 Mini review
Mini review
Selective Systematic Review: Planned Healthcare Environments Impact on Healing, Health and Well-being
Karen L Hoblet1* and Sahar Atshan2
1College of Nursing, The University of Toledo, USA
2Staff Nurse, Beaumont Hospital, Ireland
Karen L Hoblet, Associate Professor, College of Nursing, The University of Toledo, USA.
Received Date: July 02, 2020; Published Date: August 17, 2020
Abstract
Aim: The objective of this study was to review research to determine if evidence existed to support the assertion that planned healthcare environments utilizing evidence-based design improve healing, health and well-being.
Background:Millions of people are treated in hospitals in the United States annually [1]. These facilities are environments where people interact with healthcare experts to achieve healing, health, and wellbeing.
Purpose: The literature was investigated to determine if evidence-based design, the planned design of healthcare facilities, impacts human healing, health, and wellbeing.
Methods:A systematic review of selected literature was planned and attempted utilizing PRISMA 27-item check list and four-phase flow diagram. Databases included the Cumulative Index of Nursing and Allied Health Literature (CINAHL), Psych INFO produced by the American Psychological Association, and PubMed search engine of the MEDLINE database of references and abstracts from the United States National Library of Medicine at the National Institutes of Health. This exploration included research and literature regarding the design and development of planned healthcare environments that promote healing, health and wellbeing and the consideration of theory that supports the significance of environment in human development.
Results:No evidence was found that support the assertion that planned healthcare environments utilizing evidence-based design improve healing, health and well-being. Limited research evidence prohibited organization and reporting using PRISMA.
Conclusion:b> Research should be completed utilizing a design that helps determine if there is a relationship between planned healthcare environments and healing, health, and well-being.
Keywords:Evidence-based design; Healing; Health; Wellbeing
Introduction
People are treated in healthcare facilities across the globe. The Centers for Disease Control and Prevention, Summary Health Statistics: National Health Interview Survey, 2016 reported that over 36 million people are treated in hospitals across the United States (U.S.) annually [2]. These healthcare organizations are environments where people interact with healthcare experts to achieve healing, health, and wellbeing. This article was developed to share outcomes from a selective systematic review of the literature to determine if planned or built healthcare environments improve healing, health and well-being. This exploration included research and literature regarding the design and development of planned healthcare environments that promote healing, health and wellbeing [3-13].
Background
“The physical facilities in which health care services are performed play an important role in the healing process” [12]. Available evidence in print indicated a possible correlation between the planned or built healthcare environment and patient healing, health, and well-being, but no level one research evidence was identified during this review. In fact, research evidence regarding the impact of the planned or built healthcare environment on healing, health and well-being is minimal at best.
Evidence-based design in architecture and interior design is a relatively new field which involves taking patient preferences into account when designing healthcare facilities but is not based on best research evidence. The use of the term evidence-based design can be confusing for healthcare professionals whose focus on patient care outcomes is often based upon best research evidence, known as evidence-based practice.
Examination of literature found articles on evidence-based design which may be misleading to healthcare professionals who utilize the process of evidence-based practice to improve safety, quality, and performance outcomes of patient care. Evidencebased design (EBD) in architecture and interior design refers to preferences and work processes in designing and building healthcare environments. These two different evidence-based foci may cause confusion for the public. One such statement “EBD offers data on what works and what does not; it brings empiricism to the design process to support imagination, judgment, and evaluation. It makes perfect sense to use the best available evidence to create a healthcare facility that will be used for many years and for which so much is at stake” [12].
These types of statements can confuse readers who assume that the field of evidence-based design is based upon best research evidence. Currently the literature does not support this.
The work most often cited in the literature reviewed was directed by The Center for Health Design, Quality of Care Research, Johns Hopkins. This work completed in 1998 was a systematic review of research regarding healthcare facility design which defined the healthcare environment as “anything that can affect a patient through the senses” [8]. Inclusion criteria for the Johns Hopkins systematic review began by brainstorming with staff from The Center for Health Design and yielded a list of environmental design features to be studied [8]. The Center for Health Design Research Committee finalized the list of design features for inclusion [8]. Inclusion criteria included the following design features: room scale, room size, room privacy, room organization, environmental control by patient, room flow or interactivity, lighting, color or walls and furnishing, texture or finishing of walls and furnishing, pattern of walls, furnishings and artwork, type of furnishings, air and ventilation, aroma, noise, music, temperature, relationship with nature, equipment design, windows, and type of view from windows [8]. This inclusion criteria resulted in 78,761 articles being reviewed. The researchers found methodological flaws in many of the works reviewed [8]. Many of the articles involved patients observed in different built environments with different design features [8]. No blinded studies were identified. Lastly, no direct correlation was statistically noted regarding planned or built environments and improved healing, health, and well-being.
Schweitzer, Gilpin, Frampton, [9], “Most relevant research has been concentrated on a limited number of settings and is inadequate to inform the creation of design guidelines for the physical elements of an optimal healing environment” [9]. Unfortunately, this depiction of Nightingale’s work misrepresented the thrust of the differences she noted in healthcare facilities which focused on sanitation and care provision. Nightingale had nurses scrub floors, walls, bedding, and patients. Nightingale also lobbied for digging and clearing human waste channels to prevent the spread of disease. Nightingale’s efforts focused on improving the quality of the air, access to sunlight, and cleanliness of environments where care was delivered. Nightingale was known to have worked on the design of facilities that promoted sanitation and care [14].
Schweitzer, et al. [9], further stated that “modern healthcare environments are cluttered, noisy with little regard for the impact on patients” [9]. This portrayal of healthcare environments could be accurate in some organization but presents generalization that all healthcare organizations are cluttered and noisy without regard to patients. Healthcare organizations are built environments where people come for healthcare services. These facilities have evolved over time to deliver more effective and efficient quality care. Understanding if the aesthetic design of these environments has a relationship to healing, health, and well-being in delivering care is of importance. This paper will examine available literature to determine if supports can be found that evidence-based design promotes or improves healing, health, and well-being.
Purpose
The purpose of this article is to present work done for a capstone project in a graduate nursing program. The aim of the project was to complete a selective systematic review of the literature regarding planned healthcare environments to determine available research regarding environmental components that would improve healing, health and well-being. Ethical and theoretical components are presented to emphasize the importance of environment in advocating healing, health, and well-being. The methodology and design of this work is summarized for appreciation of the perspective presented as well as discussion of the results that led to conclusions and recommendation for future work.
Ethical Foundation and Theoretical Support
Ethical foundation
The nursing profession is known to be an honorable field with altruistic values. The American Nurses Association Code of Ethics for Nurses highlights these values with nine Provisional statements.
“Provision 1. The nurse practices with compassion and respect for the inherent dignity, worth, and unique attributes of every person.,
Provision 2. The nurse’s primary commitment is to the patient, whether an individual, family, group, community, or population.,
Provision 3. The nurse promotes, advocates for, and protects the rights, health, and safety of the patient., Provision 4. The nurse has authority, accountability and responsibility for nursing practice; makes decisions; and takes action consistent with the obligation to provide optimal patient care.,
Provision 5. The nurse owes the same duties to self as to others, including the responsibility to promote health and safety, preserve wholeness of character and integrity, maintain competence, and continue personal and professional growth.,
Provision 6. The nurse, through individual and collective effort, establishes, maintains, and improves the ethical environment of the work setting and conditions of employment that are conducive to safe, quality health care., Provision 7. The nurse, in all roles and settings, advances the profession through research and scholarly inquiry, professional standards development, and the generation of both nursing and health policy.,
Provision 8. The nurse collaborates with other health professionals and the public to protect human rights, promote health diplomacy, and reduce health disparities.,
Provision 9. The profession of nursing, collectively through its professional organizations, must articulate nursing values, maintain the integrity of the profession, and integrate principles of social justice into nursing and health policy.” [15].
Theoretical support
Nurses care for people in a variety of environments to promote healing, health, and well-being. “The central concepts and themes of the discipline of nursing are identified and formalized as nursing’s metaparadigm” [16]. The metaparadigm, grand theoretical components of the discipline of nursing, include four essential components which must be the focus of comprehensive care and practice. These four components include: person, environment, health, and nurse. The interaction of the person within their environment is known to impact their health. Nursing, through holistic assessment of the person and environment can develop a comprehensive, prioritized, plan of care (nursing process) to improve healing, health, and well-being.
Orem D [17], developed the self-care deficit theory of nursing to illustrate how nurses who understand the importance of the metaparadigm can develop individualized plans of care utilizing a system of assessment based on universal requisites for all human beings to improve health and well-being. These requisites include developmental requisites and universal self-care requisites. Orem posited that through assessment a nurse can identify self-care and developmental deficits that if addressed through well-planned nursing systems, can improve the health and well-being of persons in their care [17].
Orem [17], developed the self-care deficit theory of nursing to illustrate how nurses who understand the importance of the metaparadigm can develop individualized plans of care utilizing a system of assessment based on universal requisites for all human beings to improve health and well-being. Erikson [18], posited that humans develop a unique identity based upon “innate” traits inherited through genetics and interaction with the environments in which they grow and develop. Thus, each person’s identity is distinctive due to the variation in genetic combination and extensive sociocultural influences that occur in the environment in which they developed from infancy through adulthood. Erikson [23] eight stages of development present challenges that all persons must successfully navigate to adapt and thrive in their environment. These stages are:
<1. trust versus mistrust,
<2. autonomy versus shame,
<3. initiative versus guilt,
<4. industry versus inferiority,
<5. identity versus role confusion,
<6. identity versus role confusion,
7. generativity versus stagnation, and
<8. ego integrity versus despair.
Environmental determinants influence each stage in human development and impact, positively or negatively, how a person responds to healthcare providers and healthcare environments. Piaget J [21], theory of cognitive development explains how a child constructs a mental model of the world. Piaget posited that intelligence was not genetic predisposed but developed through biological development and maturation through interaction with the environment. This was reinforced by McLeod, “Children are born with a very basic mental structure (genetically inherited and influenced by environment) on which all subsequent learning and knowledge are based” [24]. Thus, each person’s lived experiences build their mental model or perceptions of healthcare and healthcare environments.
Maslow is perhaps most well-known for his theory on human development [20]. This theory is known as the hierarchy of needs theory. Maslow proposed that all human beings have common needs that must be addressed and met in a sequential order [20]. Lower level needs must be secured or met before higher level needs could be realized [20]. Maslow’s hierarchy is visually presented as a pyramid, with physiological needs at the bottom and selfactualization needs at the top. Hierarchy of needs exemplifies how the needs are layered and each person must meet the most basic physiological needs required for human survival (air, food, water) before moving on to higher level needs. The second level needs are safety and security. Ascending upward to the third level, love and belonging needs, followed by esteem for self which allows humans to attain the highest level of development called self-actualization and transcendence needs. Maslow [20] specified that each developmental need must be addressed, fulfilled prior to advancing to the next level. This process of development continues throughout each person’s life [19]. One can apprciate how experience with healthcare professionals in healthcare environments could impact perceptions and outcomes of care.
Bronfenbrenner [22], ecological systems theory stated that human development is influenced by different environmental systems.These systems include:
• the micro system which is the social system closest to a person that is experienced throughout life (family, friends, teachers, and others),
• the mesosystem is the system that influences interactions between persons in the microsystem and other systems,
• the exo-system is the system of cognitive connection a person experiences without active participation, but still influences a person’s development,
• the macrosystem is the cultural system or influences that a person is exposed and connected to, and
• the chronosystem is the transitions in development that are experienced by a person over their lifetime [22].
Bronfenbrenner [22], explains how people can act differently in a variety of social interactions, the difference of action at home with family members, in school, in church, or at work, or during extreme illness in healthcare facilities. These theories highlight the importance of environment in supporting human growth and development. These theories provide an appreciation for consideration of how planned healthcare environments should be well designed to promote efficient, effective, quality care that is delivered by competent, caring professionals.
Methods
The nursing profession utilizes tools to guide evidence-based methodology. “PICO” is one such tool which helps to determine the research question. The “P” represents population, the “I”, intervention, the “C” comparison or intervention, and the “O”, is the outcome one would like to achieve. Utilization of PICO resulted in the following questions guiding this work, “Does the esthetic environment in which hospitalized patients are cared for impact healing, health, and well-being?”.
The next step in this work was to determine what study design/methodology would best answer the research question. The research team, graduate nursing student and Associate Professor, contacted the university librarian to discuss a literature search of the concepts evidence-based design, healing, health, and well-being of hospitalized patients. Determination to conduct a selective systematic review of the literature regarding evidencebased design, healing, health, and well-being occurred following a cursory exploration of the literature in these areas which yielded no research studies and a few articles on the subject. A second meeting with the university librarian honed the search design to include literature from 1970 [19] through 2019 [20] and broadened the eligibility criteria to be utilized in the search. and broadened the eligibility criteria to be utilized in the search. The recommendation from the university librarian was to focus the search using two of the most common healthcare data bases Cumulative Index of Nursing and Allied Health Literature (CINAHL) and PubMed the free search engine of the MEDLINE database of references and abstracts from the United States National Library of Medicine at the National Institutes of Health, and Psych INFO produced by the American Psychological Association, which contained psychological and behavioral research.
Assessment of the articles was completed by simultaneous review of each article title and abstracts. Eligibility criteria were used to refine the list of articles that would be evaluated in more depth. Both of the team members reviewed all articles listed to determine if the article met eligibility requirements. This process led to the creation of a final list of articles for review. Further explanation of the methods of this work are detailed in the discussion below regarding study design, data extraction, data analysis, and results.
Design
The selected systematic review of the literature utilized the following eligibility criteria: health care environments, planned environment, built environment, planned healthcare environment, acute care, hospital, aesthetic, architecture, interior design, room design, design, healing, health, well-being, wellness, patient, client, patient perspective, patient perspective, recovery, and rehabilitation. Table 1 provides eligibility criteria that were explored in the selected databases. Twenty-one criteria were included in the hope of finding research supporting a relationship between planned healthcare environment and healing, health, and wellbeing. A review and discussion of eligible search criteria resulted in narrowing the key eligibility terms to environment, patient, and health. Literature search of the electronic databases included at least two key eligibility criteria. Optimally, a desired article would include all three key eligibility words. When looking at articles that were relevant to the topic, the majority only included two of the desired key eligibility criteria. For example, one article discussed the interest of patient and healing but did not include environment. Ultimately, these articles were not included in the final literature review (Table 1).
The literature search was conducted using three respected databases, the Cumulative Index of Nursing and Allied Health Literature (CINAHL), Psych INFO which is produced by the American Psychological Association for the field of psychology, and PubMed which is the free search engine of the MEDLINE database of references and abstracts from the United States National Library of Medicine at the National Institutes of Health. The search conducted in February 2019 yielded a total of 2237 articles. The literature search yield is displayed in (Table 2).
Table 1: Eligibility Criteria Explored.
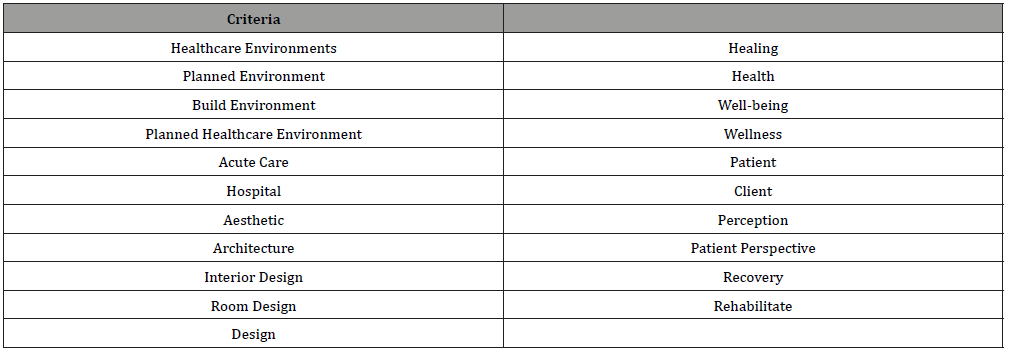
Table 2: Literature Search Yield.
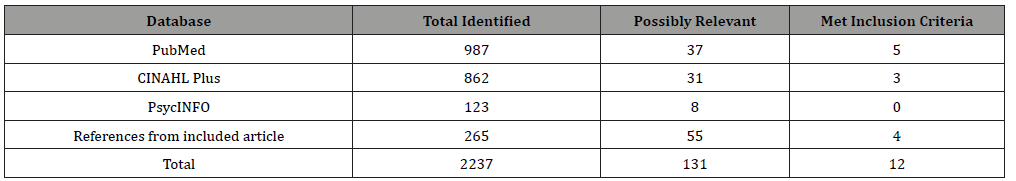
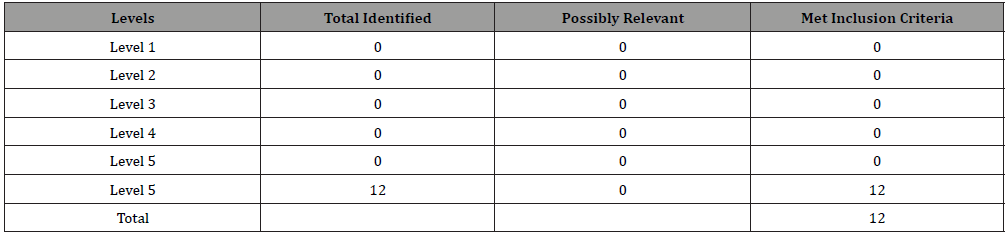
Table 3: Level of Evidence for Literature Identified.
Review and assessment of all 2237 articles for possible inclusion in the systematic review of planned healthcare environments that promote healing, health, and wellbeing was completed. The assessment of the articles from the databases resulted in a total of 1972 articles identified using the selected key criteria and criteria factors. Of that total, 0.04% were identified as relevant to those key criteria and criteria factors and only eight out of 1972 (0.004%) were included in the final systematic literature selection. The references from the eight articles which were selected were also reviewed for consideration and inclusion. Of these additional 265 articles noted in the references, only 4 were included in the final selection of the literature. In total, from an original search of 2237 articles, only 12 were included in the final select review of literature.
Results
Brown, 2009, stated the levels of evidence include “Level 1 supported by main finding from one randomized, experimental study with a statistically significant difference in group outcomes, Level 2 supported by one cohort study with a statistically significant difference in group outcomes, Level 3 supported by descriptive finding of at least one cohort study, Level 4 reported as an incidental finding in at least one study and endorsed by two thirds (2/3) of the panel, Level 5 supported by endorsement of by two thirds (2/3) of the panel” (p.224). According to Brown’s, 2009, levels of evidence, the literature identified was limited and noted to be at a Level 5 at best, but most were noted to be less than Level 5. Table 3 provides levels of evidence for the literature included in this work (Table 3).
Conclusion
No literature regarding the planned or built healthcare environment (evidence-based design) demonstrated an impact on improving healing, health and well-being [3-13]. “Ulrich noted that there are a “limited number of scientific studies on the links between environmental characteristics and outcomes. The amount of research is growing, but there is no sound, directly relevant research yet available for many healthcare designs questions or situations”. It is difficult to determine if environmental design of healthcare facilities impact healing, health, and well-being based upon the current level of available research. The works of Nightingale focused on sanitary controls which research evidence has shown to control and in some cases eliminate infection disease, thus promoting healing, health, and well-being.
Recommendations
Patient preference for design elements such as color of wall, floors, and visual availability of the outside environment were noted in the majority of the literature reviewed. It is difficult to determine any impact that environmental design has on healing, health, and well-being without further study. More randomized control studies focusing on environmental design must be completed to determine if design elements directly impact healing, health, and well-being. Opportunities exist to make meaningful contribution in this area that are likely to make a significant impact on health outcomes of human beings.
Research focused on how planned healthcare environmental design impacts human factors within these environments must go beyond patient preference. These environments are constructed to facilitate care delivery services to improve health and promote healing and well-being. Quality human interactions within healthcare environments planned to enhance well-being and promote healing and health should be examined along with design elements that promote quality interaction and function. The importance of environment and in particular healthcare environments has not been studied sufficiently to provide evidence on how to build the best planned structures to facilitate and enrich human interactions which promotes healing, health, and well-being for all who are served and receive services within these important environments.
Acknowledgement
Jodi Jameson, University of Toledo Librarian, Toledo, Ohio.
Conflict of Interest
No conflicts of interest.
References
- S. Department of Health and Human Services (2016) Summary Health Statistics: National Health Interview Survey. Centers for Disease Control and Prevention, National Center for Health Statistics.
- Freeman WJ, Weiss AJ, Heslin KC (2018) Overview of U.S. Hospital Stays in 2016: Variation by Geographic Region. Agency for Healthcare Research and Quality, Rockville, USA.
- Bishop LP, Griffin C (2006) Natural, patient-centered environments bring quality healthcare full circle by addressing patients’ spiritual, social, and emotional needs. Nursing Management: 31-35.
- Caspari S, Eriksson K, Naden D (2006) The aesthetic dimension in hospitals – An investigation into strategic plans. Int J Nurs Stud 43(7): 851-859.
- Laursen J, Danielsen A, Rosenberg J (2014) Effects of environmental design on patient outcome: A systematic review. HERD 7(4): 108-119.
- McKahan DC (1993) Healing environments: Healing by design – therapeutic environments for healthcare. J Healthc Des 5: 159-166.
- Patterson ES, Sanders, EBN, Sommerich CM, Lavender SA, Li J, et al. (2017) Meeting patient expectations during hospitalization: A grounded theoretical analysis of patient-centered room elements. HERD 10(5): 95-110.
- Rubin HR (1998) Status Report 1998: An investigation to determine whether the built environments affects the patients’ medical outcomes. J Healthc Des 10: 11-13.
- Schreuder E, Liebesque L, Bottenheft C (2016) Healing environments: What design factors really matter according to patients? An exploratory analysis. HERD 10(1): 87-105.
- Schwietzer MA, Gilpin L, Frampton S (2004) Healing spaces: Elements of environmental design that make an impact on health. J Altern Compliment Med 10 Suppl 1: S71-S83.
- Ulrich RS (2014) Evidence based environmental design for improving medical outcomes.
- Ulrich RS, Berry LL, Quan X, Parish JT (2010) A conceptual framework for the domain of evidence-based design. HERD 4(1): 95-114.
- Ulrich RS (2001) Effects of healthcare environmental design on medical outcomes. Cite Seer.
- Hong M (2015) Principles of healthcare design: Florence Nightingale’s legacy in Tucson’s desert sanatorium. Arizona State University, USA.
- Silver Spring (2015) American Nurses Association Code of ethics with interpretative statements.
- Fawcett J (1984) The metaparadigm of nursing: Present status and future refinements. Image J Nurs Sch 16(3): 84-89.
- Orem D (1991) Self-care deficit theory of nursing. Sage Publications, Inc, Newbury Park: London.
- Erikson EH (1964) Childhood and society. Norton, New York, USA.
- Maslow A H (1970) Motivation and Personality. Harper & Row, New York, USA.
- Maslow AH (1943) A theory of human motivation. Psychological Review 50(4): 370-396.
- Piaget J (1966) The child's conception of physical causality. Littlefield, Adams, Totowa, USA.
- Bronfenbrenner U (2005) Making human beings: Bioecological perspectives on human development. Sage Publications Inc, Thousand Oaks, USA.
- Erikson EH (1974) Dimensions of a new identity. Norton, New York, USA.
- McLeod S (2018) Jean Piaget’s theory of cognitive development. Simply Psychology.
- (2019) Erik Erikson’s theory of psychosocial development. Psychology Notes HQ.
- Maslow AH (1968) Toward a psychology of being. Van Nostrand Reinhold, New York, USA.
- Piaget J (1978) Behavior and evolution. Pantheon Books, New York, USA.
- Sincero SM (2019) Ecological systems theory. Explorable, Think Outside the Box.
-
Karen L Hoblet, Sahar Atshan. Selective Systematic Review: Planned Healthcare Environments Impact on Healing, Health and Well-being. On J Complement & Alt Med. 5(1): 2020. OJCAM.MS.ID.000605.
-
Evidence-based design, Healing, Health, Wellbeing, Psychological Association, Healthcare, Nursing, Allied Health Literature, Brainstorming
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






