 Research Article
Research Article
Service Evaluation of Paediatric Dental Patients Seen at Urgent Dental Care Hubs During the Initial COVID-19 Lockdown
Jasmine May Cachia Mintoff1*, Andrea Aspinall2, Susan Yadin3, Prabhleen Anand4 and Susan Parekh5
1Eastman Dental Hospital, Department of Paediatric Dentistry, London, United Kingdom
2Eastman Dental Hospital, Department of Paediatric Dentistry, London, United Kingdom & Central London Community Healthcare NHS Trust, Dentistry, London, United Kingdom
3Central London Community Healthcare NHS Trust, Dentistry, London, United Kingdom
4Eastman Dental Hospital, Department of Paediatric Dentistry, London, United Kingdom
5Eastman Dental Hospital, Department of Paediatric Dentistry, London, United Kingdom
Jasmine May Cachia Mintoff, Eastman Dental Hospital, Department of Paediatric Dentistry, London, United Kingdom.
Received Date: August 09, 2021; Published Date: September 01, 2021
Abstract
Introduction: Following closure of routine dental services in England on 23rd March 2020 due to the COVID-19 pandemic, NHS England commissioned Urgent Dental Care Hubs (UDCHs). The purpose of this service evaluation was to assess management of paediatric patients seen at two UDCHs; Eastman Dental Hospital (EDH) and Central London Community Healthcare (CLCH) during the lockdown period.
Standards: 100% patients managed according to appropriate guidelines.
Method: Retrospective analysis of cases between 1st April-15th May 2020.
Results: 393 patients seen across both sites (306 EDH, 87 CLCH).
• CLCH saw more face-to-face patients (46%) than EDH (19%)
• Most common reason for appointment was pain (43% EDH, 47% CLCH).
• Trauma was managed appropriately (95% EDH, 100% CLCH)
• Antibiotics were generally prescribed appropriately (81% EDH 89% CLCH), with incorrect prescribing due to reduced doses of amoxicillin
Discussion: Attendance increased as lockdown progressed. Fewer paediatric patients accessed the UDCHs compared to adults. Antibiotics were prescribed as an outcome in 19% EDH and 22% CLCH. Several patients (n=15) who were prescribed antibiotics received multiple courses or further treatment during the evaluation period.
Conclusion: This service evaluation showed that, at short notice, both dental services successfully provided emergency assessments and treatment within the context of a pandemic. Management of patients, on the whole, was appropriate, in keeping with standards set for the COVID-19 period. Antibiotic prescribing did not meet the appropriate standard. These initial results would be useful to help shape future care provision, should there be another lockdown.
Keywords: COVID-19; Service evaluation; Urgent Dental Care Hubs
Abbreviations: UDCH-Urgent dental care hubs; NHS-National health service; AGPs-Aerosol generating procedures; EDH-Eastman dental hospital; CLCH-Central london community health care; CDS-Community dental service; SDCEP-Scottish dental clinical effectiveness programme; FGDP-Faculty of general dental practice; GA-General anaesthetic; GDP-General dental practitioner
Introduction
Following the closure of all routine dental services in England as a result of the COVID-19 initial lockdown, NHS England commissioned Urgent Dental Care Hubs (UDCH) across England to provide only urgent dental care [1]. This consisted of remote consultation, and included [2, 3]
• Risk assessment and triage
• Advice, analgesia or antimicrobials, in line with guidelines (AAA)
• Booking face-to-face consultation and/or treatment-if appropriate
• Avoidance of Aerosol Generating Procedures (AGPs) unless absolutely necessary
The Eastman Dental Hospital (EDH) and Central London Community HealthCare (CLCH) Community Dental Service (CDS) were both commissioned as UDCHs. The Eastman was commissioned as a “hot and cold” hub site to include treatment of COVID-19 symptomatic and asymptomatic patients, CLCH solely as a “cold site”. Guidance and policies were issued when services were initiated, and continually updated in line with government guidance. We conducted a service evaluation during the period of lockdown, when General Dental Practices were closed. We used standards taken from the original version of the NHS England document on UDCH provision [1]. Reasons for emergency appointments should be swelling, severe pain affecting eating and sleeping and dental trauma [3]. We aimed to analyse the number of children with acute dental problems who accessed these hubs, their presenting dental problems and clinical management.
Specifically, we assessed antibiotic prescribing, using SDCEP and FGDP prescribing guidance during COVID-19 as the accepted standard [4], FGDP, 2020. A major concern was limited access to any dental General Anaesthetic (GA) services and for children whose pain or infection could not be managed with antibiotics and analgesics alone [5]. We therefore aimed to examine courses of antibiotics prescribed and if this adequately managed the dental complaint. Types of dental trauma presenting, and management was also analysed, utilising recent guidance as the accepted standard [6, 7]. Additional objectives were to compare sites to examine possible differences in emergency hubs between acute and community settings. Results of the service evaluation were shared between Trusts. It is anticipated that these results and learning points will also be applicable to many other paediatric dental services both in primary care and the acute settings across the country.
Methods
This evaluation was a retrospective evaluation of case notes completed by two dental clinicians (JM and AA). A standardised data collection proforma was designed and reviewed within both Trusts for approval. Data was collected over 6 weeks (1st April-May 15th, 2020). This time period was chosen as the community UDCH was commissioned to start on April 1st whereas the EDH emergency hub started on March 23rd. All paediatric dental patients seen during this period were reviewed barring those seen at the CLCH out of hours service. This service was not included in the service evaluation as it was partly commissioned independently to the UDCHs. Data was compared like for like with the Eastman over the same number of days and hours.
Standards
• 100% of patients were managed according to appropriate guidelines including trauma guidelines
• 100% of patients were prescribed antibiotics for the correct reasons
• 100% of patients were prescribed the correct dose of antibiotics
Data collected
Data Collection included:
• Date of appointment
• Route of referral
o The EDH accepted referrals via a self-referral form via NHS111, completed by either the patient or general dentist, as well as self-referral of current patients
o The CLCH accepted referrals via NHS 111 or self-referral of current patients
• Telephone or face-to-face appointment
• Reason for the appointment
• Diagnosis
• Outcome
• Antibiotics prescribed.
If antibiotics were prescribed the type and dose prescribed were recorded, and this was reviewed against national guidance to assess compliance [4] FGDP, 2020. The reasons taken as inappropriate were pain with no mention of swelling, dental abscess and/or no systemic signs. If any areas of ambiguity existed, results were discussed between both dental examiners and a paediatric dental consultant for consensus. Data was analysed using MS Excel.
Results
A total of 393 patients were managed across both UDCHs.
Eastman dental hospital
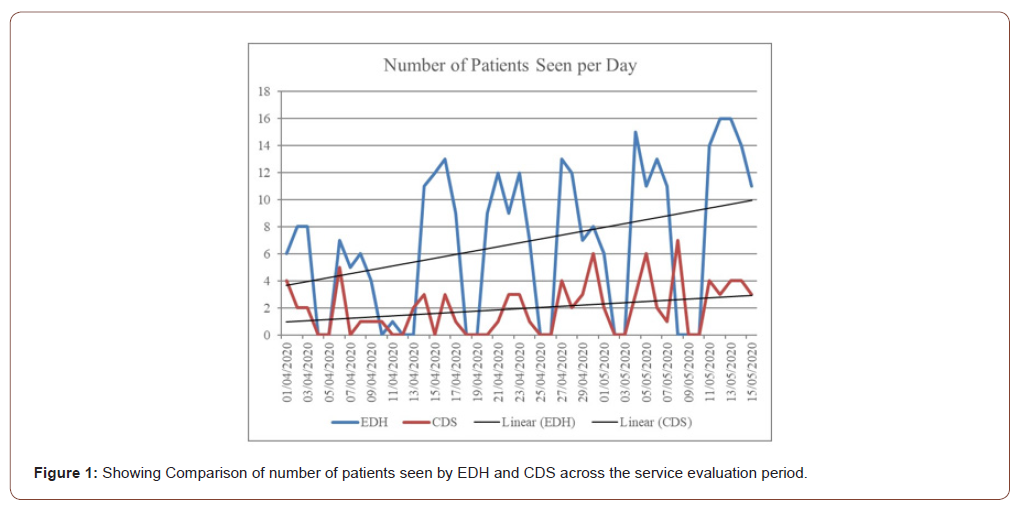
Between 1st April-15th May 2020, 185 patients were seen over 306 appointments. Ages ranged from 3 weeks to 19 years old (mean age 7.6 years). The majority of patients (n=155, 83%) were fit and healthy. The remaining 17% had a variety of medical conditions including asthma, autism, diabetes, kidney disease cerebral palsy and epilepsy. From 306 appointments, only 19% (n=58) were faceto- face appointments in clinic, the remaining 81% (n=249) were telephone appointments. Only one family was seen in the ‘hot’ area, with the mother (as opposed to the patient) being suspected to be COVID-19 positive. The number of cases seen increased from an average of 3.3 per day in week one to 14.2 in week 6. Most patients were seen mid-week on Wednesday and Thursday (Figure 1). Of the 58 patients seen, 15 needed treatments under inhalation sedation.
Referral source: Thirty-two percent (n=60) were EDH patients, 20% were referred by NHS 111, 27% were self-referred by parents using the self-referral form and 25% from other pathways including General Dental Practitioner (GDP), CDS, A&E or the Oral Maxillofacial Department.
CLCH
Seventy-six patients were seen over 87 different appointments. Ages ranged from 1 to 16 years (mean age 7.1 years). The majority of patients (78%) were fit and healthy, with 22% of patients having varying medical conditions including asthma, autism, ulcerative colitis, and previous leukaemia. Overall, 46% (n=40) of appointments were face-to-face and 54% (n=47) were telephone appointments. The number of cases seen increased from an average of 1.8 per day in the first week to 2.8 in the last week, with most patients again seen mid-week (Figure 1).
Referral source: The majority of patients were referred by NHS 111 (78%, n=59) and 20% (n=17) were CDS patients. The final patient was referred by their paediatrician.
Comparison between hubs
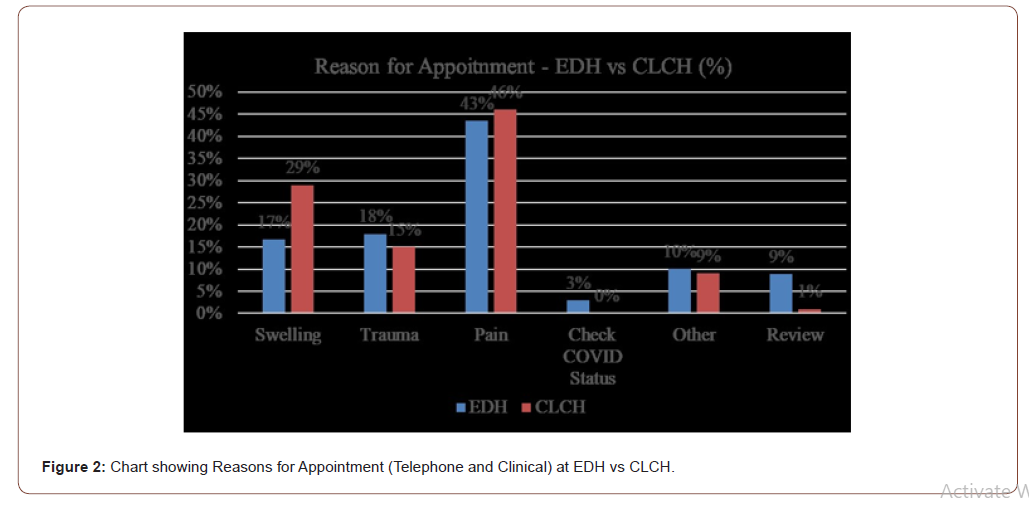
Reason for appointment: In both hubs, pain was the most common reason for appointment. Reasons for appointment varied, as shown in (Figure 2).
Those patients not meeting urgent dental care criteria specified in the Royal College of Surgeons recommendations [3] included:
• 4% of patients at EDH whose presenting complaints were a cyst, existing patients querying when treatment will continue or neonatal teeth.
• 5% of patients at CLCH whose presenting complaints were orthodontic concerns or lost restorations.
Outcomes
Table 1 shows the breakdown of outcomes by appointment at EDH compared to CLCH. The main outcome across both sites was advice only followed by advice and antibiotics. (Table 1) shows that very few AGPs (2%) were carried out at EDH and none at CLCH during this period. For patients with multiple outcomes, all were prescribed antibiotics and either had a temporary restoration or a failed extraction. The other category included:
Table 1: Comparison of Outcome by Appointment between EDH and CLCH.
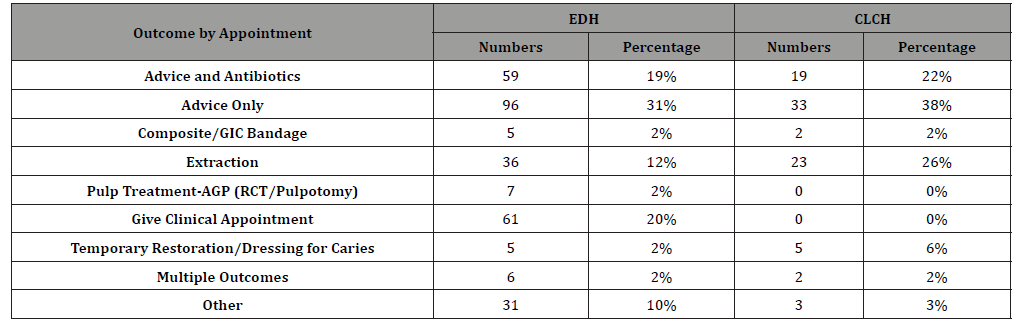
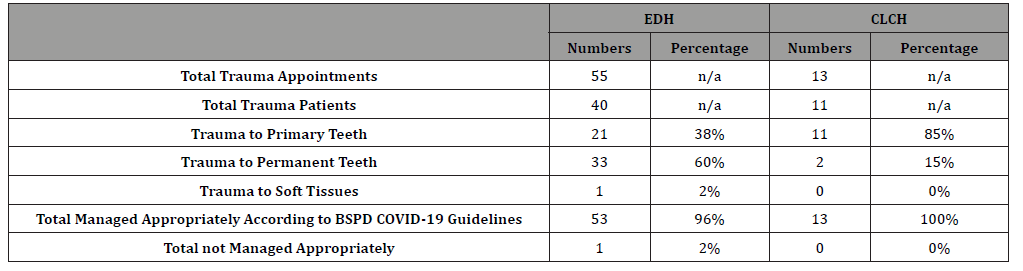
Table 2: Comparison of Trauma appointments between EDH and CLCH.
• Failed extractions/ restorations
• Placement/ removal splints
• Denture repair
• Placement on GA list
• Fluoride varnish
• Orthodontic wire cut
• Discharged
Management of trauma patients was compared to BSPD COVID-19 trauma guidelines. (Table 2) shows the data for trauma patients seen at EDH and CLCH. The EDH patient who was not managed according to trauma guidelines was a vertical crown-root fracture in the primary dentition. A restoration was attempted due to lack of GA services.
Antibiotic prescribing
In total, 86 prescriptions for antibiotics were dispensed. The most commonly prescribed antibiotic was amoxicillin (73%, n=45 at EDH; 89%, n=17 at CLCH), followed by metronidazole (19%, n=12 at EDH and 11%, n=2 at CLCH). At EDH co-amoxiclav was prescribed for 2 patients (2%) and the remaining 5% (n=3) were prescribed both amoxicillin and metronidazole.
Patients prescribed antibiotics inappropriately according to criteria were:
• EDH: 19% (n=12)
• CLCH: 11% (n=2)
Patients prescribed incorrect dose of antibiotics:• EDH: 8% (n=5), for 2% of cases, the dose was not recorded.
• CLCH: 47% (n=17)
At both hub sites, several patients who were prescribed antibiotics either by their GDP or the UDCHs (n=15 at EDH; n=3 at CLCH) went on to have further treatment, including extractions and endodontics.
Additional comparisons
For EDH patients presenting with pain, 30% were prescribed antibiotics, followed by telephone advice (28%), with only 20% receiving face-to-face treatment. Conversely, in CLCH, 48% of patients in pain had face-to-face treatment, whilst only 10% were prescribed antibiotics and 40% were given telephone advice.
Swelling was the second most common reason for appointment in CLCH (28%) and third most common at EDH (17%). The majority of these patients across both hubs were prescribed antibiotics and given advice (61% at EDH and 68% in CLCH). The remaining patients across both sites received treatment, all of which were extractions except for two extirpations in EDH. This was deemed appropriate treatment across both hub sites. Only 32% of the patients at EDH and 24% in CLCH were followed up after the course of antibiotics; all were asked to re-contact the UDCHs if the swelling did not resolve.
Trauma was the second most common reason for referral to EDH (18%) and third most common reason in CLCH (15%). The ratio of primary trauma to secondary trauma varied across both sites, with EDH seeing more secondary tooth trauma (60%) compared to CLCH, who saw more primary dentition trauma (85%). The majority of secondary tooth trauma in EDH was periodontal ligament (PDL) injury 55% compared to CLCH where the majority was hard tissue injury (66%). The primary tooth trauma across both sites showed a higher percentage of PDL injuries (69 and 56%) as would be expected [8].
Discussion
In this evaluation a significant number of patients were seen at both UDCH sites at the onset of the COVID-19 pandemic. The number of patients seen across both sites varied, with EDH seeing 3.5 times more patients. This would be expected as EDH is a larger service, with more clinicians. CLCH did have capacity for seeing more paediatric patients, but due to lack of demand, slots were not always filled. CLCH managed a higher proportion of face-to-face clinic appointments (46%) compared to the EDH (19%). A possible reason for this could be patients did not wish to attend an acute hospital setting in the middle of the pandemic.
Overall, the number of patients seen daily increased at both sites over time, with the rate of increase greater at the EDH. This could be explained by patients becoming more aware of the service and how to access it and/or becoming more comfortable to access care as lockdown progressed. The number of patients seen peaked mid-week, with low patient numbers on the Monday. This differs from what one would normally expect in emergency settings, where numbers increase after a weekend [9]. In CLCH this could be due to the out of hours service that operated over the weekend and some patients might have accessed that instead.
The overall numbers of paediatric patients accessing the UDCHs was lower than the number of adult patients both in CLCH and EDH. CLCH saw 245 adult patients during the same time period compared to 87 paediatric patients. This was similar to access to paediatric emergency care seen by our medical colleagues (Isba et al., 2020), where some have noted a disproportionately lower rate of presentations compared to adult services. This raises the question as to whether there are large numbers of paediatric patients with unmet dental needs that have not presented during the pandemic period. This could have been from lack of knowledge of how to access the UDCHs or parents not wishing to travel in the middle of a pandemic.
Autism was the most common medical condition seen at both sites. As a result of all elective GA lists being cancelled most of these patients were managed with advice and antibiotics. These patients may have required multiple courses of antibiotics and one case required an emergency GA that had to be arranged at Great Ormond Street Hospital. This highlights how the lack of access to GA services impacted our management. Surprisingly, despite the distinction of “hot” and “cold” hub sites, it was found that there was only one suspected COVID-19 positive case, who was the mother who had symptoms. This could be explained by preliminary evidence suggesting that children carry less of the virus and a lower percentage tend to contract the disease [10]. Children seem to be less infective overall, which suggests we may need to think about tailoring services differently for children.
Referral source varied across both hubs with the EDH seeing more of their own patients (32%) and self-referrals (27%), whilst most of CLCH patients came from NHS 111 (78%). This could be because CLCH did not have the self-referral option and patients could only access the hub through NHS 111. Pain was the most frequent reason for appointments at both sites, (43% EDH, 47% CLCH). This is also seen in the literature with pain being the main reason for paediatric dental emergencies in Brazil and Belgium [11, 12]. Management of most of these cases was in line with national guidelines. However, one trauma case at EDH deviated from guidance [6], due to lack of access to GA.
Antibiotics
Antibiotics were prescribed frequently as an outcome as was expected in the pandemic [1-3]. The main antibiotic was amoxicillin followed by metronidazole, following SDCEP guidance. Inappropriate prescribing accounted for 19% of EDH and 11% of CLCH cases. The reasons taken as inappropriate were pain with no mention of swelling, dental abscess and/ or no systemic signs. A high percentage of incorrect dose prescribing (47%) was seen in CLCH compared to 10% in EDH. In all cases the incorrect prescribing was too low a dose of amoxicillin for 5-11-year olds. In one case the low dose was corrected 2 days into the course of antibiotics. This incorrect dose prescribing has been similarly noted at the UDCH at Newcastle Dental Hospital [13].
As discussed by Zaitoun [5], the lack of GA services and the number of paediatric patients waiting for a dental GA means that one might expect some of these patients to suffer from multiple episodes of infection requiring antibiotics [5]. Of the patients prescribed antibiotics at both hubs, 10% of EDH patients and 36% of CDS patients were on a waiting list for a dental GA. From the patients having antibiotics, 6 EDH patients had multiple courses of antibiotics, whilst 2 known CLCH patients had multiple courses of antibiotics (both of these were waiting for a dental GA). This was often poorly recorded in the notes and could therefore be an underestimate.
Strengths and limitations
To our knowledge this is the first service evaluation comparing community and hospital emergency hub services, for paediatric dentistry, during the COVID-19 pandemic. The large numbers reviewed across both services during this time period are a strength and suggest a moderate degree of validity. A service evaluation has been published by King’s College Hospital detailing the pathway used for management of paediatric emergency patients (n=34) [14]. Weaknesses include the lack of longitudinal follow up, in particular of those cases who received antibiotics or advice only.
Conclusion
This service evaluation showed that, at short notice, both dental services successfully provided emergency assessments and treatment within the context of a pandemic. Management of patients, on the whole, was appropriate, in keeping with standards set for the COVID-19 period. Antibiotic prescribing did not meet the appropriate standard, suggesting that further education and audit is required in this area. Longer term data on those prescribed antibiotics, where this may not have been the optimal treatment choice (e.g. lack of availability of GA/limiting access to AGPs) would be useful to help shape future care provision, should there be another lockdown [15, 16].
Acknowledgment
We would like to thank all the staff at the EDH and CLCH who helped contribute to this study as well as all the people affected by dental concerns during the COVID-19 pandemic.
Conflicts of Interest
The authors declare no conflict of interest.
References
- (2020) NHS England NHS Improvement. COVID-19 Guidance and Standard Operating Procedure: Urgent Dental Care Systems in the context of Coronavirus. NHS England, UK.
- (2020) Scottish Dental Clinical Effectiveness Programme: Management of Acute Dental Problems During COVID-19 Pandemic. Dundee: SDCEP, UK, 30th March 2020a.
- Claire Stevens, Helen Rodd Recommendations for Paediatric Dentistry during COVID-19 pandemic.
- Scottish Dental Clinical Effectiveness Programme. Drugs for the Management of Dental Problems During COVID-19 Pandemic. Dundee: SDCEP, UK, 11th May 2020b.
- Zaitoun (2020) COVID-19: implications for paediatric dental general anaesthetic services. London: Faculty Dental Journal.
- Peter Day, Serpil Djemal, Sondos Albadri (2020) Permanent Dentition Acute Management of Traumatic Injuries and Follow-up Care during the COVID-19 Pandemic, 2020b.
- Peter Day, Serpil Djemal, Sondos Albadri (2020) Primary Dentition Acute Management of Traumatic Injuries and Follow-up Care during the COVID-19 Pandemic, 2020a.
- DiAngelis AJ (2012) International Association of Dental Traumatology guidelines for the management of traumatic dental injuries: 1. Fractures and luxations of permanent teeth. Dent Traumatol 28(6): 2-12.
- (2013) Scottish Dental Clinical Effectiveness Programme: Emergency Dental Care; Dental clinical Guidance. Dundee: SDCEP, UK.
- Li X, Xu W, Dozier M, He Y, Kirolos A, et al. (2020) The role of children in transmission of SARS-CoV-2: A rapid review. Journal of Global Health 10(1).
- Martens L (2018) Paediatric dental emergencies: a retrospective study and a proposal for definition and guidelines including pain management. Eur Arch Paediatr Dent 19(4): 245-253.
- Shqair AQ (2012) Dental emergencies in a university pediatric dentistry clinic: a retrospective study. Braz Oral Res 26(1): 50-56.
- Sumner O, Datta S (2020) Age-appropriate antibiotics. Br Dent J 228: 1-810.
- Ilyas N, Agel M, Mitchell J (2020) COVID-19 pandemic: the first wave-an audit and guidance for paediatric dentistry. Br Dent J 228: 927-931.
- (2016) Faculty of General Dental Practitioners. Antimicrobial prescribing for General Dental Practitioners. London: FGDP, UK.
- Isba R (2020) Where have all the children gone? Decreases in paediatric emergency department attendances at the start of the COVID-19 pandemic of 2020. Arch Dis Child 105(7): 1-704.
-
Jasmine May Cachia Mintoff, Andrea Aspinall, Susan Yadin, Prabhleen Anand, Susan Parekh. Service Evaluation of Paediatric Dental Patients Seen at Urgent Dental Care Hubs During the Initial COVID-19 Lockdown. On J Dent & Oral Health. 4(5): 2021. OJDOH. MS.ID.000600.
-
Dental structure, Dental caries, Dental vital bleaching, Teeth, Enamel morphology, Dental anomalies, Dental bleaching, Oral health, Anterior teeth.
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






