 Case Report
Case Report
Acute Lung Injury Following Cement Inhalation-A Case Report
Babar Dildar*, Arisha Babar and Muhammad Noor
Manchester University NHS Foundation Trust, UK
Babar Dildar, Manchester University NHS Foundation Trust, UK.
Received Date: March 08, 2021; Published Date:April 01, 2021
Abstract
Inhalational lung injuries caused by heat, smoke, or chemical irritants are described as causing pulmonary toxicity, ranging from upper airway symptoms to acute respiratory distress syndrome. We are reporting a case of a 25 years old man with accidental massive cement dust inhalation, who developed diffuse lung injury and hypoxic respiratory failure along with skin and mucosal injuries. Management of such cases is challenging in the absence of clinical guidelines. This patient responded well to steroids, antibiotics and supportive care. To the best of our knowledge, effects of acute massive cement dust inhalation have not been reported in English literature so far.
Keywords:Inhalation injury; Acute respiratory failure; Cement dust
Introduction and Background
Inhalation lung injury is commonly caused by accidental or occupational exposure to noxious gases, mists, aerosols, or particle dusts. The degree of lung injury is variable and is dependent on chemical properties of inhaled irritants, the magnitude of exposure, and individual host factors. An inhalational injury may affect respiratory epithelium from proximal to distal airways and may result in tracheitis, bronchitis and/or alveolitis. Absorption in the blood may result in systemic toxicity [1,2].
With the rapid growth of industries, the incidence of occupational lung diseases related to acute or chronic irritant exposure has been increased. Rhinitis, chronic obstructive pulmonary disease, and pneumoconiosis are well-known respiratory consequences of chronic exposure to particle dust [3- 5]. Numerous irritants can lead to acute inhalational injury but little is known about the consequences of exposure to individual substances. Consequences of acute inhalation injuries from smoke inhalation and thermal injuries are common [1,2]. Exposure to hazardous dust in survivors of World Trade Center attack of 2001 in New York City was extensively studied and shown significant association with high incidence of asthma and other respiratory diseases [6].
Portland cement is the most widely used cement in the construction industry worldwide. Fine particulate cement dust is composed of minerals of calcium with silica, aluminum, and iron [7]. Data regarding the effect of acute occupational dust (including cement) inhalation is very limited and mainly comprises of few case reports [8-10].
Case History
25 years old man, cement factory worker with unremarkable past medical history, was brought to emergency department* after being trapped under heaps of cement near a crusher for 40 minutes. He was dyspneic, drowsy and irritable, coated with cement head to toe, oozing frothy secretions from the mouth. Oxygen saturation was 58% on ambient air, pulse 156/min, blood pressure 136/84mmHg, and respiratory rate 30/min. On examination, there were bilateral corneal opacities and minor burn marks on feet and legs (Figure 1). On chest auscultation, he had scattered wheezing and fine crackles. Cardiac and abdominal examination was unremarkable. Chest radiograph showed bilateral alveolar opacities (Figure 2). Arterial blood gas values with (high flow oxygen) were: pH 7.13, PaCO2 37.4mmHg, PaO2 61.6 mmHg.
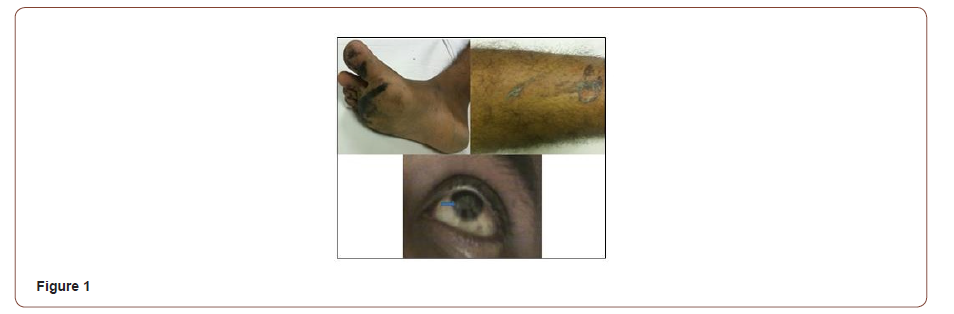
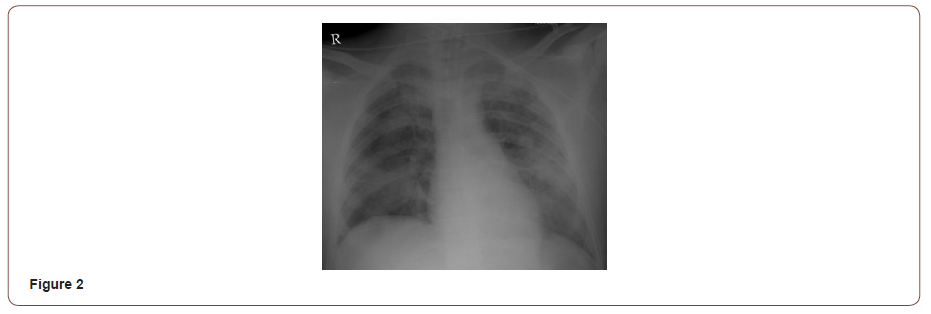
Bicarbonate 12.7mmol/L; Hemoglobin14.6gm/dl, Hematocrit 44.6%, Total Leukocyte Count 23,310/mm3, Urea 33mg/dl and Creatinine 1.5mg/dl. Patient was intubated and placed on the mechanical ventilator. Intravenous fluids, bronchodilators piperacillin-tazobactum, and methylprednisolone (1.5mg/kg) were started. Fiberoptic bronchoscopy showed diffuse erythema and greyish/white patches bilaterally (Figure 3) corresponds to moderate to severe grade injury as per abbreviated injury score (AIS) criteria [11].
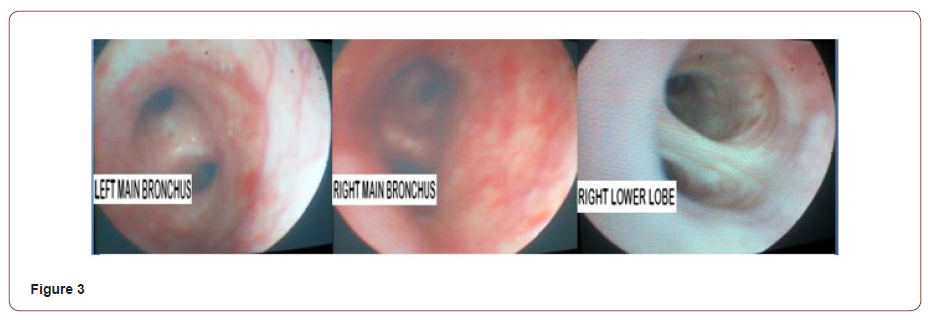
Bronchoalveolar lavage smear showed neutrophils (75%), foamy histiocytes (20%), lymphocytes (4%) and occasional macrophages containing black pigment in a hemorrhagic background. Hemodynamics and conscious level improved gradually, so did the laboratory parameters and chest X-ray opacities. Patient was weaned off from mechanical ventilation after 60 hours. Tracheal aspirate culture grew Staphylococcus aureus and Pseudomonas aeroginosa, sensitive to piperacillin/tazobactam which continued for one week. Methylprednisolone changed to oral prednisolone and tapered over two weeks which corresponds to his clinical recovery. Small areas of skin burns and superficial ocular injury responded well to supportive care.
Our patient was found to be symptom-free at 4 weeks follow up along with complete resolution of chest X-ray opacities (Figure 4). *Patient was admitted and managed in Memon Medical Institute Hospital, Karachi, Pakistan.
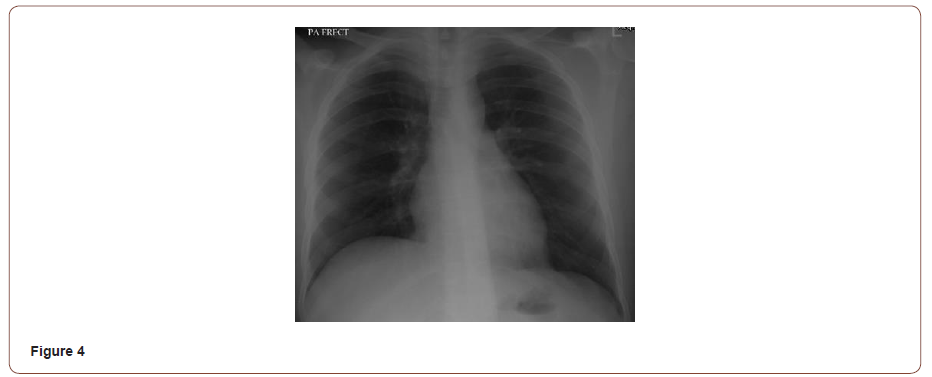
Discussion
Severe inhalation injury is usually associated with high mortality due to direct effect on airways and lung parenchyma leading to impairment in gas exchange and asphyxsia [1]. Clinical manifestations of inhalational injury depends on solubility, particle size and amount of irritant exposure. Highly soluble substances deposit in the nose, upper airway and up to larger bronchi whereas less soluble substances usually deposits in small airways and alveoli. Increased level of exposure to highly soluble substances like cement dust, can cause both upper and lower airway injury [12]. Particles in size greater than 10μm, deposit in the nose; between 5 to 10μm in large airways and<5μm deposit in small airways and alveoli. The particle size of cement dust ranges from 0.05 to 5μm, and mainly affects distal airways and alveoli but in higher exposure it can deposit in the entire respiratory tract [13,14].
When the mucous membranes of respiratory tract are exposed to cement, it results in severe alkaline reaction with pH of 12.0 to 13 and causes tissue damage by denaturing proteins and collagen, dehydrating cells, and saponifying fat. It also causes injury to skin and eyes [15-18]. Non-cardiogenic pulmonary edema may result from pulmonary capillary damage and subsequent transudation of fluid into the alveoli. The onset may be within minutes or hours, after the exposure. Persistent hypoxemia is associated with a higher mortality rate. In addition to duration and extent of exposure, the patient’s underlying respiratory status may affect the clinical response [10,19].
In addition to conventional critical care severity assessment tools, the extent of endobronchial injury can be assessed bronchoscopically by abbreviated injury score (AIS) criteria. AIS criteria grades mucosal injury on bronchoscopic examination from grade 0 (no injury) to grade 4 (massive injury). Hasan Z, et al. [20] described a significant correlation between the degree of inhalation injury on bronchoscopy and mortality, in patients with thermal injuries [20]. Impaired local and probable systemic immune function has been postulated to result from number of mechanisms; including loss of protective ciliary action in respiratory epithelium, enhanced pulmonary leukocyte activity, pronounced alveolar neutrophilia and bacterial overgrowth, which predispose to pneumonia [11]. Evidence of pneumonia was seen in our patient and reported in another case of cement dust inhalation, which was published in Swiss medical forum [9].
Presence of predominant neutrophilic inflammatory cells in bronchoalveolar lavage fluid, moderate to severe endobronchial injury (according to AIS criteria), and hypoxemia revealed the severe nature of inhalational injury in our patient. Despite a controversy of glucocorticoid use in ARDS, early ARDS has been shown to speed up clinical improvement and reduce hospital mortality in recent literature [21]. The decision to give steroids in our patient was made due to the presence of bronchospasm, inflammatory nature of lung injury and features of severe acute respiratory distress syndrome.
Our patient responded well to supportive treatment along with steroids and antibiotics. Further studies are required to confirm the beneficial effect of steroids and empirical antibiotics in acute inhalational injury. Clinical approach to inhalational injury comprises airway protection, ventilatory and hemodynamic support, high flow oxygen, bronchodilators and chest physiotherapy. Patients with ARDS, requiring mechanical ventilation, should be managed by lung protective ventilation [1]. Patients should be monitored for systemic toxicity and multi-organ dysfunction. For patients with moderate to severe inhalation injury, we recommend an early assessment with bronchoscopy to evaluate the extent of mucosal involvement.
Acknowledgement
None.
Conflict of Interest
No conflict of interest.
References
- Gorguner M, Akgun M (2010) Acute inhalation injury. Eurasian J Med 42(1): 28-35.
- Keith A Lafferty KA, Bonhomme K, Martinez CV, Wiener SW, Serebrisky D, et al. (2018) Smoke Inhalation Injury.
- Neghab M, Choobineh A (2007) Work-related respiratory symptoms and ventilatory disorders among employees of a cement industry in Shiraz, Iran. J Occup Health 49: 273-278.
- Nordby KC (2011) Exposure to thoracic dust, airway symptoms and lung function in cement production workers. Eur Respir J 38(6): 1278-1286.
- Karkhanis V, Joshi JM (2011) Cement dust exposure-related emphysema in a construction worker. Lung India 28(4): 294-296.
- Alper HE, Yu S, Stellman SD, Brackbill RM (2017) Injury, intense dust exposure, and chronic disease among survivors of the World Trade Center terrorist attacks of September 11, 2001. Inj Epidemiol 4(1): 17.
- Barron Andrew R (2010) Chemical Composition of Portland Cement. OpenStax-CNX module: m16445.
- Gilomen S, Brack T, Klinik M, Glarus K (2012) Cement accident with severe consequences. Swiss Medical Foru 12(26): 539-541.
- Brun P, Kunz A, Funke M (2013) Buried under gypsum powder-A rare respiratory complication. Respir Med Case Rep 8: 36-39.
- Morin AM, Zahringer J, Kasper M, von Schmadel E, Suhayda A (1997) Acute respiratory insufficiency after inhaling concrete dust--a case report. Anasthesiol Intensivmed Notfallmed Schmerzther 32(1): 56-60.
- Albright JM, Davis CS, Bird MD, Ramirez L, Kim H, et al. (2012) The acute pulmonary inflammatory response to the graded severity of smoke inhalation injury. Crit Care Med 40(4): 1113-1121.
- Glazer CS (2003) Acute Inhalational Injury. In: Hanley ME, Welsh CH (eds.) Current Diagnosis & Treatment in Pulmonary Medicine. International (Edn.), New York: Mc-Graw Hill, Pp: 354-360.
- (1999) Hazard Prevention and Control in the Work Environment: Airborne Dust (WHO, 1999) WHO/SDE/OEH/99.14.
- Heyder J, Gebhart J, Rudolf G, Schiller CF, Stahlhofen W (1986) Deposition of particles in the human respiratory tract in the size range 0.005-155. Journal of Aerosol Science 17: 811-825.
- (2006) Portland Cement Dust- Hazard assessment document. UK Health and Safety Executive (HSE).
- Coumes CCD, Courtois S, Nectoux D, Leclercq S, Bourbon X (2006) Formulating a low-alkalinity, high-resistance and low-heat concrete for radioactive waste repositories. Cement and Concrete Research 36(12): 2152-2163.
- Catalano F, Mariano F, Maina G, Bianco C, Nuzzo J, et al. (2013) An unusual case of extensive self-inflicted cement burn. Ann Burns Fire Disasters 26(1): 40-43.
- Peters WJ (1984) Alkali burns from wet cement. Can Med Assoc J 130(7): 902-904.
- Gregoretti C, Decaroli D, Stella M, Mistretta A, et al. (2007) Management of Blast and Inhalation Injury. Breathe 3(4): 364-373.
- Hassan Z, Wong JK, Bush J, Bayat A, Dunn KW (2010) Assessing the severity of inhalation injuries in adults. Burns 36(2): 212-216.
- Meduri GU, Bridges L, Shih MC, Marik PE, Siemieniuk RAC, Kocak M (2016) Prolonged glucocorticoid treatment is associated with improved ARDS outcomes: analysis of individual patients' data from four randomized trials and trial-level meta-analysis of the updated literature. Intensive Care Med 42(5): 829-840.
-
Babar Dildar, Arisha Babar, Muhammad Noor. Acute Lung Injury Following Cement Inhalation-A Case Report. Anaest & Sur Open Access J. 2(4): 2020. ASOAJ.MS.ID.000542.
-
Pulmonary toxicity, Mucosal injuries, Lung parenchyma, Respiratory tract, Chest physiotherapy, Multi organ dysfunction, Mucosal involvement, Lung injury.
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






