 Research Article
Research Article
An Intervention to Build Hope
Karin Richards*
Department of Kinesiology, University of the Sciences, Philadelphia, USA
Karin Richards, Department of Kinesiology, University of the Sciences, Philadelphia, USA.
Received Date: August 12, 2021; Published Date: August 20, 2021
Abstract
The purpose of the study was to determine if brief, ten-minute stress management exercises held at the beginning of class impacted the levels of hope in university students during months 10-13 of a pandemic, including national and international lockdowns, social distancing and mandated online learning. A repeated-measures multivariate analysis of variance (MANOVA) was conducted to determine if there were differences between groups on the pretest and posttest measures of temporality, positive readiness, and interconnectedness. While not statistically significant, the experimental group increased their aggregate levels of hope while the control group experienced a slight decrease in hope. Brief, incremental activities, even done online, resulted in improved perceptions and feelings of hope.
Keywords: COVID; hope; mental health; students
Introduction
Resiliency can be favorably preferred as a character trait when an individual is experiencing hardship [1,2] Overcoming those hardships, potentially faced with obstacles, has been suggested to develop an individual’s physical and mental strength and flexibility when facing future challenges [1]. Yet to build an individual’s resilience, that person must also have hope [1-4]. An individual who has hope, therefore, may be defined as thinking of new favorable possibilities, while planning and acting for improved conditions than what an individual is experiencing [2-4]. During the 2020-2021 COVID pandemic and racial unrest in the United States, individuals, especially college students, struggled with their mental health and how to maintain hope [5-9]. After many months which turned into over a year of social isolation, worry, and despair, it is suggested students may still not have the resources or knowledge to adequately cope with the post-pandemic life [8-10]. The methods for building hope, however, are not clearly defined for each individual. Literature has included suggestions to increase hope such as teaching students executive functioning training; social and emotional learning; engaging in journaling, meditation, breathing techniques, and visualization [9,11-15]. This study sought to measure the levels of hope in first year university students in the beginning and at the conclusion of the spring semester to determine if interventions, delivered online during a pandemic, would impact the aggregate concentration of hope among students.
Materials and Methods
Twenty first-year university students completed the 12- item, Likert Scale, Herth Hope Index questionnaire in a pre and posttest evaluation.16 The amount of hope in an individual was calculated by totaling the scores of the 12 items, (values ranging from 1-4) [16]. The higher the total, the greater the concentration of hope.16 Aggregate levels of hope and among the constructs of temporality and future; positive readiness and expectancy; and interconnectedness with self and others were evaluated in the control (n=10) and experimental (n=10) groups.16 Students were randomly assigned to the experimental and control groups. The experimental group participated in 10 minutes of hope building exercises once per week prior to the start of their second semester orientation class. These exercises were comprised of journaling; breathing techniques; self-Reiki; tapping; visualization; and meditation. Descriptive statistics were completed for the central tendencies for each of the two groups utilizing the Statistical Package for Social Sciences (Version 26). Composite scores were computed for the constructs of temporality, positive readiness, and interconnectedness at both the pretest and posttest by summing the items corresponding to each construct. A repeated-measures multivariate analysis of variance (MANOVA) was conducted to determine if there were differences between groups on the pretest and posttest measures of temporality, positive readiness, and interconnectedness. Normality was assessed by inspection of normal Q-Q plots of the residuals for each dependent variable (Figures 1-6).
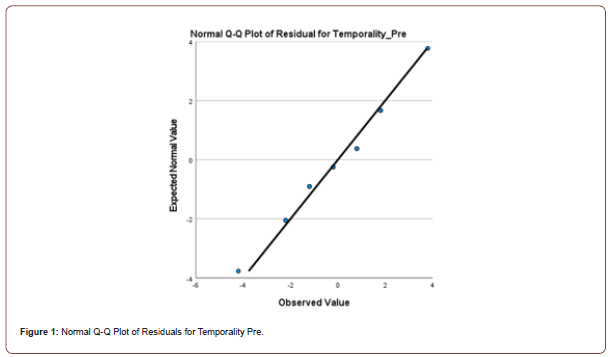
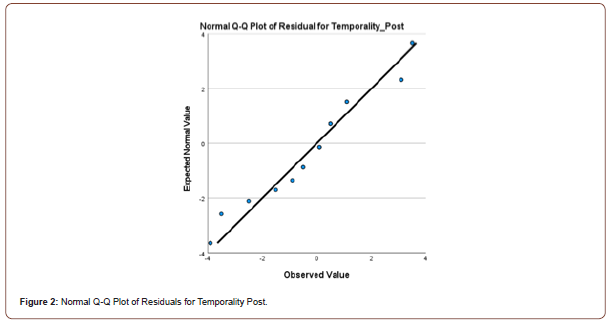
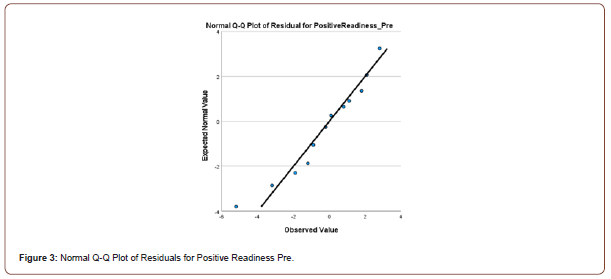
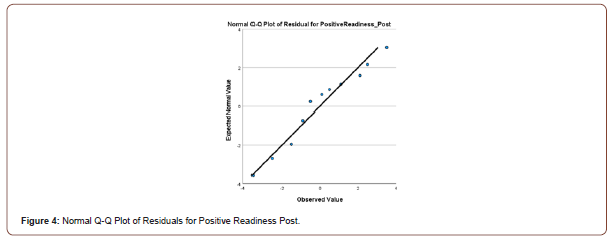
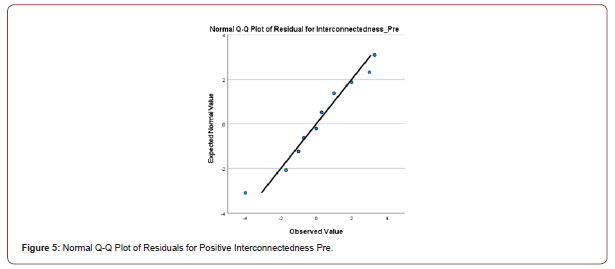
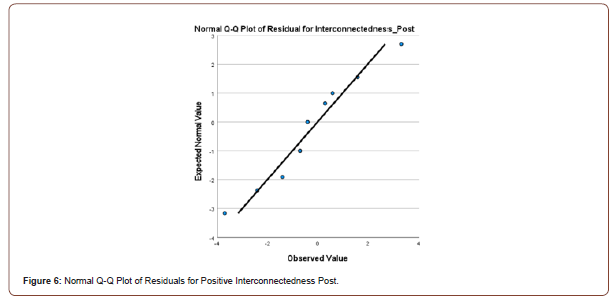
Homogeneity of variance and covariance were assessed through Levene’s tests and Box’s M tests, respectively. To determine if there were differences in the levels of temporality, positive readiness, and interconnectedness on the pretest and the posttest, a repeated measures analysis of variance (ANOVA) was conducted. The assumption of sphericity was assessed using Mauchly’s test.
Results and Discussion
There was little deviation from the normal line of the Q-Q plots of the residuals for each dependent variable, indicating that the assumption of normality was met. The Levene’s and Box’s M tests were not significant (all p-values > .05), indicating that the assumptions homogeneity of variance and covariance were also met.
The Pillai’s Trace multivariate test for group was not significant, F (3, 16) = 0.10, p = .960, indicating that there were no significant differences between Group 1 and Group 2 on the measures of temporality, positive readiness, and interconnectedness. The Pillai’s Trace multivariate test for time was not significant, F (3, 16) = 3.15, p = .054, indicating that there were no significant differences between the pretest and posttest on the measures of temporality, positive readiness, and interconnectedness. The Pillai’s Trace multivariate test for the group x time interaction was not significant, F (3, 16) = 0.62, p = .610, indicating that there were no significant differences between the pretest and posttest on the measures of temporality, positive readiness, and interconnectedness that depended on group.
(Table 1) displays means and standard deviations for the dependent variables by group and time. The Mauchly’s test for the pretest was significant (p = .002), indicating that the results of the ANOVA should be interpreted with a correction for non-sphericity (i.e., Greenhouse-Geisser). The results of the ANOVA with the Greenhouse-Geisser correction were significant, F (1.34, 25.43) = 10.78, p = .001, indicating that there were differences in the levels of temporality, positive readiness, and interconnectedness on the pretest. Pairwise comparisons revealed that positive readiness scores (M = 13.05, SD = 2.04) were significantly higher than temporality scores (M = 11.20, SD = 2.02, p = .001) and interconnectedness scores (M = 11.85, SD = 1.66, p < .001).
Table 1: Descriptive Statistics for Temporality, Positive Readiness, and Interconnectedness by Group and Time.
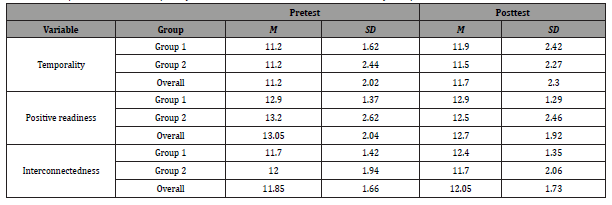
The assumption of sphericity was not significant (p = .092), indicating that the results of the ANOVA may be interpreted with sphericity assumed. The results of the ANOVA were significant, F (2, 38) = 5.69, p = .007, indicating that there were differences in the levels of temporality, positive readiness, and interconnectedness on the posttest. Pairwise comparisons revealed that positive readiness scores (M = 12.70, SD = 1.92) were significantly higher than temporality scores (M = 11.70, SD = 2.30, p = .005) and interconnectedness scores (M = 12.05, SD = 1.73, p = .008).
While not statistically significant, the construct of temporality, (positive outlook towards life; having goals; future fears and a day’s potential), did improve on both the experimental and control groups. Having a particular instructor or topic related discussion may have contributed to this increase in both of the groups. However, the construct of positive readiness, (seeing possibilities; ability to recall joy; life direction; life worth), remained the same in the experimental group and actually decreased in the control group. Finally, the construct of interconnectedness, (feeling alone; comforting faith; inner strength and love), increased in the experimental group and decreased in the control group. Overall levels of hope in the experimental group ranged from 33-42 (mean of 35.8) in the pretest and increased to a range of 32-44 (mean of 37.2) in the posttest. The control group experienced a decrease in the overall levels of hope. Pretest scores ranged from 23-43 (mean of 36.4) with posttest scores ranging from to 25-46 (mean of 35.7).
This study contains possible limitations. The small size of the convenience sample as well as the online environment in which the intervention occurred during this study limits the ability to generalize the results to the population.17 Additional limitations of the study include self-reported data bias, random error in scoring of the results and potential cultural bias of the topic [17].
This study was small in scope and while not statistically significant, the results suggest incremental activities, even done online, improved students’ perceptions and feelings of hope in their outlook of the present moment as well as the future. Additionally, aggregate levels of hope increased in the experimental group who participated in activities of meditation, journaling, self-Reiki, tapping, breathing techniques and other positive focused activities.
Conclusion
Future research could be conducted using one method of building hope and stress management with a larger subject population to evaluate the effectiveness of the specific technique. Additional research could include the impact of online exercises compared to in-person exercises. Qualitative research may also benefit future studies of hope building exercises.
Acknowledgement
None.
Conflict of Interest
No conflicts of interest.
References
- Rutter M (2012) Resilience as a dynamic concept. Dev Psychopathol 24(2): 335-344.
- American Psychological Association (2020) Building your resilience.
- Snyder CR (1994) The psychology of hope: You can get there from here. New York NY: Simon and Shuster
- Frederickson B (2009) Why choose hope: The choice of hope over fear is vital. Psychology Today.
- Milligan S (2020) Pandemic, recession, unrest: and the confluence of crises. US News and World Report.
- Panchal N, Kamal R, Cox C, Garfield R (2021) The implications of COVID-19 for mental health and substance use. Kaiser Family Foundation.
- Son C, Hegde S, Smith A, Wang X, Sasangohar F (2020) Effects of COVID-19 on college students’ mental health in the United States: Interview survey study. Journal of Medical Internet Research 22(9): 21279.
- Lumpkin L (2021) A mental health crisis was spreading on college campuses. The pandemic has made it worse. The Washington Post.
- Krislov M (2021) I’m worried about student mental health post-pandemic-Here’s how we can help. Forbes.
- Villani L, Pastorino R, Molinari E, et al. (2021) Impact of the COVID-19 pandemic on psychological well-being of students in an Italian university: a web-based cross-sectional survey. Global Health 17: 39.
- Chahal R, Kirshenbaum JS, Miller JG, Ho TC, Gotlib IH (2020) Higher executive control network coherence buffers against puberty-related increases in internalizing symptoms during the COVID-19 pandemic. Biol Psychiatry Cogn Neurosci Neuroimaging 6(1): 79-88.
- Sweeney S, Kirby K, Armour C, Goetzel K, Dunne M, et al. (2019) The Efficacy of Hopeful Minds: Can teaching Hope improve well-being and protective factors in child and early adolescent groups. International Foundation for Research and Education on Depression White Paper.
- Goodman J (2004) The anatomy of hope. The Permanente Journal 8(2): 43-47.
- Berg CJ, Ritschel LA, Swan DW, An LC, Ahluwalia JS (2011) The role of hope in engaging in healthy behaviors among college students. Am J Health Behav 35(4): 402-415.
- Goetzke K (2020) The biggest little book on hope. Innovative Analysis, LLC.
- Herth K (1992) Abbreviated instrument to measure hope: development and psychometric evaluation. J Adv Nurs 17(10): 1251-1259.
- Brutus S, Agunis H, Wassmer U (2013) Self-Reported Limitations and Future Directions in Scholarly Reports: Analysis and Recommendations. Journal of Management 39: 48-75.
-
Karin Richards. An Intervention to Build Hope. Annal of Pub Health & Epidemiol. 1(4): 2021. APHE.MS.ID.000519.
-
Body Mass Index, Public Health, Obesity, Public Policy, Food Desert, Food Swamp, Low-income minorities, Junk-food, Unhealthy restaurants
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






