 Research Article
Research Article
The Impact of Language Proficiency on Tonsillectomy Treatment Timing in Pediatric Patients: A Retrospective Cohort Study
Benjamin Rosen BS1, Hari Roth BS1, Michael Nicolette BA1, Bailey Balouch MD2* and Donald Solomon MD2
1 Cooper Medical School of Rowan University, Camden, NJ 08103
2 Department of Otolaryngology, Cooper University Hospital, Camden, NJ 08103
Bailey Balouch, Department of Otolaryngology, Cooper University Hospital, Camden, NJ, USA.
Received Date: September 22, 2025; Published Date: October 07, 2025
Abstract
Background: Obstructive sleep apnea (OSA) in children is commonly caused by adenotonsillar hypertrophy and is effectively treated with
tonsillectomy. While prior studies have examined post-tonsillectomy outcomes across demographic groups, less is known about disparities in the
pre-treatment phase. This study investigates whether English proficiency of a child’s caregiver influences time-to-treatment for pediatric patients
undergoing tonsillectomy.
Methods: This retrospective cohort study included 274 pediatric patients (ages 0–18) who underwent tonsillectomy with or without
adenoidectomy at a tertiary care academic hospital between 2016–2022. Patients were categorized based on their caregiver’s English proficiency—
those with English proficiency (EP) and limited English proficiency (LEP)—using interpreter documentation during the consent process. Primary
outcomes included time intervals from initial otolaryngology visit to surgical recommendation, from recommendation to consent signing, from
consent to surgery, and total time-to-treatment. Non-parametric tests (Wilcoxon rank-sum and Chi-square) were used to assess statistical significance.
Results: 62 patients had LEP caregivers, and 212 had EP caregivers. No significant differences were observed in time from first visit to surgical
recommendation (median of 0 days for both groups) or from recommendation to consent signing (median of 0 days for both groups) between
groups. However, the interval from consent to surgery was significantly longer for patients with LEP caregivers (median of 32.5 days) than for
patients with EP caregivers (median of 24.5 days). Total time-to-treatment was longer for patients with LEP caregivers (median of 72 days) than for
patients with EP caregivers (median of 53 days), but this result was not statistically significant.
Conclusion: Caregiver LEP is associated with delayed surgical intervention following consent for pediatric patients undergoing tonsillectomy.
This delay highlights a disparity in surgical care timeliness for pediatric patients with LEP caregivers.
Keywords: Obstructive sleep apnea, Adenotonsillar hypertrophy, Tonsillectomy, Language proficiency, Surgical consent
Introduction
Obstructive sleep apnea (OSA) is characterized by repeated episodes of complete or partial airway obstruction during sleep, leading to intermittent hypoxia and increased arousals [1]. The greatest risk factor for OSA in the pediatric population is adenotonsillar hypertrophy, with definitive treatment being tonsillectomy [1]. It has been shown that pediatric OSA is associated with significant morbidities and negatively impacts a child’s overall health, specifically affecting behavior, brain development, and metabolism [2]. Therefore, timely diagnosis and treatment of OSA are essential for proper pediatric development.
Several studies have examined how key demographic factors influence post-tonsillectomy outcomes. It has been shown that pediatric patients with non-English-speaking caregivers are more likely to visit the emergency department (ED) rather than make remote phone calls to the office to address post-tonsillectomy issues, even when ED visits are unnecessary for said complications [3]. Other researchers have found that patients with LEP are not at increased risk of post-tonsillectomy hemorrhage compared to those with EP [4]. Following tonsillectomy, Asian patients with non- English language preference had 2.1 times the odds of readmission [5].
Extensive research has focused on post-tonsillectomy outcomes and how they are affected by language and other demographic factors, yet there is limited research on how these factors influence the pre-treatment phase. Several key steps are involved in obtaining a tonsillectomy for pediatric patients for whom this procedure is indicated, including scheduling an appointment with an otolaryngologist, attending the appointment, being recommended for surgery after a thorough clinical evaluation, providing informed consent, and scheduling and undergoing the procedure. Patients with LEP face longer wait times to access otolaryngologic care compared to those with EP, even after controlling for socioeconomic factors [6]. These extended wait times include both the period from referral to appointment scheduling and from scheduling to attendance [6]. The consent process for surgery presents additional challenges, especially when healthcare providers and patients are primarily proficient in different languages. One study examining how English-speaking physicians obtain informed consent from patients with LEP found that surgeons often rely on non-professional interpreters, such as a patient’s family member or friend, or their own limited proficiency in the patient’s language, even if it is inadequate [7]. It is clear that patients with LEP needing otolaryngologic care experience disadvantages in the pre-treatment phase; however, no studies have investigated how the total time-totreatment is affected for these patients.
This study aims to assess how caregiver language proficiency influences the total time-to-treatment in pediatric patients undergoing tonsillectomy at a tertiary care academic hospital. We hypothesize that among pediatric patients with OSA, those with LEP caregivers experience longer time intervals from initial otolaryngology appointment to surgical intervention compared to those with EP caregivers. Recognizing these disparities is vital for developing targeted strategies to ensure equitable and timely healthcare access for all pediatric patients, regardless of language proficiency.
Materials and Methods
This retrospective cohort study was approved by the Cooper Institutional Review Board. Inclusion criteria included pediatric patients 0-18 years old who underwent tonsillectomy surgery with or without adenoidectomy at a tertiary care academic hospital from 2016-2022. Exclusion criteria included adult patients aged 19 years or older. A total of 274 patients were included in this study. Data was collected retrospectively from electronic health records. The exposure group consisted of patients with LEP guardians, defined in this study as evidence of utilizing a non-English interpreter to obtain surgical consent. The control group comprised patients with EP guardians, defined by no interpreter required for consent. Consent forms, viewed as scanned documents in the electronic health records, included all necessary interpreter information for patients included in the LEP group. Demographic data collected included age, sex, the patient’s primary language as recorded in the electronic medical record, the guardian’s primary language as documented in the digital consent form, and medical insurance status.
Primary outcome variables included the time from the first otolaryngology office visit to surgical recommendation, the time from surgical recommendation to signing the consent form, the time from signing the consent form to the surgical date, and total treatment duration. One potential confounder is insurance status. It should be noted that we did not control for insurance status because only one subject in the LEP group had private insurance, making it difficult to match insurance status between the exposure and control groups.
All variables were expected to be non-normally distributed. Statistical significance was set at a p-value < 0.05. The Wilcoxon rank-sum test, a non-parametric method, was used to compare continuous outcomes across categories. For analysis involving only categorical variables, the Chi-square test was employed.
Results
Out of 274 patients included in the analysis, 62 were in the LEP group, and 212 were in the EP group. The average age was 7.21 years for the LEP group and 7.32 years for the EP group (p = 0.85). The number of males was 38 in the LEP group and 115 in the EP group (p = 0.33). The number of patients with private insurance was 1 in the LEP group and 56 in the EP group (p < 0.001). Demographic data is summarized in Table 1.
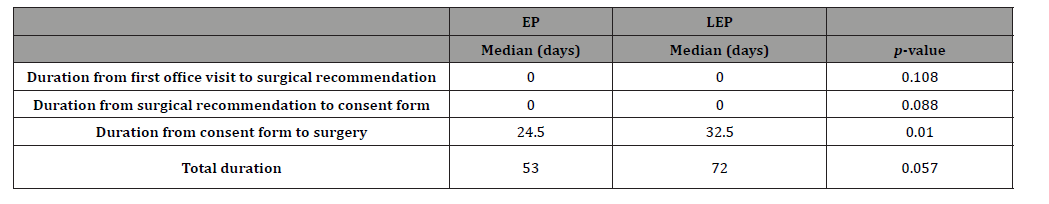
Given the data’s non-normal distribution and presence of outliers, results are presented as medians. The detailed findings are shown in Table 2. The median number of days from the first otolaryngology visit to surgical recommendation was zero in both groups (p = 0.108). The median number of days from surgical recommendation to signing the surgical consent form was also zero in both groups (p = 0.088). From signing the consent to surgery, the median was 24.5 days in the EP group and 32.5 days in the LEP group (p = 0.010). The total median days from the first office visit to surgery were 53 in the EP group and 72 in the LEP group (p = 0.057).
Table 1:Demographic data of subjects
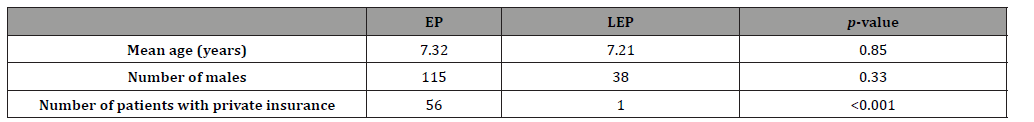
Table 2:Primary outcomes.
Discussion
Key Findings
This retrospective cohort study evaluated the impact of caregiver language proficiency on time-to-treatment in pediatric patients undergoing tonsillectomy for OSA. Our primary findings suggest that while most steps in the pre-treatment timeline are comparable between patients with EP and LEP caregivers, a significant delay exists in the final stage: from signing the surgical consent form to undergoing surgery. Additionally, the total time from initial otolaryngology visit to surgery was longer for patients with LEP caregivers, though this result was not statistically significant.
The only statistically significant delay was observed in the time from consent signing to surgery, with a median difference of 8 days. This suggests that there may be barriers in scheduling a tonsillectomy surgery after signing consent that disproportionately affect patients with LEP caregivers. One potential contributor to this significant delay is the impact of the medical interpreters. While interpreters are available for use throughout all clinical settings, the efficacy of interpretation is in question. While the error rate in noncertified interpreters can be as high as 22%, errors in translation can occur up to 12% of the time even with medically trained interpreters [8]. The level of training for interpreters can vary widely. It is shown that there is a significant reduction in translation errors when professional medical interpreters have at least 100 hours of training [9]. Ultimately, reducing the number of interpreter errors has consequences for patient safety and the quality of care a physician can provide.
Even when no translational errors are made, LEP caregivers may still leave an office visit or phone call and not fully understand their child’s condition or the treatment plan. In a survey study analyzing concerns for non-English-speaking patients and their caregivers, while the large majority of parents and guardians felt that their concerns were clearly addressed, about half of parents or guardians reported not knowing why they were seeing that specialty provider or the treatment plan. Compounding this confusion, these same individuals had difficulty understanding the interpreters and felt the translation was not accurate [10]. Rather than unidirectional communication from physician to interpreter to caregiver, caregivers and patients can benefit from active communication, relaying caregivers’ concerns back to them to ensure all concerns are met. This may be one contributing factor in the differences in duration from consent form signing to surgery between LEP and EP patients.
Limited access to professional interpreter services during calls can also influence the duration from consent to surgery. At our institution, once caregivers sign the consent form, a surgical scheduler contacts the patients’ guardians to help schedule a surgery date based on the surgeon’s availability. If there is a language barrier between the caller and caregiver and no interpreter is available, communication difficulties might prevent scheduling a surgical date.
Although not statistically significant, the total duration of treatment from the first otolaryngology visit to surgery was longer for LEP patients, with a median difference of 19 days. This result is not statistically significant likely because the total duration of treatment is an accumulation of each phase from the first visit to surgery. The results of this study show that the duration from consent to surgery was the only statistically significant duration between LEP and EP groups. The other durations in the pretreatment phase, including time from office visit to surgical recommendation and from recommendation to consent, are not statistically significant between the two groups. This non statistically significant difference may reflect cumulative minor delays at multiple points in the pre-treatment process, collectively contributing to prolonged treatment timing in the LEP group.
Interestingly, no significant difference was found between LEP and EP groups in the time from first visit to surgical recommendation or from recommendation to consent signing. These findings may indicate that once patients access specialist care, the otolaryngologist already has all the required information, including lab and diagnostic tests, to confidently recommend surgical treatment. When surgery is recommended during that first visit, the physician will talk through the consent form with the patient and caregiver, discussing the benefits and risks of the surgery. For patients with LEP caregivers at our institution, a professional interpreter through a video service or in person must be utilized during the surgical consent process.
Limitations
This study has several limitations. First, as a retrospective chart review, it is limited by the accuracy and completeness of documentation in electronic medical records. Language proficiency was determined using interpreter documentation on consent forms, which may misclassify some patients if interpreter use was not recorded or recorded improperly. Additionally, the sample size of the LEP group (n = 62) may limit the power to detect statistically significant differences in some treatment intervals. Lastly, this study reflects a single-center experience and may not be generalizable to all healthcare settings.
Conclusion
This study highlights a meaningful disparity in surgical care delivery for pediatric patients with LEP caregivers, specifically in the interval between obtaining surgical consent and undergoing surgery. While earlier steps in the treatment pathway appear unaffected, there is a significant delay in scheduling or coordinating surgery once the consent form is signed in those patients with LEP caregivers. These findings may underscore the need for interventions that ensure timely care for all pediatric patients undergoing tonsillectomy, regardless of caregiver language proficiency.
Acknowledgement
None.
Conflict of Interest
None.
References
- Gouthro K, Slowik JM (2022) Pediatric Obstructive Sleep Apnea.
- Chang SJ, Chae KY (2010) Obstructive sleep apnea syndrome in children: Epidemiology, pathophysiology, diagnosis and sequelae. Korean J Pediatr 53(10): 863-871.
- Dai X, Ryan MA, Clements AC (2021) The Effect of Language Barriers at Discharge on Pediatric Adenotonsillectomy Outcomes and Healthcare Contact. Ann Otol Rhinol Laryngol 130(7): 833-839.
- Plocienniczak M, Rubin BR, Kolli A, Levi J, Tracy L (2022) Outcome Disparities and Resource Utilization Among Limited English Proficient Patients After Tonsillectomy. Ann Otol Rhinol Laryngol 131(11): 1241-1246.
- Wentzel S, Craft A, Onwuka A, Lind M (2024) Racial, ethnic and language disparities in healthcare utilization in pediatric patients following tonsillectomy. Int J Pediatr Otorhinolaryngol 176: 111805.
- Lopez B, Gottlieb BR, Naples JG (2023) Longer Times to Delivery of Otolaryngology Care for Patients With Limited English Proficiency. Otolaryngol Head Neck Surg 169(3): 651-659.
- Patel DN, Wakeam E, Genoff M, Mujawar I, Ashley SW, Diamond LC (2016) Preoperative consent for patients with limited English proficiency. J Surg Res 200(2): 514-522.
- DeCamp LR, Kuo DZ, Flores G, O’Connor K, Minkovitz C (2013) Changes in language services use by US pediatricians. Pediatrics 132: e396-e406.
- Flores G, Abreu M, Barone CP, Bachur R, Lin H (2012) Errors of medical interpretation and their potential clinical consequences: a comparison of professional versus ad hoc versus no interpreters. Ann Emerg Med 60: 545-553.
- Raynor EM (2015) Factors Affecting Care in Non-English-Speaking Patients and Families. Clinical Pediatrics 55(2): 145-149.
-
Benjamin Rosen BS, Hari Roth BS, Michael Nicolette BA, Bailey Balouch MD* and Donald Solomon MD. The Impact of Language Proficiency on Tonsillectomy Treatment Timing in Pediatric Patients: A Retrospective Cohort Study. On J Otolaryngol & Rhinol. 8(1): 2025. OJOR.MS.ID.000679
-
Tonsillectomy treatment, Obstructive sleep apnea, Otolaryngologic care, Tonsillectomy surgery, Language proficiency, Diagnostic tests, Translation errors, Healthcare access, Otolaryngologist
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






