 Research Article
Research Article
Comparison Between an External Fixator Model Developed to Fit Clavicle and Locking Plates for Displaced Middle Third Clavicle Fractures Treatment
Fábio Lucas Rodrigues1*, Edson Viriato Memória2 and Adriana Mendes Vanzin3
1 Orthopedic Doctor, Chief of the Trauma and External Fixation Group of the Orthopedics and Traumatology Service, linked to the Department of Locomotor System Diseases Brazil
2 Assistant Orthopedic Doctor of the Orthopedics and Traumatology Services linked to the Department of Locomotor System Diseases Brazil
3 Assistant Orthopedic Doctor of the Pediatric Group of the Orthopedics and Traumatology Service, linked to the Department of Locomotor System Diseases Brazil
Corresponding AuthorFábio Lucas Rodrigues, Orthopedic Doctor, Chief of the Trauma and External Fixation Group of the Orthopedics and Traumatology Service, linked to the Department of Locomotor System Diseases of the Faculdade de Medicina do ABC, Brazil.
Received Date:December 15, 2025; Published Date:December 23, 2025
Abstract
Fractures of the middle third of the clavicle have good outcomes with conservative treatment, but there are cases where significant displacement of fragments occurs, leading to an increase in the indication for surgical treatment. The aim of this study was to obtain a comparative mechanical analysis between an external fixator model developed for the clavicle and two models of plates with screws. Fifteen synthetic fracture models were used, equally divided into 3 Groups: 1, using reconstruction plate; 2, using locking plate; and 3, using external fixator for clavicle. Mechanical tests were performed comparing the resistance of the assemblies. In static four-point bending tests until assembly failure, it was evident that Group 2 showed the highest mean flexural rigidity (245.4 + 14.08), with Group 1 at (207.6 + 16.38) and Group 3 at (180.8 + 14.89), with a statistically significant difference (p = 0.003). The other tests were not significant. The tests performed were based on previous biomechanical studies, serving as a parameter for comparisons and conclusions. It was observed that there is no mechanical difference between the assemblies in axial compression and four17 point bending fatigue tests, however, the assembly with the locking plate was the most rigid and resistant to failure, corroborating literature data. The tested external fixator has properties similar to the plates used in terms of resistance to deformation and load supported, offering, however, less rigidity to the assembly.
Keywords:Biomechanics; Clavicle; Fracture; External Fixator; Surgical Treatment
Introduction
Fracture of the clavicle represents approximately 4% of all fractures, and in the young adult, it is among the most common, representing 5 to 16% of all cases. Its primary incidence (76%) is in the middle third of the bone [1, 2]. Traditionally, there is a tendency towards indicating the conservative treatment, since the low rate of pseudarthrosis reported in articles, about 1% [3-6, 2], makes it seem like an efficient treatment. However, current studies have shown substantially higher indices of this complication (around 15%) [7-9] when there is a large deviation among the fragments or shortening of the fracture site (>20mm), and when there is comminution or segmental fracture traces (Lazarus, 2006). Another complication is the high level of dissatisfaction related to factors such as pain, functional deficit, esthetic aspect, bone shortening, and decreased strength (25 -31%) [2, 6-8].
Considering these findings, currently there is a greater tendency towards indicating surgical treatment for displaced fractures of the middle third of the clavicle, with open reduction and plates or flexible rods [8, 10-13]. These treatments, however, are not exempt from complications. There are cases reported of migration of intramedullary pins, plate and screw failures, local infection, suture dehiscence, hypertrophic scars, unsatisfactory aesthetics, refracture, discomfort related to the synthesis material, and protrusion of the material through the skin [14].
One alternative fixation for the surgical treatment of the clavicle is external fixation, first described by Lambotte in 1905 and performed during the 1980s and 1990s [15-19]. There are few studies related to the application of this method, and its use is mostly restricted to cases of exposed fracture or when initially there was damage of the local soft tissues [17]. Since this is an exception technique, there is no external fixator with characteristics specific for the fixation of the clavicle, rather, only adaptations of models used in other anatomical regions. This hiatus led us to plan this biomechanical study in order to evaluate the properties of the external fixator model designed for application on the clavicle, and to compare it to the commonly used synthesis materials.
Material and Methods
Fifteen standardized bone models were used. These were divided randomly into three groups of five models. Each model was then sectioned transversely into two equal parts (10 cm each) and fixed, maintaining a 5-mm space between the fragments (Figure 1). In group 1, fixation was performed using a 6-hole acetabular reconstruction plate for small fragments (Figure 2) and six cortical screws; in Group 2, 3.5-mm 6-hole locking acetabular reconstruction plates (Figure 2) were used with six locking (blockhead) screws and two cannulated cortical screws. All the plates and screws used were stainless steel implants from the Wings Line (Biomecanica, Jaú, SP, Brazil); in Group 3, we used external fixators adapted for the clavicle (Figure 2), fastened with 6 3.5-mm pins and cannulated two cortical screws, with a total of 6 cortical screws in each fragment (Biomecanica, Jaú, SP, Brazil). Each model was submitted to three types of tests following the same sequence. The tests consisted of dynamic axial compression, four-point flexion, and four-point flexion fatigue. The load used was previously established in a pilot test.


For dynamic axial compression, standard testing equipment, Brasválvulas BME 5 120AT/MNB model was used, with 5 kN capacity and 500 N load cell. The bone models were placed between loading rollers and a support at a standardized distance (Figure 3), and compression tests were carried out along the axial axis of the assembly with a minimum load of 11.29 N and maximum load of 113 N, with a 10.0 Hz frequency; 9000 cycles were performed.
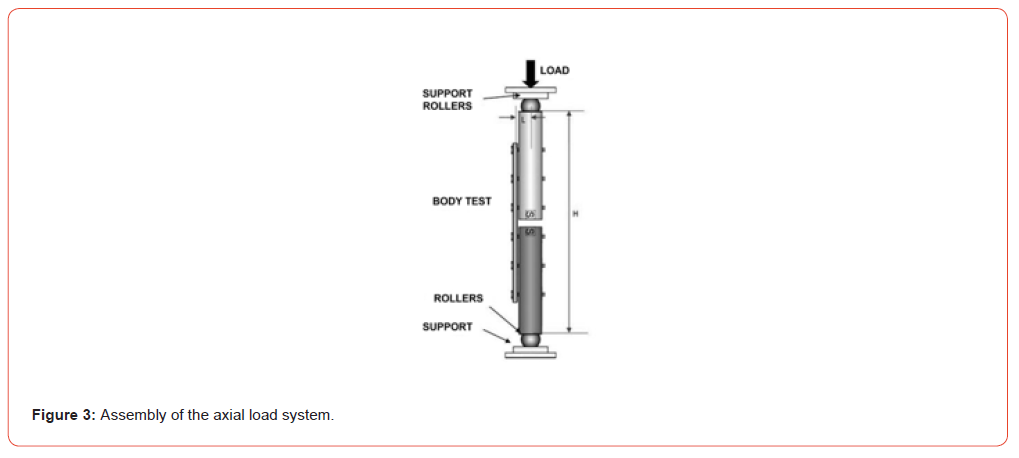
Next, fatigue tests were applied with four-point flexion, using standard Brasválvulas BME 5 120AT/MNB model testing equipment, with a 5 kN capacity and 1 kN load cell. The bone models were placed between loading rollers and a support at a standardized distance (Figure 4), and the tests were conducted with maximum load of 365 N, frequency of 10.0 Hz, and 9000 cycles.

Lastly, static flexion tests were carried out with four-point support, which would elevate the load until a failure in the assembly occurred in order to check the maximal load supported. Standard EMIC DL10000 model testing equipment was used (Figure 5), with a 100 kN capacity and load cell of 10 kN. The models were placed between the loading rollers and the support at a standardized distance (Figure 4) and tested with a progressive load at a rate of 5 mm/min until a failure in the assembly (Figure 6).
The results were grouped according to the assemblies. Statistical analysis was done using Epi Info version 3.5.2 and Spss version 16 programs, with values of means and standard deviation for crossing the variables with the nonparametric Kruskal-Walli’s test. The significance level adopted was p<0.05, along with a 95% confidence interval.


Results
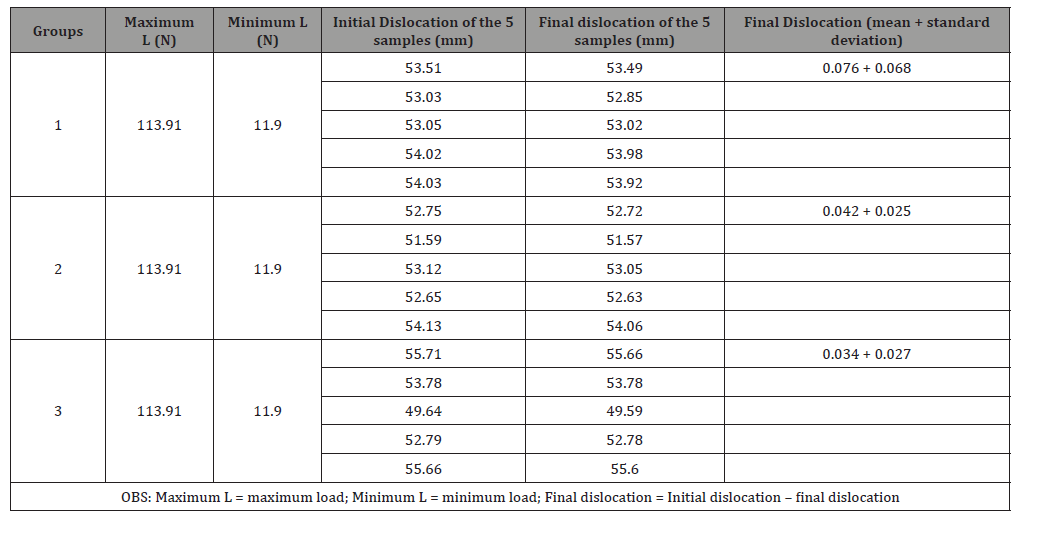
All the data are presented as means and 104 standard deviations (mean + standard deviation). In dynamic axial compression tests, the cyclic application of a maximum load of 113 N produced a greater mean dislocation in millimetres between the fragments of Group 1 (0.076 + 0.068), with (0.042 + 0.025) in Group 2 and (0.034 + 0.027) in Group 3; there was no statistically significant difference p=0.293) (Table 1). No catastrophic failure, such as cracks or release of the materials, was observed in any of the assemblies.
Table 1: Results of the axial compression tests on the 15 samples.
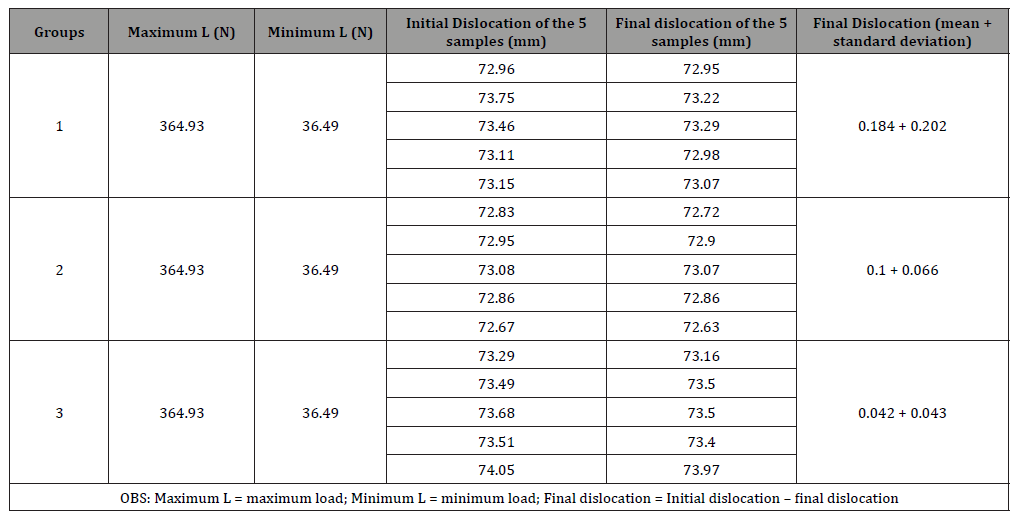
In the flexion tests with four support points, it was noted that the cyclic application of a maximum load of 365 N produced greater mean dislocation in millimetres among the fragments of Group 1 (0.184 + 0.202), in which (0.1 + 0.066) were in Group 3 and (0.042 + 0.043) in Group 2, with no statistically significant difference (p=0.236) (Table 2). No catastrophic failure was observed.
Table 2: Results of the flexion fatigue tests with four support points in the 15 samples.
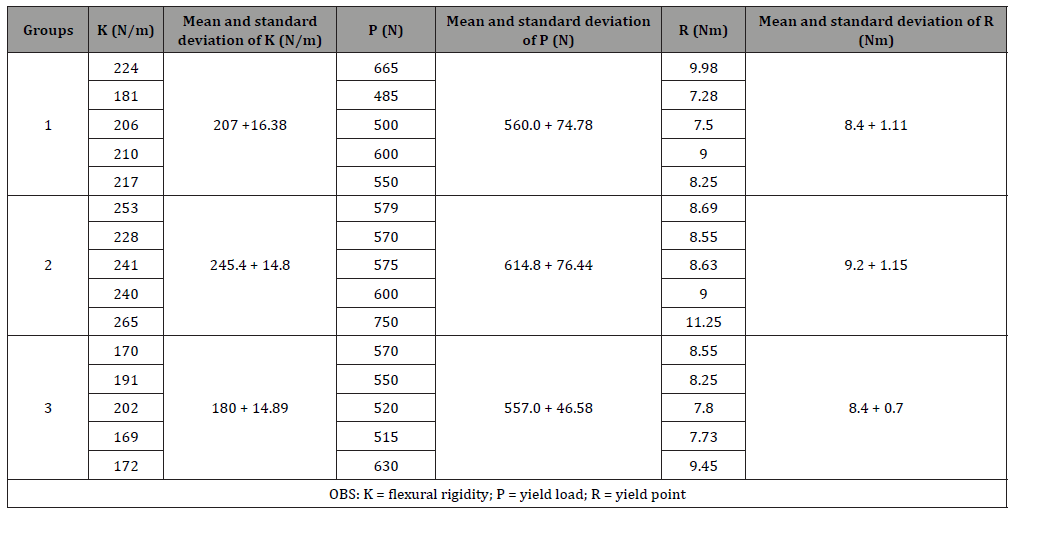
In the static flexion tests with four support points until failure of the assembly, it was evident that Group 2 showed the highest mean flexural rigidity (K values on Table 3) (245.4 + 14.08); in Group 1 (207.6 + 16.38) and in Group 3 (180.8 + 14.89), with a statistically significant difference (p=0.003). The greatest mean yield load (P values on Table 3) was noted in Group 2 (614.8 + 76.44), with (560.0 + 74.08) in Group 1 and (557.0 + 46.58) in Group 3, and no statistically significant difference (p=0.279). Also noted was a greater mean resistance to flexion (R values on Table 3) in Group 2 (9.2 + 1.15), with (8.4 + 1.11) in Group 1 and (8.4 + 0.7) in Group 3, and no statistically significant difference (p=0.279).
Table 3: Results of the flexion fatigue tests with four points of support in the 15 samples.
Discussion
For many years, there was a consensus that clavicular fractures were treated by a nonoperative method, and the discussion was as to the best type of immobilization [18]. After the work done by Hill et al. (1997), when functional limitations from a dislocated consolidated fracture became evident, the indication for surgical resolution increased. The most popular technique is absolute stability with plate and screws. However, in communitive fractures, this aggressive technique increases the chances of infected pseudarthrosis [7]. We believe that for this fracture the preferred method should be one of relative stability. The difficulty is in finding a synthesis material stable enough to maintain the reduction and suitable for application by a minimally invasive technique. The primary options are the bridge plate, the intramedullary wire, and the external fixator.
There are no national studies using external fixators for treatment of clavicle fractures, and the scarcity of international studies also motivated our research as to the beneficial potential of using this synthesis material. As positive points, we hope to offer a technique that is carried out quickly and simply, which is less invasive and easily removed, which would not cover the fracture site and hematoma, and would be capable of providing stability without excessive rigidity for secondary consolidation. With this, we desire to minimize damage to soft tissues and the discomfort related to the synthesis material, which constitute some of the main complications and complaints related to the surgical approach in these fractures (Lazarus, 2006).
There are no implants on the market with size, insertion angle, and thickness of the pins compatible with the shape of the clavicle. We developed a specific implant, and this study was carried out to evaluate the biomechanical resistance of this model of external fixator when compared to locked or conventional plates, seeking to offer another surgical treatment for fractures of the middle third of the clavicle with great displacement 156 or shortening (>20mm), comminution, or segmental fracture trace, which literature shows have an unfavourable outcome when treated by nonoperative methods (Lazarus, 2006). Our proposal was to observe if the external fixator tested would withstand loads similar to those of other synthesis methods, while offering less rigidity in order to allow micro movements at the fracture site, thus stimulating consolidation similar to what happens in nonoperative treatment, which in most cases has satisfactory results (Rowe, 1968; Crenshaw, 1992; Neer, 1960; Robinson, 2004; Brinker, 2005).
The types of synthesis materials used and the form of fixation of the models, as well as the assembly and sequence of tests performed followed what had previously been presented in other biomechanical studies, so they would serve as parameter for our comparisons and conclusions. For the axial compression tests, a maximum load of 113N was used, performing 9000 compression cycles. We used a smaller load that that of prior biomechanical studies that had used 500 N, but we performed 90 times more cycles. Our test represents an elevation of 10 Kg weight 100 times a day during 90 days, the period of rehabilitation of a patient with a fractured clavicle. Considering that the weight of the upper limb itself is around 100 to 150 N, the load used is representative. We noted that the assemblies using an external fixator showed smaller dislocation when compared to the plates, but with no statistically significant difference, and are, therefore, similar as to resistance to compression along the axial axis.
In the four-point cyclic flexion tests, we used a load of 365 N in 9000 cycles. The greatest deformity was found in Group 1, which used the conventional reconstruction plate, and the smallest in Group 2, which used locking plates, suggesting greater resistance of this type of plate, and was in agreement with literature data (Celestre, 2008). Nevertheless, there was no statistically significant difference, and the assemblies had similar mechanical properties when flexed with four support points. The four-point linear flexion tests until failure of the material revealed that assemblies of Group 2, using locking plates, displayed greater flexural rigidity when compared to the assemblies using our model of external fixator. Such data corroborate the literature data that show that the locking 189 plate has greater rigidity in its assembly (Celestre, 2008).
Failure of the assemblies happened, in all cases, at the transition between the screws, and sometimes a longitudinal fracture trace was noted along the axis of the bone model and the fixation holes (Figure 7). This differs from literature data that showed greater rates of breakage due to failure of the plate at the site of the bone failure or due to fracture at the hole of the last screw, at the extremity of the plate (Celestre, 2008). This must be a result of the type of assembly and the orientation of the force applied during the linear flexion test until failure of the material. In prior projects, the force of flexion had been applied perpendicularly to the plane of the plate surface, while in our tests, the position of the plate towards the bone and in its spatial orientation was respected when applied to the patient, in whom the plane of the plate surface would coincide with the coronal plane of the patient’s body on the anterior surface of the bone. The force applied in this way is tangent to the plane of the plate surface, and can thus justify the pattern of failure found. Such a position was chosen since it is the only one viable for the use of the external fixator on the patient.

Criticism pertinent to this study and other biomechanical studies is their “in vivo” reproducibility, since the properties of live bone are varied. Some prior studies used cadaver bones, and even these studies received criticism as to alterations in the properties of these bones, and had great variability in the shapes and sizes of the bones. Our models were cylindrical compounds with 20 cm in length, with a 1-mm thin layer of polyurethane and a 3-mm layer of spongy plastic compound, simulating medullary bone. They had an internal canal with 6 mm in diameter, simulating the medullary canal. This type of model was preferred since it more faithfully reproduces the properties of real bone. Clavicle models available in our country are made of solid material, and are, therefore, less similar to real bone. Reproducibility is lost when one considers that the clavicle is an “S”-shaped bone, and that the synthesis materials would need to be molded, which could modify their mechanical properties. This study, however, tests the three synthesis materials under equal conditions, allowing variables such as molding, shape, and size of the bone, and the position of these materials on the bone to be eliminated, increasing reliability in the comparison.
Conclusion
The external fixator model tested has mechanical properties similar to those of conventional small fragment reconstruction plates and small fragment locking reconstruction plates regarding resistance to deformity and to the load supported, offering, however, less rigidity to the assembly.
Author contributions
The authors equally contributed.
Conflict of Interest
The authors declare no conflict of interest.
References
- Nordqvist A, Petersson C (1994) The incidence of fractures of the 304 clavicle. Clin Orthop Relat Res (300): 127-132.
- Robinson CM, Court-Brown CM, McQueen MM (2004) Wakefield AE. Estimating the risk of nonunion following nonoperative treatment of a clavicular fracture. J Bone Joint Surg Am. 86(7): 1359-1365.
- Rowe CR (1968) An atlas of anatomy and treatment of midclavicular fractures. Clin Orthop Relat Res 58: 29-42.
- Crenshaw AH (1992) Fractures of the shoulder girdle, arm and forearm. In: Crenshaw AH, editor. Campbell's operative orthopaedics. 8th edition. St. Louis (MO): Mosby-Yearbook Inc p. 989–995.
- NEER CS 2nd (1960) Nonunion of the clavicle. J Am Med Assoc 172: 1006-11.
- Brinker MR, Edwards TB, O'Connor DP (2005) Estimating the risk of nonunion following nonoperative treatment of a clavicular fracture. J Bone Joint Surg Am 87(3): 676-677.
- McKee MD, Schemitsch EH, Stephen DJ, Kreder H, Yoo DJ, et al. (1999) Functional Outcome Following Clavicle Fractures in Polytrauma Patients. Journal of Trauma-injury Infection and Critical Care 47(3): 616.
- Hill JM, McGuire MH, Crosby LA (1997) Closed treatment of displaced middle-third fractures of the clavicle gives poor results. J Bone Joint Surg Br 79(4): 537-539.
- Nordqvist A, Petersson CJ, Redlund-Johnell I (1998) Mid-clavicle fractures in adults: end result study after conservative treatment. J Orthop Trauma 12(8): 572-576.
- Nowak J, Holgersson M, Larsson S (2005) Sequelae from clavicular fractures are common: a prospective study of 222 patients. Acta Orthop 76(4): 496-502.
- Chu CM, Wang SJ, Lin LC (2002) Fixation of mid-third clavicular fractures with knowles pins: 78 patients followed for 2-7 years. Acta Orthop Scand 73(2): 134-139.
- Chuang TY, Ho WP, Hsieh PH, Lee PC, Chen CH, et al. (2006) Closed reduction and internal fixation for acute midshaft clavicular fractures using cannulated screws. J Trauma 60(6):1315-20.
- Shen WJ, Liu TJ, Shen YS (1999) Plate fixation of fresh displaced midshaft clavicle fractures. Injury 30(7): 497-500.
- Lazarus MD (2006) Fraturas da clavícula. Rockwood e Green: fraturas em adultos –ed. Barueri SP: Manole 1(5a): 1041-1078.
- Schuind F, Pay-Pay E, Andrianne Y, Donkerwolcke M, Rasquin C, et al. (1988) External fixation of the clavicle for fracture or non-union in adults. J Bone Joint Surg Am 70(5): 692-695.
- Bernal González M de J, Álvarez Cambras R, Cabrera Viltres N, Álvarez Placeres L (1999) Fractura de clavícula con minifijador externo RALCA. Rev Cubana Ortop Traumatol 13(1-2): 73-76.
- Celestre P, Roberston C, Mahar A, Oka R, Meunier M, et al. (2008) Biomechanical evaluation of clavicle fracture plating techniques: does a locking plate provide improved stability? J Orthop Trauma 22(4): 241-247.
- McKee MD (2010) Clavicle fractures in 2010: sling/swathe or open reduction and internal fixation? Orthop Clin North Am 41(2): 225-31.
- Wang XH, Guo WJ, Li AB, Cheng GJ, Lei T, et al. (2015) Operative versus nonoperative treatment for displaced midshaft clavicle fractures: a meta-analysis based on current evidence. Clinics 70(8): 584-592.
-
Fábio Lucas Rodrigues*, Edson Viriato Memória and Adriana Mendes Vanzin. Comparison Between an External Fixator Model Developed to Fit Clavicle and Locking Plates for Displaced Middle Third Clavicle Fractures Treatment. Glob J Ortho Res. 5(3): 2025. GJOR. MS.ID.000613..
-
Biomechanics, Clavicle, Fracture, External Fixator, Surgical Treatment, Clavicular Fractures, Shoulder Girdle Biomechanics, External Fixation, Fracture Stabilization, Surgical Management, Orthopedic Trauma, Bone Healing
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






