 Review Article
Review Article
The Multi-Artery Fractional Flow Reserve (FFR) Method in The Percutaneous Coronary Intervention (PCI) Practice
Ilan A Yaeger, Department of Cardiology, Israel, Email: ilan.yaeger41@gmail.com
Received Date: March 11, 2020; Published Date: April 13, 2020
Abstract
Current single-artery FFR-oriented coronary stenosis severity assessment methods (resting Pd/Pa, wave-free iFR and hyperemic FFR) are used successfully in single vessel disease (SVD) cases. In such cases the stenotic artery is in an independent stand-alone position with a proximal intracoronary aortic driving pressure. The treatment decision criteria of each method (FFR threshold value and FFR ‘grey range’) apply to FFR of the artery (denoted FFRtrue) which is the remnant fraction left in the stenotic artery of the calculated virtual blood flow of the very same artery prior to the onset of stenosis. As FFRtrue can be expressed in terms of the total stenotic resistance Rs of the artery and the microvascular resistance Rmv associated with the artery, FFRtrue can be also justifiably regarded as an ad-hoc intrinsic property of the stenotic artery. It doesn’t change unless the artery undergoes revascularization, turning its FFRtrue to nearly 1.00. The general scenario however encountered in the PCI practice is one in which a stenotic artery interconnects with other stenotic arteries and it is no longer in an independent stand-alone position since inter-arterial stenosisstenosis interactions take place. Due to this substantial change of circumstances, treatment decision criteria no longer apply to FFRtrue of an artery, rather to its actual FFR (denoted FFRreal).
The multi-artery FFR method is not intended to constitute a substitute for any of the current FFR-oriented methods. As single-artery FFRoriented methods cannot resolve complex scenarios of interacting stenotic coronary arteries, in this article the novel multi-artery FFR method extends these methods to the multi-artery domain with no need to alter their associated experimental techniques nor their treatment decision criteria. Reduction of the mathematics to minimal number of simple formulas in this article enables the PCI practitioner to apply the formulas to measured intracoronary pressures in real time.
Keywords: Multi-artery fractional flow reserve; Fractional flow reserve; Percutaneous coronary intervention; Revascularization; Percutaneous transluminal coronary angioplasty
Abbreviations: FFR: Fractional Flow Reserve; PCI: Percutaneous Coronary Intervention; iFR: Instantaneous Wave-Free Ratio; CABG: Coronary Artery Bypass Graft; ISR: In-Stent Restenosis; DES: Drug-Eluting Stent; ST: Stent Thrombosis; MACE: Major Adverse Coronary Event; MVD: Multi- Vessel Disease; SVD: Single Vessel Disease
Introduction
Single-artery FFR-oriented methods
Upon encountering a coronary stenosis, the percutaneous coronary intervention (PCI) practitioner is faced with a familiar dilemma: Revascularization or Conservative Medical Treatment? An unjustified revascularization can expose the patient unnecessarily to risks. The risks of a coronary artery bypass graft (CABG) operation are well known. Stenting however has its own risks. Though in-stent restenosis (ISR) has been substantially diminished by using drug-eluting stents (DES), it has not been eradicated. Within a period of a year or two, in cases of simple lesions and without particular risk factors, the ISR rate is usually less than 5% [1]. In cases of complex lesions and additional risk factors however, double digit rates are not uncommon [2]. The sudden incidence of stent thrombosis (ST) is around 1% [3]. By the traditional PCI method, in each of the two extreme cases, the very low and the very high stenosis severity ranges, the decision from which the patient can benefit is obvious from visual inspection and can be readily made. It is in the intermediate stenosis severity range (30%-70% diameter stenosis) where visual stenosis severity assessment can be difficult due to the absence of a well-defined quantitative criterion. The PCI terrain was consequently ripe for the appearance of some FFR-oriented methods.
At the time of its inception, the hyperemic FFR method has conceptually revolutionized the field of coronary stenosis severity assessment [4]. In contrast to the traditional and essentially qualitative angiographic approach, the FFR method focused on a quantitative measure of the functional performance of the stenotic artery in a pharmacologically induced state of hyperemia. In this method the hyperemia state is mandatory, and the resulting microvascular resistance is minimal and stable while maximal dilatation of the coronary artery and of its associated microvasculature takes place. The hyperemic FFR index of a stenotic coronary artery is the currently available remnant fraction of the (calculated) original maximal blood flow through the artery in its virtual stenosis-free state, namely
FFR=Qs/Qo
Qs - blood flow through artery in stenotic state
Qo - blood flow through artery in a virtual stenosis-free state
As the hyperemic pressure and blood flow are in a linearity relationship, the FFR index is obtained experimentally from measurements of intracoronary pressures. If a single stenotic artery is exposed to the aortic pressure, and the venous pressure is assumed to be nearly zero, its hyperemic FFR index (denoted FFRtrue) is equal numerically to the ratio of the mean distal pressure Pd and the mean proximal aortic pressure Pa [4], namely
FFRtrue = Pd/Pa
FFRtrue of a single stenotic artery can be also expressed in terms of the total stenotic resistance Rs of the artery and its associated microvascular resistance Rmv:
FFRtrue = 1/(1 + Rs/Rmv)
In an experimental statistical study FFR-guided decision for
treatment of stenotic coronary arteries proved to be superior to
angiography-guided approach when the number of major adverse
coronary events (MACE) over a period of several years was taken
into consideration [4]. It was also found experimentally that
for a single stenotic artery a condition of FFRtrue<0.75 implies
a mandatory revascularization of the stenotic artery whereas
0.85
Despite the establishment of the superiority of the hyperemic FFR method over angiographic stenosis severity assessment in the FAME study [8], there is a grave downside associated with the 3 FFR-oriented methods - they do not take into account inter-arterial interactions as can be seen in the FAME study itself. The cases treated in that study were formally multi vessel disease (MVD) cases involving 2 or 3 major coronary arteries LAD, LCx and RCA. However, an inspection of the conditions of the FAME study reveals that cases of diseased LMCA were excluded from the study, leaving each of LAD and LCx arteries directly exposed to the aortic pressure. This fact rendered all 3 arteries independent of each other since the proximal pressure in each one was the full aortic pressure, and each was consequently treated in that study as an independent single vessel disease (SVD) case. The inevitable conclusion is that the basic hyperemic FFR method cannot yield a rigorous resolution of complex MVD cases. In recent years attempts have been made to study the effect of downstream stenoses on LMCA employing the hyperemic single-artery FFR method but since this method does not take into account inter-arterial interactions, those attempts provided only general quantitative results rather than rigorous resolution of stenotic coronary configurations involving LMCA on an individual case basis [9,10].
Multi-artery FFR method
The multi-artery FFR method made its first appearance online at the end of 2015 [11]. The method is based essentially on the familiar Kirchhoff’s laws of analogous direct-current circuits. It considers inter-arterial interactions and has demonstrated its capability to resolve a variety of 2-artery and 3-artery stenotic coronary configurations [12]. The method does not constitute a substitute for any of the current 3 single-artery diagnostic methods, it just provides the correct pressure-flow relationships in coronary configurations encountered in the PCI practice. As for the treatment-decision criteria of the multi-artery FFR method used in this article, a cut-off value of FFR < 0.75 with a ‘grey range’ of treatment-decision uncertainty of 0.75 ≤ FFR ≤ 0.85 , which are usually associated with the hyperemic single-artery FFR method, have been chosen. This choice of treatment-decision criteria has been made just for the establishment of a common basis for comparison purposes, but it does not imply in any way that the hyperemic FFR method is superior to the iFR or to the resting Pd/ Pa methods.
At this point it should be stressed that when a stenotic coronary artery is just by itself, in a stand-alone position, without possible influence by interconnected stenotic arteries, then the treatment decision criteria (FFR cut-off value and FFR ‘grey range’) apply to its FFRtrue. However when there are other stenotic arteries in connection with the stenotic artery under consideration, the flow through the stenotic artery is no longer determined just by its total stenotic resistance Rs and the resistance Rmv of the microvasculature associated with the artery (like in formula (3) here) but also by the influence of the other stenotic arteries. These arteries impede and reduce the blood flow through the stenotic artery compared to its blood flow in the virtual state of these arteries being stenosisfree. The multi-artery FFR is the appropriate method for resolving such scenarios and the treatment decision criteria no longer apply directly to FFRtrue , rather to FFRreal which is defined as the current remnant fraction left of the original blood flow Qo through the stenotic artery in the virtual state of all arteries being stenosis-free (including the artery under consideration):
FFRreal = Qs real/Qo
Qsreal - actual blood flow through the stenotic artery
Qo - blood flow through the artery when all arteries are virtually in stenosis-free state
FFRreal reflects the condition of the stenotic artery and obviously FFRreal ≤ FFRtrue.
This inequality is extremely important to the PCI practitioner. It indicates that FFRreal of an artery can be improved indirectly by revascularizing other arteries (that are interacting with the artery under consideration) but only up to a certain limit, because FFRtrue is the upper bound of FFRreal. If it is needed and if feasible, this restriction can be practically lifted by revascularizing the stenotic artery itself, thus turning its FFRtrue to nearly FFRtrue=1.00 (but even then, it does not necessarily imply FFRreal =1.00).
Being a relatively novel method, the multi-artery FFR method deals essentially with the salient features of stenotic coronary configurations. On the grounds of simplicity, it is assumed in the present article that collaterals are not involved with the arteries of these stenotic coronary configurations. At an advanced stage of coronary disease however, collaterals may assume a substantially significant role. The scenarios under consideration in this article are mostly of a stenotic unprotected LMCA with stenoses also in one or two downstream main arteries, occasionally combined with a stenotic small side branch as well as ‘mother’-’daughter’ configurations and a variety of other equivalent configurations as will be indicated in the various sections of the article.
Methodology - The Basic Essentials
The full extent of the mathematics associated with the multiartery FFR method will not be presented in this article, it is described in the various articles about the capabilities of the method that have been published in recent years [11-15]. For the convenience of the reader, a concise methodology is given in the supplementary Appendix A of this article. In this paragraph stenotic coronary configurations associated with various scenarios in the PCI practice will be presented and the basic formulas for obtaining their current status and condition (FFRtrue and FFRreal of each artery) will be given in terms of the measured intracoronary pressures at locations marked in the appropriate figures in the article. The condition of each artery is reflected by its FFRreal and it may be improved by revascularizing some other artery that impedes its blood flow. This potential improvement is limited by the inequality FFRreal ≤ FFRtrue which implies that if FFRtrue of an artery is low, not much can be gained by revascularizing other arteries and therefore the stenotic artery itself should be revascularized, if technically feasible and if hemodynamically justifiable. The formulas given in this paragraph constitute the first stage of the resolution of the stenotic coronary configuration associated with each of the scenarios presented in this paragraph. Further stages of the resolution process are presented in the supplementary Appendix A of the article. However, to experienced PCI practitioners sometimes the FFRtrue and FFRreal of each artery obtained in the first stage suffice for devising the appropriate strategy for the resolution of the configuration under consideration.
3-artery coronary configurations of sizable arteries
The most common 3-artery configuration of sizable coronary arteries encountered in the PCI practice is the unprotected [LMCA]- [LCx]-[LAD] configuration (Figure 1). In the general case, each one of the arteries of the configuration is potentially stenotic and the current status and condition of each artery can be obtained from the values of the measured intracoronary pressures at the locations marked in (Figure 1). The current condition of the arteries is given by the following formulas [13]:
FFRreal(1)=(P3d + P2d)/(2∙Pa)
FFRreal(2)=P2d/Pa
FFRreal(3)=P3d/Pa
By the FFRreal of an artery one can immediately tell if its condition is acceptable or not. Sometimes the condition of the configuration is unacceptable without a noticeable stenotic culprit artery, it is the combined effect of more than just one stenotic artery. It can be occasionally seen that each artery, if it were just by itself (in a standalone position), its condition would be acceptable but due to the interference of other stenotic arteries its blood flow is impeded to an unacceptable level.
The FFRtrue values of the arteries are given by the following formulas [13]:
FFRreal(1) = 1/{[2∙(Pa-Pp)]/(P3d+P2d) + 1}
FFRreal(2) = P2d / Pp
FFRreal(3) = P3d / Pp
The FFRtrue values of the arteries can be very useful to the PCI practitioner for devising a proper resolution strategy, especially by assessing the potential of optional revascularizations considering the inequality FFRreal ≤ FFRtrue (see Example 1 in Section 3.1).
It should be noted that sometimes 2-artery scenarios can be resolved by an equivalent 3-artery configuration of (Figure 1). Occasionally the first diagonal artery D1 is a sizable artery and sometimes the first obtuse marginal artery OM1 happens to be a sizable artery. Under such circumstances, if LMCA is stenosis-free (thus maintaining the aortic pressure as the driving pressure of the configuration), the formulas of this section can be applied for example also to the following 2 configurations:
1) [prox LAD]-[remainder LAD]-[sizable D1]
Artery 1=prox LAD; Artery 2=remainder LAD; Artery3=sizable D12) [prox LCx]-[remainder LCx]-[sizable OM1]
Artery 1=prox LCx; Artery 2=remainder LCx; Artery3=sizable OM1

A ‘mother’-’daughter’ scenario – resolution by an equivalent 3-artery configuration
In this scenario there is a sizable (‘mother’) artery and its small side branch (‘daughter’) artery, each one potentially stenotic (Figure 2). Due to size difference, clearly the inter arterial interactions in this configuration are completely different from the interactions in the 3-artery configuration of sizable arteries. On the same grounds, the small side branch is obviously affected by the sizable ‘mother’ artery but has no influence on the latter. This will manifest itself in the relevant formulas. It should be noted that it is assumed that the arteries preceding the ‘mother’ artery are stenosis-free so that the aortic pressure is maintained all the way to the proximal segment of the ‘mother’ artery. In (Figure 2) Artery 1 and Artery 2 constitute the sizable ‘mother’ artery: Artery 1 is the proximal segment of the ‘mother’ artery (all the way to the split-off point of the small side branch) whereas Artery 2 is the remainder of the ‘mother’ artery. Artery 3 is the small side branch in (Figure 2).
The current condition of the arteries can be obtained from the measured intracoronary pressures at the locations marked in Figure 2 [14]:
FFRreal (1) =P2d/Pa
FFRreal (2) =P2d/Pa
FFRreal (3) =P3d/Pa
The FFRtrue values can be also obtained from the measured intracoronary pressures [14]:
FFRtrue (1) =1/{[(Pa-Pp)]/P2d + 1}
FFRtrue (2) =P2d/Pp
FFRtrue (3) =P3d/Pp

As indicated already, FFRtrue of an artery does not change unless the artery is revascularized, in which case FFRtrue becomes nearly 1.00. The PCI practitioner can use the FFRtrue values for assessment of possible outcomes of optional revascularizations (Example2 in Section 3.2).
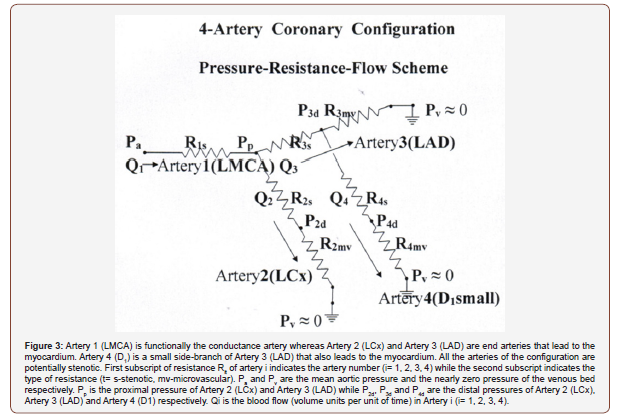
A complex 4-artery configuration
The configuration of Figure 3 consists of the familiar 3 sizable arteries, unprotected LMCA, LCx and LAD with an additional small first diagonal side branch D1. Due to the substantial differences in size, the sizable arteries can affect D1 but D1 cannot affect LAD nor any of the other sizable arteries. After performing intracoronary pressure measurements, the first step that the PCI practitioner must take in order to assess the current condition of each artery is calculating its FFRreal from the measured intracoronary pressures by the following formulas [13,14] (see Figure 3):
In order to make initial assessments regarding the outcomes of potential revascularizations, the PCI practitioner should calculate the current FFRtrue values for each artery in the configuration by the following formulas [13] (Figure 3):
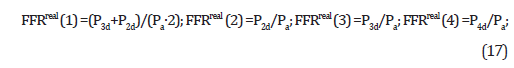
As indicated already, the FFRtrue of an artery remains constant unless the artery is revascularized, turning its FFRtrue to nearly 1.00. Note that FFRreal ≤ FFRtrue. This inequality states the simple fact that the blood flow through a stenotic coronary artery is highest when the artery is just by itself in the absence of interconnected stenotic arteries the interference of which can possibly impede and reduce the blood flow through the artery. FFRtrue therefore indicates the maximal FFRreal that the artery can have under best conditions of no interference at all and being exposed to aortic pressure. A low value of FFRtrue implies that the artery itself may be the culprit for its possibly unacceptable condition, therefore other directions of seeking an optimal resolution may deserve a lower priority. In the scenario described here, the 3 sizable arteries dominate the scene, therefore the partial 3-artery configuration [LMCA]- [LCx]-[LAD] (Figure 1) should be resolved first (Section 3.1) and only then the attention should turn to the small side branch D1. Once the PCI practitioner calculates the outcomes of the desired revascularizations within the 3-artery configuration of the sizable arteries (FFRtrue and FFRreal of each artery), their anticipated effect on the small side branch D1 should be figured out. As can be seen by the formulas in this section, FFRtrue and FFRreal of D1 are dependent on the intracoronary pressures at specific locations marked in (Figure 3). One needs to calculate the intracoronary pressures anticipated in the wake of the revascularizations planned by the PCI practitioner for the resolution of the 3-artery configuration of the sizable arteries. The anticipated intracoronary pressures in terms of FFRtrue of the arteries are the following (Appendix A):
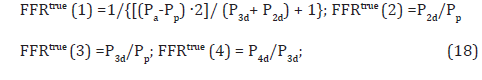
It should be noted that from the formulas it is obvious that FFRtrue of D1 (Artery 4 in (Figure 3)) does not affect the intracoronary pressures Pp , P2d and P3d within the 3-artery configuration of sizable arteries but P4d within the side branch D1 is affected by all the arteries. The predicted values of FFRtrue and FFRreal of D1 resulting from the implementation of some of the optional revascularizations can be obtained from the expressions for P3d and P4d because one has:

In Section 3.3 of this article Example 3 of a resolution of a 4-artery stenotic coronary configuration (Figure 3) by the multi-artery FFR method employing the formulas of the present section and simulated intracoronary pressures is presented in detail.
Results –Numerical Simulation Examples
Example #1 – Stenotic 3-artery configuration of sizable arteries (Figure 1)
The coronary configuration of (Figure 1) is (1) LMCA - (2) LCx - (3) LAD
In this configuration of sizable arteries each artery is potentially stenotic. The simulated intracoronary pressures in this case are the following (in units of mmHg):
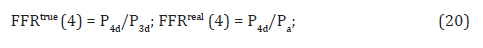
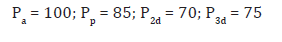
The FFRtrue values of the arteries here indicate that if each artery had been the only stenotic artery around, its condition would have been acceptable. The inter-arterial stenosis-stenosis interaction however severely impedes the blood flow through the configuration and renders its condition unacceptable. Obviously, revascularization is in order, but strategy is important too. Revascularization of LMCA, if considered by the PCI practitioner, should be usually carried out by a CABG operation (unless it is contraindicated due to circumstances). This will consequently not be the PCI practitioner’s first choice. Turning to the other two arteries, LCx and LAD, in search for a ‘candidate’ for revascularization, the practitioner should take a good look at the FFRtrue of each artery. It is true that the condition of an artery in a configuration is reflected by its FFRreal, not by its FFRtrue, but it is the inequality FFRreal ≤ FFRtrue that one needs to consider. If the number of stenotic arteries connected to an artery decreases (by revascularization), its FFRreal increases but the inequality indicates that this increase is limited since FFRtrue of an artery constitutes the upper bound of FFRreal. A glance at FFRtrue of LCx and LAD shows that FFRreal of LCx is more restricted than FFRreal of LAD (because FFRtrue (2) < FFRtrue (3)). It seems therefore more beneficial to revascularize LCx, increasing its smaller FFRtrue to nearly FFRtrue (2) =1.00.
The post-revascularization status of the arteries would be

It is evident that the condition of LAD artery is unacceptable. The condition of LAD has deteriorated since the blood flow in LCx competes with the blood flow in LAD. With the reduction of the stenosis in LCx to zero, increase of the blood flow in LCx results in some decrease of the flow in LAD.
It seems that LAD should be revascularized too. Revascularization of both LCx and LAD arteries yields the following results:
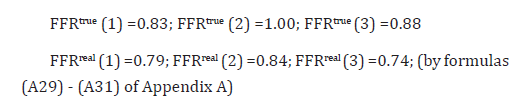
Evidently, the condition of the arteries of the configuration is acceptable and no revascularization of LMCA is required.
Example #2 – A ‘mother’-’daughter’ scenario resolved by an equivalent 3-artery configuration (Figure 2) of Section 2.2
The coronary configuration of (Figure 2) is (1) proxLAD - (2) remainderLAD - (3) smallD1
In this scenario the ‘mother’ artery is the LAD artery preceded by a non-stenotic LMCA. The aortic pressure Pa is therefore maintained all the way to the proximal segment of LAD. The LAD artery in the scheme of (Figure 2) is a combination of Artery 1 which is the proximal part of the LAD artery and Artery 2 which is the remainder of the LAD artery. It should be noted that each part of the LAD artery may be stenotic. Artery 3 represents the optionally stenotic small ‘daughter’ artery D1. The simulated intracoronary pressures in this example (in units of mmHg) are the following:
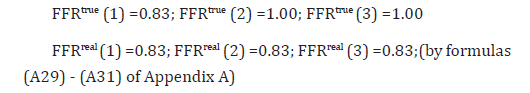
Calculated present status of the arteries:

It is obvious that the condition of both the ‘mother’ artery and the ‘daughter’ artery is unacceptable. In devising the proper strategy to resolve this scenario, the PCI practitioner has to take into account that due to the substantial difference in size, an event that takes place in the ‘mother’ artery affects also the condition of the ‘daughter’ artery but the opposite is not true. Namely, the ‘mother’ artery is not affected by whatever takes place in the ‘daughter’ artery. Also, it is obvious that stenting the proximal section of LAD artery (Artery 1 in Figure 2) exposes the remainder of LAD artery, as well as the D1 artery, to the aortic pressure. In such a case, just by the definitions of FFRtrue and FFRreal and without any further calculations one has:
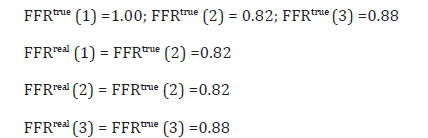
The condition of both the ‘mother’ and ‘daughter’ arteries is acceptable but should the PCI practitioner desire to further improve the condition of the LAD artery, the remainder of the LAD artery can be stented too, yielding (just by the definitions of FFRtrue and FFRreal):
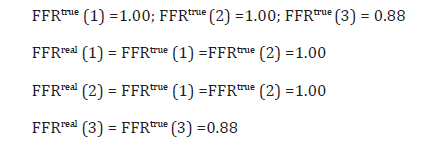
Evidently, this improves substantially the condition of LAD artery and provides an optimal resolution of this ‘mother’-’daughter’ configuration but at the ‘cost’ of one more revascularization.
Example #3 – A complex 4-artery configuration (Figure 3) – resolved by the formulas of Section 2.3
The coronary configuration of Figure 3:(1) LMCA - (2) LCx - (3) LAD – (4)D1(small): The simulated intracoronary pressures for this MVD case are the following (in units of mmHg):
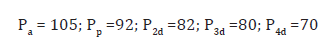
Note that FFRtrue of an artery is equal to the maximal FFRreal obtained if most favorable conditions are created. Present real condition of the arteries (see formulas (17)):
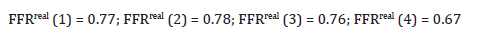
By the treatment criteria of the hyperemic FFR method chosen to be followed in this article, the condition of the 4-artery configuration of (Figure 3) is obviously unacceptable (one of the FFRreal values here is below the cut-off value of 0.75 whereas others barely exceed it). The PCI practitioner therefore needs to explore firstly the various revascularization options of the sizable arteries (that will be potentially also beneficial to the D1 artery) the outcomes of which can be predicted by formulas (A47) of Appendix A prior to possible implementation.
Revascularization Options
Revascularization option a:
From a glance at the present FFRtrue values of the arteries it seems that revascularization of Artery 3 (LAD) (Figure 3) could improve substantially its condition, as well as the condition of Artery 4 (D1) and possibly of other arteries too. LAD artery has the lowest FFRtrue of all the sizable arteries of the configuration so elevating its FFRtrue theoretically up to 1.00 (in practice it is somewhat less) could be most beneficial. In the optional revascularization of Artery 3 (LAD) therefore the FFRtrue values of the other arteries remain at their present values while FFRtrue (3) changes to 1.00:
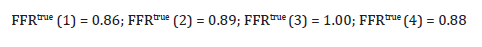
Using these values in formulas (A47) of Appendix A, the postrevascularization condition of the sizable arteries can be predicted:
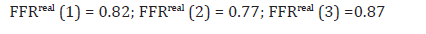
As expected, such a revascularization results in a substantial improvement of the condition of Artery 3 (LAD). Also, the condition of Artery 2 (LCx) remains the same (no change in its FFRreal) which is understandable since the blood flows in LAD and LCx are competing. The revascularization improves also the condition of Artery 1 (LMCA) because of the reduction in resistance to the outflow from LMCA. Let’s turn now to Artery 4 (D1) and calculate its anticipated distal pressure P4d following the optional revascularization described here. Using formulas (19) one has (in units of mmHg):
P4d = 80
This yields the condition of Artery 4 (D1) by formulas (20):
FFRreal (4) = 0.76
Which is a substantial improvement compared to its present condition but still barely acceptable. Note that FFRtrue (4) does not change since it is an intrinsic property of D1 which has not been revascularized and it remains FFRtrue (4) = 0.88.
If now artery D1 is revascularized, one has:
FFRtrue (4) = 1.00
The intracoronary distal pressure is
P4d = 91 (by formulas (19)) which yields
FFRreal (4) = 0.87
Revascularization option b:
Despite the potential improvement of the condition of several arteries, the downside of Revascularization option a is that the full potential of LMCA would not have been realized. The maximal FFRreal of LMCA is equal to its FFRtrue and this would not have been achieved. In the present revascularization option, the outcome of revascularizing both Artery 2 (LCx) and Artery 3 (LAD) will be therefore predicted. As the resistance to the outflow from LMCA would be drastically reduced, it is expected that such a revascularization would result in a substantial improvement of the condition of LMCA. Naturally, a substantial improvement would be also expected in the condition of arteries LCx and LAD, compared to their present condition. However, no significant improvement of the condition of D1 beyond the improvement that could have been obtained in Revascularization option a) is expected.
In the present optional revascularization, the FFRtrue values of the sizable arteries are the following:

As expected, if this revascularization option had been realized, there would have been a substantial improvement in the condition of all 3 sizable arteries (compared to their present condition) and the full present potential of LMCA would have been realized.
Turning now to Artery 4 (D1) one should take it into account that in the present revascularization option D1 artery is not involved directly therefore there is no change in its FFRtrue and it remains
FFRtrue (4) = 0.88
The post-revascularization value of P4d can be calculated (in units of mmHg) from formulas (19):
P4d = 79
FFRreal (4) can now be calculated from formulas (20):
FFRreal (4) = 0.75
As expected, the condition of Artery 4 (D1), should one carry out the present revascularization option, would be about the same as in Revascularization option a) which renders the condition of D1 barely acceptable.
If now artery D1 is revascularized, one has
FFRtrue (4) = 1.00 and the distal intracoronary pressure is
P4d = 90 (by formulas (19)) which yields
FFRreal (4) = 0.86
This renders artery D1 quite acceptable.
Conclusions from predicted outcomes of revascularization options
Since a CABG operation is usually the way for revascularizing LMCA, this is not to be taken lightly and such an option is therefore avoided here. Option b) yields better results than option a) regarding the 3 sizable arteries. The two revascularization options improve substantially the condition of Artery 4 (D1) compared to its present condition. Deplorably the improved condition of D1 is barely acceptable because of its low FFRreal, therefore stenting D1 would be beneficial, as shown here, if it is accessible geometrically (angle and diameter) and if it is functionally justifiable (namely if it is not too tiny to be hemodynamically of interest).
To conclude, under the circumstances, revascularization option b) (preferably combined with revascularization of D1) provides the optimal resolution of the stenotic 4-artery coronary configuration of (Figure 3).
Discussion
Single-artery FFR-oriented methods
About 25 years ago the emergence of the single-artery FFR method marked the dawn of a new era in the field of coronary stenosis severity assessment [1]. In contrast to the traditional visual and essentially subjective and qualitative stenosis severity assessment by the morphological appearance of the stenosis, FFRoriented methods are based on quantitative assessment of the functional performance of the stenotic artery. The 3 FFR-oriented single-artery methods, resting Pd/Pa ratio, induced-hyperemia FFR and free-wave iFR are all based on intracoronary pressure measurements under very specific conditions that maintain a linearity relationship between blood flow and pressure drop. Because of the different techniques involved in the 3 FFR-oriented methods, each method has its specific FFR threshold value and its FFR ‘grey range’ of treatment-decision uncertainty. A typical threshold usually employed with the resting Pd/Pa method is about 0.88 with a ‘grey range’ of about 0.88 ≤ Pd/ Pa ≤ 0.95 [16]. In the free wave iFR method, the threshold value is about 0.86 with a ‘grey range’ of about 0.86 ≤ iFR ≤ 0.93 [17]. As indicated already in this article, a threshold value in the hyperemic FFR method is about 0.75 with a ‘grey range’ of about 0.75 ≤ FFR ≤ 0.85 [5].
The 3 single-artery FFR-oriented coronary stenosis severity assessment methods are well designed to handle SVD cases, both simple cases with a single localized stenosis and more complex cases that involve serial stenoses within the same artery [18]. The phenomenon of collaterals has been also addressed by some of these methods [4]. However, the reality of the epicardial arterial network is in most cases much more complicated than that of a single artery. Initial attempts to study the effect of downstream stenoses (in LAD and LCx arteries) on unprotected LMCA by a single-artery approach have not yielded a rigorous resolution of stenotic unprotected LMCA-LCx-LAD configurations on a case to case basis, rather general quantitative results [9,10].
Multi-artery FFR method
The specific conditions under which the intracoronary pressure measurements are carried out in the single-artery FFRoriented methods maintain a linearity relationship between blood flow through a stenosis and the associated pressure drop over the stenosis. The epicardial arterial network is analogous to an electric interconnected network of conductors and resistors which implies that the rules that govern the relationship between the epicardial intracoronary pressures and blood flow are analogous to Kirchhoff’s laws of direct-current circuits. These analogous rules combined with appropriate mathematical transformations constitute the multi-artery FFR method which can practically extend each of the 3 single-artery coronary stenosis severity assessment methods to the multi-artery domain. This extension does not violate the basic experimental techniques nor the treatment-decision criteria of any of the single-artery methods. However, the virtual transition from the single artery ‘stand-alone’ position to the multi-artery scenario is in principle associated with a substantial change of circumstances. Therefore, in the multi-artery scenario these criteria no longer apply to FFRtrue of a stenotic artery, rather to its actual FFR, namely to its FFRreal that reflects the current condition of an artery. In a multi-artery coronary configuration, the FFRtrue of a stenotic artery assumes a new role, it is potentially the maximal possible FFRreal of the artery, FFRreal ≤ FFRtrue. This current maximal potential of FFRreal is fully realized if the aortic pressure is maintained all the way to the beginning of the stenotic artery. The potential is further increased if the stenotic artery itself is revascularized and its FFRtrue is turned into nearly 1.00. The most important aspect of the superiority of the multi-artery FFR method over the single-artery FFR-oriented methods is the inclusion of inter-arterial interactions.
The capability of handling stenotic coronary multi-artery configurations of interacting arteries was not available to the designers of the FAME study [8] in 2009. They chose to get around this obstacle by excluding cases of diseased LMCA from the FAME study. This exclusion rendered the LCx and LAD arteries independent of each other and reduced the seemingly MVD cases of the study practically to SVD cases and they were indeed treated as such in that study. The multi-artery FFR method emerged in 2015 [11] and the mathematical formulas for resolving the stenotic LMCA-LCx-LAD configuration (and other 3-artery configurations of sizable arteries) were finalized in 2017 [13]. Nevertheless, there are still researchers that apply the ‘exclusion principle’ to cases of diseased LMCA in their statistical studies even in 2020 [19] thus losing unnecessarily invaluable statistical data that would have potentially affected the results of those studies. What may have been understandable under the circumstances in 2009 should not be acceptable in 2020.
Current obstacles and future perspectives
Theoretically the multi-artery FFR method seems superior to the single-artery FFR-oriented methods by the mere inclusion of inter-arterial interactions. However, it should be noted that the analogy between the epicardial arterial network and an electric interconnected network of conductors and resistors is not complete. Resistors are discrete components whereas stenoses are not always localized. LMCA stands out as an example. The plaque in LMCA is often diffusely distributed and in most cases protrudes also partly into the neighboring LCx and LAD arteries [20]. Under such circumstances, when the boundaries of a diffuse plaque are not well-defined, the accuracy of the FFRtrue and FFRreal values obtained by the multi-artery FFR method is reduced. This can be alleviated to some extent by measuring separately the proximal intracoronary pressure of LCx artery and the proximal intracoronary pressure of LAD artery and regarding their arithmetic average as the common proximal intracoronary pressure of arteries LCx and LAD [15] (Pp in Figure 1).
It should be noted that it would be beneficial to have the quality of revascularizations of stenotic arteries checked postrevascularization by the PCI practitioner in limiting cases (by the same kind of intracoronary pressure measurements that preceded the revascularizations) so that operational conclusions can be drawn if necessary. In the numerical examples in this article (3. Results – Numerical Simulation Examples) it has been assumed that the FFRtrue value of a revascularized artery is 1.00 but, it might be less, as indicated already. In this context note that possible different results of the FFRreal values of the arteries due to such a variation of FFRtrue can be observed in Example 3 when outcomes of Revascularization option a) (with FFRtrue(2)=0.89 ) and Revascularization option b) (with FFRtrue(2)=1.00 ) are considered. On the practical level, the multi-artery FFR method is very convenient. Firstly, the PCI practitioner can readily identify to what category belongs the arterial scenario encountered in the catheterization laboratory. Then the practitioner turns to the right pressure-resistance-flow scheme and measures the appropriate intracoronary pressures. This experimental data is then used with the relevant formulas of paragraph 2. Methodology – The Basic Essentials in order to obtain the current values of FFRtrue and FFRreal of each artery of the arterial scenario. At this point it is important not to be led astray by the values of FFRtrue and FFRreal of an artery. Arteries with a reasonable FFRtrue may end up with a very low and unacceptable FFRreal. This should not come as a surprise because unlike in the SVD case, the presence of each additional stenotic artery in the configuration impedes further the blood flow through the multi-artery system.
It is important to comprehend the meaning of FFRtrue and FFRreal. The initial FFRreal (prior to possible revascularizations) reflects the current condition of an artery and therefore regardless of the FFR-oriented method that is being used, hyperemic FFR or instantaneous free-wave iFR or resting Pd/Pa , the treatmentdecision criteria should be applied to FFRreal , rather than to FFRtrue . If the value of FFRreal is less than the FFR threshold value associated with the method that is being used, the condition of the artery is unacceptable. At this point, it would be beneficial to take also a good look at the numerical value of FFRtrue obtained for each artery since this may point the way to devising the most appropriate revascularization strategy on the way to optimal resolution of the stenotic coronary configuration. FFRtrue indicates potential, not condition. It is the upper bound of possible FFRreal for the artery that can be obtained by revascularization of other arteries. If the value of FFRtrue of an artery is too low, there is no alternative but to revascularize the artery itself (turning its FFRtrue to nearly 1.00), provided that it is technically feasible and that the artery is hemodynamically sufficiently important to the coronary blood circulation. Such a revascularization provides direct relief to the artery or enables potential relief through optional revascularization of other arteries.
There are two downsides of the multi-artery FFR method that involve strategy. Firstly, the method does not (and actually cannot) consider the exact location of stenoses. Assuming a same FFRreal, a stenosis in the proximal section of an artery potentially puts at risk more downstream side branches than a stenosis in the distal section of an artery. Such a matter can be taken into consideration only by a PCI practitioner who can weigh the importance of such a state of a configuration. Secondly, when the PCI practitioner is confronted with an unfavorable numerical value of FFRreal of an artery then if FFRreal is below the lower end of the ‘grey zone’ of the FFR treatment decision range then it is undisputedly not acceptable. However, if FFRreal is within the ‘grey zone’ or slightly above it, it is up to the PCI practitioner to decide what can be regarded ‘safe’ for the patient under consideration, regarding also future prospects given the patient’s way of life, and if revascularization would be a clinically justifiable ‘price’ for it. Although the multi-artery FFR method provides the PCI practitioner with precise data about the status of a configuration (namely FFRreal and FFRtrue of each artery), in order to devise a strategy of handling a complex stenotic coronary configuration, professional experience and careful judgement on the part of the PCI practitioner are virtually irreplaceable.
In some cases, the final stages of the procedure, predicting the outcomes of optional revascularizations, are obvious to the experienced PCI practitioner. However, should the practitioner nevertheless choose to continue following closely the multi-artery FFR method in the footsteps given in this article (Appendix A), the appropriate formulas are relatively simple and can be used by the PCI practitioner in real time or incorporated for convenience into a software application module. Note that such a software application module should enable constant scrutiny from the PCI practitioner who inputs the data (measured intracoronary pressures, FFRtrue values, optional FFRtrue values, as appropriate) and the output data (FFRtrue and FFRreal values) should be presented in raw form for direct evaluation by the practitioner. The practitioner can use his/ her past experience from SVD cases in order to visually estimate FFRtrue of arteries and so rudimentarily verify the validity of the output data from the software application module to be assured that the output data is flawless and very likely reflects reality (note however that FFRreal of an artery may be substantially different from estimated FFRtrue and therefore cannot be used for verification purposes).
It should be noted that the intracoronary pressure values used in the numerical simulations for the demonstration of the capabilities of the multi-artery FFR method [11-14] have been all taken from the experimental intracoronary pressure range encountered in the catheterization lab. The obvious current advantage of the multiartery FFR method is therefore the possible smooth transition from the use of simulated intracoronary pressures to the use of real intracoronary pressure data obtained in the catheterization lab.
Conclusion
The current FFR-oriented methods (resting Pd/Pa, wave-free iFR and hyperemic FFR) are single-artery methods that cannot resolve stenotic multi-artery configurations in which inter arterial interactions take place. The multi-artery FFR method extends these methods to the multi-artery domain without imposing any changes in the experimental technique of any of these methods nor in the treatment decision criteria (FFR threshold value and FFR ‘grey range’) of any of them. The multi-artery FFR method is not intended to constitute a substitute for any of the current single-artery FFRoriented methods. It however provides these methods with the necessary capabilities for resolving stenotic multi-artery coronary configurations.
Acknowledgement
None.
Conflict of Interest
No conflict of interest.
References
- Sarno G, Lagerqvist B, Frobert O, Nilsson J, Olivecrona G, et al. (2012) Lower risk of stent thrombosis and restenosis with unrestricted use of 'new-generation' drug-eluting stents: a report from the nationwide Swedish Coronary Angiography and Angioplasty Registry (SCAAR). Eur Heart J 33: 606-613.
- Dangas GD, Claessen BE, Caixeta A, Sanidas EA, Mintz GS, et al. (2010) In-Stent Restenosis in the Drug-Eluting Stent Era. J Am Coll Cardiol 56: 1897-1907.
- Iakovou I, Schmidt T, Bonizzoni E, Ge L, Sangiorgi GM, et al. (2005) Incidence, Predictors, and Outcome of Trombosis After Successful Implantation of Drug-Eluting Stents. JAMA 293: 2126-2130.
- Pijls NH, van Son JA, Kirkeeide RL, De Bruyne B, Gould KL (1993) Experimental basis of determining maximum coronary, myocardial, and collateral blood flow by pressure measurements for assessing functional stenosis severity before and after percutaneous transluminal coronary angioplasty. Circulation 87: 1354-1367.
- Petraco R, Sen S, Nijjer S, Echavarria-Pinto M, Escaned J, et al. (2013) Fractional Flow Reserve-Guided Revascularization – Practical Implications of a Diagnostic Gray Zone and Measurement Variability on Clinical Decisions. JACC Cardiovasc Interv 6: 222-225.
- Sen S, Escaned J, Malik IS, Mikhail GW, Foale RA, et al. (2012) Development and validation of a new adenosine-independent index of stenosis severity from coronary wave-intensity analysis: results of the ADVISE (Adenosine Vasodilator Independent Stenosis Evaluation) study. J Am Coll Cardiol 59: 1392-1402.
- de Waard GA, Danad I, Petraco R, Driessen RS, Raijmakers PG, et al. (2018) Fractional flow reserve, instantaneous wave-free ratio, and resting Pd/Pa compared with [15O] H2O positron emission tomography myocardial perfusion imaging: a PACIFIC trial sub-study. Eur Heart J 39: 4072-4081.
- Tonino PAL, De Bruyne B, Pijls NHJ, Siebert U, Ikeno F, et al. (2009) Fractional Flow Reserve versus angiography for guiding Percutaneous Coronary Intervention. N Engl J Med 360: 213-224.
- Fearon WF, Yong AS, Lenders G, Toth GG, Dao C, et al. (2015) The impact of downstream coronary stenosis on fractional flow reserve assessment of intermediate left main coronary artery disease: human validation. JACC Cardiovasc Interv 8: 398-403.
- Daniels DV, van’t Veer M, Pijls NHJ, van der Horst A, Yong AS, et al. (2012) The Impact of Downstream Coronary Stenoses on Fractional Flow Reserve Assessment of Intermediate Left Main Disease. JACC Cardiovasc Interv 5: 1021-1025.
- Yaeger IA (2016) A multi-artery Fractional Flow Reserve (FFR) approach for handling coronary stenosis-stenosis interaction in the multi-vessel disease (MVD) arena. Int J Cardiol 203: 807-815.
- Yaeger IA (2015) Practicability of Multi-Artery Fractional Flow Reserve (FFR) Method in the Assessment of Some Stenotic Coronary Artery Configurations in Percutaneous Coronary Intervention (PCI) Procedures. Interv Cardiol J 2(3): 31.
- Yaeger IA (2017) Resolution of All-stenotic 3-Artery Configurations in Percutaneous Coronary Intervention (PCI) Procedures by the Multi-artery Fractional Flow Reserve (FFR)Method. Cardiovasc Investig 1(1): 2.
- Yaeger IA (2018) Resolution of coronary ‘mother’-’daughter’ configurations by multi-artery FFR method – a comparison with basic FFR method. Interv Cardiol 10: 65-71.
- Yaeger IA (2019) Strategies of Handling a Stenotic Unprotected Left Main Coronary Artery by Multi-Artery Fractional Flow Reserve Method. On J Cardiovas Res 1(4): 1-7.
- Ammar KA, Kazmi SS, Ahmad MN, Ahmad MM, Riaz A, et al. (2016) Use of Resting Non-hyperemic Indices for Avoidance of Fractional Flow Reserve Measurement: The Goal of 100% Accuracy. J Invasive Cardiol 28: 265-270.
- Petraco R, Escaned J, Sen S, Nijjer S, Asrress KN, et al. (2013) Classification performance of instantaneous wave-free ratio (iFR) and fractional flow reserve in a clinical population of intermediate coronary stenoses: results of the ADVISE registry. EuroIntervention 9: 91-101.
- De Bruyne B, Pijls NHJ, Heyndrickx GR, Hodeige D, Kirkeeide R, et al. (2000) Pressure-Derived Fractional Flow Reserve to Assess Serial Epicardial Stenoses Theoretical Basis and Animal Validation. Circulation 101: 1840-1847.
- Wijntjens GWM, van de Hoef TP, Meuwissen M, Echavarría-Pinto M, Murai T, et al. (2020) Prognostic implications of resting distal coronary-to-aortic pressure ratio compared with fractional flow reserve: a 10-year follow-up study after deferral of revascularization. Neth Heart J 28: 96-103.
- Oviedo C, Maehara A, Mintz GS, Araki H, Choi SY, et al. (2010) Intravascular Ultrasound Classification of Plaque Distribution in Left Main Coronary Artery Bifurcations – Where Is the Plaque Really Located. Circ Cardiovasc Interv 3: 105-112.
-
Ilan A Yaeger. The Multi-Artery Fractional Flow Reserve (FFR) Method in The Percutaneous Coronary Intervention (PCI) Practice. On J Cardio Res & Rep. 3(5): 2020. OJCRR.MS.ID.000573.
-
Physical activity, Exercise, Angiogenesis, Vascular Endothelial Growth Factor, Blood vessel, Neovascularization, Vasculogenesis, Hypertension, Atherosclerosis, Myocardial fibrosis, Heart disease, Cardiovascular disease
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






