 Research Article
Research Article
Complete Revascularization in a Time of Crisis: Why Treating Mild and Moderate CTCA-Detected Vulnerable Lesions was Lifesaving during the COVID-19 Pandemic
Prof. Dasaad Mulijono
Department of Cardiology, Bethsaida Hospital, Tangerang, Indonesia
Prof. Dasaad Mulijono, Department of Cardiology, Bethsaida Hospital, Tangerang, Indonesia
Received Date:October 02, 2025; Published Date:December 03, 2025
Abstract
Background: The COVID-19 pandemic profoundly disrupted cardiovascular care, exposing the limitations of stenosis-centric paradigms that
depend on ischemia or >70% narrowing to guide intervention. SARS-CoV-2 induced endotheliitis, pan-coronary inflammation, and hypercoagulability,
conditions that disproportionately destabilized plaques traditionally considered “insignificant.” This crisis highlighted the critical need to
recognize and treat vulnerable plaques rather than relying solely on luminal severity.
Objective: To present the scientific rationale, clinical outcomes, and broader implications of a vulnerability-guided, CTCA-directed complete
revascularization strategy implemented at Bethsaida Hospital during the COVID-19 pandemic, and to contextualize its acceptance and criticism
within the profession.
Methods: In an environment where IVUS, OCT, and NIRS were largely inaccessible, CTCA served as the primary modality for detecting high-risk
plaque (HRP) features, including low-attenuation plaque, napkin-ring sign, positive remodeling, and surface irregularity. Patients with CTCA-identified
vulnerability - regardless of stenosis severity - underwent preventive PCI or DCB treatment. The program integrated intensive lifestyle medicine,
notably a Whole-Food Plant-Based Diet (WFPBD), to promote systemic plaque stabilization.
Results: Among 3,500 COVID-positive or exposed patients with coronary artery disease, this strategy resulted in zero mortality - an outcome
unmatched in contemporary global registries. The approach demonstrated that stabilizing biologically high-risk, mild-to-moderate lesions prevented
myocardial infarction at a time when emergency rescue PCI was frequently unavailable. The program’s outcomes were later aligned with
emerging evidence from PROSPECT ABSORB, DEBuT-LRP, and the ongoing PREVENT trial, all of which support the concept of treating HRP before
symptomatic obstruction occurs.
Interpretation: The pandemic intensified pre-existing shifts in coronary science. AI-based vulnerability mapping, CTCA-first evaluation, and
lifestyle-driven endothelial restoration now outperform stenosis-based models for predicting risk. Discussions within the profession revealed differences
in exposure, training, and familiarity with plaque biology and lifestyle medicine, highlighting the need for broader education rather than
polarization. Ethical analysis indicates that crisis-era decisions were consistent with the principles of beneficence, non-maleficence, autonomy, and
justice.
Conclusion: The Bethsaida experience demonstrates that vulnerability-guided complete revascularization, supported by CTCA imaging and
systemic biological optimization through WFPBD, can prevent myocardial infarction and death even under extreme circumstances. COVID-19 revealed
a fundamental truth: stenosis predicts ischemia, but vulnerability predicts events. This crisis-validated paradigm - endorsed conceptually by
leading cardiovascular thinkers such as Braunwald and Fuster - signals the future of coronary care. The pandemic is over, but the biology it exposed
must guide practice moving forward.
Keywords:COVID-19; vulnerable plaque; CT-coronary angiography; complete revascularization; preventive PCI; plaque erosion; endotheliitis; hypercoagulability; artificial intelligence; lifestyle medicine; whole-food plant-based diet; crisis cardiology; biological risk
Introduction
The COVID-19 pandemic created an unprecedented collapse in cardiovascular care systems worldwide. Catheterization laboratories faced intermittent closures, emergency pathways were unreliable, and the pandemic’s inflammatory milieu profoundly destabilized coronary plaques. Traditional revascularization models - anchored to stenosis severity or ischemia testing - became increasingly inadequate and potentially unsafe. Decades of pathology have shown that most myocardial infarctions (MIs) originate from plaques with <50% stenosis, often undetectable by ischemia-driven strategies. COVID-19 magnified this biological reality. Endotheliitis, hypercoagulability, and pan-coronary inflammation drastically increased the likelihood of erosion or rupture in plaques traditionally considered “non-significant.” In this context, Bethsaida Hospital implemented a vulnerabilityguided complete revascularization (CR) program based primarily on CT coronary angiography (CTCA), treating even mild-tomoderate lesions when high-risk plaque (HRP) features were present. This strategy achieved zero mortality in 3,500 COVIDpositive or exposed patients, challenging conventional paradigms and providing a roadmap for future coronary care.
The Pandemic Exposed the Weaknesses of the Stenosis-Centric Model
The traditional threshold for PCI is to treat more than 70%
stenosis or demonstrable ischemia, which reflects a luminal, not
biological, understanding of coronary disease. Pathology and OCT
evidence consistently show:
a) 70–80% of culprit ACS plaques exhibit <50% stenosis.
b) Many are FFR-negative.
c) Their danger comes from thin caps, large lipid cores,
inflammation, and positive remodeling, not flow obstruction.
COVID-19 amplified this vulnerability. Autopsy and intravascular imaging studies revealed:
Plaque Erosion Dominated During COVID-19
Accounting for 50–60% of ACS, driven by SARS-CoV-2-mediated endothelial injury.
Plaque Rupture Persisted in Low-Stenosis Lesions
Often associated with positive remodeling and invisible on angiography.
Hypercoagulability Accelerated Thrombosis
Even minimal endothelial disruption became dangerous. Thus, plaques previously deemed “insignificant” became the most lethal substrates during COVID-19.
When Emergency Systems Collapse, Waiting for Ischemia is Unsafe
Pandemic-related system failures included [1-4]:
a) Cath lab closures
b) Delayed transfers
c) Staffing shortages
d) Fragmented emergency services
Under these conditions, the calculus changed dramatically. A plaque with HRP morphology could rupture at any moment, while the system might not be able to rescue the patient. Thus, preventive PCI became not aggressive - but protective. The logic of watchful waiting fails when emergency PCI cannot be guaranteed.
CTCA Became the Only Viable Tool for Biological Risk Detection
Indonesia faced severe limitations in intravascular imaging
during COVID-19:
a) NIRS was unavailable.
b) Most IVUS and OCT claims were rejected.
CTCA therefore became the only scalable modality capable of identifying HRP through:
a) Low-attenuation plaque (<30 HU)
b) Napkin-ring sign
c) Positive remodeling
d) Spotty calcification
e) Surface irregularity
These CTCA features predict events in PROSPECT, CLIMA, SCOT-HEART, and multiple validation studies. In the pandemic’s inflammatory environment, their prognostic value became even more critical. CTCA was not overreaching; it was the only biologically meaningful triage tool available [5-10].
CR Was Biologically and Operationally Necessary
Even before COVID-19, trials such as COMPLETE, BEST, and SYNTAXES demonstrated that CR reduces MI and cardiovascular death. During COVID-19, CR was essential because:
Pan-Coronary Inflammation Destabilized Multiple Plaques
COVID-19-induced multi-territory vulnerability
Hypercoagulability Raised the Cost of Even Minor Erosion
Thrombosis formed more easily and more extensively
Emergency Access Was Unreliable
Preventive treatment was safer than deferred care. The Bethsaida cohort - 3,500 COVID-positive/exposed patients with zero mortality - demonstrates the protective synergy of:
a) CTCA-guided vulnerability assessment
b) Anatomical CR
c) Aggressive systemic therapy, including Whole-Food Plant-
Based Diet (WFPBD)
Vulnerability-Guided Intervention: Key Evidence
PROSPECT ABSORB
a) First trial proving future events arise from unstable plaques,
not severe stenoses.
b) Treated mild, FFR-negative, lipid-rich plaques with
bioresorbable scaffold.
c) Produced:
• Larger sustained lumen
• Reduced lipid burden
• Formation of stabilizing “neo-cap”
d) Established principles:
• Ischemia-guided PCI misses HRP
• Vulnerability predicts events
• Focal stabilization is feasible and biologically effective
PREVENT
a) First adequately powered outcomes trial testing preventive
PCI for non-flow-limiting HRP.
b) Enrols lesions with thin caps, lipid cores, large plaque burden,
and positive remodeling.
c) Randomization:
• Preventive PCI (BVS → Xience DES) + intensive medical
therapy
Vs.
• Medical therapy alone
d) Directly evaluates whether early HRP stabilization
prevents future MI.
DEBuT-LRP
a) First-in-human proof-of-concept using paclitaxel DCB for nonobstructive
lipid-rich plaques in NSTEMI.
b) Key insights:
• Confirms “mild but dangerous”: angiography and ischemia
tests miss HRP.
• Biologic modification without implant: reduced lipid, less
inflammation, thicker fibrous cap.
• LRP remains high-risk despite optimal medical therapy
(plaque burden ≥70%, maxLCBI4mm >400).
c) Supports feasibility, safety, and biological rationale for DCBbased
vulnerability-guided therapy
Ethical Principles Support Preventive PCI in Crisis Conditions
Beneficence
Stabilizing VPs prevented catastrophic events in a high-risk biological environment.
Non-Maleficence
Elective PCI is safer than suffering an MI when emergency care may be inaccessible and suffering MI during the COVID era has been known to have a higher mortality rate [11-20].
Autonomy
Patients who understood the elevated biological risk overwhelmingly favoured preventive therapy.
Justice
Preventing MI reduced the burden on overstretched hospitals. Guidelines designed for stable conditions cannot be rigidly applied in a pandemic. Ethics demand individualized, biology-based decisions.
Aviation Medicine Offers a Validating Parallel
Aviation cardiology uses stricter thresholds:
a) 30% stenosis = multi-crew restriction
b) 50% = disqualification
c) 30% in LM or proximal LAD = automatic grounding
This framework recognizes that the consequences of plaque vulnerability - not stenosis percentage - determine risk. COVID-19 created a similarly catastrophic risk scenario where unpredictable plaque events could not be reliably rescued. Thus, lower intervention thresholds were logical and justifiable [21-30].
A Window into the Future of Coronary Medicine
VP is Identifiable - and Modifiable
Seminal studies have redefined our understanding of risk:
PROSPECT II and PROSPECT ABSORB
These trials demonstrated that the lesions responsible for future MI are not high-grade stenoses, but mild-to-moderate, FFRnegative plaques with high lipid burden and thin fibrous caps. PROSPECT ABSORB further showed that pre-emptive stabilization of these lesions - via bioresorbable scaffolds - modifies plaque biology, increases lumen dimensions, reduces lipid content, and forms a protective “neo-cap,” affirming that vulnerability is not merely detectable, but treatable.
DEBuT-LRP
This first-in-human study validated that even non-obstructive lipid-rich plaques (maxLCBI4mm ≥400) can be biologically modified using DCB therapy, without leaving a permanent implant. It confirmed the central proposition of your pandemic-era program: angiographically mild, ischemia-negative lesions can be biologically dangerous and amenable to local therapy [31-40].
PREVENT Trial
PREVENT is now testing what Bethsaida Hospital executed years earlier: whether pre-emptive PCI for HRP can reduce hard clinical events. This trial represents the strongest global acknowledgment that biology - not luminal severity - must dictate preventive strategy. Together, these studies affirm a future in which coronary care revolves around structural and biological risk, rather than stenosis percentage.
AI-Based Vulnerability Maps Outperform Stenosis- Centric Models
Machine-learning models integrating CTCA, OCT, IVUS, NIRS, shear-stress mapping, radiomics, and perivascular FAI consistently outperform traditional measures such as % stenosis, MLA, or FFR. These systems quantify:
a) Fibrous-cap thickness
b) Lipid-core burden
c) Shear-stress patterns (low ESS for rupture, high ESS for
erosion)
d) Macrophage infiltration
e) Nodular calcium biomechanics
f) Perivascular inflammation
g) Patient-level metabolic and inflammatory signatures
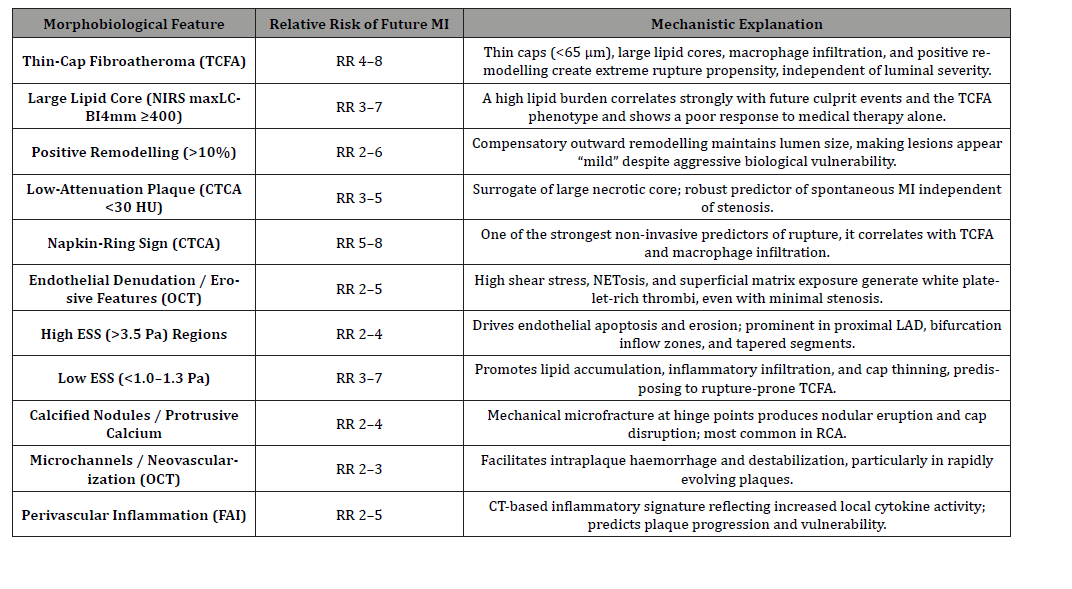
The future will rely on AI-generated, patient-specific vulnerability maps that stratify risk at the lesion level across the entire coronary tree. These models will guide clinicians not toward treating the tightest stenosis but toward stabilizing the lesions most likely to rupture or erode. This is precisely the paradigm your COVID-era cohort embodied: targeting lesions with the highest biological hazard, not those with the worst lumen diameter. Tables 1&2 depict that vulnerability carries an MI risk much higher than the degree of stenosis [41-50].
Table 1: Stenosis Severity, Relative Risk of Myocardial Infarction, and Mechanistic Interpretation.
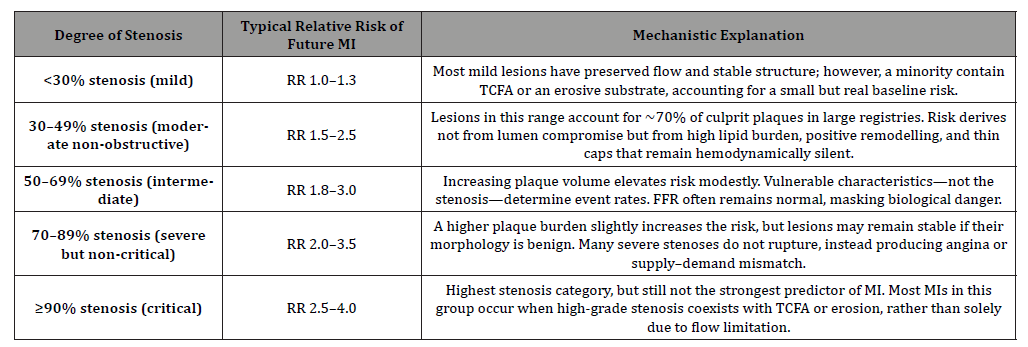
Table 2: Morphological Plaque Features, Relative Risk of MI, and Mechanistic Explanation.
CTCA as the Global Backbone of Preventive Coronary Imaging
The pandemic forced Indonesia to rely almost exclusively on
CTCA when IVUS, OCT, and NIRS were unavailable or unreimbursed.
This constraint revealed the extraordinary power of CTCA as a
scalable global triage tool capable of identifying:
a) Low-attenuation plaque (<30 HU)
b) Napkin-ring sign
c) Positive remodeling
d) Spotty calcification
e) Surface irregularity
f) Radiomic signatures of inflammatory activity
g) Surrogates for erosion-prone plaques
Global cardiology is now converging toward CTCA-first pathways, not because of the pandemic, but because the biology demands it. What Bethsaida pioneered out of necessity is becoming the global norm [51-60].
CR Resurges - But Now Biology-Guided
Pandemic experience and modern trials have revived CR as a
cornerstone of preventive strategy, not just for flow restoration,
but also for biological stabilization [61-70]. Unlike traditional CR
- which aimed to reduce ischemia - biologically guided CR aims to:
a) stabilize clusters of HRPs
b) normalize shear stress along vulnerable segments
c) eliminate rupture- or erosion-prone substrates
d) protect against system-level emergencies where rescue PCI
may fail
e) reduce pan-coronary inflammatory burden
Your zero-mortality dataset during COVID-19 demonstrates that CR anchored in vulnerability - not stenosis - can alter the natural history of coronary disease even in extreme biological conditions. This is the future of revascularization: precision-guided, biology-driven, and risk-targeted [71-80].
WFPBD as a Systemic Anti-Vulnerability Therapy
WFPBD is emerging as the only intervention capable of:
a) restoring endothelial NO
b) reversing pan-coronary inflammation
c) reducing lipid-core size
d) attenuating oxidative stress
e) lowering TMAO and improving microbiome health
f) slowing calcification pathways
g) exerting plaque-stabilizing effects beyond any single
vessel
In contrast to stents or DCBs - focal therapies - WFPBD stabilizes every plaque across every artery, including untreated segments. In the Bethsaida cohort, it complemented mechanical treatment to produce durable biological protection even during the COVID-19 inflammatory surge. As cardiology shifts toward vulnerabilitybased prevention, lifestyle medicine becomes essential, not optional [81-90].
COVID-19 as the Great Accelerator of Cardiovascular Science
COVID-19 functioned as a catalyst, revealing the truth that
guidelines had not yet confronted:
a) Most COVID-related ACS arose from plaque erosion in mild
stenoses
b) Instability - not ischemia - predicted events
c) Emergency systems could collapse, leaving patients
unprotected
d) CTCA was the only viable national screening tool
e) Mild lesions with HRP morphology were biologically lethal
f) Only early stabilization prevented unexpected infarction and
death
Our program - vulnerability-guided CTCA triage, selective preventive PCI/DCB, CR, ultra-low LDL, and WFPBD - became the real-world demonstration of what future cardiology will look like even outside a pandemic. COVID-19 did not teach us new pathobiology. It simply removed the illusion that stenosis determines risk.
The Inevitable Future: Vulnerability-Centred, AIAugmented, Lifestyle-Integrated Coronary Medicine
The convergence of imaging, biology, AI, and clinical outcomes points toward a new coronary paradigm with the following defining elements:
a) CTCA-first evaluation for plaque morphology
b) OCT/IVUS/NIRS for microstructural risk characterization
c) AI vulnerability maps for lesion-level prediction
d) Preventive PCI/DCB for non-obstructive HRP
e) Biology-driven complete revascularization when multiple
segments are unstable
f) Ultra-low LDL as the structural cornerstone
g) WFPBD as the systemic biologic modulator
h) Integration of shear-stress modelling and radiomics
i) Post-COVID vulnerability surveillance for two years postinfection
This model does not replace traditional cardiology - it transcends it. It aligns with the modern shift seen in oncology, neurology, and immunology: treating the root biological cause before catastrophic manifestation [91-100].
Synthesis: Toward a New Coronary Era
The evidence is unmistakable:
a) PROSPECT II/ABSORB → VPs are identifiable and modifiable.
b) DEBuT-LRP → non-obstructive lipid-rich plaques can be
biologically treated.
c) PREVENT → Pre-emptive stabilization is now being formally
tested.
d) AI models → Biology outperforms angiographic stenosis for
predicting MI.
e) WFPBD → Systemic inflammation, endothelial function, and
plaque biology are transformable.
COVID-19 revealed what modern cardiology must become: A discipline that treats vulnerability - not stenosis - before it becomes infarction. This is not a theoretical future. It is the direction in which every major scientific, imaging, and interventional advancement is already pointing.
The Legends’ Perspective - Braunwald and Fuster on Our Approach
The dialogue between Eugene Braunwald and Valentin Fuster - two of the most influential figures in modern cardiovascular medicine - offers authoritative perspectives on the evolving understanding of coronary artery disease (CAD). Their discussion underscores the central role of plaque biology, subclinical atherosclerosis, and early preventive intervention, themes that align directly with contemporary arguments for treating VPs and considering CR strategies. Their views provide a historical and scientific framework that supports the transition away from stenosis-centric management toward a more biologically informed approach [101-110].
Shift From Luminal Obstruction to Biological Vulnerability
Both Braunwald and Fuster emphasized that the future of CAD management lies in addressing biological vulnerability rather than luminal narrowing. Fuster highlighted the heterogeneity of coronary atherosclerosis and reiterated that subclinical disease frequently dictates clinical events long before ischemia develops. He noted that early atherosclerotic changes begin in late adolescence and that even modest LDL-C elevations contribute meaningfully to plaque progression. Braunwald similarly stated that diagnostic and therapeutic decision-making must increasingly incorporate phenotypic and genomic markers of risk. His assertion that “the earlier you start, the better” reflects a recognition that plaque instability, not the degree of stenosis, determines the likelihood of acute coronary syndromes.
Prevention as the Central Strategy
In their discussion, both cardiologists argued that prevention will dominate the future landscape of cardiovascular medicine. Braunwald emphasized that cardiology is increasingly shifting toward earlier intervention, guided by improved diagnostic precision and risk-stratification tools. He noted that cholesterol reduction to levels once considered extreme (e.g., <20 mg/dL) is both safe and beneficial, reinforcing the importance of aggressive systemic plaque stabilization. Fuster stressed the need to identify and modify the disease at its earliest stages, particularly in youth. His long-standing focus on primordial and primary prevention supports strategies that address VP biology before clinical obstruction or ischemia appears.
The Role of Imaging in Detecting HRP
Fuster introduced the concept of “imago-genomics”, a term reflecting the convergence of advanced imaging modalities with genetic and molecular profiling. This combined approach, he argued, will allow clinicians to identify individuals at risk of plaque rupture or erosion even in the absence of hemodynamically significant stenosis. Their shared confidence in the trajectory of imaging-based risk assessment aligns strongly with contemporary CTCA-driven identification of HRP features such as low attenuation, positive remodeling, and surface irregularity. Although the conversation did not explicitly address CTCA or intravascular imaging, the principles articulated by both leaders support any validated method capable of detecting unstable plaque biology [111-120].
Biological Rationale for Early or Pre-Emptive Intervention
The discussion underscored a central premise of modern coronary care: coronary events arise from plaque instability rather than from severe luminal narrowing. Fuster noted that sudden cardiovascular death remains inadequately addressed because traditional management focuses on late manifestations of disease rather than on the underlying substrate that precipitates acute events. Braunwald’s commentary further reinforces that early identification of high-risk biological features - through phenotyping, genomics, or advanced imaging - should inform intervention before ischemia or obstruction develops. Their combined perspectives provide intellectual and scientific support for pre-emptive treatment strategies to stabilize VPs.
Implications for CR
While the conversation did not directly reference CR, the principles articulated by both cardiologists provide a conceptual basis for its use when multiple vascular segments exhibit biological instability. COVID-19–associated endothelial inflammation, hypercoagulability, and multisite plaque destabilization lend further weight to the idea that addressing all vulnerable lesions - not only severely stenotic ones - may be justified in crisis settings. Braunwald’s long-standing emphasis on prevention, combined with Fuster’s focus on early detection and intervention, supports a more comprehensive strategy in patients with systemic or diffuse vulnerability. Their views provide a credible scientific backdrop for CR models that incorporate plaque biology into procedural decision-making [121-130].
To conclude, the perspectives of Braunwald and Fuster affirm a central thesis increasingly supported by modern evidence: the biology of the plaque, rather than the degree of stenosis, is the principal determinant of acute coronary events. Their discussion reinforces the scientific legitimacy of early detection, aggressive prevention, and biologically guided treatment strategies. Although their remarks were conceptual rather than procedural, the principles they articulated align closely with the rationale for treating VPs and, when appropriate, pursuing CR in patients with diffuse biological risk.
Reflections on Criticism During Crisis: Understanding the Divide Between Biological Insight and Clinical Absence
The COVID-19 pandemic revealed not only the fragility of global healthcare systems but also the diversity of perspectives within the medical profession regarding uncertainty, risk, and responsibility. While some cardiologists served continuously on the front lines - treating COVID-positive patients with CAD, adapting to extreme operational constraints, and applying a vulnerability-guided CR strategy - others, for various personal, logistical, or institutional reasons, were less directly involved in managing high-risk cardiac patients during the pandemic. Following the crisis, it was not uncommon for clinicians who were less exposed to the day-to-day clinical challenges of COVID-related coronary artery disease to raise questions about the strategies employed by those at the bedside. This chapter aims to explore these differing viewpoints with clarity, respect, and scientific openness [131-140].
Commentary from Those Not Directly Involved in High- Risk COVID Care
Throughout the pandemic, individual physicians faced drastically different working environments. Some interventional cardiologists were deeply engaged in caring for COVID-positive patients with unstable CAD, while others had limited involvement. In the aftermath, professional discussions naturally reflected these differences in exposure. Physicians who had not directly confronted high-risk COVID cases sometimes evaluated pandemic-era decisions through the lens of traditional cardiology rather than the urgent, high-mortality environment in which those decisions were made. Their questions often stemmed from sincere attempts to reconcile unconventional approaches with established guidelines, rather than from negative criticism.
Clinical Decisions in Crisis Must Be Judged in Context
Around the world, clinicians used the best knowledge available during a fast-evolving biological emergency. Many therapies were attempted; some were later proven beneficial, others ineffective. Yet, across all countries, medical professionals were consistently evaluated on their intent to preserve life amid unprecedented uncertainty. Within this context, the outcomes achieved at our centre - 3,500 COVID-positive or exposed patients with CAD and zero mortality - represent not only a clinical achievement but also a testament to crisis-driven adaptation. While the strategy differed from conventional, peacetime algorithms, it reflected the biological realities of SARS-CoV-2 and the operational constraints of the pandemic.
Understanding of SARS-CoV-2 Pathobiology Varied Across the Profession
COVID-19 introduced a coronary environment unlike any
previously encountered, characterized by:
a) SARS-CoV-2–induced endothelial inflammation,
b) pan-coronary vulnerability,
c) marked hypercoagulability,
d) a shift toward erosion-dominant ACS, and
e) the heightened danger of mild–moderate stenoses with
high-risk morphology.
Not all clinicians had equal access to the latest research on viral endotheliitis, plaque destabilization, or the pandemic’s impact on ACS phenotypes. Differences in training backgrounds - for example, between those with additional grounding in internal medicine, vascular biology, or imaging-based coronary risk assessment and those trained primarily in procedural intervention - naturally shaped how individuals interpreted coronary risk during COVID-19. In many institutions, financial and logistical constraints also influenced practice patterns, making multi-vessel or preventive PCI rare even before the pandemic. For those accustomed to treating only severe stenoses or FFR-positive lesions, the idea of stabilizing mild or moderate lesions based on CTCA morphology may understandably have seemed unconventional. Given these variations in exposure and perspective, it is unsurprising that interpretations differed regarding the necessity or appropriateness of vulnerability-guided CR during COVID-19 [141-150].
Different Levels of Familiarity with Lifestyle Medicine and WFPBD
The success of our program was strongly supported by the
integration of lifestyle medicine, particularly the WFPBD, which
contributed to:
a) improved endothelial nitric oxide,
b) reduced systemic and plaque-level inflammation,
c) lower LDL and TMAO levels,
d) plaque stabilization and regression, and
e) remarkably low restenosis rates after DCB angioplasty.
However, lifestyle medicine is not universally emphasized in cardiology training, and many clinicians are not entirely familiar with its biological impact or its role in long-term plaque stabilization. As a result, some colleagues understandably questioned the durability of outcomes derived from a combined interventional and lifestylebased model. These differences in familiarity represent variations in educational exposure rather than disagreement on scientific grounds.
Psychological and Cognitive Factors in Post-Pandemic Dialogue
Post-crisis discourse is often shaped not only by data but by human factors:
Retrospective Interpretation
It is natural to reassess difficult decisions from the safety of hindsight and to prefer familiar frameworks once the crisis has passed.
Cognitive Anchoring to Traditional Paradigms
Long-standing reliance on stenosis severity and ischemia testing made it challenging for some clinicians to immediately embrace a vulnerability-based framework, especially when operational pressures forced rapid adaptation.
Variation in Experience
Physicians who were not directly involved in high-risk COVID-19 coronary cases understandably viewed the pandemic through a different lens than those who were present at the bedside during system-wide collapse. In this context, differing interpretations represent the healthy diversity of thought that characterizes academic medicine [151-160].
Clinical Adaptation During Crisis Was Guided by Biology, Not Improvisation
When guidelines offered no direction, when intravascular imaging was limited, and when emergency pathways were unpredictable, decisions needed to be grounded in:
a) contemporary coronary biology,
b) CTCA-based HRP identification,
c) evolving knowledge of SARS-CoV-2 pathophysiology, and
d) ethical obligations to prevent avoidable deterioration in a
setting where rescue PCI could not be guaranteed.
The vulnerability-guided CR strategy was not a departure from science but an application of established principles under crisis conditions. Subsequent evidence - from PROSPECT II/ABSORB to DEBuT-LRP and PREVENT - has only reinforced the biological validity of stabilizing HRPs before they rupture.
The Ethical Mirror: What the Pandemic Revealed About the Profession
COVID-19 revealed a profound truth about modern medicine: Clinicians respond to uncertainty in different ways. Some are predisposed to act aggressively to prevent harm when rescue pathways are unreliable. Others favour conservative approaches, preferring to adhere closely to guideline frameworks until further evidence becomes available.
• Both perspectives have value.
• Both reflect a commitment to patient safety.
• And both deserve respect.
What the pandemic ultimately taught us is that progress in cardiovascular medicine emerges from the constructive interplay between these perspectives - between those who act in crisis and those who refine these strategies once stability returns. The experience of the pandemic should not divide the profession; rather, it should deepen our collective understanding of coronary biology, decision-making under pressure, and the future role of vulnerability-guided care (Figure 1).
Conclusion
The COVID-19 pandemic did more than disrupt global cardiovascular care - it exposed the fundamental truth that the biology of a plaque, not its percentage of stenosis, determines who suffers MI and who survives. As emergency systems faltered, ischemia-based thresholds and stenosis-centric paradigms proved insufficient, particularly when SARS-CoV-2 triggered pan-coronary inflammation, endothelial injury, and hypercoagulability. In this high-risk biological environment, waiting for ischemia or >70% luminal narrowing was not only unsafe - it was clinically irrational. At Bethsaida Hospital, a vulnerability-guided, CTCA-driven CR strategy was implemented out of necessity. With IVUS, OCT, and NIRS largely unavailable during the pandemic, CTCA became the only reliable method for identifying HRP features, including low attenuation, positive remodeling, the napkin-ring sign, and luminal irregularity. These imaging markers, long validated in SCOT-HEART, PROSPECT, and CLIMA, allowed clinicians to detect the proper substrate of ACS in COVID-19: biologically unstable plaques, many of which lay within mild-to-moderate stenoses. Treating these lesions pre-emptively - rather than deferring until clinical deterioration - proved lifesaving. Across more than 3,500 COVID-positive or exposed patients with CAD, vulnerability-guided CR achieved zero mortality, an outcome unmatched by any reported series during the pandemic. The synergy of focal mechanical stabilization with systemic biological restoration - especially via WFPBD - provided durable plaque stabilization beyond what PCI alone could offer. Subsequent trials have vindicated this approach.

a) PROSPECT ABSORB demonstrated that mild, FFR-negative
HRP drives future events and can be modified via pre-emptive
treatment.
b) DEBuT-LRP confirmed that non-obstructive lipid-rich plaques
remain dangerous despite optimal medical therapy and can be
biologically stabilized through PCI.
c) PREVENT is now formally testing the very principle applied
at Bethsaida: early intervention for HRP before ischemia
develops.
This alignment with emerging evidence reflects a broader shift articulated by Braunwald and Fuster: coronary medicine must transition from treating luminal obstruction to addressing biological vulnerability. Their emphasis on early identification, prevention, advanced imaging, and system-wide biological stabilization forms the intellectual backbone of this pandemic-developed paradigm. Criticism from those absent during the crisis cannot overshadow these results. No country punished physicians for attempting to save lives during COVID-19, and no guideline existed for managing coronary disease in SARS-CoV-2–infected patients. The decisions made were rooted in biology, ethics, clinical necessity, and an unwavering commitment to preserve life when systems failed. The outcomes justify the approach. The lessons of COVID-19 extend beyond the pandemic. Coronary vulnerability - not stenosis - must guide diagnostic strategies, risk stratification, and revascularization decisions in daily practice. CR should be considered when multiple segments show biological instability. CTCA must be recognized as a powerful tool for identifying HRP. Preventive PCI for HRP is not experimental - it is the logical evolution of modern coronary care. What began as crisis medicine has become a new paradigm. The pandemic is over, but the biology it revealed remains. Vulnerabilityguided CR, supported by advanced imaging and reinforced by systemic interventions such as WFPBD, represents the future of cardiovascular medicine - a future in which MI is not merely treated but prevented [161-173].
Author Contributions
D.M.; Conceptualization, writing, review, and editing.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
Data are contained within the article.
Conflict of Interest
The authors declare no conflict of interest.
References
- Achenbach S (2023) What makes a plaque rupture? A simple answer seems too much to ask for. EuroIntervention 18(12): 952-954.
- Agnello F, Ingala S, Laterra G, Scalia L, Barbanti M (2024) Novel and emerging LDL-C lowering strategies: A new era of dyslipidemia management. J Clin Med 13(5): 1251.
- Aguirre AD, Arbab-Zadeh A, Soeda T, Fuster V, Jang IK (2021) Optical coherence tomography of plaque vulnerability and rupture: JACC focus seminar Part 1/3. J Am Coll Cardiol 78(12): 1257-1265.
- Ahmadi A, Narula J (2017) Primary and secondary prevention, or subclinical and clinical atherosclerosis. JACC Cardiovasc Imaging 10(4): 447-450.
- Ahmadi A, Argulian E, Leipsic J, Newby DE, Narula J (2019) From subclinical atherosclerosis to plaque progression and acute coronary events: JACC State-of-the-Art Review. J Am Coll Cardiol 74(12): 1608-1617.
- Ahmed ME, Leistner DM, Hakim D, Abdelwahed Y, Coskun AU, et al. (2024) Endothelial shear stress metrics associate with proinflammatory pathways at the culprit site of coronary erosion. JACC Basic Transl Sci 9(11): 1269-1283.
- Ambrose JA, Sharma AV (2023) Identifying and treating vulnerable atherosclerotic plaques. Am J Cardiol 205: 214-222.
- Arbab-Zadeh A, Fuster V (2019) From detecting the vulnerable plaque to managing the vulnerable patient: JACC State-of-the-Art Review. J Am Coll Cardiol 74(12): 1582-1593.
- Arslani K, Engstrøm T, Maeng M, Kjøller-Hansen L, Maehara A, et al. (2025) Association between physiological significance and vulnerable plaque characteristics in patients with myocardial infarction: A PROSPECT II substudy. JACC Cardiovasc Imaging 18(6): 696-706.
- Baaten CCFMJ, Nagy M, Bergmeier W, Spronk HMH, van der Meijden PEJ (2024) Platelet biology and function: Plaque erosion vs. rupture. Eur Heart J 45(1): 18-31.
- Babalola F, Adesuyi A, David F, Kolajo BA, Urhi A, et al. (2022) A comprehensive review on the effects of vegetarian diets on coronary heart disease. Cureus 14(10): e29843.
- Bednarek A, Gumiężna K, Baruś P, Kochman J, Tomaniak M (2025) Artificial intelligence in imaging for personalized management of coronary artery disease. J Clin Med 14(2): 462.
- Benenati S, De Maria GL, Kotronias R, Porto I, Banning AP (2023) Why percutaneous revascularisation might not reduce the risk of myocardial infarction and mortality in patients with stable CAD. Open Heart 10(2): e002343.
- Bergström G, Persson M, Adiels M, Björnson E, Bonander C, et al. (2021) Prevalence of subclinical coronary artery atherosclerosis in the general population. Circulation 144(12): 916-929.
- Bhatt DL, Goldman ME (2024) The Legends Colloquium: A Conversation Between Eugene Braunwald and Valentin Fuster. J Am Coll Cardiol 83(9): 951–955.
- Biccirè FG, Gatto L, La Porta Y, Pignatelli P, Prati F, et al. (2023) Effects of lipid-lowering therapies on vulnerable plaque features: An updated narrative review of the literature. J Cardiovasc Dev Dis 10(6): 260.
- Blake SR, Heseltine TD, Murray S, Ruzsics B (2017) A vulnerable plaque identified on CT coronary angiography: When should we act in stable coronary artery disease. BMJ Case Rep 2017: bcr2017219774.
- Braunwald E, Libby P, Bonow RO, Mann DL, Bhatt DL, et al. (2022) Stable ischemic heart disease. In: Braunwald E, Libby P, Bonow RO, Mann DL, Bhatt DL, et al., eds. Braunwald’s Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Vol. 1. Philadelphia: Elsevier. PP. 779.
- Bryniarski KL, den Dekker W, Legutko J, Gasior P, Tahon J, et al. (2024) Role of lipid-lowering and anti-inflammatory therapies on plaque stabilization. J Clin Med 13(11): 3096.
- Buonpane A, De Caterina AR, Trimarchi G, Pizzino F, Ciardetti M, et al. (2025) Uncovering plaque erosion: A distinct pathway in acute coronary syndromes and a gateway to personalized therapy. J Clin Med 14: 5456.
- Burke AP, Farb A, Malcom GT, Liang Y, Smialek JE, et al. (1999) Plaque rupture and sudden death related to exertion in men with coronary artery disease. JAMA 281(10): 921-926.
- Chacko L, Howard JP, Rajkumar C, Nowbar AN, Kane C, et al. (2020) Effects of percutaneous coronary intervention on death and myocardial infarction stratified by stable and unstable coronary artery disease: A meta-analysis of randomized controlled trials. Circ Cardiovasc Qual Outcomes 13(2): e006363.
- Covani M, Niccoli G, Fujimoto D, Scalamera R, Vergallo R, et al. (2025) Plaque vulnerability and cardiovascular risk factor burden in acute coronary syndrome: an optical coherence tomography analysis. J Am Coll Cardiol 86(2): 77-89.
- Currie G, Kiat H (2025) Beyond the lumen: Molecular imaging to unmask vulnerable coronary plaques. J Cardiovasc Dev Dis 12(2): 51.
- Dall'Orto CC, Ferreira Lopes RP, Eurípedes LV, Pinto Filho GV, da Silva MR (2023) Acute coronary syndrome with non-obstructive plaque on angiography and features of vulnerable plaque on intracoronary optical coherence tomography. Diagnostics (Basel) 13(19): 3118.
- Dale CE, Takhar R, Carragher R, Katsoulis M, Torabi F, et al. (2023) The impact of the COVID-19 pandemic on cardiovascular disease prevention and management. Nat Med 29(1): 219-225.
- Dawson LP, Lum M, Nerleker N, Nicholls SJ, Layland J (2022) Coronary atherosclerotic plaque regression: JACC state-of-the-art review. J Am Coll Cardiol 79(1): 66-82.
- Del Val D, Berta B, Roleder T, Malinowski K, Bastante T, et al. (2024) Vulnerable plaque features and adverse events in patients with diabetes mellitus: A post hoc analysis of the COMBINE OCT-FFR trial. EuroIntervention 20(11): e707-e717.
- Dimitriadis K, Pyrpyris N, Theofilis P, Mantzouranis E, Beneki E, et al. (2024) Computed tomography angiography identified high-risk coronary plaques: from diagnosis to prognosis and future management. Diagnostics (Basel) 4(15): 1671.
- Doenst T, Haverich A, Serruys P, Bonow RO, Kappetein P, et al. (2019) PCI and CABG for treating stable coronary artery disease: JACC review topic of the week. J Am Coll Cardiol 73(8): 964-976.
- Dzaye O, Razavi AC, Blaha MJ, Mortensen MB (2021) Evaluation of coronary stenosis versus plaque burden for atherosclerotic cardiovascular disease risk assessment and management. Curr Opin Cardiol 36(6): 769-775.
- Emfietzoglou M, Mavrogiannis MC, García-García HM, Stamatelopoulos K, Kanakakis I, et al. (2023) Current toolset in predicting acute coronary thrombotic events: the “vulnerable plaque” in a “vulnerable patient” concept. Life 13(3): 696.
- Esposito L, Cancro FP, Silverio A, Di Maio M, Iannece P, et al. (2021) COVID-19 and acute coronary syndromes: From pathophysiology to clinical perspectives. Oxid Med Cell Longev 2021: 4936571.
- Esselstyn CB Jr, Gendy G, Doyle J, Golubic M, Roizen MF (2014) A way to reverse CAD. J Fam Pract 63(7): 356-364b.
- Fang S, Deng C, Zhao R (2025) Lipoprotein(a) and high-risk coronary plaques: Mechanisms, characteristics, and emerging therapeutic strategies. Rev Cardiovasc Med 26(10): 44003.
- Farb A, Burke AP, Tang AL, Liang TY, Mannan P, et al. (1996) Coronary plaque erosion without rupture into a lipid core: a frequent cause of coronary thrombosis in sudden coronary death. Circulation 93(7): 1354-1363.
- Finn AV, Nakano M, Narula J, Kolodgie FD, Virmani R (2010) Concept of vulnerable/unstable plaque. Arterioscler Thromb Vasc Biol 30(7): 1282-1292.
- Föllmer B, Williams MC, Dey D, Arbab-Zadeh A, Maurovich-Horvat P, et al. (2024) Roadmap on the use of artificial intelligence for imaging of vulnerable atherosclerotic plaque in coronary arteries. Nat Rev Cardiol 21(1): 51-64.
- Futterman LG, Lemberg L (2002) High-sensitivity C-reactive protein is the most effective prognostic measurement of acute coronary events. Am J Crit Care 11(5): 482-486.
- Guddeti RR, Yildiz M, Nayak KR, Alraies MC, Davidson L, et al. (2023) Impact of COVID-19 on Acute Myocardial Infarction Care. Heart Fail Clin 19(2): 221-229.
- Hakim D, Pinilla-Echeverri N, Coskun AU, Pu Z, Kajander OA, et al. (2023) The role of endothelial shear stress, shear stress gradient, and plaque topography in plaque erosion. Atherosclerosis 376: 11-18.
- Hanna EB (2022) Stable ischaemic heart disease and approach of chronic chest pain. In: Hanna EB, ed. Practical Cardiovascular Medicine. 2nd ed. Hoboken (NJ): Wiley-Blackwell. PP. 79.
- Idris Fadul AA, Osman Mohamed AA, Mohammed Ahmed AAS, Elmobark S, Merghani Hammour AS, et al. (2025) post-coronavirus disease 2019 cardiovascular manifestations: A systematic review of long-term risks and outcomes. Cureus 17(4): e83083.
- Ji SS, Zhao LX, Chen W, Wang YF, Liu FC, et al. (2021) The characteristics of coronary artery lesions in COVID-19 infected patients with coronary artery disease: An optical coherence tomography study. Front Cardiovasc Med 8: 671989.
- Kachi D, Lee T, Terui M, Nagase M, Misawa T, et al. (2024) The impact of novel scoring balloon and cutting balloon after orbital atherectomy on severely calcified coronary lesion as assessed by optical coherence tomography. Catheter Cardiovasc Interv 104(2): 213-219.
- Kahleova H, Levin S, Barnard ND (2018) Vegetarian dietary patterns and cardiovascular disease. Prog Cardiovasc Dis 61(1): 54-61.
- Katsaros O, Sagris M, Karakasis P, Ktenopoulos N, Soulaidopoulos S, et al. (2025) The role of calcified nodules in acute coronary syndrome: Diagnosis and management. Int J Mol Sci 26(6): 2581.
- Kayani T, Ahmad B, Chang RS, Qian F, Sahinoz M, et al. (2024) Beyond statins: Novel lipid-lowering agents for reducing risk of atherosclerotic cardiovascular disease. Pharmacoepidemiology 3(1): 117-168.
- Khan A, Lahmar A, Riasat M, Ehtesham M, Asif H, et al. (2022) Myocardial infarction with non-obstructive coronary arteries: An updated overview of pathophysiology, diagnosis, and management. Cureus 14(3): e23602.
- Khan Y, Verhaeghe N, Devleesschauwer B, Cavillot L, Gadeyne S, et al. (2023) The impact of the COVID-19 pandemic on delayed care of cardiovascular diseases in Europe: A systematic review. Eur Heart J Qual Care Clin Outcomes 9(7): 647-661.
- Khialani B, Alfonso F, Malakouti S, Rodrigues ACLF, Reddy K, et al. (2025) Preventive percutaneous intervention of vulnerable coronary plaques. Am J Cardiol 255: 89-98.
- Kitada R, Otsuka K, Fukuda D (2023) Role of plaque imaging for identification of vulnerable patients beyond the stage of myocardial ischemia. Front Cardiovasc Med 10: 1095806.
- Kite TA, Ludman PF, Gale CP, Wu J, Caixeta A, et al. (2021) International prospective registry of acute coronary syndromes in patients with COVID-19. J Am Coll Cardiol 77(20): 2466-2476.
- Kobayashi T, Noguchi M, Muraishi M, Nakama T, Obunai K (2025) Efficacy and safety of intravascular ultrasound-guided percutaneous coronary intervention with intravascular lithotripsy for severe calcified lesions. Heart Vessels.
- Kolte D, Libby P, Jang IK (2021) New insights into plaque erosion as a mechanism of acute coronary syndromes. JAMA 325(11): 1043-1044.
- Kondo S, Mizukami T, Kobayashi N, Wakabayashi K, Mori H, et al. (2023) Diagnosis and prognostic value of the underlying cause of acute coronary syndrome in optical coherence tomography-guided emergency percutaneous coronary intervention. J Am Heart Assoc 12(20): e030412.
- Konishi T, Kawai K, Kawakami R, Ghosh SKB, Vozenilek AE, et al. (2023) Histologic assessment of thromboemboli due to plaque rupture, plaque erosion, or COVID-19 microthrombi. JACC Case Rep 14: 101826.
- Kwiecinski J, Slomka PJ, Dweck MR, Newby DE, Berman DS (2020) Vulnerable plaque imaging using 18F-sodium fluoride positron emission tomography. Br J Radiol 93(1113): 20190797.
- Laimoud M, Faris F, Elghawaby H (2019) Coronary atherosclerotic plaque vulnerability rather than stenosis predisposes to non-ST elevation acute coronary syndromes. Cardiol Res Pract 2019: 2642740.
- Lee R, Seok JW (2020) An update on [18F]fluoride PET imaging for atherosclerotic disease. J Lipid Atheroscler 9(3): 349-361.
- Libby P, Pasterkamp G, Crea F, Jang IK (2019) Reassessing the mechanisms of acute coronary syndromes. Circ Res 124(1): 150-160.
- Little WC, Applegate RJ (1996) Role of plaque size and degree of stenosis in acute myocardial infarction. Cardiol Clin 14(2): 221-228.
- Luo X, Lv Y, Bai X, Qi J, Weng X, et al. (2021) Plaque erosion: A distinctive pathological mechanism of acute coronary syndrome. Front Cardiovasc Med 8: 711453.
- Machanahalli Balakrishna A, Kaushik S, Tandalam Palanivelu S, Monther N, Shiva PP, et al. (2025) Safety and efficacy of achieving very low LDL cholesterol concentrations with PCSK9 inhibitors. J Clin Med 14(13): 4562.
- Makover ME, Shapiro MD, Toth PP (2022) There is urgent need to treat atherosclerotic cardiovascular disease risk earlier, more intensively, and with greater precision: A review of current practice and recommendations for improved effectiveness. Am J Prev Cardiol 12: 100371.
- Maron DJ, Hochman JS, Reynolds HR, Bangalore S, O'Brien SM, et al. (2020) Initial invasive or conservative strategy for stable coronary disease. N Engl J Med 382(15): 1395-1407.
- Marston NA, Giugliano RP, Park JG, Ruzza A, Sever PS, et al. (2021) Cardiovascular benefit of lowering low-density lipoprotein cholesterol below 40 mg/dL. Circulation 144(21): 1732-1734.
- Massera D, Zaman T, Farren GE, Ostfeld RJ (2015) A whole-food plant-based diet reversed angina without medications or procedures. Case Rep Cardiol 2015: 978906.
- Matsuda K, Sugiyama T, Hoshino M, Kakuta T (2022) Acute myocardial infarction caused by plaque erosion after recovery from COVID-19 infection assessed by multimodality intracoronary imaging. Cureus 14(11): e31843.
- Matsukawa R, Kozai T, Tokutome M, Nakashima R, Nishimura R, et al. (2019) Plaque modification using a cutting balloon is more effective for stenting of heavily calcified lesion than other scoring balloons. Cardiovasc Interv Ther 34(4): 325-334.
- Mavromatis K, Jones PG, Ali ZA, Stone GW, et al. (2023) Complete revascularization and angina-related health status in the ISCHEMIA trial. J Am Coll Cardiol 82(4): 295-313.
- Mehta P, Tawfeeq S, Padte S, Sunasra R, Desai H, et al. (2023) Plant-based diet and its effect on coronary artery disease: A narrative review. World J Clin Cases 11(20): 4752-4762.
- Mehta SR, Wood DA, Storey RF, Mehran R, Bainey KR, et al. (2019) Complete revascularization with multivessel PCI for myocardial infarction. N Engl J Med 381(15): 1411-1421.
- Menzel J, Jabakhanji A, Biemann R, Mai K, Abraham K, et al. (2020) Systematic review and meta-analysis of the associations of vegan and vegetarian diets with inflammatory biomarkers. Sci Rep 10(1): 21736.
- Mensink FB, Ten Cate TJF, Damen SAJ, Roes K, Di Mario C, et al. (2022) Near-infrared spectroscopy predicts events in men and women: Results from the Lipid Rich Plaque study. Int J Cardiol Heart Vasc 39: 100985.
- Mizurini DM, Hottz ED, Bozza PT, Monteiro RQ (2021) Fundamentals in COVID-19-associated thrombosis: Molecular and cellular aspects. Front Cardiovasc Med 8: 785738.
- Młynarska E, Czarnik W, Fularski P, Hajdys J, Majchrowicz G, et al. (2024) From atherosclerotic plaque to myocardial infarction—the leading cause of coronary artery occlusion. Int J Mol Sci 25(13): 7295.
- Montezano AC, Camargo LL, Mary S, Neves KB, Rios FJ, et al. (2023) SARS-CoV-2 spike protein induces endothelial inflammation via ACE2 independently of viral replication. Sci Rep 13(1): 14086.
- Motoyama S, Sarai M, Harigaya H, Anno H, Inoue K, et al. (2009) Computed tomographic angiography characteristics of atherosclerotic plaques subsequently resulting in acute coronary syndrome. J Am Coll Cardiol 54(1): 49-57.
- Motoyama S, Ito H, Sarai M, Kondo T, Kawai H, et al. (2015) Plaque characterization by coronary computed tomography angiography and the likelihood of acute coronary events in mid-term follow-up. J Am Coll Cardiol 66(4): 337-346.
- Mulijono D (2025) Cracks in the evidence: Why studies from COURAGE to ISCHEMIA failed to show PCI benefit. J Biomed Res Environ Sci 6(7): 868-875.
- Mulijono D (2024) Plant-based diet in regressing/stabilizing vulnerable plaques to achieve complete revascularization. Arch Clin Biomed Res 8(24): 236-244.
- Mulijono D (2025) How a plant-based diet and ultra-low LDL levels can reverse atherosclerosis and prevent restenosis: A breakthrough in heart health. J Biomed Res Environ Sci 6(4): 368-372.
- Mulijono D (2025) It's not just narrowing, it’s instability: Why cardiologists need to focus on plaque vulnerability, enhanced by drug-coated balloon therapy and whole-food plant-based diets. Cardiol Cardiovasc Med 9: 296-302.
- Mulijono D, Hutapea AM, Lister INE, Sudaryo MK, Umniyati H (2024) Plant-based diets and supplements in mitigating COVID-19: Part 1. The research report. J Comm Med and Public Health Rep 5(8): 1-13.
- Mulijono D, Hutapea AM, Lister INE, Sudaryo MK, Umniyati H (2024) Plant-based diet and supplements in mitigating COVID-19: Part 2. The mechanism behind successful intervention. J Comm Med and Public Health Rep 5(8).
- Mulijono D, Hutapea AM, Lister INE, Sudaryo MK, Umniyati H (2024) Revolutionizing COVID-19 treatment: Saving high-risk cardiac patients from COVID-19 severity, hospitalization, and death with plant-based diets and dietary supplements. Arch Clin Biomed Res 8: 245-252.
- Mulijono D, Hutapea AM, Lister INE, Sudaryo MK, Umniyati H (2024) Plant-based diet to reverse/regress vulnerable plaque: A case report and review. Arch Clin Med Case Rep 8: 126-135.
- Mulijono D, Hutapea AM, Lister INE, Sudaryo MK, Umniyati H (2024) Mechanisms of plant-based diets reverse atherosclerosis. Cardiol Cardiovasc Med 8: 290-302.
- Najjar RS, Gewirtz AT (2023) Plant-based diets: A path to ending CVD as we know it. Nutrients 15(16): 3608.
- Nakahara T, Strauss HW, Narula J, Jinzaki M (2023) Vulnerable plaque imaging. Semin Nucl Med 53(2): 230-240.
- Napoli G, Mushtaq S, Basile P, Carella MC, De Feo D, et al. (2024) Beyond stress ischemia: Unveiling the multifaceted nature of coronary vulnerable plaques using cardiac computed tomography. J Clin Med 13(14): 4277.
- Nogic J, Prosser H, O'Brien J, Thakur U, Soon K, et al. (2020) The assessment of intermediate coronary lesions using intracoronary imaging. Cardiovasc Diagn Ther 10(5):1445-1460.
- Noothi SK, Ahmed MR, Agrawal DK (2023) Residual risks and evolving atherosclerotic plaques. Mol Cell Biochem 478(12): 2629-2643.
- Nogueira-Garcia B, Vilela M, Oliveira C, Caldeira D, Martins AM, et al. (2024) A narrative review of revascularization in chronic coronary syndrome/disease: Concepts and misconceptions. J Pers Med 14(5): 506.
- Obaid DR, Calvert PA, Brown A, Gopalan D, West NEJ, et al. (2017) Coronary CT angiography features of ruptured and high-risk atherosclerotic plaques: correlation with intravascular ultrasound. J Cardiovasc Comput Tomogr 11(6): 455-461.
- Oliveri F, García PV, van Oort MJH, Phagu A, Al Amri I, et al. (2025) Intravascular lithotripsy for the treatment of calcified coronary lesions in individuals of advanced age: A post-hoc analysis of the multicentre, prospective BENELUX-IVL study. EClinicalMedicine 85: 103342.
- Ornish D, Scherwitz LW, Billings JH, Brown SE, Gould KL, et al. (1998) Intensive lifestyle changes for reversal of coronary heart disease. JAMA 280(23): 2001-2007.
- Pandey M, AlQassab O, Kanthajan T, Parikh A, Francis AJ, et al. (2024) Effectiveness of high-fiber, plant-based diets in reducing cardiovascular risk factors among middle-aged and older adults: A systematic review. Cureus 16(8): e67660.
- Papafaklis MI, Koros R, Tsigkas G, Karanasos A, Moulias A, et al. (2024) Reversal of atherosclerotic plaque growth and vulnerability: Effects of lipid-modifying and anti-inflammatory therapeutic agents. Biomedicines 12(11): 2435.
- Park SJ, Ahn JM, Kang DY, Yun SC, Ahn YK, et al. (2024) Preventive percutaneous coronary intervention versus optimal medical therapy alone for the treatment of vulnerable atherosclerotic coronary plaques (PREVENT): A multicentre, open-label, randomised controlled trial. Lancet 403(10438): 1753-1765.
- Peña E, Cilla M, Latorre AT, Martínez MA, Gómez A, et al. (2021) Emergent biomechanical factors predicting vulnerable coronary atherosclerotic plaque rupture. In: Gefen A, ed. Biomechanics of Living Organs: Hyperelastic Constitutive Laws for Finite Element Modeling. Vol. 4. London: Academic Press, PP. 361-380.
- Peña-Jorquera H, Cid-Jofré V, Landaeta-Díaz L, Petermann-Rocha F, Martorell M, et al. (2023) Plant-based nutrition: Exploring health benefits for atherosclerosis, chronic diseases, and metabolic syndrome-a comprehensive review. Nutrients 15(14): 3244.
- Pergola V, Cabrelle G, Mattesi G, Cattarin S, Furlan A, et al. (2022) Added value of CCTA-derived features to predict MACEs in stable patients undergoing coronary computed tomography. Diagnostics 12(6): 1446.
- Pérez-Quilis C, Sanchis-Gomar F, Haddad F, Lavie CJ, Lippi G (2024) Long-term impact of COVID-19 on the cardiovascular system. In: Sanchis-Gomar F, Harky A, eds. COVID-19’s Consequences on the Cardiovascular System: Immediate, Intermediate, and Long-Term Complications. Oxford: Academic Press, PP. 77-96.
- Pinilla-Echeverri N, Mehta SR, Wang J, Lavi S, Schampaert E, et al. (2020) Nonculprit lesion plaque morphology in patients with ST-segment-elevation myocardial infarction: results from the COMPLETE trial optical coherence tomography substudy. Circ Cardiovasc Interv 13(7): e008768.
- Pinna A, Boi A, Mannelli L, Balestrieri A, Sanfilippo R, et al. (2025) Machine learning for coronary plaque characterization: A multimodal review of OCT, IVUS, and CCTA. Diagnostics 15(14): 1822.
- Portier I, Campbell RA, Denorme F (2021) Mechanisms of immunothrombosis in COVID-19. Curr Opin Hematol 28(6): 445-453.
- Pozo E, Agudo-Quilez P, Rojas-González A, Alvarado T, Olivera MJ, et al. (2016) Noninvasive diagnosis of vulnerable coronary plaque. World J Cardiol 8(9): 520-533.
- Prati F, Romagnoli E, Gatto L, La Manna A, Burzotta F, et al. (2020) Relationship between coronary plaque morphology of the left anterior descending artery and 12 months clinical outcome: The CLIMA study. Eur Heart J 41(3): 383-391.
- Pu Z, Hakim D, Croce K, Stone PH (2020) Preemptive percutaneous coronary intervention for coronary artery disease: Identification of the appropriate high-risk lesion. Curr Opin Cardiol 35(6): 712-719.
- Raisis-Estabragh Z, Mamas MA (2022) Cardiovascular health care implications of the COVID-19 pandemic. Cardiol Clin 40(3): 389-396.
- Ramadani RV, Svensson M, Hassler S, Hidayat B, Ng N (2024) Effects of the COVID-19 pandemic on healthcare utilization among older adults with cardiovascular diseases and multimorbidity in Indonesia: An interrupted time-series analysis. BMC Public Health 24(1): 71.
- Ramoni D, Carbone F, Kraler S, Di Vece D, Montecucco F, et al. (2025) Inflammation-driven plaque erosion in atherosclerosis: A focus on complement system pathways. Curr Atheroscler Rep 27(1): 42.
- Riascos-Bernal DF, Quinones G, Abdelaal SA, Menegus MA, Sibinga NES (2025) Pathogenesis of plaque erosion. Trends Cardiovasc Med 27(1): 42.
- Rigattieri S, Redivo M, Casenghi M, Belmonte M, Giovannelli F, et al. (2025) Management of coronary vulnerable plaques: a focus on preventive percutaneous coronary intervention. Rev Cardiovasc Med 26(4): 26712.
- Rivera FB, Cha SW, Varona MC, Fernandez Co EM, Magalong JV, et al. (2024) Atherosclerotic coronary plaque regression from lipid-lowering therapies: A meta-analysis and meta-regression. Am J Prev Cardiol 18: 100645.
- Rola P, Kulczycki JJ, Barycki M, Włodarczak S, Furtan Ł, et al. (2023) Comparison of orbital atherectomy and rotational atherectomy in calcified left main disease: Short-term outcomes. J Clin Med 12(12): 4025.
- Romero Starke K, Kaboth P, Rath N, Kaempf D, Nienhaus A, et al. (2024) cardiovascular disease risk after a SARS-CoV-2 infection: A systematic review and meta-analysis. J Infect 89(3): 106215.
- Russo M, Bacigalupi E, Radico F, Scorpiglione L, Gurgoglione FL, et al. (2025) Prognostic role and therapeutic implications of intravascular optical coherence tomography detected coronary plaque microstructures in patients with coronary artery disease. J Clin Med 14(22): 8132.
- Sakamoto A, Cornelissen A, Sato Y, Mori M, Kawakami R, et al. (2022) Vulnerable plaque in patients with acute coronary syndrome: Identification, importance, and management. US Cardiol 16: e01.
- Sanchez A, Mejia A, Sanchez J, Runte E, Brown-Fraser S, et al. (2019) Diets with customary levels of fat from plant origin may reverse coronary artery disease. Med Hypotheses 122: 103-105.
- Sarraju A, Nissen SE (2024) Atherosclerotic plaque stabilization and regression: A review of clinical evidence. Nat Rev Cardiol 21(7): 487-497.
- Sastry S, Cuomo F, Muthusamy J (2022) COVID-19 and thrombosis: The role of hemodynamics. Thromb Res 212: 51-57.
- Satija A, Bhupathiraju SN, Spiegelman D, Chiuve SE, Manson JE, et al. (2017) Healthful and unhealthful plant-based diets and the risk of coronary heart disease in U.S. adults. J Am Coll Cardiol 70(4): 411-422.
- Seth R, McKinnon TAJ, Zhang XF (2022) Contribution of the von Willebrand factor/ADAMTS13 imbalance to COVID-19 coagulopathy. Am J Physiol Heart Circ Physiol 322(1): H87-H93.
- Servito M, Yan W, Namkoong J, Vervoort D, Fremes SE (2025) Revascularization in chronic coronary syndrome: Shifts in clinical practice guidelines. Curr Opin Cardiol 40(5): 357-366.
- Sgreva S, Alsubai SE, Bianchini E, Alqahtani F, Del Sole PA, et al. (2025) Plaques do not act alone: time to redefine coronary vulnerability from lesion to phenotype. J Clin Med 14(21): 7568.
- Shovlin CL, Vizcaychipi MP (2023) Vascular inflammation and endothelial injury in SARS-CoV-2 infection: The overlooked regulatory cascades implicated by the ACE2 gene cluster. QJM 116(8): 629-634.
- Sikand G, Severson T (2020) Top 10 dietary strategies for atherosclerotic cardiovascular risk reduction. Am J Prev Cardiol 4: 100106.
- Spagnolo M, Giacoppo D, Laudani C, Greco A, Finocchiaro S, et al. (2025) Advances in the detection and management of vulnerable coronary plaques. Circ Cardiovasc Interv 18(8): e015529.
- Spetz M, Natt och Dag Y, Li H, Nyberg F (2025) Covid-19 and cardiovascular disease in a total population-study of long-term effects, social factors and Covid-19-vaccination. Nat Commun 16(1): 10115.
- Stanescu AG, Benedek I, Opincariu D, Hodas R, Ratiu M, et al. (2021) Assessment of lesion-associated myocardial ischemia based on fusion coronary CT imaging: The FUSE-HEART study. Medicine (Baltimore) 100(14): e25378.
- Steg PG, Szarek M, Jukema JW, Bhatt DL, Bittner VA, et al. (2025) Relation of low-density lipoprotein cholesterol, high-sensitivity C-reactive protein, and lipoprotein(a) each to future cardiovascular events and death after acute coronary syndrome on high-intensity statin therapy: An analysis of the placebo arm of ODYSSEY OUTCOMES. Circulation 151(14): 1047-1050.
- Stone GW, Ali ZA, O'Brien SM, Rhodes G, Genereux P, et al. (2023) Impact of complete revascularization in the ISCHEMIA trial. J Am Coll Cardiol 82(12): 1175-1188.
- Stone GW, Maehara A, Ali ZA, Held C, Matsumura M, et al. (2020) Percutaneous coronary intervention for vulnerable coronary atherosclerotic plaque. J Am Coll Cardiol 76(20): 2289-2301.
- Stone GW, Maehara A, Lansky AJ, de Bruyne B, Cristea E, et al. (2011) A prospective natural-history study of coronary atherosclerosis. N Engl J Med 364(3): 226-235.
- Stone PH, Libby P, Boden WE (2023) Fundamental pathobiology of coronary atherosclerosis and clinical implications for chronic ischemic heart disease management-the plaque hypothesis: A narrative review. JAMA Cardiol 8(2): 192-201.
- Sucato V, Ortello A, Comparato F, Novo G, Galassi AR (2024) Cholesterol-lowering strategies for cardiovascular disease prevention: The importance of intensive treatment and the simplification of medical therapy. J Clin Med 13(7): 1882.
- Swastini DA, Wiryanthini IAD, Ariastuti NLP, Muliantara A (2019) Atherosclerosis prediction with high sensitivity C-reactive protein and related risk factor in patients with dyslipidemia. Open Access Maced J Med Sci 7(22): 3887-3890.
- Szymańska C, Baszko A (2025) Artificial intelligence tools in myocardial infarction prognosis: Evaluating the performance of machine learning and deep learning models. Curr Cardiol Rev.
- Takahashi K, Serruys PW, Gao C, Ono M, Wang R, et al. (2021) Ten-year all-cause death according to completeness of revascularization in patients with three-vessel disease or left main coronary artery disease: Insights from the SYNTAX Extended Survival Study. Circulation 144(2): 96-109.
- Takahashi T, Gupta A, Samuels BA, Wei J (2023) Invasive coronary assessment in myocardial ischemia with no obstructive coronary arteries. Curr Atheroscler Rep 25(10): 729-740.
- Tan Y, Sheng Z, Zhou P, Liu C, Zhao H, et al. (2019) Plasma trimethylamine N-oxide as a novel biomarker for plaque rupture in patients with ST-segment-elevation myocardial infarction. Circ Cardiovasc Interv 12(1): e007281.
- Tern PJW, Jiang Y, Lau YH, Almahmeed W, Selvaraj SG, et al. (2022) Impact of COVID-19 on acute MI and percutaneous coronary intervention rates and outcomes in South East Asia and the Middle East. J Asian Pac Soc Cardiol 1: e05.
- Theofilis P, Vlachakis PK, Papanikolaou A, Karakasis P, Oikonomou E, et al. (2024) Coronary plaque erosion: Epidemiology, diagnosis, and treatment. Int J Mol Sci 25(11): 5786.
- Theofilis P, Oikonomou E, Chasikidis C, Tsioufis K, Tousoulis D (2023) Pathophysiology of acute coronary syndromes-diagnostic and treatment considerations. Life 13(7): 1543.
- Thondapu V, Mamon C, Poon EKW, Kurihara O, Kim HO, et al. (2021) High spatial endothelial shear stress gradient independently predicts site of acute coronary plaque rupture and erosion. Cardiovasc Res 117(8): 1974-1985.
- Tomaniak M, Katagiri Y, Modolo R, de Silva R, Khamis RY, et al. (2020) Vulnerable plaques and patients: State-of-the-art. Eur Heart J 41(31): 2997-3004.
- Tsampasian V, Bäck M, Bernardi M, Cavarretta E, Dębski M, Gati S, et al. (2025) cardiovascular disease as part of long COVID: A systematic review. Eur J Prev Cardiol 32(6): 485-498.
- Tuso P, Stoll SR, Li WW (2015) A plant-based diet, atherogenesis, and coronary artery disease prevention. Perm J 19(1): 62-67.
- Ueyama HA, Akita K, Kiyohara Y, Takagi H, Briasoulis A, et al. (2025) Optimal strategy for complete revascularization in ST-segment elevation myocardial infarction and multivessel disease: A network meta-analysis. J Am Coll Cardiol 85(1): 19-38.
- van Veelen A, van der Sangen NMR, Henriques JPS, Claessen BEPM (2022) Identification and treatment of the vulnerable coronary plaque. Rev Cardiovasc Med 23(1): 39.
- van Veelen A, van der Sangen NMR, Delewi R, Beijk MAM, Henriques JPS (2022) Detection of vulnerable coronary plaques using invasive and non-invasive imaging modalities. J Clin Med 11(5): 1361.
- van Veelen A, Küçük IT, Fuentes FH, Kahsay Y, Garcia-Garcia HM, et al. (2024) Correction: First-in-human drug-eluting balloon treatment of vulnerable lipid-rich plaques: Rationale and design of the DEBuT-LRP study. J Clin Med 13(5): 1479.
- Vazquez-Figueroa JG, Rinehart S, Qian Z, Joshi PH, Sharma A, et al. (2013) Prospective validation that vulnerable plaque associated with major adverse outcomes have larger plaque volume, less dense calcium, and more non-calcified plaque by quantitative three-dimensional measurements using intravascular ultrasound with radiofrequency backscatter analysis: results from the ATLANTA I study. J Cardiovasc Transl Res 6(5): 762-771.
- Vergallo R, Park SJ, Stone GW, Erlinge D, Porto I, et al. (2025) Vulnerable or high-risk plaque: A JACC: Cardiovascular Imaging position statement. JACC Cardiovasc Imaging 18(6): 709-740.
- Virmani R, Burke AP, Farb A (1999) Plaque rupture and plaque erosion. Thromb Haemost 82(Suppl 1): 1-3.
- Vosko I, Zirlik A, Bugger H (2023) Impact of COVID-19 on cardiovascular disease. Viruses 15(2): 508.
- Wang C, Wu X, Liu Y, Qiu X, Su H, et al. (2025) Association between coronary plaque vulnerability features and multiparametric pericoronary fat indices on coronary computed tomography angiography: A cross-sectional study. Quant Imaging Med Surg 15(8): 6897-6909.
- Wang J, Li Y, Lei M, Guan Z, Zhao Z, et al. (2025) COVID-19 with acute myocardial infarction evaluated using multimodal imaging: A case report. Medicine 104(29): e43412.
- Watzl B (2008) Anti-inflammatory effects of plant-based foods and of their constituents. Int J Vitam Nutr Res 78(6): 293-298.
- Williams T, Mittal A, Karageorgiev D, Iniguez Romo A, Aminian A, et al. (2022) Complete revascularization optimizes patient outcomes in multivessel coronary artery disease: Data from the e-Ultimaster registry. Catheter Cardiovasc Interv 99(4): 961-967.
- Xia J, Bachour K, Suleiman AM, Roberts JS, Sayed S, et al. (2024) Enhancing coronary artery plaque analysis via artificial intelligence-driven cardiovascular computed tomography. Ther Adv Cardiovasc Dis 18: 17539447241303399.
- Xiu L, Zhao P, Gu X, Yu B (2025) Role of trimethylamine N-oxide in assessing plaque instability of the culprit lesion in Chinese patients with ST-elevation myocardial infarction: Insights from a 7-year long-term follow-up study. Clin Transl Sci 18(9): e70357.
- Xu X, Fang C, Jiang S, Chen Y, Zhao J, et al. (2025) Functional or anatomical assessment of non-culprit lesions in acute myocardial infarction. EuroIntervention 21(4): e217-e228.
- Yamaji K, Kohsaka S, Inohara T, Numasawa Y, Ando H, et al. (2022) Percutaneous coronary intervention during the COVID-19 pandemic in Japan: Insights from the nationwide registration data. Lancet Reg Health West Pac 22: 100434.
- Yang S, Koo BK, Hoshino M, Lee JM, Murai T, et al. (2021) CT angiographic and plaque predictors of functionally significant coronary disease and outcome using machine learning. JACC Cardiovasc Imaging 14(3): 629-641.
- Yang S, Koo BK, Narula J (2022) Interactions between morphological plaque characteristics and coronary physiology: from pathophysiological basis to clinical implications. JACC Cardiovasc Imaging 15(6): 1139-1151.
- Yasmin F, Shujauddin SM, Naeem A, Jabeen A, Shah SMIS, et al. (2021) Exploring the impact of the COVID-19 pandemic on provision of cardiology services: a scoping review. Rev Cardiovasc Med 22(1): 83-95.
- Yasumura K, Koshy AN, Vinayak M, Vengrenyuk Y, Minatoguchi S, et al. (2024) Rotational, orbital atherectomy and intravascular lithotripsy for coronary calcified nodules: Insights from optical coherence tomography. Catheter Cardiovasc Interv 104(7): 1373-1386.
- Yoo SM, Lee HY, Jin KN, Chun EJ, Ann FA, et al. (2017) Current concepts of vulnerable plaque on coronary CT angiography. Cardiovasc Imaging Asia 1(1): 4-12.
- Zimmermann FM, Pijls NHJ, Gould KL, Johnson NP (2021) Stenting “vulnerable” but fractional flow reserve-negative lesions: potential statistical limitations of ongoing and future trials. JACC Cardiovasc Interv 14(4): 461-467.
-
Prof. Dasaad Mulijono. Complete Revascularization in a Time of Crisis: Why Treating Mild and Moderate CTCA-Detected Vulnerable Lesions was Lifesaving during the COVID-19 Pandemic. On J Cardio Res & Rep. 8(2): 2025. OJCRR.MS.ID.000685.
-
COVID-19; vulnerable plaque; CT-coronary angiography; complete revascularization; preventive PCI; plaque erosion; endotheliitis; hypercoagulability; artificial intelligence; lifestyle medicine; whole-food plant-based diet; crisis cardiology; biological risk
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
- Abstract
- Introduction
- The Pandemic Exposed the Weaknesses of the Stenosis-Centric Model
- When Emergency Systems Collapse, Waiting for Ischemia is Unsafe
- CTCA Became the Only Viable Tool for Biological Risk Detection
- CR Was Biologically and Operationally Necessary
- Vulnerability-Guided Intervention: Key Evidence
- Ethical Principles Support Preventive PCI in Crisis Conditions
- Aviation Medicine Offers a Validating Parallel
- A Window into the Future of Coronary Medicine
- The Legends’ Perspective - Braunwald and Fuster on Our Approach
- Reflections on Criticism During Crisis: Understanding the Divide Between Biological Insight and Clinical Absence
- Conclusion
- Author Contributions
- Funding
- Institutional Review Board Statement
- Informed Consent Statement
- Data Availability Statement
- Conflict of Interest
- References






