 Case Report
Case Report
Blephaochalasis Syndrome in A Patient With Polycystic Kidney Disease
Maria Cecilia Argibay1*, Matias Agustin Intili2
1Department of Opthalmology, Chief of oculoplastic service, Santa Lucia Eye Private Clinic, Argentina
2Department of Opthalmology, MD pgy3 ophthalmology, Argentina
Maria Cecilia Argibay, Department of Opthalmology, Chief of oculoplastic service, Santa Lucia Eye Private Clinic, Argentina.
Received Date: July 27, 2020; Published Date: August 27, 2020
Abstract
Diabetic retinopathy (DR) is a complication of diabetes due to damage of blood vessels in the retina. Aside from being a major cause of blindness in the world, DR also has a significant impact on quality of life. Although there are methods to delay the progression of DR, there are no existing therapeutic regimens for early intervention. Thus, it is critical to develop cost-effective therapies towards preventing DR development.
Keywords: Diabetic retinopathy; Vision
Abbreviations: DR: Diabetic retinopathy; HRP: Human retinal pericytes; TGFβ: Transforming Growth Factor Beta; BIGH3: TGFβ-induced Gene Human Clone 3
Introduction
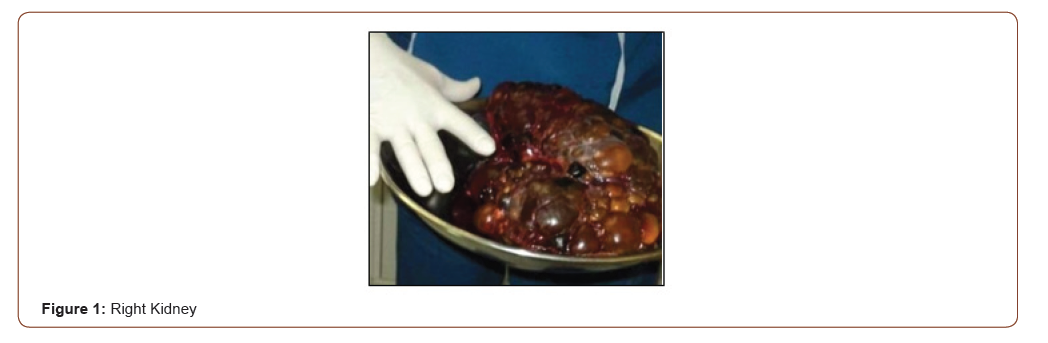
Polycystic kidney disease is caused by an inherited genetic defect. It develops into chronic kidney disease producing generalized edema.
Blepharochalasis syndrome is a rare disease with repeated episodes of eyelid edema followed by loss of subcutaneous tissue with consequent eyelid ptosis and weakening of the orbital septum. It must be differentiated from other pathologies that have some of its main characteristics such as edema, ptosis and recurrent inflam mation. The etiology is still unknown, being its incidence higher in young adults with no gender difference. Current medical and/or surgical treatments fail to guarantee long-term solutions or definitive resolution to disease-related relapses.
In most of the researched works, they opt for surgical resolution, despite the fact that in many cases patients usually have re currences, even reaching ptosis. Surgical intervention was decided after removing both kidneys since the patient stopped having orbital angioedema [1,2].
Case
45-year-old female patient arrives to the medical appointment very distressed and unsatisfied with the appearance of her eyes, “feeling like a little ceiling in both upper eyelids” that causes tiredness, fatigue and the appearance of aging. She was questioned and reported that she suffered from polycystic kidney disease. Both kidneys were removed more than a year ago. As a consequence of poor water management, she presents multiple orbital angioedemas, leaving an excess and laxity of skin in both upper eyelids. She feels permanent irritation, change of texture in the skin of the eyelids and decrease in the lateral visual field. Bio microscopy reveals palpebral laxity that generates significant bilateral blepharochalasis.
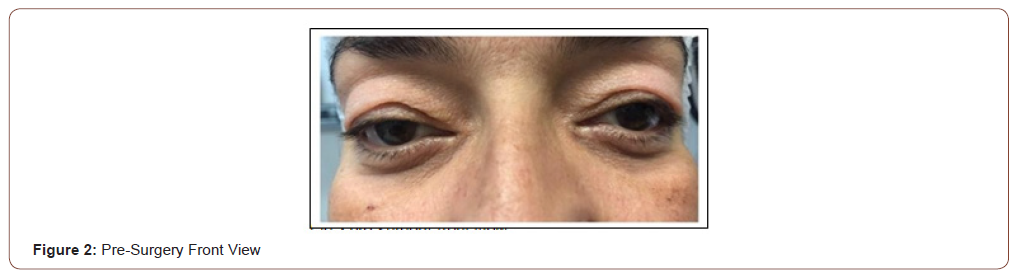
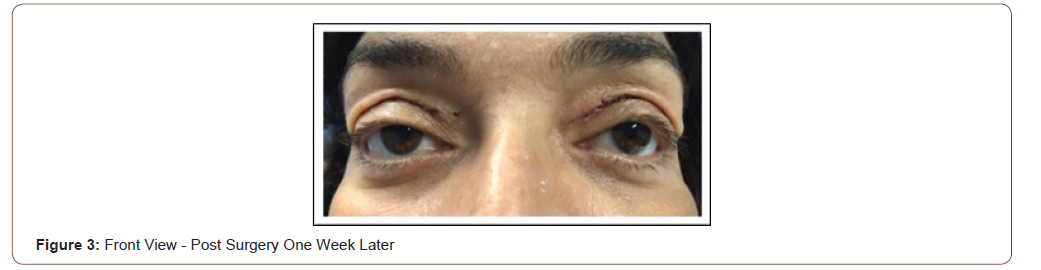
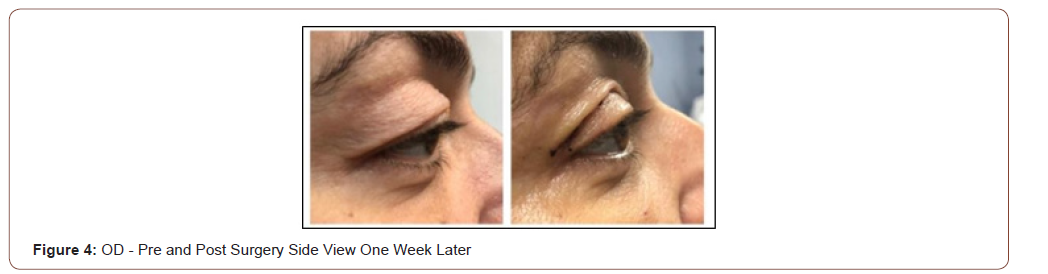
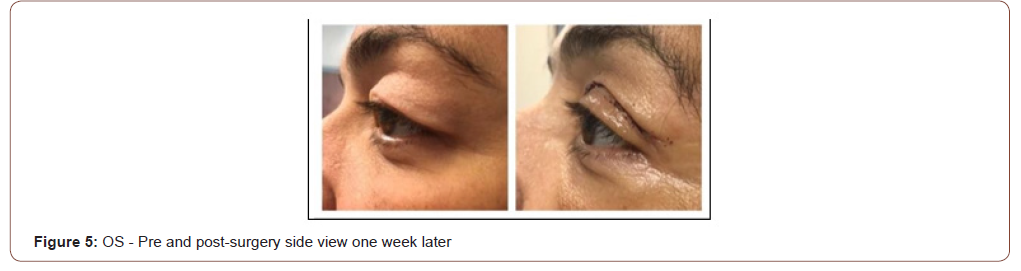
It was decided to perform a superior bilateral blepharoplasty to release excess skin and tighten the orbicularis muscle, as well as to remove the excess fat and remove the upper eyelid pockets.
Conclusion
She underwent surgery a year ago with a satisfactory emotional and functional result.
Acknowledgement
None.
Conflicts of Interest
Authors declares no conflict of interest.
References
- [2016] Kanski’s Clinical Ophthalmology: a systematic approach, pag 55, [Ed: 8], Editorial Eisevier España.
- [2017] Colour Atlas of Ophthalmic surgery, Tyers-Collin, [Ed: 4], Editorial Eisevier España.
-
Maria Cecilia Argibay, Matias Agustin Intili. Blephaochalasis Syndrome in A Patient With Polycystic Kidney Disease. W J Opthalmol & Vision Res. 3(2): 2020. WJOVR.MS.ID.000559.
-
Eneka community, Pingueculum, Pterygium, Nigeria, Fibrovascular, Froliferation, Pingueculum, Ultraviolet radiation, Keratinization, Histopathologically, Immunologic, Metaplasia, Ophthalmologists, Optometrists, Ophthalmic
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






