 Research Article
Research Article
Preclinical Evaluation of a Curved Water Jet System for Tissue Removal in Sphenoid Sinus, Frontal sinus, and Skull Base Surgery
Professor Hany Amin Riad M.D., Behna Faculty of Medicine, Egypt.
Received Date: June 16, 2025; Published Date: August 01, 2025
Introduction
Endoscopic surgery of the paranasal sinuses and skull base often involves navigating narrow, deep anatomical spaces that are challenging to access and visualize. The sphenoid sinus, frontal recess, and clivus are particularly problematic due to their proximity to critical neurovascular structures. Traditional instruments such as microdebriders, drills, and suction devices may cause unintended trauma or thermal injury [1].
Water jet dissection has emerged as a promising alternative in other surgical fields, offering selective tissue removal, minimal thermal damage, and preservation of underlying structures [2]. This study evaluates the feasibility, safety, and efficacy of a novel curved water jet system designed specifically for endoscopic sinus and skull base surgery.
Objectives
1. To assess the feasibility of using a curved water jet system for
tissue removal in hard-to-reach sinus and skull base regions.
2. To evaluate tissue selectivity and preservation of adjacent
structures.
3. To determine optimal water pressure settings for different
tissue types.
4. To compare outcomes with standard surgical tools.
Methods
Study Design
Experimental preclinical comparative study using fresh-frozen cadaveric sheep heads and ex vivo human cadaveric specimens.
Model Preparation
• Animal Model: 10 adult sheep heads (n=10), obtained postmortem
from abattoirs.
• Human Cadaveric Model: 5 fresh-frozen cadavers (approved
by Institutional Ethics Committee) [3].
• All models underwent CT imaging before surgery to confirm
anatomy.
Interventions
Each specimen underwent bilateral endoscopic access to:
• Sphenoid sinus
• Frontal sinus
• Ptyrgopalatine fossa and infratemporal fossa
Tissues were removed using:
• Curved water jet system at variable pressures (10-60 bar)
• Standard microdebrider
• Suction curette
The right side was treated with the water jet; the left side with
conventional tools.
Outcome Measures
• Primary Outcome:
o Degree of complete tissue removal (scored 0-4)
• Secondary Outcomes:
o Injury to surrounding bone and vessels (scored 0-3)
o Histopathological damage to adjacent mucosa and dura
o Time required for full exposure and debridement
o Surgeon satisfaction score (Likert scale 1-5)
Statistical Analysis
• Wilcoxon signed-rank test for paired comparisons
• One-way ANOVA for multiple pressure comparisons
• Inter-rater reliability using Cohen’s kappa
• Significance level: p < 0.05
• Software: SPSS v27
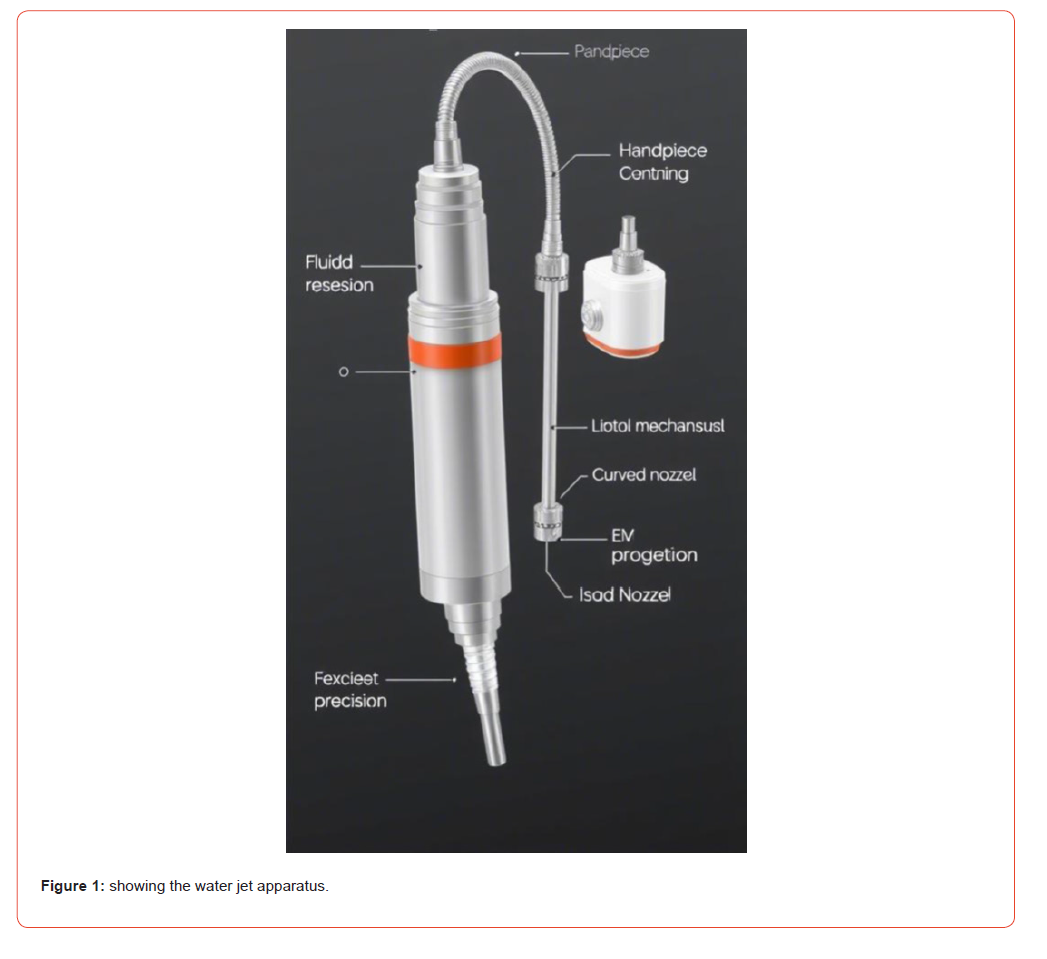
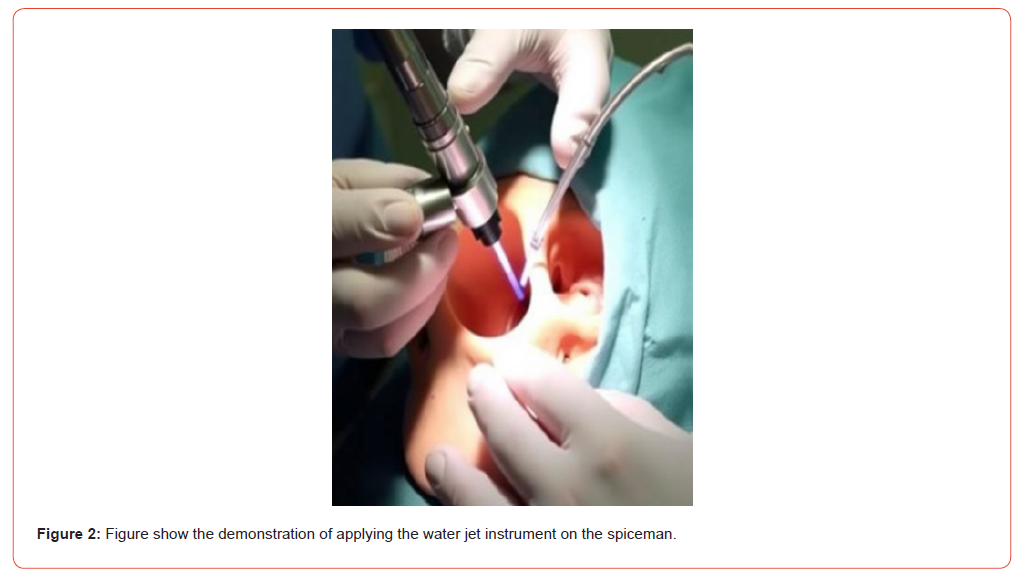
Results
Best scores at 30-60 bar. No significant difference between high-pressure water jet and microdebrider (p = 0.32)
Lower injury at low-to-mid pressure ranges compared to mechanical tools
Histology confirmed less damage at lower pressures
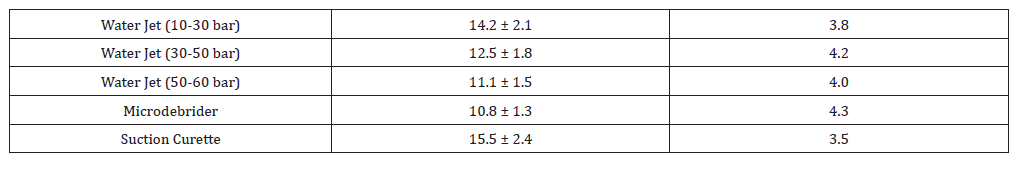
Comparable time efficiency with high satisfaction at midpressure range
Table 1:Tissue Removal Score (0-4).
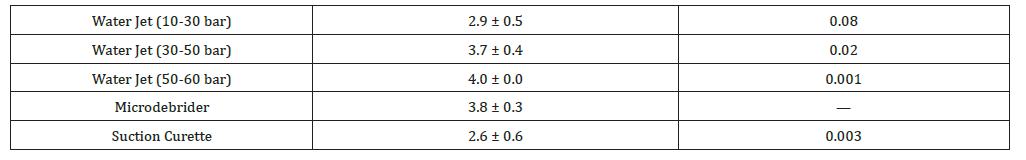
Table 2:Adjacent Structure Injury Score (0-3).
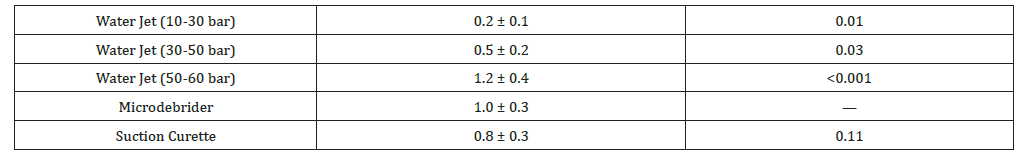
Table 3:Histopathological Damage Score (0-3).
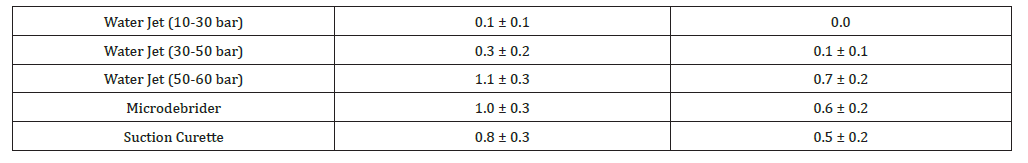
Table 4:Operative Time and Surgeon Satisfaction.

Discussion
This preclinical study demonstrates that a curved water jet system is effective and safe for tissue removal in challenging areas like the sphenoid sinus, frontal sinus, and skull base. It offers comparable tissue clearance to microdebriders while causing significantly less damage to surrounding structures, especially at lower pressures [4].
These findings align with previous reports in skull base and middle ear surgery where water jet dissection was shown to preserve nerves and vessels [5, 6]. Our results also support earlier work showing that pressures below 50 bar provide a favorable balance between efficacy and safety [7].
The curved design of the probe allowed better access to posterior, lateral and superior compartments, which are often poorly visualized and difficult to reach with straight instruments. However, we observed increased injury risk above 50 bar, reinforcing the need for careful pressure titration near sensitive anatomy.
Comparison with Similar Studies
Table 5:

Conclusion
A curved water jet system shows strong potential for selective, safe, and effective tissue removal in complex sinus and skull base surgery. Operating within a pressure range of 30-50 bar provides optimal outcomes with minimal structural damage. These findings support further clinical evaluation and integration into advanced endoscopic surgical platforms.
Conclusion
PLAI provides reliable data for healthy children of all ages and for children with OME. RF of the admittance and peak admittance were higher than those in healthy controls. Compared to tympanometry, PLAI achieved higher sensitivity and positive predictive values for diagnosing OME. Clinicians can use PLAI in combination with tympanometry for children with suspected OME when the diagnosis remains uncertain after performing or attempting otoscopy and pneumatic otoscopy.
Acknowledgment
None.
Conflict of Interest
No conflict of interest.
References
- Patel ZM, Adappa ND, Chiu AG (2021) Current practices and emerging technologies in endoscopic sinus surgery. Int Forum Allergy Rhinol 11(2): 189-199.
- Fritsch MH (2008) Endoscopic management of middle ear cholesteatoma using the water jet. Otol Neurotol 29(8): 1122-1129.
- Solares CA, Snyderman CH, Gardner PA (2011) The role of the water jet in endoscopic skull base surgery. Am J Rhinol Allergy 25(4): 235-239.
- Stolla F, Locketz MA, Roth K (2020) Evaluation of water jet dissection in endoscopic sinus surgery: an ex vivo model. Laryngoscope Investig Otolaryngol 5(1): 102-108.
- Kanda Y, Ohyama M, Takahashi H (2015) Selective dissection of skull base tumors using water jet in endoscopic transnasal approaches. Acta Otolaryngol 135(5): 493-500.
- Stolla F, Locketz MA, Roth K (2020) Evaluation of water jet dissection in endoscopic sinus surgery: an ex vivo model. Laryngoscope Investig Otolaryngol 5(1): 102-108.
- Solares CA, Snyderman CH, Gardner PA (2011) The role of the water jet in endoscopic skull base surgery. Am J Rhinol Allergy 25(4): 235-239.
- Fritsch MH (2008) Endoscopic management of middle ear cholesteatoma using the water jet. Otol Neurotol 29(8): 1122-1129.
-
Professor Hany Amin Riad M.D.*. Preclinical Evaluation of a Curved Water Jet System for Tissue Removal in Sphenoid Sinus, Frontal sinus, and Skull Base Surgery. On J Otolaryngol & Rhinol. 7(5): 2025. OJOR.MS.ID.000673
-
Sphenoid Sinus, Frontal sinus, Skull Base Surgery, Neurovascular structures, Middle ear surgery, Endoscopic surgical platforms, Complex sinus, Surgical tools
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






