 Case Report
Case Report
Mevalonate Kinase Deficiency with Normal IgD Levels Mimicking Recurrent Severe Infections: A Case Report and Mini Review of the Literature
Sonila Boriçi1,2* and Elisa Baci2
1Service of Pediatric Pulmonology and Allergy, UHC “Mother Teresa”, Tirana, Albania
2Pediatric Department, Albania
Sonila Boriçi, Service of Pediatric Pulmonology and Allergy, UHC Mother Teresa, Tirana, Albania.
Received Date: February 19, 2026; Published Date: February 24, 2026
Abstract
Background: Mevalonate kinase deficiency (MKD), historically termed Hyper-IgD syndrome (HIDS), is a rare autosomal recessive
autoinflammatory disorder caused by mutations in the MVK gene [1,2]. Normal IgD levels do not exclude the diagnosis and may contribute to
diagnostic delay [3,4].
Case Presentation: A 7-year-old boy was admitted with community-acquired pneumonia (cCAP) complicated by parapneumonic effusion.
Although he initially improved under broad-spectrum antibiotic therapy, new episodes of high fever, abdominal pain, mucositis, lymphadenopathy,
and splenomegaly developed. Inflammatory markers were markedly elevated while procalcitonin remained negative and cultures were sterile. IgA
was elevated, IgD normal. Corticosteroid therapy resulted in rapid improvement. Genetic testing confirmed compound heterozygous MVK mutations
(Leu315GlyfsX51 and Val377Ile), variants frequently associated with intermediate phenotypes [3]. Anakinra reduced attack frequency. The patient
later developed inflammatory bowel disease requiring mesalazine.
Conclusion: This case highlights the diagnostic challenge of differentiating autoinflammatory flares from bacterial infection and emphasizes
that normal IgD does not exclude MKD [3,4].
Introduction
Mevalonate kinase deficiency is caused by mutations in the MVK gene, leading to defective isoprenoid biosynthesis and dysregulated IL-1–mediated inflammation [2,5]. The phenotype ranges from mild periodic fever to severe mevalonic aciduria [6]. Although elevated IgD is classically associated with the disease [1], it lacks sensitivity and specificity, particularly in pediatric patients [3,4]. Clinically, MKD may closely resemble recurrent bacterial infections, frequently resulting in diagnostic delay [5,7].
Case Presentation
A 7-year-old boy was admitted for community-acquired pneumonia (cCAP) complicated by right-sided parapneumonic effusion. He presented with high fever (39–40°C), cough, and respiratory distress. Broad-spectrum antibiotic therapy (ceftriaxone and vancomycin) led to initial clinical improvement with reduction of fever and inflammatory parameters. However, during the second week of hospitalization, shortly before discharge, the patient developed a new febrile episode characterized by high temperature, severe abdominal pain, oral mucositis, cervical lymphadenopathy, and splenomegaly. This raised a critical diagnostic dilemma: was this a relapse or complication of bacterial infection, or an independent autoinflammatory flare?
Notably, blood and sputum cultures remained negative, and procalcitonin levels were within normal limits despite markedly elevated CRP and leukocytosis (Table 1). A detailed history revealed recurrent febrile episodes since the second day of life, occurring every 2–3 weeks, associated with lymphadenopathy, abdominal pain, rash, and hepatosplenomegaly.
Table 1:Laboratory Findings During Hospitalization.
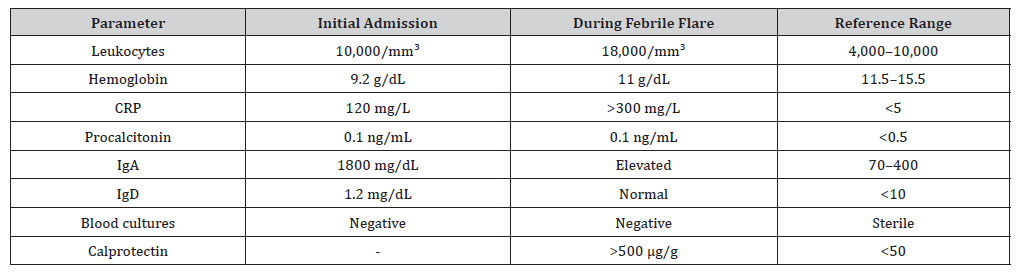
Immunological evaluation demonstrated elevated IgA levels but normal IgD concentrations. Given the periodic pattern, negative microbiological studies, and the systemic inflammatory phenotype, an autoinflammatory syndrome was suspected. Treatment with corticosteroids (1 mg/kg/day) resulted in immediate and dramatic clinical improvement. Genetic analysis revealed compound heterozygous MVK mutations (Leu315GlyfsX51 and Val377Ile), confirming MKD. Anakinra therapy was initiated with significant reduction in attack frequency. Subsequent evaluation revealed inflammatory bowel disease, managed with mesalazine alongside IL-1 blockade.
Table 2:Bacterial Infection vs Autoinflammatory Flare.
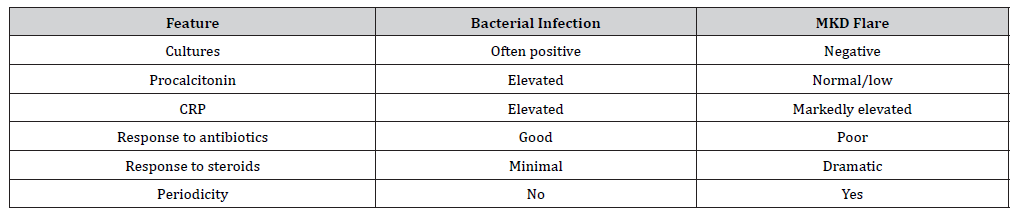
Discussion
This case illustrates the complex interplay between infectious and autoinflammatory processes in pediatric patients. The child was initially hospitalized for confirmed bacterial pneumonia (cCAP), a genuine infectious condition. However, the subsequent febrile episode during recovery represented an autoinflammatory flare rather than persistent infection.
Diagnostic delay is common in MKD due to clinical overlap with infectious diseases [5,7]. The differentiation between bacterial infection and autoinflammatory activation is clinically crucial. In bacterial infection, fever is typically accompanied by positive cultures and elevated procalcitonin levels, and responds consistently to antibiotic therapy. In contrast, autoinflammatory flares are characterized by recurrent sterile inflammation, markedly elevated CRP, negative cultures, normal or low procalcitonin, and dramatic response to corticosteroids or IL-1 blockade [8,9]. In our patient, the absence of microbiological evidence, normal procalcitonin, recurrence of systemic symptoms, and immediate steroid responsiveness strongly supported an autoinflammatory mechanism. Misinterpretation as ongoing infection could have resulted in prolonged unnecessary antibiotic exposure and delayed definitive diagnosis.
Normal IgD levels further complicated the diagnostic pathway. Although historically termed Hyper-IgD syndrome, normal IgD levels are well described in pediatric MKD and should not discourage genetic testing [3,4]. Recent genotype–phenotype analyses confirm that IgD elevation is not mandatory for diagnosis and may be absent in a significant proportion of children [3]. The Val377Ile mutation identified in this case is among the most commonly reported variants and is typically associated with intermediate phenotypes [3].
Gastrointestinal involvement, including Crohn-like inflammatory bowel disease, has been increasingly reported in MKD [10]. This likely reflects chronic IL-1–mediated inflammation and immune dysregulation [11,12]. IL-1 blockade remains the cornerstone of therapy and significantly reduces attack frequency and systemic inflammation [8,4,13]. Advances in molecular genetics and understanding of autoinflammatory pathways have improved diagnostic precision and targeted treatment strategies in recent years [11,12,14].
Conclusion
This case emphasizes the importance of differentiating autoinflammatory flares from bacterial infection in children with recurrent fever. MKD should be suspected in children with periodic fever, sterile inflammation, and negative procalcitonin, even in the presence of normal IgD levels [3,4]. Early genetic confirmation is essential for accurate diagnosis and appropriate targeted therapy [12,13,15].
References
- Drenth JP, van der Meer JW (2001) Hyperimmunoglobulinemia D syndrome. N Engl J Med 345: 1748-1757.
- Houten SM (1999) Mutations in MVK cause hyperimmunoglobulinemia D syndrome. Nat Genet 22: 175-177.
- Ter Haar NM (2021) Phenotype and genotype of MKD. Arthritis Rheumatol 73: 558-567.
- Federici S (2022) Evidence-based management of autoinflammatory diseases. Front Pediatr 10: 821699.
- Jeyaratnam J, Frenkel J (2020) Update on mevalonate kinase deficiency. Curr Opin Rheumatol 32: 484-492.
- Van der Hilst JC, et al. (2008) Long-term follow-up in MKD. Medicine (Baltimore) 87: 301-310.
- Ombrello MJ (2021) Advances in autoinflammatory diseases. Nat Rev Rheumatol 17: 225-237.
- Ter Haar NM (2018) Recommendations for management of autoinflammatory diseases. Ann Rheum Dis 77: 1706-1716.
- Ozen S, Bilginer Y (2020) Clinical guide to autoinflammatory diseases. Pediatr Clin North Am. 67: 563-578.
- Stojanov S (2023) Gastrointestinal involvement in MKD. Front Pediatr 11: 1183456.
- Papa R, Lachmann HJ (2022) Expanding spectrum of autoinflammatory diseases. Nat Rev Rheumatol 18: 513-528.
- Zhou Q, Aksentijevich I (2023) Genetic advances in autoinflammatory diseases. Nat Rev Rheumatol 19: 95-110.
- Ter Haar NM (2023) Long-term outcome and biologic therapy in MKD. Front Immunol 14: 1132456.
- Ozen S (2024) Autoinflammatory diseases: from bedside to bench. Lancet Rheumatol 6: e12-e24.
- Batu ED (2019) Periodic fever syndromes in children. Curr Rheumatol Rep 21: 45.
-
Sonila Boriçi* and Elisa Baci. Mevalonate Kinase Deficiency with Normal IgD Levels Mimicking Recurrent Severe Infections: A Case Report and Mini Review of the Literature. Glob J of Ped & Neonatol Car. 6(1): 2026. GJPNC.MS.ID.000629.
Syndrome, Bacterial infections, Fever, Antibiotic therapy, Diseases, Children, Pediatric
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






