accordance with 45 CFR 46.104(d), this study was considered exempt from Human Research Subject Regulations.
Results
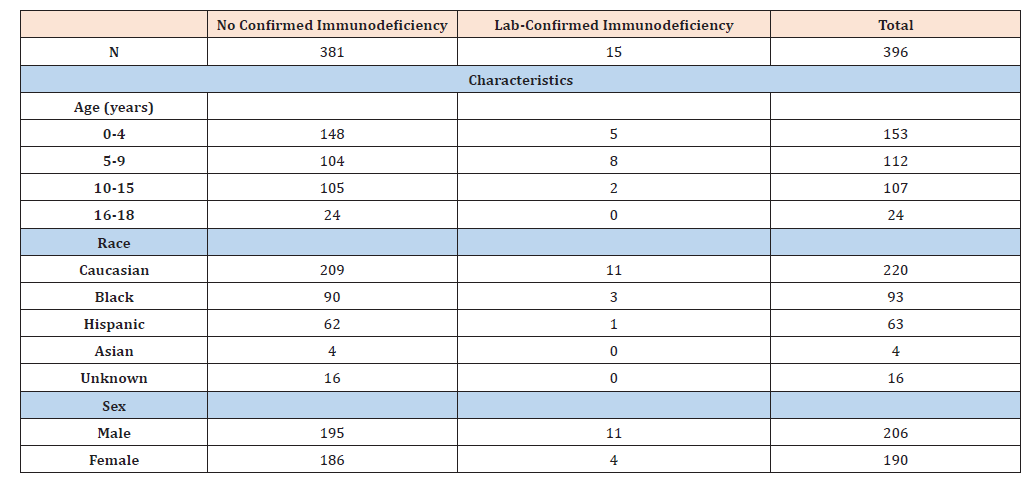
We identified 400 patients that were 18 years & under and diagnosed with Trisomy 21. Of the 400 patients, 4 patients were excluded given a history of open airway surgery related to congenital malformations. The excluded patients’ demographics were: 3 Black males and 1 Caucasian female; none were referred to immunology/ allergy or diagnosed with an immunodeficiency. Of the 396 patients included in data analysis, the majority were Caucasian (55.6%), followed by Black (23.5%), and Hispanic (15.9%). The average age at time of data extraction was 7.25 years old (Table 1). There was no statistically significant difference between the average ages of our two populations.
Table 1:Demographic Distribution of Patients with Trisomy 21 and ≤ 18 years old.
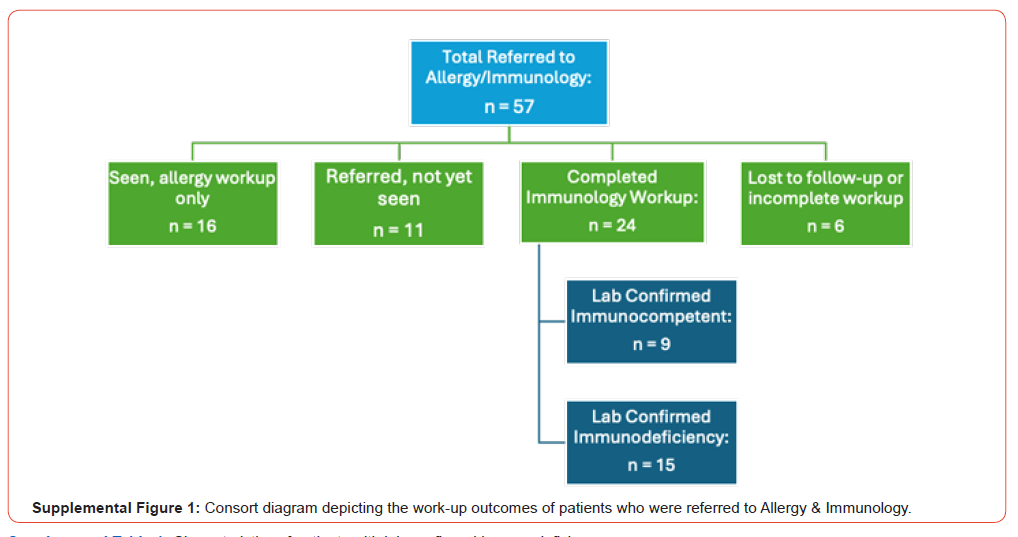
Of the patients included in analysis, 57 (14.4%) were referred to Allergy and Immunology specialists. The mean age at time of first Allergy & Immunology referral was 4.5 years old versus 3.4 years old for referral to Otolaryngology. The majority of patients referred to Allergy & Immunology were males (65.5%). At time of data extraction, 24 out of the 57 referred patients had completed an immunologic workup. 15 of the 24 patients (62.5%) who completed a full immunologic workup were diagnosed with immunodeficiency (Supplemental Figure 1). 73% of the patients with confirmed immunodeficiency were males, while males comprised 51.3% the immunocompetent population. Anti-pneumococcal polysaccharide antibody deficiency (memory subtype) was the most common diagnosed immunodeficiency (67%) followed by IgM deficiency (33%). Other immunodeficiencies identified include common variable immunodeficiency, B cell lymphopenia, and T cell lymphopenia. Some children had multiple immune abnormalities, such as co-occurring IgM deficiency and B-cell lymphopenia (Supplemental Table 1).
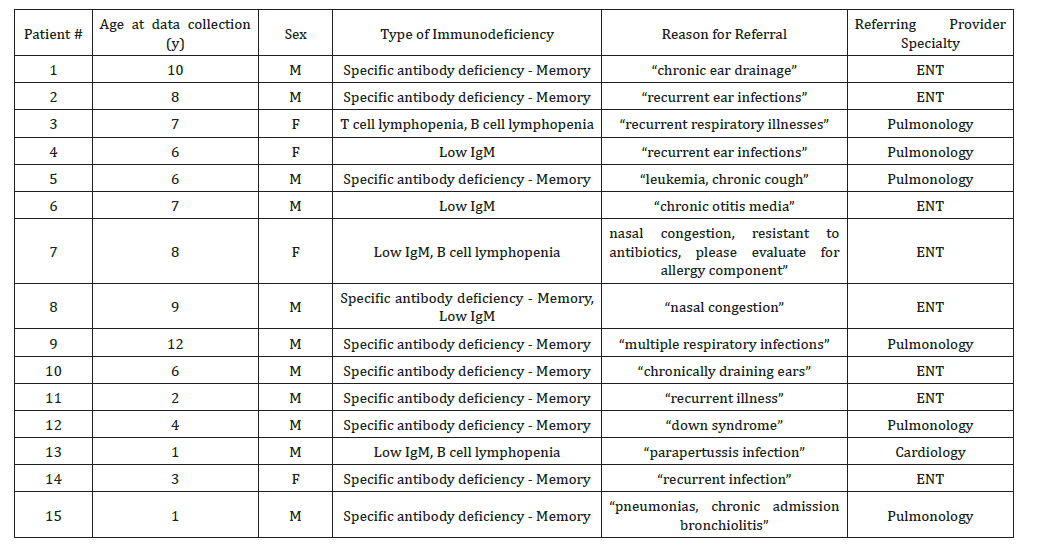
Supplemental Table 1:Characteristics of patients with lab-confirmed immunodeficiency
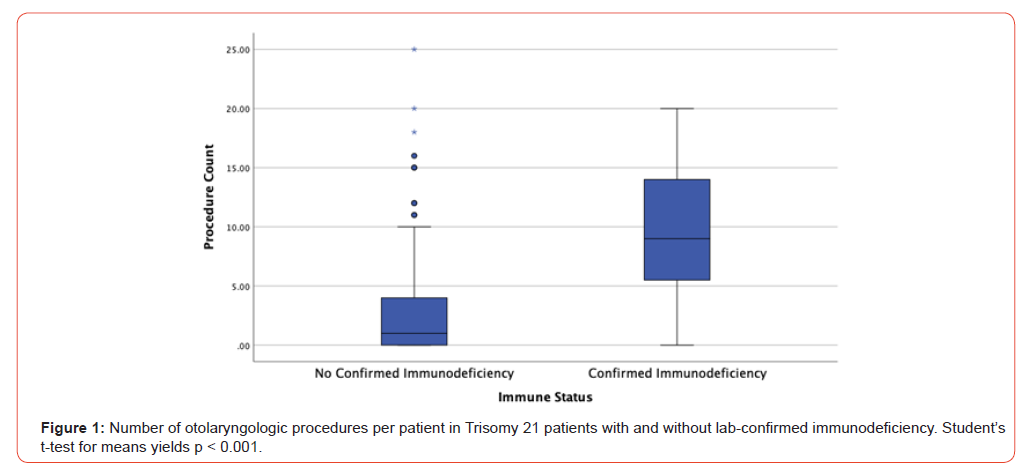
The average number of otolaryngologic procedures for patients without a lab-confirmed immunodeficiency was 2.35 [95% CI 2.02,2.69] versus 9.60 [6.34,12.86] for patients with a diagnosed immunodeficiency (p<0.001) (Figure 1). We also compared the mean number of procedures in patients with lab-confirmed immunodeficiency — 9.60 [6.34,12.86] — with the mean in patients with proven immunocompetence, 4.22, 95% CI [6.34,12.86]). The difference between these means was also significant (p<0.05). Patients were considered to have proven immunocompetence if they underwent immune evaluation, but findings were consistent with normal immune function.
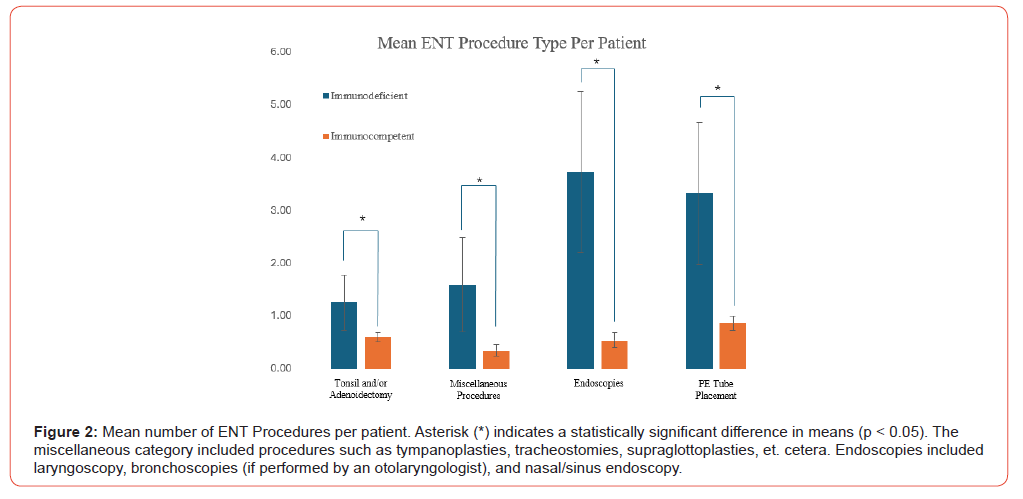
The most performed ENT procedure in our patient population overall was tympanostomy tube placement (36.1% of all procedures), followed by endoscopic airway procedures (25%). The prevalence of tonsillectomy & adenoidectomy was higher among patients with an immunodeficiency (78.6%) than in patients without an immunodeficiency (42.9%). Endoscopic airway procedures, including laryngoscopies/micro laryngoscopies, sleep endoscopies, and bronchoscopies (excluding those performed by pulmonologists), were also more commonly performed in the immunodeficient patients than T21 patients without immunodeficiency. 93% of immunodeficient patients required at least one endoscopic airway procedure, versus only 24.6% of patients without immunodeficiency. The average number of pressure-equalizing (PE) tube placements per patient in the immunodeficient group was 3.3 (n=15) compared to 0.9 per patient in the immunocompetent group (n=381) (p < 0.05) (Figure 2). Of note, 100% of patients with confirmed immunodeficiency were found to be vaccinated against Hemophilus influenza and Streptococcus pneumoniae at the time of data collection.
Given the small number of patients with confirmed immunodeficiency (n=15), logistic regression was not performed. In order to define a threshold of otolaryngologic procedures above which patients should be referred to Allergy/Immunology, we calculated sensitivity, specificity, and positive predictive values of various procedural count cutoffs in identifying patients with confirmed immunodeficiency (see Table 2). Procedure count cutoffs chosen were 0.5, 1, and 1.5 standard deviations above the mean procedure count for an immunocompetent patient.
Table 2:Sensitivity, specificity, and positive predictive value of several procedural counts in correctly identifying confirmed immunodeficiency
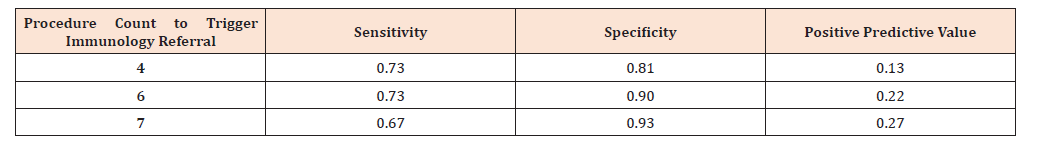
The test characteristics in Table 2 represent the use of number of procedures of any type in screening for immunodeficiency. Alternatively, clinicians could use the number of PE tube placements alone to screen for immunodeficiency. Using > 3 tube placements as the cutoff above which a child should have an immune evaluation yields a positive predictive value of 0.23 in capturing immunodeficiency (sensitivity 0.47, specificity 0.94).
Discussion
Our findings demonstrate that an increased necessity for otolaryngologic procedures may be correlated with an increased probability of underlying immunodeficiency in children with T21. Given this finding, we recommend that otolaryngologists caring for patients with trisomy 21 maintain a low threshold of suspicion for potential immunodeficiency and consider early referral to Immunology providers. However, we recognize that an objective threshold may be beneficial given that patients with T21 are already tasked with seeing multiple subspecialists and that their otolaryngologic providers may not know when the burden of surgical intervention is abnormal. We propose a threshold of six ENT procedures of any type as the cutoff above which patients should be recommended for immune evaluation. This threshold has 73% sensitivity and 90% specificity for the identification of patients with confirmed immunodeficiency. More specifically, we propose a threshold of three PE tube placements as a point above which immune evaluation is recommended for children with T21 (47% sensitivity, 94% specificity).
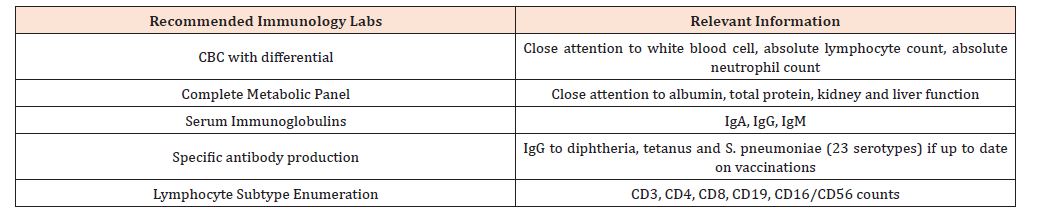
A measurement with high sensitivity is desirable in this instance given the significant negative outcomes (prolonged hospitalization and increased sepsis-related mortality) associated with undiagnosed immunodeficiency. Further, a measurement with high specificity is desired to avoid unnecessary workups which may be expensive and invasive. An initial immune evaluation for a patient with Trisomy 21 typically includes a complete blood count with differential, complete metabolic panel, serum immunoglobulins, specific antibody production to some vaccinations, and lymphocyte subtype enumeration by flow cytometry (see Table 3). Estimated cost for these tests by self-pay is $923.50. Estimated blood volume for these tests is 5 mL. If abnormalities are identified on initial immunology labs, more detailed flow cytometry and functional assays are required. We recognize that immunologists may not be readily accessible in all communities. The recommended initial immunology labs (see Table 3) are readily available at most commercial laboratories. While the cost and burden of these labs may be high for some patient families, it is worth noting that this is less than the cost of a single tympanostomy tube placement. As such, we recommend a shared decision-making process between providers and their patients regarding whether it would be preferable to consider even earlier immune evaluation in order to avoid further otolaryngologic interventions.
Table 3:Recommended immune function labs as part of an initial immunodeficiency workup. These labs can be ordered by pediatricians and otolaryngologists, in addition to immunologists.
Our evaluation has identified that patients with T21 who have confirmed underlying immunodeficiency require significantly more otolaryngologic procedures, including tympanostomy tubes, than those without immunodeficiency. This finding is likely multifactorial. Patients with immunodeficiency and T21 have an increased incidence of upper respiratory tract infections (URIs) [2, 4]. This acute infectious state detracts from proper mucociliary tract clearance by causing inflammation of the nasopharyngeal and tubal mucosa [8]. Consequently, frequent URIs in patients with immunodeficiency can lead to impaired clearance of otitis media and cause chronic middle ear effusions. As such, patients with Trisomy 21 and immunodeficiency may require more PE tube placements than those without immunodeficiency. Additionally, children with Trisomy 21 and immunodeficiency may more frequently require tonsillectomies and/or adenoidectomies than their immunocompetent counterparts. To our knowledge, there has not yet been a study to evaluate potential correlations between obstructive sleep apnea and immunodeficiency in Trisomy 21. One study conducted by Andersen et al. did find evidence of altered immune function in tonsillar hypertrophy specimens, namely increased Th17 cells [9]. This finding may suggest a role of autoimmunity, another common finding in the spectrum of immune dysregulation amongst patients with Trisomy 21. Finally, an immature immune system (superimposed on anatomic differences) may also contribute to an increased incidence of chronic rhinosinusitis [10].
There are several limitations to this study. First, our sample size of patients with confirmed immunodeficiency was small, making it inappropriate to perform logistic regression to model our data. The small sample size also limits generalizability of the data. 15 of 24 (63%) patients who had completed an immunology workup were found to have confirmed immunodeficiency. Unfortunately, several patients were either lost to follow-up or had yet to complete their immune evaluation at the time of data collection. Additionally, there is no way to confirm whether patients who have not undergone immunologic evaluation are truly immunocompetent. For this reason, we conducted a brief subgroup analysis comparing mean number of ENT procedures in the confirmed immunodeficiency versus confirmed immunocompetence groups. Of note, this analysis did produce a significant difference of means. Further follow-up on the patients in this study that have not yet completed immune evaluation would improve the power of this study and allow for more thorough statistical analysis.
Furthermore, this study involves a potential selection bias, as patients are often referred to immunologists based on a clinical suspicion of immunodeficiency – often because of frequent otolaryngologic procedures or persistent otorrhea after tube placement. In our study, 53% of patients with confirmed immunodeficiency were originally referred to Immunology by an otolaryngologist. The most common reason for referral was chronic otitis media (33%). While this selection bias may falsely emphasize the difference in number of procedures between immunodeficient and non-immunodeficient patients, this finding further supports that otolaryngologists can play a critical role in connecting patients with Trisomy 21 with immunologic evaluation. Finally, the limited awareness surrounding immunodeficiency in patients with Trisomy 21 may be contributing to low referral rate and underdiagnosis. This study was also limited by inconsistent and/or incomplete documentation in EMR. From patient to patient, procedures were recorded in different places in the chart in different manners – we relied largely on matching procedures listed in operative notes to procedure dates listed in a patient’s “surgical history”. This process leaves margin for error in data collection. Vaccination history could also not reliably be gathered due to inconsistent charting. As such, we only collected vaccination status for the immunodeficient group, as this was reliably documented during patients’ immune evaluation.
The small number of patients with confirmed immunodeficiency also limits a thorough analysis of possible confounding variables. Our sample of immunodeficient patients was not any older, on average, than our control population. This suggests that age did not significantly impact the difference in mean number of procedures between the two groups. It is possible that socioeconomic status, not assessed in this study, could impact the ability for patients to undergo surgical procedures or attend immunology consultations. The same families which have the resources to pursue a thorough immunologic workup may have greater resources to pursue surgical treatment for their children.
Despite it being well established that T21 patients may have underlying immunodeficiency and experience recurrent infections [3, 4, 6], we noted a delay in patients being referred for immunology evaluation, as suggested by the mean age of referral to immunology (4.5 years) vs. ENT (3.4 years). Given the higher number of tube placement procedures in the T21 patients with immunodeficiency (mean 3.3 vs 0.9, p < 0.05), it is essential to evaluate children with Trisomy 21 for immunodeficiency because it is possible to prevent further illness-related morbidity and mortality through proper treatment. Patients with immunodeficiency can be treated with prophylactic antibiotics, immunoglobulin replacement therapy, booster vaccinations, and additional vaccines (i.e. palivizumab) to prevent infection. These interventions can improve quality of life and reduce hospital stays in children with Trisomy 21 and immunodeficiency.
Conclusion
Children with T21 have high rates of recurrent infections and require multiple otolaryngologic interventions. A portion of patients with T21 will also have underlying immunodeficiency, which is likely a contributor to their high healthcare utilization. Patients with T21 and underlying immunodeficiency require more otolaryngologic operations than their counterparts without confirmed immunodeficiency. Thus, patients with trisomy 21 who require multiple ENT surgical procedures, specifically tympanostomy tube placements, should be recommended for immune evaluation. These findings highlight the critical need for multidisciplinary care involving both otolaryngology and immunology to improve health outcomes in the vulnerable trisomy 21 population. These findings also emphasize the need for further research into the pathophysiology and natural course of immunodeficiency in patients with Trisomy 21.
Statements and Declarations
Acknowledgements: Not applicable.
Ethical Considerations: This project was reviewed and approved by IRB-I – Medical University of South Carolina. In accordance with 45 CFR 46.104(d), this study was considered exempt from Human Research Subject Regulations.
Declaration of Conflicting Interest: KW has research support from GlaxoSmithKline, ADMA Biologics, Cogent Biosciences, Pharming Healthcare, serves as a consultant and speaker with Amgen and Pharming Healthcare, and has served on the medical advisory boards with Kenota Health, Amgen, Pharming Healthcare, Blueprint Medicines. All other authors have no conflicts of interest.
Funding Statement: This project had no funding.
Data Availability: The data that support the findings of this study are available on request from the corresponding author, AC. The data are not publicly available in order to protect the privacy of patients studied, as they were collected from the electronic medical record.
References
- Parker SE, Mai CT, Canfield MA (2010) Updated National Birth Prevalence estimates for selected birth defects in the United States, 2004-2006. Birth Defects Res A Clin Mol Teratol 88(12): 1008-1016.
- Ramia M, Musharrafieh U, Khaddage W, Sabri A (2014) Revisiting Down syndrome from the ENT perspective: review of literature and recommendations. Eur Arch Otorhinolaryngol 271: 863-869.
- Lagan N, Huggard D, Mc Grane F (2020) Multiorgan involvement and management in children with Down syndrome. Acta Paediatr 109(6): 1096-1111.
- Ram G, Chinen J (2011) Infections and immunodeficiency in Down syndrome. Clin Exp Immunol 164(1): 9-16.
- Hilton JM, Fitzgerald DA, Cooper DM (1999) Respiratory morbidity of hospitalized children with Trisomy 21. J Paediatr Child Health 35(4): 383-386.
- Verstegen RHJ, Chang KJJ, Kusters MAA (2020) Clinical implications of immune-mediated diseases in children with Down syndrome. Pediatr Allergy Immunol 31(2): 117-123.
- Dalrymple RA, Somerville LH, Hamza S, Matta N (2022) Fifteen-minute consultation: The review of a child with trisomy 21 (Down's syndrome). Arch Dis Child Educ Pract Ed 107(2): 88-94.
- Iino Y, Imamura Y, Harigai S, Tanaka Y (1999) Efficacy of tympanostomy tube insertion for otitis media with effusion in children with Down syndrome. Int J Pediatr Otorhinolaryngol 49(2): 143-149.
- Anderson ME Jr, Buchwald ZS, Ko J, Aurora R, Sanford T (2014) Patients with pediatric obstructive sleep apnea show altered T-cell populations with a dominant TH17 profile. Otolaryngol Head Neck Surg 150(5): 880-886.
- Zalzal HG, Lawlor CM (2023) Down Syndrome for the Otolaryngologist: A Review. JAMA Otolaryngol Head Neck Surg 149(4): 360-367.
-
Chang A*, Pitts M, Eidson N, Downs E, White DR and Williams KW. Prevalence of Immunodeficiency in Children with Trisomy 21 Requiring Frequent ENT Intervention. On J Otolaryngol & Rhinol. 8(3): 2026. OJOR.MS.ID.000687.
-
ENT intervention, Otolaryngology, Obstructive sleep apnea, Chronic otitis media, Hearing loss, Chronic rhinosinusitis, Ears, Mose, Throat
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






