 Case Report
Case Report
Simultaneous Buccal Mucosa Composite Resection with Total Laryngectomy for Double Synchronous Primary Squamous Cell Carcinoma: A Case Report and Literature Review
Dr. Kaushal Yadav MS, MCh*
Unit Head Surgical Oncology, Max Hospital Gurugram, Haryana
Dr. Kaushal Yadav MS, MCh, Unit Head Surgical Oncology, Max Hospital Gurugram, Haryana.
Received Date: December 18, 2025; Published Date: January 12, 2026
Abstract
The emergence of synchronous primary malignancies within the context of head and neck squamous cell carcinoma (HNSCC) constitutes a rare yet clinically pertinent dilemma, manifesting in approximately 5.3% of HNSCC patients. Treatment in such clinical conditions requires a multidisciplinary approach. This article describes a unique case involving double synchronous primary squamous cell carcinomas of soft palate area and larynx, post chemoradiotherapy. As a salvage treatment patient underwent composite resection along with total laryngectomy in same surgery. At the conclusion of five years, he remained free from disease and experienced an adequate quality of life.
Keywords: Synchronous primary tumors; Head and neck cancer; Composite resection; Total laryngectomy; Salvage surgery; Field cancerization; Second primary; Metachronous cancer; Stappler laryngectomy
Introduction
The occurrence of multiple primary malignancies associated with head and neck squamous cell carcinoma (HNSCC) presents a significant management challenge. Multiple primary tumors are categorized as either synchronous or metachronous primary tumor. Synchronous primary tumors (SPT) are defined as the identification of two or more distinct primary malignancies within a six-month period. Metachronous primary tumors (MPT) are defined as two or more primary malignancies appearing at an interval of more than six months [1, 2]. Coca-Pelaz et al. evaluated data from 456,130 patients over 61 studies, reported 5.3% (95% CI: 4.24–6.36%) incidence of SPT and 9.4% (95% CI: 7.9–10.9%) incidence of MPT [3]. According to the SEER database, nearly 11% of individuals diagnosed with HNSCC exhibit a secondary primary tumor, with 3.2% occurring as a head and neck primary [4]. Findings from a single center studies indicate SPT rates of 3.7-6.4% [5, 6]. Overall incidence of multiple primary tumors in patients with head and neck cancer is reported as 9.4% to 13.2% in various studies [3, 7].
The anatomical distribution of synchronous primary malignancies in HNSCC demonstrates a tendency for the upper aerodigestive tract. Anatomical regions mostly associated with SPT involve the oral cavity, pharynx, larynx, esophagus, and lung [3, 4]. Literature on cohorts of panendoscopy report that nearly 61% of SPT are detected in the oral cavity, pharynx, or larynx [6]. Esophageal second primaries tend to present synchronously, whereas lung second primaries more commonly manifest as metachronous lesions; however both lung and esophagus can present as SPT or MPT [7]. The risk of developing metachronous second cancers is highest for tongue primary and overall incidence of second primary within two years was 1.7%, within five years 4.9 and within 10 years 7.8% [8].
Specific SPT pairs within the head and neck region have been documented in the literature, though reported frequency for individual combinations is limited. The combination of laryngeal and oral cavity (including buccal mucosa) synchronous primaries has been reported in institutional series and case reports, representing one of the recognized patterns of synchronous HNSCC [8, 9]. Considering rarely reported estimates of specific combination of laryngeal and buccal mucosa synchronous primaries, each documented case is valuable for understanding.
The pathogenesis of synchronous and metachronous primaries in head and neck cancer is primarily attributed to the field cancerization phenomenon and shared carcinogenic exposures, particularly tobacco and alcohol use [10]. Field cancerization describes the widespread mucosal genetic and premalignant changes induced by chronic carcinogen exposure, creating a susceptible “field” throughout the upper aerodigestive tract that predisposes to multiple independent primary malignancies [10]. The strong association with tobacco exposure is evidenced by data showing second cancer incidence rates of 3% in nonsmokers versus 32% in heavy smokers and drinkers [8]. Furthermore, smoking cessation significantly impacts risk, with 15-year cumulative risks of second primary malignancy ranging from 14% in never-smokers to 32% in current smokers [11].
Management of synchronous primary malignancies in the head and neck region requires individualized treatment strategies based on the extent, location, and resectability of both lesions. Published institutional guidelines suggest treating the more advanced or life-threatening cancer first when simultaneous treatment is not feasible, performing synchronous resections when both lesions can be safely addressed in a single operation, and tailoring radiation therapy fields based on cumulative dose constraints and treatment intent [12]. The complexity of managing double synchronous primaries, particularly when involving both the larynx and oral cavity, necessitates multidisciplinary decision-making and often requires innovative surgical approaches to achieve oncologic control while maintaining acceptable functional outcomes. The combination of laryngeal and buccal mucosa synchronous primaries managed simultaneously has been reported only once previously in a 47‑year‑old male who underwent wide local excision with total laryngectomy in a single sitting [13].
Case Presentation
54 years male with no comorbidities was detected with soft palate growth and right vocal cord growth in 2018. Laryngoscopy biopsy of vocal cord growth confirmed it as squamous cell carcinoma. From December 2018 to February 2019, he received definitive chemoradiotherapy for right vocal cord malignancy. Considering the small superficial growth of the soft palate, it was kept under observation initially. In June 2019, growth increased as multifocal erythematous patch over hard palate and soft palate junction of size 3cm. Biopsy from this lesion confirmed moderately differentiated squamous cell carcinoma. PET Scan showed uptake in the soft palate lesion only, with no other evidence of hypermetabolic uptake. From July to August 2019, he received definitive radiation therapy. After treatment he remained on followup. In June 2020, thickening is seen in the right side soft palate with involvement of right glossotonsillar sulcus with minimal extension in retromolar trigone (RMT) (SUV 5.2).
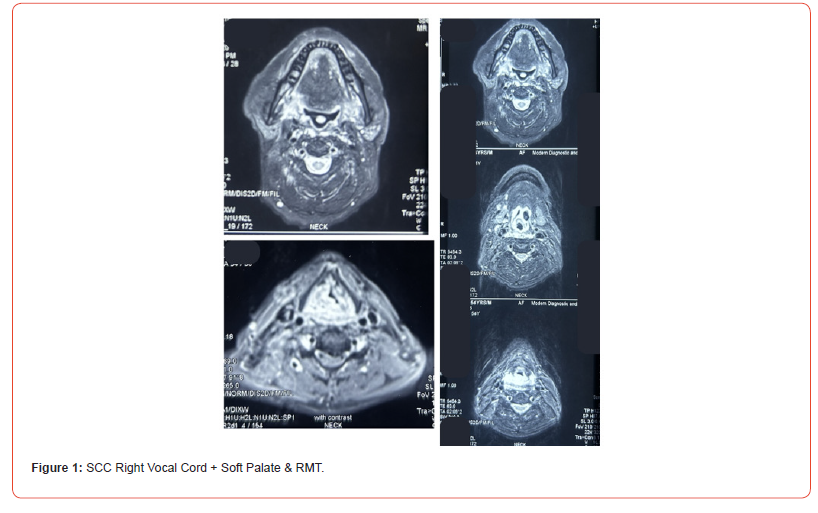
In larynx, FDG avid soft tissue thickening was seen in the anterior two-third of right vocal cord with involvement of anterior commissure and contralateral extension on the left side involving anterior one-third of the left vocal cord. Soft palate and retromolar lesion biopsy revealed moderately differentiated squamous cell carcinoma. Biopsy from vocal cord lesion confirmed moderately differentiated squamous cell carcinoma. Patient received three cycles of chemotherapy (docetaxel+cisplatin + 5 FU) till August 2020. He had disease progression and presented in the emergency with stridor, for which emergency tracheostomy was done. Contrast CT scan revealed bilateral vocal cord lesion with near complete airway obstruction. In view of further poor tolerance of chemotherapy, he received oral capecitabine along with nutritional rehabilitation. December 2020 PET CECT highlighted the persistent lesion in the right lateral aspect of soft palate extending to retromolar trigone and glossotonsillar sulcus. A second primary lesion was present in the vocal cord. Metastatic disease was absent (Figure 1). In December 2020, he was scheduled for surgery for both primary sites simultaneously. He underwent right soft palate/RMT lesion bite composite resection (wide excision with upper alveolectomy with posterior segmental mandibulectomy) along with Total Laryngectomy with appropriate neck dissection. Oral cavity reconstruction was done with pectoralis major myocutaneous flap. Laryngectomy was done with the use of an endo GI stapler, resulting in stapled closure of the laryngopharyngectomy defect (Video 1) . Considering two simultaneous surgery, primary voice prosthesis was not inserted during surgery. Patient was discharged on the 7th postoperative day. Following recovery, he remained on regular followup. At 5 years of followup; he remined disease free with an acceptable quality of life.
Discussion
For the management of synchronous primary HNSCC three principal management approaches exist: sequential treatment of individual primaries, concurrent chemoradiation therapy (CCRT) addressing both lesions, and simultaneous surgical resection of both tumors [1-3]. Traditionally, concurrent chemoradiotherapy has been utilized to address synchronous head and neck primaries when the tumors are situated within overlapping radiation fields. CCRT has the advantage of treating multiple lesions at same time. However, cumulative radiation dose of the upper aerodigestive tract may be exceeded when treating anatomically separate primary lesions. This toxicity burden may increases substantially with dysphagia, xerostomia, and late complications [3, 14].
The patient in this clinical case initially received radiation therapy and chemotherapy. The disease progression underlines the poor outcomes for radiation-refractory synchronous disease with further nonsurgical treatment modalities [15].
Salvage surgery represents the definitive therapeutic option for locoregionally advanced, radiation-refractory synchronous primaries. Current multidisciplinary guidelines recommend considering salvage surgical resection in patients with persistent or recurrent head and neck cancer following primary chemoradiation or radiotherapy, provided the patient is medically fit and the tumor is resectable with negative margins [16]. Recent investigations have identified R0 resection as one of the most common determinant of long-term survival in the salvage setting. In a cohort of patients undergoing salvage total laryngectomy subsequent to the failure of radiotherapy or chemoradiotherapy, lymphovascular invasion and positive surgical margins emerged as independent predictors of inferior overall survival, disease-specific survival, and diseasefree survival [17]. Achievement of negative surgical margins was the strongest independent predictor of durable disease control. The 5-year disease-free survival rate following salvage total laryngectomy varies between 50–53%, with superior outcomes in patients with negative surgical margins, absence of lymphovascular invasion, and N0 or N1 nodal disease [18, 19]. The patient in this case remained disease-free at the 5-year follow-up subsequent to the simultaneous resection of both primary sites with negative margins.
Re-radiation of previously treated HNSCC have higher cumulative toxicity and lesser therapeutic efficacy [14, 20]. Chemotherapy in the palliative setting provides temporary control but rarely achieves durable response [21]. In contrast, R0 surgical resection is the only realistic opportunity for cure. This principle is supported by fact that upfront surgery in selected locally advanced head and neck cancers achieves superior survival outcomes compared to primary CCRT [22, 23]. Contemporary multidisciplinary guidelines emphasize that treatment advice for patients with SPT must be individualized and multidisciplinary [16]. The decision to pursue salvage surgery in this patient reflects adherence to evidence-based principles: comprehensive staging with imaging (PET-CT) documenting absence of metastatic disease; assessment of medical fitness for extended surgery; documented progression on nonsurgical therapies; and identification of both tumors as resectable with expectation of negative margins.
The presentation of synchronous laryngeal and oral cavity primaries reflects the phenomenon of field cancerization— widespread mucosal premalignant changes induced by chronic carcinogen exposure, primarily tobacco and alcohol [10]. Treatment of grossly apparent tumors through surgery does not eliminate the genetically altered field, which remains at ongoing risk for additional malignant transformation [10, 24]. This highlights the necessity for comprehensive surveillance of the treated HNSCC [25].
Conclusion
The management of SPT necessitates personalized multidisciplinary evaluations. In cases of chemoradiotherapy failure, salvage surgery may yield a cure if negative margins are attainable and the patient’s health permits. The presented case demonstrated that simultaneous resection of laryngeal and oral cavity primaries achieved five-year disease-free status in a selectively chosen patient with radiation-refractory disease.
Acknowledgement
None.
Conflict of Interest
None.
References
- Ha JF, Parham G, Baerg T, Harrop AR (2019) Synchronous and metachronous head and neck squamous cell carcinoma in western Australia—a single center experience. Asian J Oncol 4: 16.
- Liu K, Zhang XX, Chen N (2020) Clinical characteristics, treatments, and prognosis of patients with multiple primary carcinoma of head and neck. Chin Med J (Engl). 133(4): 424-431.
- Coca-Pelaz A, Rodrigo JP, Suárez C (2020) The risk of second primary tumors in head and neck cancer: a systematic review. Head Neck 42(3):456-466.
- Chinn SB, Spector ME, Prince ME, et al. (2013) Synchronous and metachronous tumors in head and neck cancer: analysis of the SEER database. Otolaryngol Head Neck Surg 149(2 Suppl): P169.
- Stoeckli SJ, Zimmermann R, Schmid S (2001) Role of routine panendoscopy in cancer of the upper aerodigestive tract. Otolaryngol Head Neck Surg 124(2): 208-212.
- Panosetti E, Luboinski B, Mamelle G, Richard J (1999) Multiple synchronous and metachronous cancers of the upper aerodigestive tract: a nine-year study. Laryngoscope 99(12): 1267-1273.
- Schwartz LH, Ozsahin M, Zhang GN (1994) Synchronous and metachronous head and neck carcinomas. Cancer 74(7): 1933-1938. doi:10.1002/1097-0142(19941001)74: 7<1933::AID-CNCR2820740718>3.0.CO;2-X
- Rogers SN, Swain A, Carroll C (2019) Incidence, timing, presentation, treatment, and outcomes of second primary head and neck squamous cell carcinoma after oral cancer. Br J Oral Maxillofac Surg 57(10): 1068-1075.
- Badwelan M, Muaddi H, Lee KT (2023) Oral squamous cell carcinoma and concomitant primary tumors, what do we know? A review of the literature. Curr Oncol 30(4): 3721-3734.
- Ng SP, Pollard C, Kamal M (2019) Risk of second primary malignancies in head and neck cancer patients treated with definitive radiotherapy. NPJ Precis Oncol 3: 22.
- Tona R, Shinohara S, Kikuchi M (2013) Synchronous multiple malignancies in patients with head and neck squamous cell carcinoma. Practica Oto-Rhino-Laryngologica 106(2): 155-161.
- Ioannides G, Gourin CG, Hayden RE (2020) Survival outcomes and predictors for patients who failed chemoradiotherapy/radiotherapy and underwent salvage total laryngectomy. Int J Radiat Oncol Biol Phys 108(4): 980-988.
- Sen I, Ghosh D, Guha G (2020) Synchronous Buccal Carcinoma and Laryngeal Carcinoma- A Rare Presentation. 28(2): 182-186.
- Vermorken JB, Remenar E, van Herpen C (2007) Cisplatin, fluorouracil, and docetaxel in unresectable head and neck cancer. N Engl J Med 357(17): 1695-1704.
- Dietz A, Rudat V, Dreyhaupt J, Pritsch M, Hoppe F, et al. (2009) Induction chemotherapy with paclitaxel and cisplatin followed by radiotherapy for larynx organ preservation in advanced laryngeal and hypopharyngeal cancer offers moderate late toxicity outcome (DeLOS-I-trial). Eur Arch Otorhinolaryngol 266(8): 1291-300.
- Payam Afzali, Brent Benson Ward (2019) Management of the Neck in Oral Squamous Cell Carcinoma: Background, Classification, and Current Philosophy. Oral Maxillofac Surg Clin North Am 31(1): 69-84.
- Shoushtari ST, Gal J, Chamorey E, Schiappa R, Dassonville O, et al. (2023) Salvage vs. Primary Total Laryngectomy in Patients with Locally Advanced Laryngeal or Hypopharyngeal Carcinoma: Oncologic Outcomes and Their Predictive Factors. J Clin Med 12(4): 1305.
- Silverman DA, Puram SV, Rocco JW, Old MO, Kang SY (2019) Salvage laryngectomy following organ-preservation therapy - An evidence-based review. Oral Oncol 88: 137-144.
- Meulemans J, Demarsin H, Debacker J, Batailde G, Mennes T, et al. (2020) Functional Outcomes and Complications After Salvage Total Laryngectomy for Residual, Recurrent, and Second Primary Squamous Cell Carcinoma of the Larynx and Hypopharynx: A Multicenter Retrospective Cohort Study. Front Oncol 10: 1390.
- Wulff N B, Andersen E, Kristensen C, Sørensen C H, Charabi B, et al. (2017) Prognostic factors for survival after salvage total laryngectomy following radiotherapy or chemoradiation failure: a 10-year retrospective longitudinal study in eastern Denmark. Clin Otolaryngol 42(2): 336-346.
- Kish JA, Weaver A, Jacobs J, Cummings G, Al-Sarraf M (1984) Cisplatin and 5-fluorouracil infusion in patients with recurrent and disseminated epidermoid cancer of the head and neck. Cancer 53(9):1819-24. doi: 10.1002/1097-0142(19840501)53:9<1819::aid-cncr2820530903>3.0.co;2-r.
- Galeone C, Edefonti V, Garavello W (2009) Field cancerization and its relationship with multiple cancers in the head and neck. Curr Opin Otolaryngol Head Neck Surg 17(2): 99-104.
- Shimada A, Tanaka M, Ishii S, Okamoto N, Yamamoto Y, Osaki M, et al. (2022) Utility of Concurrent Surgical Treatment Strategy with Thoracoscopic Esophagectomy for Patients with Synchronous Esophageal and Head and Neck Cancer. J Laparoendosc Adv Surg Tech A 32(5): 550-555.
- Braakhuis BJ, Tabor MP, Leemans CR, van der Waal I, Snow GB, Brakenhoff RH (2002) Second primary tumors and field cancerization in oral and oropharyngeal cancer: molecular techniques provide new insights and definitions. Head Neck 24(2): 198-206.
- Chung CS, Liao LJ, Wu CY, Lo WC, Hsieh CH, et al. (2022) Endoscopic Screening for Second Primary Tumors of the Esophagus Among Head and Neck Cancer Patients. Front Oncol 12: 906125.
-
Dr. Kaushal Yadav MS, MCh*. Simultaneous Buccal Mucosa Composite Resection with Total Laryngectomy for Double Synchronous Primary Squamous Cell Carcinoma: A Case Report and Literature Review. On J Otolaryngol & Rhinol. 8(2): 2026. OJOR. MS.ID.000685.
-
Squamous cell carcinoma, Head and neck, Larynx, Esophagus, Oral cavity, Buccal mucosa, Heavy smokers, Tobacco, Chemotherapy
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






