 Research Article
Research Article
Investigating Perineural Spread in Oral Squamous Cell Carcinoma Using Computed Tomography in Resource Constrained Setting
Bibek Keshari1, Pankaj Sharma2*, Amit Kumar Tyagi3, Sanjeev Kishore4 and Santosh Kumar5
1 Junior Resident Radiodiagnosis, All India Institute of Medical Sciences Rishikesh, India
2 Additional Professor Radiodiagnosis, All India Institute of Medical Sciences Rishikesh, India
3 Additional Professor Otorhinolaryngology & Head and Neck Surgery, All India Institute of Medical Sciences Rishikesh, India
4 Professor Pathology, All India Institute of Medical Sciences Rishikesh, India
5 Additional Professor Community and Family Medicine, All India Institute of Medical Sciences Rishikesh, India
Pankaj Sharma, Department of Diagnostic and Interventional Radiology, All India Institute of Medical Sciences, Rishikesh, Uttarakhand, India.
Received Date: July 24, 2025; Published Date: August 07, 2025
Abstract
Background: Oral squamous cell carcinoma (OSCC) accounts for a considerable number of head and neck cancer cases, particularly in India.
Perineural spread (PNS) is a vital prognostic factor influencing treatment strategies and surgical outcomes. Although Magnetic Resonance Imaging
(MRI) is the preferred method for detecting PNS, Computed Tomography (CT) offers a practical and accessible alternative, especially in low-resource
setting.
Objective: The study aimed to assess the diagnostic performance of CT in identifying PNS in OSCC, examine the relationship between PNS and
TNM staging, and analyse the patterns of PNS across various subsites.
Methods: This prospective study spanned 18 months at a tertiary care centre in Northern India involving 100 treatment-naive OSCC patients.
Preoperative CT scans were analysed for signs of PNS and cross-referenced with histopathological findings from post-surgical specimen, serving
as the gold standard. Sensitivity, Specificity, Positive Predictive Value (PPV), and Negative Predictive Value (NPV) were determined. Correlations
between PNS and tumor stage, along with anatomical patterns of spread were evaluated.
Results: The cohort consisted of 100 patients (mean age: 50.08 ±12.15 years), with 90% being male. Buccal mucosa (48%) and tongue (23%)
were the predominant tumor sites. CT demonstrated a sensitivity of 73% and a specificity of 93% in detecting PNS. Key predictors included foraminal
widening, nerve thickening, and muscle atrophy. Advanced tumor stages (TNM stage III and IV) were significantly associated with PNS. The buccal
mucosa displayed the highest prevalence of PNS (48%), followed by the tongue (23%).
Conclusion: CT provides a reliable, accessible diagnostic option for identifying PNS in OSCC and offers critical insights into its correlation
with tumor stage and anatomical subsites. Subclassification of T4b disease using CT findings facilitates personalized treatment planning. Further
research on advanced CT protocols is recommended to enhance diagnostic accuracy.
Keywords: Oral squamous cell carcinoma, Perineural spread, Computed tomography, Diagnostic accuracy, TNM staging, T4b sub-classification
Introduction
Oral squamous cell carcinoma (OSCC) is a common and aggressive cancer. India is considered capital of OSCC with more than 70,000 new cases diagnosed annually [1]. Perineural spread (PNS) is a critical factor that affects OSCC prognosis, where tumor cells invade nerve pathways, leading to more aggressive disease behavior, higher recurrence, and also directly impacts surgical planning and radiation therapy complex treatment planning [2]. It is one of the primary forms of local invasion, affecting major cranial nerves, especially branches of the trigeminal (CN V) and facial (CN VII) nerves.
Detecting PNS is vital for OSCC management, as untreated perineural involvement often signifies advanced disease and poor prognosis. Furthermore, various studies have suggested subclassification of T4b disease as T4 disease with infra-notch extension has favorable prognosis, and is considered surgeon friendly; while those with supra-notch extension are usually unresectable [3- 8]. Detection of PNS aids in this subclassification. PNS is often clinically silent and often occurs in areas that are difficult to biopsy, making histopathological confirmation challenging. This brings in crucial role of Radiology in detecting PNS and guiding treatment decisions. CT scan is the modality of choice for staging the cancer. However, PNS is often under-reported on CT. MRI is more sensitive but is costly, time consuming and has limited availability at various centers across India. And with no clinical suspicion of PNS, MRI often not acquired. Hence, it is essential to detect perineural spread or at least raise the suspicion of perineural spread on staging CT scans (specially in resource constrain setting), so as to improve the patient outcome. The current study focuses on evaluating CT’s diagnostic accuracy for PNS detection in OSCC, exploring its association with TNM staging, and analysing the distribution of PNS across different anatomical sites. Additionally, the study investigates CT’s potential in subclassifying T4b cases, a step toward enhancing treatment outcomes.
Materials and Methods
Study Design: A prospective diagnostic validation study conducted over 1.5 years at AIIMS Rishikesh.
Standard & Reference Test: Histopathology of surgical specimen.
Participants: Treatment-naive OSCC patients referred for preoperative CT were included. Patients with prior head and neck interventions or contraindications to contrast were excluded.
Imaging Protocol: All CT studies were performed using Siemens Somatom Flash 128 slice CT scanner and Philips 64 slice CT scanner. Patient were placed in supine position with feet first and scanning was done in caudo-cranial direction. 50ml non-ionic contrast (Iohexol) was given at the rate of 2.5ml/sec, followed by 20ml saline flush. Scan were taken at 45-50 sec after contrast injection from the base of skull to the diaphragm, using soft tissue and bone algorithms.
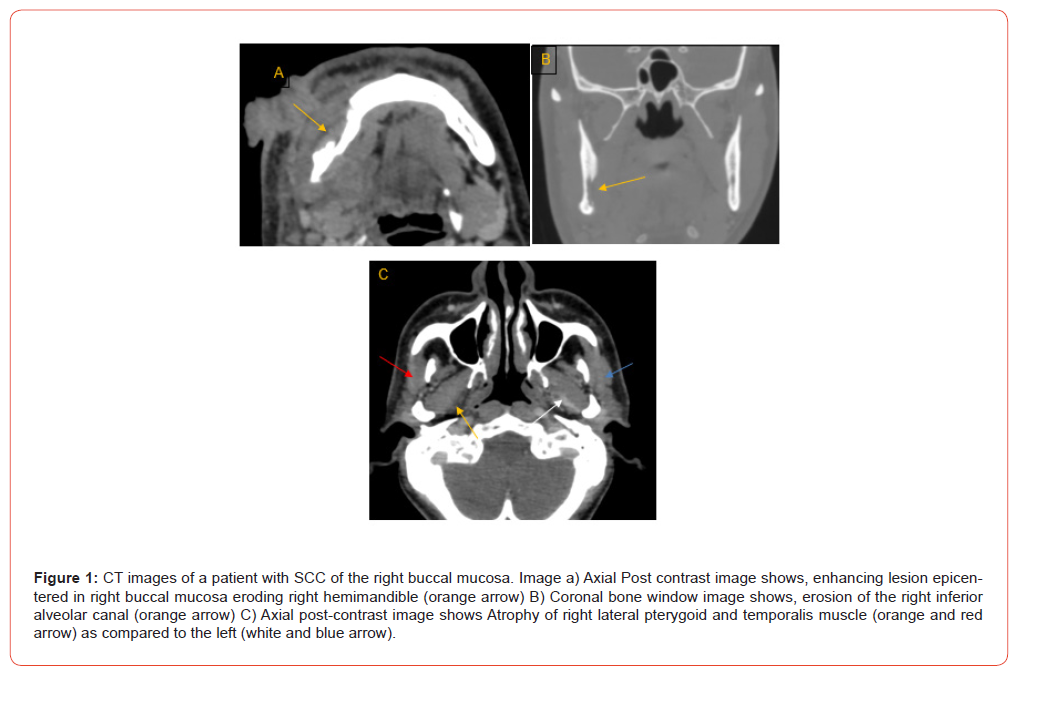
Here Place Table in document Images acquisition was done before and after 50ml of iodinated contrast administration. Axial, sagittal, and coronal reformations were performed in both bone and soft tissue windows.
Data Analysis: CT findings for PNS such as nerve thickening, foraminal widening, and muscle atrophy were evaluated and reported by single Radiologist and finalized by two senior Radiologists (experience more than fifteen years). The different direct and indirect signs of PNS were looked for, and spread if any present was noted, before looking for extensions. The maxillary nerve’s extension was looked for at inferior orbital canal, greater and lesser palatine foramen, pterygopalatine fossa, Foramen Rotundum and Cavernous sinus. The mandibular nerve can extend to Inferior alveolar nerve or canal, Mandibular foramen, Infratemporal fossa (ITF), Foramen ovale, Meckels cave and cavernous sinus. The presence or absence of nerve enhancement, nerve thickening, foraminal widening or erosion, loss of fat and denervation changes in muscle were noted. Histopathology served as the reference standard, and reporting was done by a senior pathologist (experience more than twelve years) from post-surgical specimen.
Statistical Analysis
Statistical analysis included Sensitivity, Specificity, Positive Predictive value (PPV), and Negative Predictive value (NPV) calculations, along with correlation analysis between PNS, TNM staging, and subsites. Chi-squared test was used for group comparisons for categorical data. In case the expected frequency in the contingency tables was found to be <5 for >20% of the cells, Fisher’s Exact test was used instead.
Observation and Result
All available data of 100 patients in the form of pathological specimens, image characteristics and clinical course were reviewed. Most patients were in age group of 41-50 years, followed by 51-60 years, and 31-40 years (Table 1). Out of 100 patients, the majority were male (90%), with an average age of 50 years. Most patients presented with oral or tongue ulcers (75%), while other symptoms included restricted mouth opening (8%) and palpable masses (7%) (Table 2). Most common subsite involved was buccal mucosa (48%), followed by tongue (23%), retro-molar trigone (10%), lower alveolus (7.0%), gingiva-buccal sulcus (6.0%), floor of mouth (4.0%) and hard palate (2.0%) (Table 3). Out of 100 patients, 36 had T4A, 22 had T4B, 25 had T2, 10 had T3 and 7 had T1 Radiological T stage (Table 4). Out of 100 patients, 43 had N0, 26 had N1, 19 had N2B, 6 had N2A, 4 had N2C, 1 had N3A and 7 had N3B Radiological N stage (Table 5).
Table 1:Distribution of participants according to age.
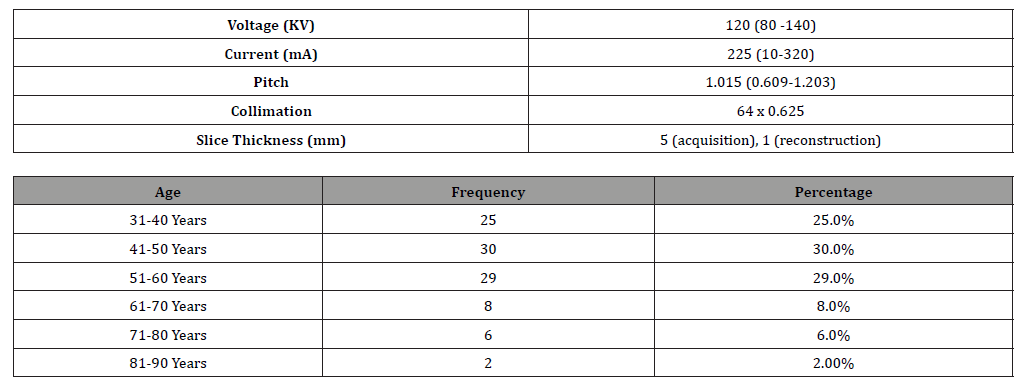
Table 2:Distribution of participants in terms of ‘Chief Complaint’.
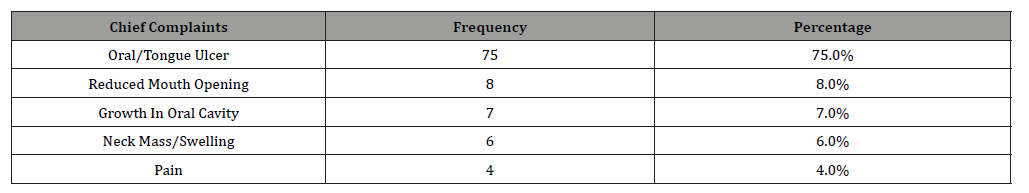
Table 3:Distribution of Participants in Terms of ‘Subsite’.
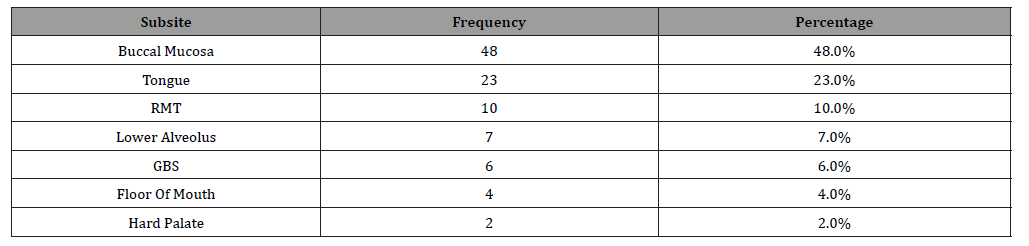
Table 4:Distribution of participants in terms of ‘Radiological T Stage’.
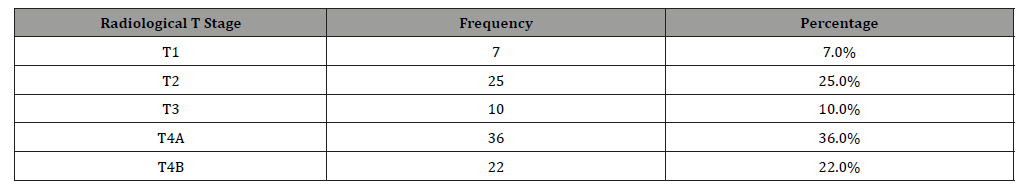
Table 5:Distribution of participants according to ‘Radiological N Stage’.

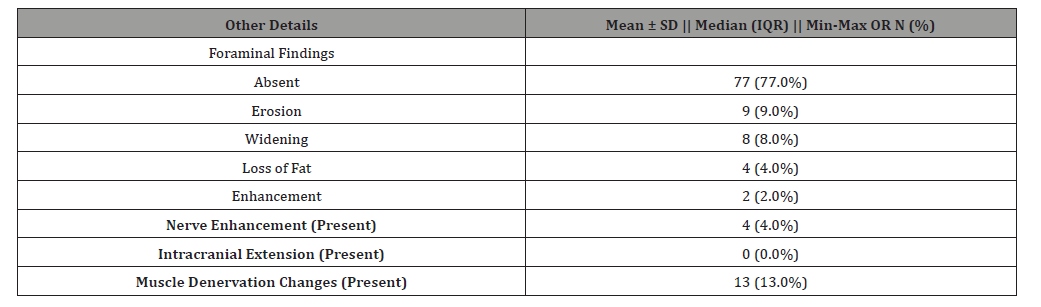
24 out of 100 patients had PNS on CT (Table 6, Figures 1-5), whereas 26 of 100 patients had histopathologically proven PNS. The two methods agreed in 88.0% of the cases and disagreed in 12.0% of the cases. There was a statistically significant agreement between the two variables, with kappa value of 0.680. Sensitivity, specificity, PPV, NPV and diagnostic accuracy of CT images for the detection of PNS were 73.1%, 93.2%, 79.2%, 90.8% and 88% respectively (Table 7). The most common nerve involved was mandibular nerve followed by maxillary nerve. Strongest predictors of PNS included foraminal widening, nerve thickening, and muscle denervation (Table 8).
Table 6:Comparison of Perineural Spread (CT) with Perineural Spread (HPE).
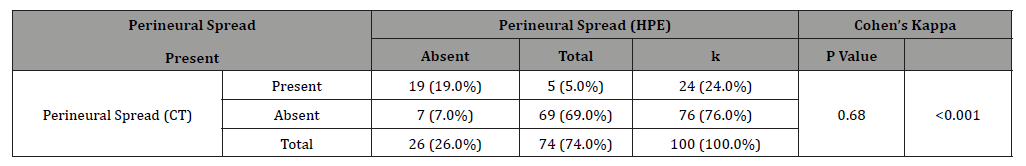
The two methods agreed in 88.0% of the cases and disagreed in 12.0% of the cases.
There was a statistically significant agreement between the two variables (Cohen’s Kappa = 0.680, p = <0.001). As per statistical convention, a kappa value of 0.680 denotes Substantial agreement.
Table 7:Sensitivity, specificity, PPV, NPV, PLR & NLR of CT in detecting perineural spread with HPE of post-surgical specimen as reference.
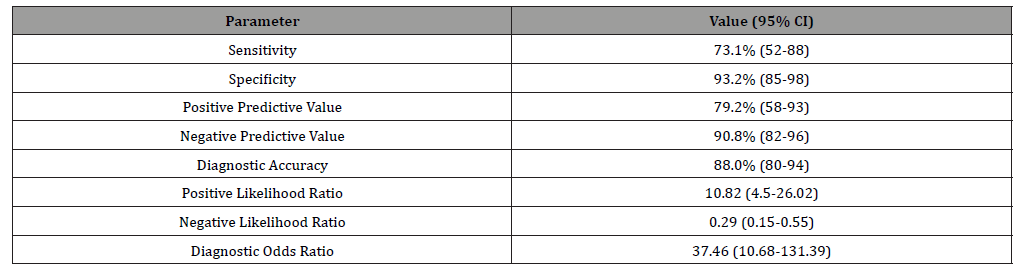
Table 8:Distribution of participants according to CT findings of perineural spread.
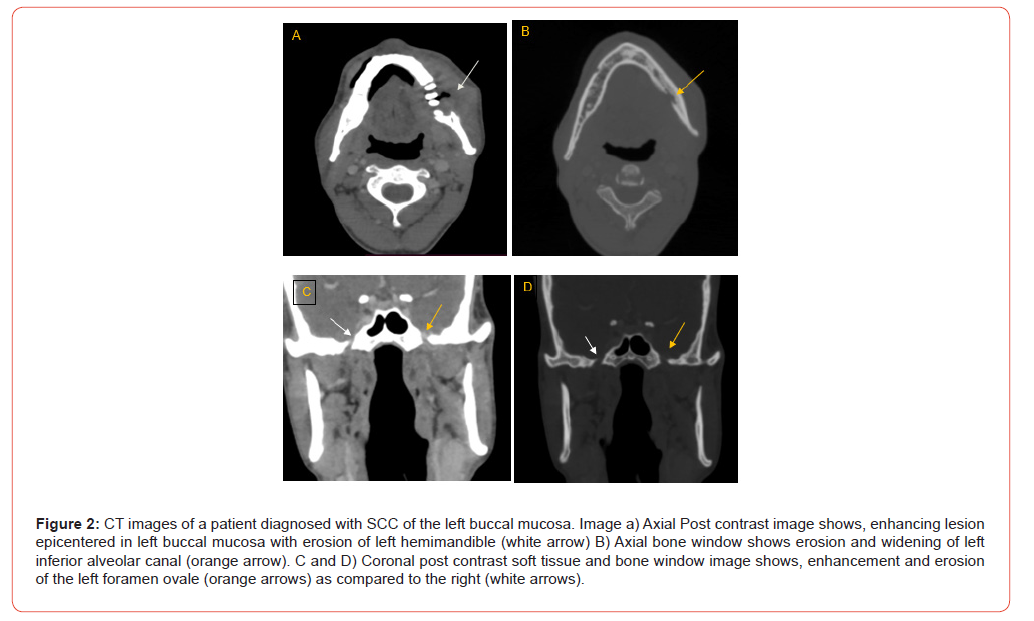
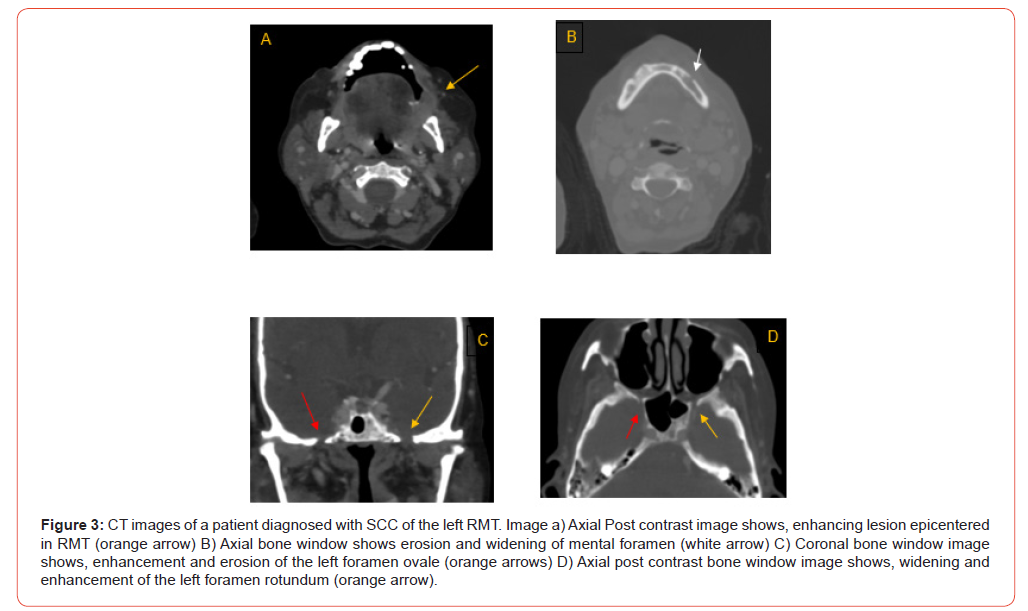
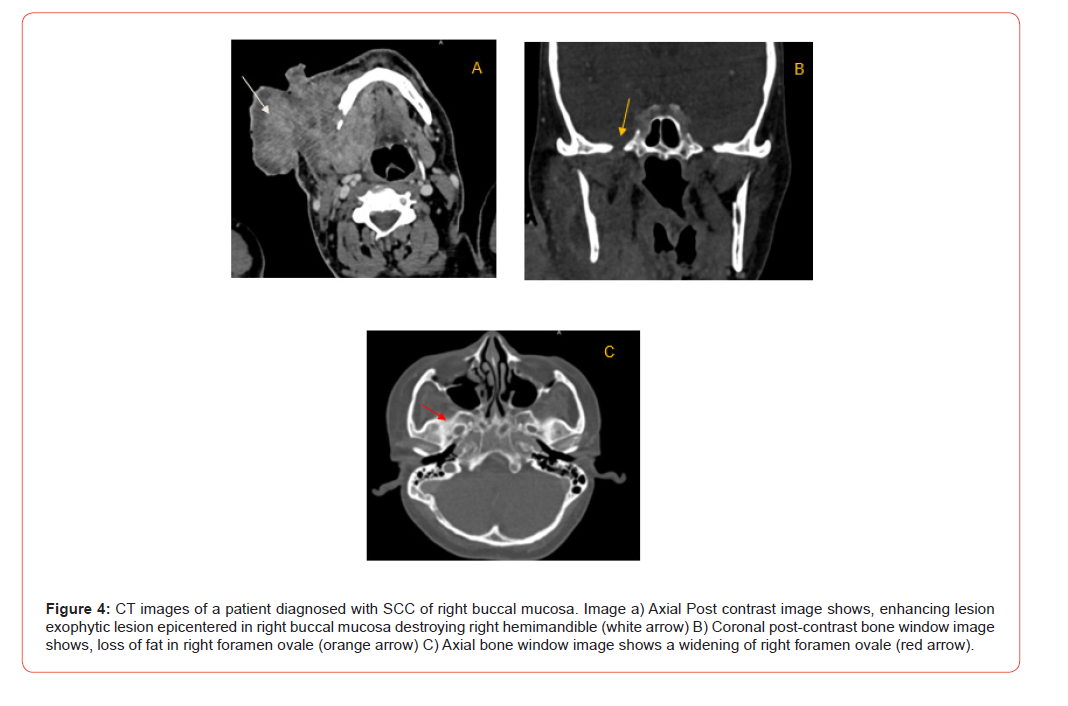
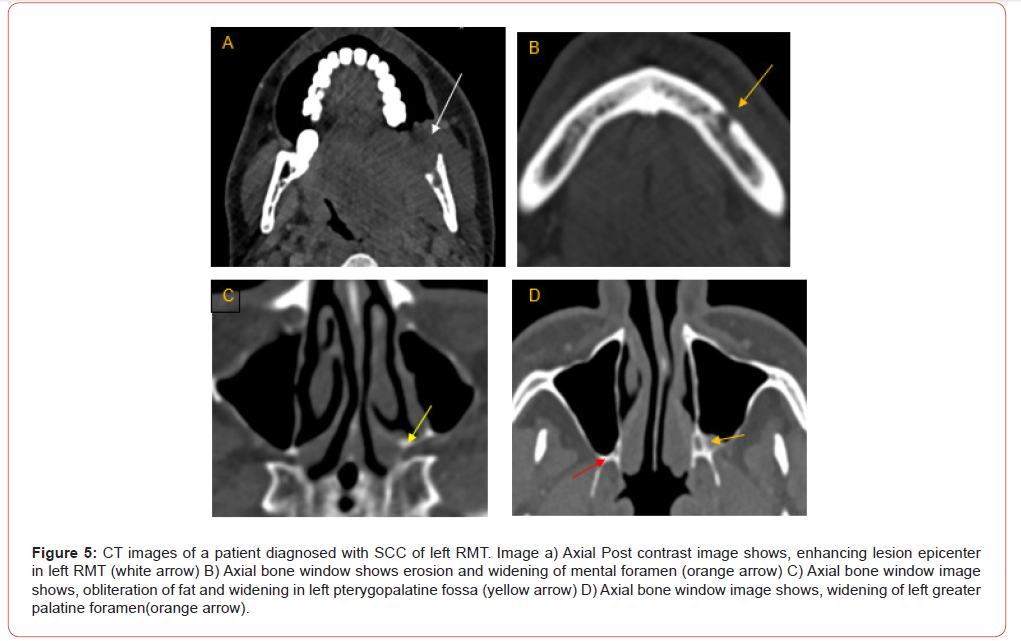
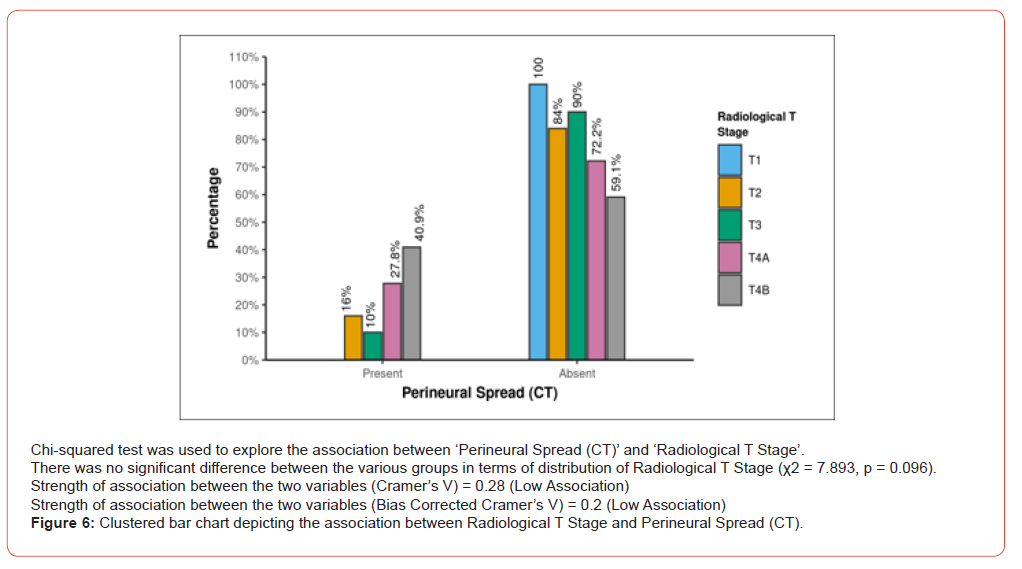
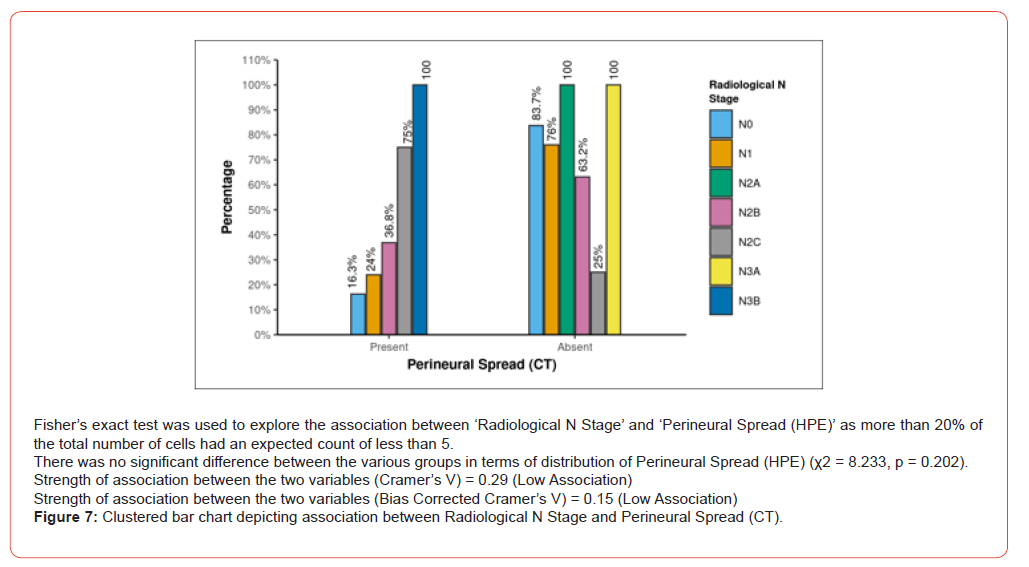
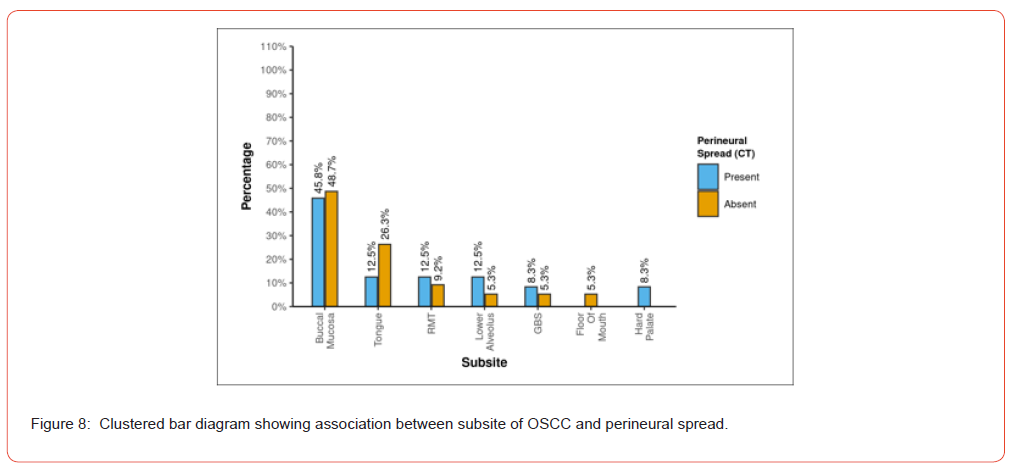
Analysis of TNM staging indicated that advanced-stage tumors (III and IV) showed a higher prevalence of PNS. However, statistically, no significant relation was seen between the T and N stage of tumour and presence of PNS (Figure 6 and 7). Anatomical patterns revealed that PNS was most common in the buccal mucosa, followed by tongue, retro-molar trigone, alveolus, gingiva-buccal sulcus and hard palate (Figure 8).
Discussion
This study highlights CT as a practical and efficient diagnostic tool for PNS detection in OSCC, especially in settings where MRI is unavailable. OSCC has a high tendency to spread along nerves. In this study, the prevalence was found to be 24 % which aligns with several previous studies. For instance, Schiff BA, et al in 2013 found PNS incidence of 20.3% [9]. Our study included cases that prospectively underwent surgery (excluding the supranotch T4b disease). This could have resulted in low incidence of PNS as compared to study by Varsha BK, et al. in 2015, in which incidence of PNS was found to be as high as 40% [10].
With a sensitivity of 73.1%, specificity of 93.2%, PPV of 79.2%, NPV of 90.8%; CT achieved a diagnostic accuracy of 88% in identifying PNS. Comparing our findings with existing literature, prior studies have also acknowledged CT’s utility in detecting PNS. For instance, Mukherji SK, et al. reported a sensitivity and specificity of 88% and 83% respectively, for CT in identifying PNS in carcinoma oral cavity and tongue base [11]. Our study has low sensitivity and high specificity in comparison to study done by Mukherji SK, et al. This discrepancy could be, at least in part, because of imaging criteria they used to define PNS. In their criteria, they included aggressive tumour margins, invasion of the sublingual space, and direct adjacency of tumour to enhanced lingual vasculature in sublingual space. Another study by Shimamoto H, et al yielded slightly lower sensitivity for CT at 55% but achieved 100% specificity [12]. These variations may be attributable to small sample size, and imaging protocol, which influences CT’s diagnostic performance.
Our study, conducted within a larger, regionally specific patient population, addresses some of these limitations by presenting data relevant to Indian clinical landscape. This perspective is essential given the distinctive patient characteristics and healthcare accessibility challenges in the region. The significant number of false negative cases can be attributed to the fact that CT changes as foraminal widening and erosion appear late in course of spread.
Our study also highlights the relatively increase incidence of perineural spread with T and N stage of tumours. Perineural involvement is more frequent in advanced, recurrent, and highgrade tumors. However, statistically, there is a lack of a significant association between PNS presence and tumor T and N stages. In this study, while perineural invasion was recognized as an important histopathologic feature, researchers found no statistically significant association between PNS and TNM stage in their cohort of OSCC patients. The findings suggested that while PNS may correlate with prognosis, its presence did not consistently align with TNM staging, indicating that PNS can occur independently of primary tumor size, nodal involvement, or metastasis status in some cases, suggesting that PNS can occur across various stages of OSCC, which underscores the need for routine PNS evaluation, irrespective of TNM classification. The mandibular and maxillary nerves were identified as most common pathways involved in PNS, with characteristic CT findings including foraminal widening, bone erosion, and nerve thickening.
The study also aimed to identify patterns of PNS involvement across different anatomical subsites. Results showed that PNS along maxillary nerve was most frequently associated with OSCC in buccal mucosa, RMT, and hard palate; while PNS along mandibular nerve was more common in OSCC affecting buccal mucosa, RMT, lower alveolus, and tongue. These patterns align with studies by Parker GD, et al. [13] and Caldemeyer KS, et al. [14] which reported that OSCC spread along mandibular and maxillary nerves often follows primary tumors in these locations. Such findings are significant for surgical planning, as they highlight specific nerve pathways that may require more intensive examination and possible resection to achieve clear margins.
The ability of CT to detect characteristic findings of PNS, including foraminal widening, nerve thickening, and bone erosion, has critical implications for treatment planning in OSCC. Detecting these features on CT helps identify patients who may benefit from more aggressive surgical intervention or adjuvant therapies, such as radiotherapy, to reduce recurrence risk. Furthermore, PNS identification aids in subclassifying T4b OSCC cases into supranotch and infra-notch compartments, which has implications for surgical resectability and prognosis. Tumors with infra-notch involvement are more likely to be resectable, offering a more favourable outcome than supra-notch tumors, which frequently involve critical structures near skull base and are associated with poorer prognoses.
These findings suggest that while CT is a valuable initial modality for detecting perineural involvement, certain limitations in early detection remain. Specifically, the accuracy of CT in identifying PNS is limited by its reliance on visible anatomical changes, such as foraminal widening and erosion, which tend to appear in later stages of disease progression. Consequently, early PNS cases may evade detection on CT, as these subtle features often fall below the resolution capacity of standard imaging techniques.
Studies have shown, better sensitivity and specificity of Magnetic Resonance Imaging (MRI) in detecting perineural spread. It remains the superior modality for detecting subtle or early perineural involvement, due to its higher soft-tissue resolution. However, MRI’s relatively high cost and limited availability across India, and obtained accuracy of CT in diagnosing perineural spread, make CT an accessible alternative, especially for initial screening or in resource-constrained setting, where advanced imaging modalities are scarce. Thus, an active search for key radiological landmarks can help detecting PNS early, hence impacting both prognosis and quality of life of patients with oral squamous cell carcinoma.
Limitations
This study has several limitations. CT struggles with early PNS detection, relying on significant anatomical changes, and lacks soft tissue resolution of MRI, limiting its ability to detect subtle neural changes. Variability in equipment, imaging protocols, and observer interpretations affects diagnostic consistency. The single-centre study design, small sample size, and lack of MRI comparison reduce generalizability and comprehensive evaluation. Demographic constraints further limit the applicability of findings beyond the studied population. Additionally, false positives from CT anomalies like asymmetric foramina, and absence of longitudinal data, hinder correlations between initial findings and long-term outcomes, impacting diagnostic and prognostic accuracy.
Conclusion
Our findings demonstrate that CT is useful imaging modality for detecting perineural involvement, particularly in advanced cases. CT emerges as a robust tool for detecting perineural spread in OSCC, offering critical insights into its association with tumor staging and anatomical patterns. An in-depth neuroanatomical knowledge and active search for the key radiologic landmarks can predict PNS on CT. The ability of CT to detect PNS is clinically significant, as early identification of perineural involvement can impact treatment planning, including extent of surgical resection, and need for radiotherapy. Given the impact of PNS on treatment strategies and prognosis, it is mandatory to describe this condition when staging patients with oral cancers.
Ethical approval
All procedures performed in the studies involving human participants were in accordance with the Ethical Standards of the Institutional and /or National Research Committee and with the 1964 Helsinki Declaration and its later amendments or comparable Ethical Standards.
Informed Consent
Informed consent was obtained from all individual participants included in this study.
Financial Support and Sponsorship
None.
Acknowledgement
None.
Conflict of Interest
No conflict of interest.
References
- Akashanand, Zahiruddin QS, Jena D, Ballal S, Kumar S, et al. (2024) Burden of oral cancer and associated risk factors at national and state levels: A systematic analysis from the global burden of disease in India, 1990-2021.Oral Oncology 159: 107063.
- Caldemeyer KS, Mathews VP, Righi PD, Smith RR (1998) Imaging features and clinical significance of perineural spread or extension of head and neck tumors. Radiographic 18(1): 97-110.
- Mahajan A, Agarwal U, Patil VM, Patil V, Vaish R, et al. (2022) Proposed sub-compartmentalization of high infratemporal fossa involvement in gingivobuccal cancers and its impact on clinical outcome and staging: A narrative review. Cancer Res Stat Treat 5: 269-275.
- Liao CT, Lee LY, Hsueh C, Lin CY, Fan KH, et al. (2013) Comparative outcomes in oral cavity cancer with resected pT4a and pT4b. Oral Oncol 49(3): 230-236.
- Liao CT, Ng SH, Chang JTC, Wang HM, Hsueh C, et al. (2007) T4b oral cavity cancer below the mandibular notch is resettable with a favorable outcome. Oral Oncol 43(6): 570-579.
- Mohiyuddin SMA, Harsha P, Maruvala S, Sumanth KR, Suresh TN, et al. (2018) Outcome of compartment resection of locally advanced oral cancers extending to infratemporal fossa: A tertiary rural hospital experience. Eur Arch Otorhinolaryngol 275(11): 2843-2850.
- Trivedi NP, Kekatpure VD, Shetkar G, Gangoli A, Kuriakose MA (2015) Pathology of advanced buccal mucosa cancer involving masticator space (T4b). Indian J Cancer 52(4): 611-615.
- Kumar A, Singh R, Santhosh M, Vijay S, Surendran N, et al. (2021) Role of structures in the masticator space in selecting patients with resectable T4b oral cancer: Findings from a survival analysis. Int J Oral Maxillofac Surg 50(5): 579-584.
- Schiff BA, Fried MP, Undavia S, Talavera F (2023) Perineural Spread of Tumor Along the Fifth and Seventh Cranial Nerves.
- Varsha BK, Radhika MB, Makarla S, Kuriakose MA, Kiran GVV S, et al. (2015) Perineural invasion in oral squamous cell carcinoma: Case series and review of literature. J Oral Maxillofac Pathol 19(3): 335-341.
- Mukherji SK, Weeks SM, Castillo M, Yankaskas BC, Krishnan LA, et al. (1996) Squamous cell carcinomas that arise in the oral cavity and tongue base: can CT help predict perineural or vascular invasion? Radiology 198(1): 157-162.
- Shimamoto H, Chindasombatjaroen J, Kakimoto N, Kishino M, Murakami S, et al. (2012) Perineural spread of adenoid cystic carcinoma in the oral and maxillofacial regions: Evaluation with contrast-enhanced CT and MRI. Dentomaxillofac Radiol 41(2): 143-151.
- Parker GD, Harnsberger HR (1991) Clinical-radiologic issues in perineural tumor spread of malignant diseases of the extracranial head and neck. Radiographics 11(3): 383-399.
- Caldemeyer KS, Mathews VP, Righi PD, Smith RR (1998) Imaging features and clinical significance of perineural spread or extension of head and neck tumors. Radiographics 18(1): 97-110.
-
Bibek Keshari, Pankaj Sharma*, Amit Kumar Tyagi, Sanjeev Kishore and Santosh Kumar. Investigating Perineural Spread in Oral Squamous Cell Carcinoma Using Computed Tomography in Resource Constrained Setting. On J Otolaryngol & Rhinol. 7(5): 2025. OJOR.MS.ID.000675
-
Oral squamous cell carcinoma, Computed tomography, Neuroanatomical knowledge, Tumor, Oral cancers, Skull base, Maxillary nerve, Head and neck, Soft tissue, CT scan
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






