 Research Article
Research Article
Dietary Supplements and Supplemented Diets
Dénes Kleiner1,2*, Hegyi Gabriella3, István Horváth1, Mária Matuz4, Magdolna Dank2, and Balázs Hankó1
1University Pharmacy Department of Pharmacy Administration, Semmelweis University, Hungary
2Semmelweis University Oncology Center, Budapest, Hungary
3Pecs University, CAM Department, Doctoral School, Hungary
4Department of Clinical Pharmacy, University of Szeged, Hungary
Gabriella Hegyi, Pecs University, CAM Department, Doctoral School, Hungary, Pecs, Vörösmarty u.4.Hungary.
Received Date:May 15, 2021; Published Date:September 09, 2021
Abstract
With the spreading of complementary and alternative medicine, countless questions were raised. These queries are particularly important in the field of oncology, where patients seek every possibility to cure cancer. Most oncology treatments have narrow therapeutic index, thus patients more likely to use some as these complementary agents. We wanted not just to measure the use of these complementary products, but also to estimate the patient’s knowledge about them with a guided interview in the Semmelweis University Oncology Center. At the end of the study 71 patients answered the questionnaire. Most of them (91,6%) used products, that contained only vitamin(s). We also measured those regularly consumed foods, which were not functional foods, nor dietary supplements but may influence the bioavailability of drugs (e.g.: daily consumed herbal teas). These agents were utilized by 80,2% of the participants. From the results, it should be also highlighted, that some participants used grapefruit or St. John’s wort, which may cause interactions. So, it is not surprising, that patients, who used herbal remedies or fungal substances did not thought, that agents from these complementary products may interfere with other drugs. On the other hand, majority of the patients hear about or ask about the complementary products from physician and other health care specialists. This means, that most of the negative effects of complementary medicine may be avoidable with a good physician-pharmacist-patient relationship.
Keywords:Oncology, Dietary supplements, Complementary medicine
Introduction
In recent decades, the use of complementary and alternative medicine has become widespread during chemotherapy as well as at targeted therapies [1-4]. In many cases, the utilized therapies are among the spiritual and similar procedures, which are difficult to define pharmaceutically, but at the same time rarely involved in interactions and side effects. On the other hand, numerous foods and dietary supplements are also known and used for medical purposes. It should be also emphasized, that dietary supplements cannot be used as anticancer therapies. According to Lugasi et al. (2010), even in the case of healthy individuals, they can only be recommended in the prevention of certain conditions, for example in the winterassociated vitamin-deficient diet, or in the case of supplementing special diets [5]. As they are in the category of “foods”, they can be used for therapeutic purposes by dietitian, which can be aided by the health claims, in accordance with European regulations [6]. All in all, their efficacy and safety do not have to be proven, so they are not suitable for the treatment of tumors. Based on these facts, in many cases, the question is not whether the patient is using a complementary or alternative method, but whether it is compatible with the applied antitumor therapy. Furthermore, the most important question is whether the patient communicates the used complementary or alternative therapy with the physician. Therefore, in our work, we wanted to assess the consumption of the supplementary foods and foods for special medical purposes at patients, who appeared in the Oncology Center of Semmelweis University. We paid special attention to some agents, that had already well described interactions. Furthermore, we asked about the consumption of functional foods and some other foods, that have well-known beneficial effect [7].
Materials and Methods
Study design
We conducted a non-interventional study with questionnaires at the Oncology Center of Semmelweis University (Tömő utca 25- 29, 4th floor, Budapest, H-1083, Hungary).
Following the demographic data, we defined the concepts of dietary supplement and functional food for patients, and then examined their use and knowledge about them. We also asked about consumption habits related to foods that have not been examined as functional food but have well-known beneficial effects. In our study, we were unable to distinguish between certain pharmaceutical products, certain medical formulations that meet special needs and food supplements due to their confusability by patients. The aforementioned pharmaceutical-quality products (such as vitamin-containing, over-the-counter products) have been taken as dietary supplements by patients without medical advice, so they were displayed as dietary supplements in this paper [8,9].
The questionnaire was completed in the form of a guided interview, anonymously, with the help of specialists working at the institute, trained medical and pharmacist students.
The study was carried out in accordance with the Declaration of Helsinki and approved by the Health Science Council, Scientific and Research Ethics Committee [ETT-TUKEB (Egészségügyi Tudományos Tanács, Tudományos és Kutatásetikai Bizottság) approval number: 31/2016].
Statistical analysis
Microsoft Excel 2013 (Microsoft Corp., Redmond, USA) and R (R Foundation for Statistical Computing; Austria) were used for statistical analysis.
Results
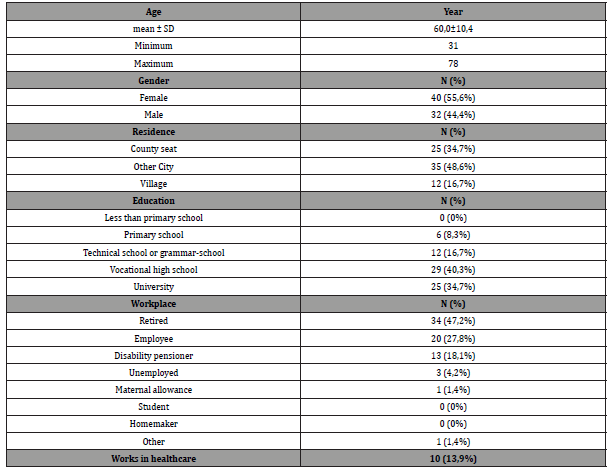
Patient characteristics are summarized in Table 1. It should be highlighted, that there was a higher proportion of women among the participants. The mean age was in accordance with the general concept, of older people are affected with cancer. Nearly a third of the respondents lived in the county seat, but a large proportion of the residents of other cities also took part in the survey. In terms of education, vocational high school (40.3%) and university education (34.7%) were typical. According to age, the proportion of retirees was outstanding (47.2%), but a significant number of active earners also completed the questionnaire (27.8%).
Table 1: Demography
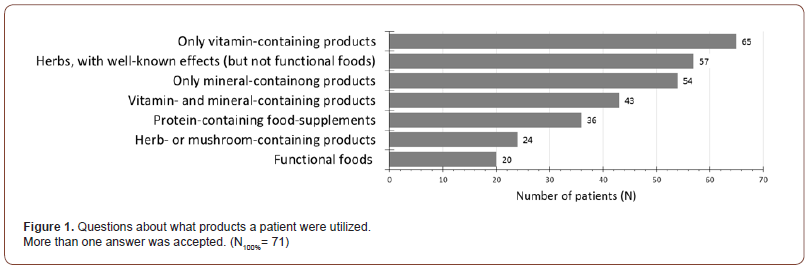
Of the respondents, 71 out of 72 respondents answered questions about food supplements (medicines used as food supplements and foods for special medical purposes), functional foods and non-functional foods, with well-known good effects. Patients had multiple choices. Figure 1 shows that the highest proportion of patients consumed vitamin-only formulation (91.6%). Although functional food consumption was moderate (28.2%), daily or weekly consumption of those foods and herbs that had not been tested as functional food, but had a well-known beneficial effect were utilized in 80.2% of patients. In this group, the beetroot or beetroot juice (20 people), garlic (11 people), rosehips (9 people), pomegranate (5 people), ginger (5 people) and nettle (3 people) were mentioned by at least three people. There was also an example of grapefruit consumption, and one patient mentioned here the apricot kernel capsules, along with freshly squeezed wheatgrass, celery extract and a special herb-containing tea (made of cat’s claw, atractilodes, stinging nettle, peppermint, burdock, St. John’s wort, milk thistle).
Figure 1 also shows that more than 90% of the patients (66 people) indicated at least 2 categories. The most common response combination (12 subjects; 16%) included 4 categories: vitaminonly, mineral-only, vitamin- and mineral-containing dietary supplements, and protein-containing supplements.
We asked about whose advice the patients consumed these various dietary supplements, functional foods, other herbs, plants. The source was typically a doctor, a pharmacist, a dietitian, or other healthcare specialist (26 people; 36.6%). On the other hand, in 35.2% of cases (25 people) the recommendation was not solely made by a healthcare specialist. Moreover, 16 people (22.5%) usually followed the advice of a non-specialist; and 4 further people (5.6%) consumed the above-mentioned food supplements and foods because their acquaintances advised it.
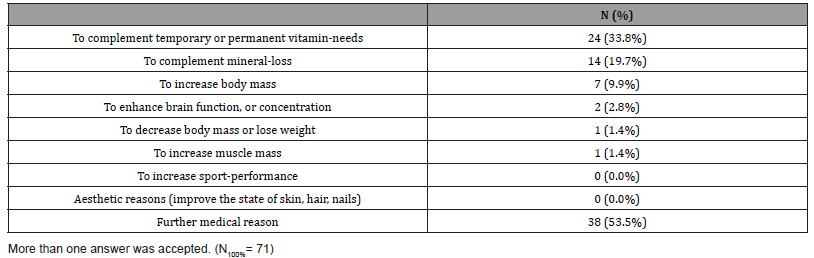
The purposes of these therapies were also examined. It can be seen from Table 2, that mainly people wanted to complement the need of minerals (14 people, 19.7%) or vitamins (24 people, 33.8%), but the main answer was “further medical causes” (38 people, 53,5%). From these latter group, people principally used them (13 persons), because a healthcare Provider advised it. In these cases, the real reason was not revealed. In those, who answered “further medical cases”, 6 people used these products to enhance their immune system and 2 more participants used them against common cold.
Table 2: Causes of the utilization of food supplement, special foods for special medical purposes and same products.
In our article, the patients’ knowledge about the utilized preparations and products were examined according to the two major topics, which can be seen in Figure 1.
Dietary supplements containing vitamins and minerals
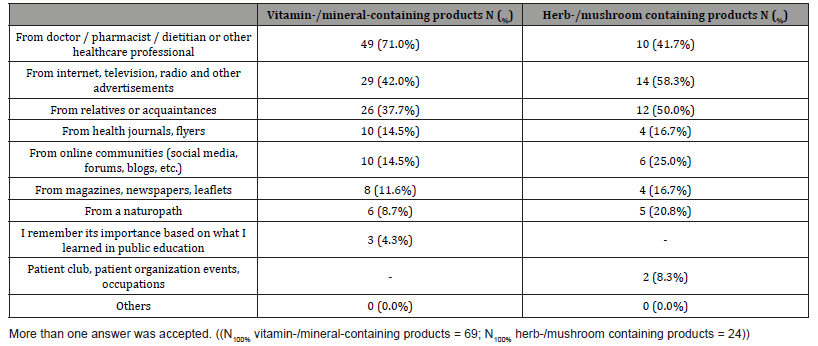
Sixty-nine patients answered our questions about vitamin and mineral containing products. It has been asked that where they had heard about the dietary supplement and other products containing the vitamin and / or mineral they were taking. Surprisingly, very few patients mentioned that they had heard in public education about the importance of these vitamins and minerals (Table 3). At the same time, remarkably high proportion of patients were informed by their doctor, pharmacist and dietitian. The second most common source of information was the Internet, while the third was “family members and acquaintances”.
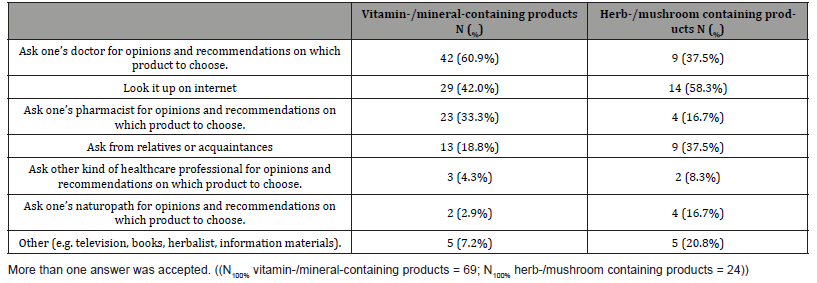
Table 3: Sources of information, from where patients heard about the utilized products.
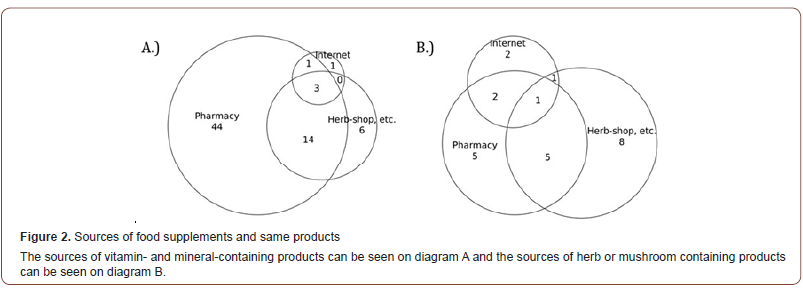
For further information about the given bioactive substances and preparations, people would have inquired their doctors primarily (60.0%) or would looked it up on the internet (41.4%). Although it is difficult to draw clear conclusions with the relatively small number of samples, it is noteworthy that the internet was mentioned more often as a source of information compared to the pharmacist’s opinion (32.9%) (Table 4). The latter observation is also striking because such products are still purchased primarily by patients from pharmacies (Figure 2) [10].
Table 4: Sources of information, from where patients ask about purchasing and taking of a food supplement.
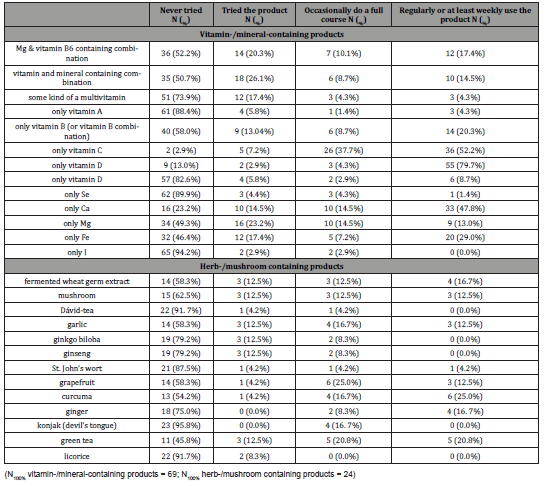
Among the vitamin and mineral-containing preparations regularly used at the Oncology Center, the most typical are products containing only vitamin C or vitamin D, and products containing Ca (often recommended in addition to vitamin D) (Table 5). However, it should not be overlooked that many patients have tried countless additional products for a shorter or longer period.
Table 5: Dietary-supplement consumption habits at the Oncology Center.
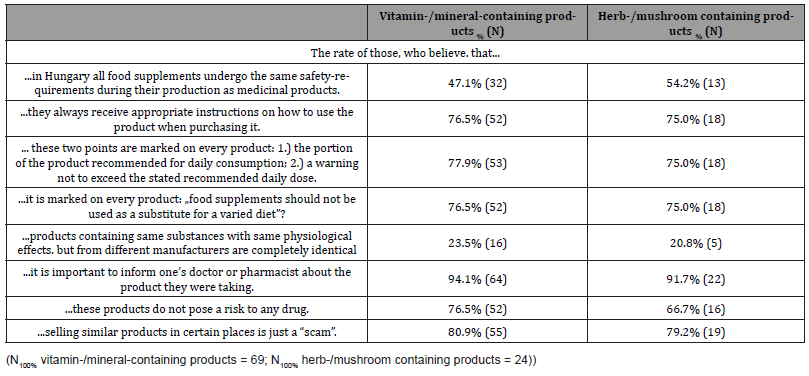
Therefore, it is remarkable, as almost half of the respondents thought that vitamin- and/or mineral-containing food supplements undergo the same safety-requirements during their production as medicinal products (Tables 5&6). Moreover, a noteworthy proportion of patients (33.5%) thought that vitamin/mineralcontaining products did not pose a risk to any drug. Table 6 shows that the majority of patients considered, it is important to inform their doctor about the vitamin/mineral-containing product they were taking. In contrast, less than two-thirds and about one-third of patients would ask about the products from their physicians or from their pharmacists, respectively (Table 4). In evaluating the data reported in Table 6, we had to exclude one patient because he answered “I don’t know” to each question in this block.
Herbal or mushroom based food supplements
Only 24 patients answered our questions about herbal or fungal preparations. Although the number of patients is lower than in the previous group, remarkable differences in trends can be seen between the two groups, especially in terms of information sources. Patients heard about the utilized products primarily from the internet, television and radio advertisements, secondly from family members and acquaintances, while doctors, pharmacists and dietitians could be considered only the third most common source of information (Table 3). In parallel, Table 4 also highlights, that further information about the used products were obtained rather from the internet (58,3%), than from their doctors (37,5%) or pharmacists (16,7%). Moreover, same proportion of people (37%) would ask about these products from their relatives and acquaintances. Another difference is that a quarter of patients buy herbal or mushroom-based products
Surprisingly few people mentioned pharmacists as the source of further information about these supplements, despite the fact that in this group, the majority of respondents (54,2%), obtained the products from a pharmacy (Figure 2). It should also be highlighted that the general knowledge and opinion of patients about these preparations is similar to those containing vitamins and minerals. Approximately half of the patients believed that all of them were subjected to the same safety-requirements during their manufacture as medicinal products, and one third (33.3%) did not think they could pose a risk when taken with certain medicines (Table 6).
Table 6: Patients’ opinions on vitamin/mineral containing supplements as well as on mushroom/plant-based dietary supplements.
Discussion
In our work, we wanted to examine the dietary supplement consumption habits of patients who appeared at the Oncology Center of Semmelweis University. The main limiting factor was that we examined only one institute in Budapest, however, demographic data show that it is the health-provider of further towns and villages. In addition, the number of patients was relatively low, thus only a descriptive statistical analysis seemed relevant.
During the guided interviews, it had to be considered, that for the general population it was hard to define the differences between dietary supplements, over-the-counter drugs (especially vitamincontaining over-the-counter drugs), and foods for special medical purposes. Therefore, we only asked about dietary supplements, foods for special medical purposes, functional foods, and so-called “foods that have not been tested as functional foods but are known to have beneficial effects”.
Seventy-two patients were asked, whereof 69 consumed vitamin- and/or mineral-containing products. Furthermore, patients have often consumed foods, that have not been examined as functional food but have well-known beneficial effects. In this group, those foods were listed, that patents regularly used, and therefore could influence the side-effect profile of therapies and health-status. It should be also mentioned, that by using this category, we revealed unseen sources of interactions, too. Pomegranate for example can modulate cytochrome P activity and thus cause interactions [11]. Garlic should also be highlighted, as it can increase bleeding, hence can be problematic at surgeries and in combination with anticoagulants [12,13]. It should be noted that such dangerous products were also mentioned, like grapefruit or apricot kernels. While grapefruit is one of the most known interacting herbs the latter is considered to be highly toxic [14,15]. Thus, the therapeutic consumption of the fruits and vegetables mentioned here is also not harmless, but at the same time they can easily slip out of medical control, as the patient believes, it is only a food and does not mention them to the medic. In addition to the few examples listed here, there are countless foods or spices that can be dangerous, so we consider it important to create and develop accessible summaries, monographs and the training about these foods, products [16,17].
On Figure 1 it is also visible, that all of the above-mentioned types of products were consumed at least about quarter of the patients. All in all, only one patient did not use any of these supplements or same kind of foods. It should be also noticed that mainly older adults participated in our study, hence the high rate of comorbidities could not be excluded. It seems worrisome, because one third of the patients used these agents not exclusively based on an expert’s opinion; moreover, more than quarter of the patients consumed these foods especially not because of a healthcare professional’s recommendation. In other words, a noticeable amount of people used these supplements and other foods with no professional control, therefore experts cannot help in cases of side effects, overdose or interactions, while polypharmacy is also frequent. In the context of negligence, well-known barriers should be mentioned i) the lack of interest (like non inquiry or disinterest) of the doctor or ii) the lack of appropriate information from them should be mentioned. Furthermore, some patients believe, these supplements or functional foods, etc. are not mentionable, as well as some patients fear from the disapproval of the doctor. The limited time for a patient is also a noticeable barrier [18,19]. Accordingly, the oncologist has to achieve the faith of the patient and the disclosure of complementary and alternative medicines, furthermore the involvement of a pharmacist seems necessary, with regard to the differences in the curriculum.
It should be noticed that patients are informed about the role and relevance of vitamins and minerals from physicians, pharmacists, dietetics and other healthcare specialists. Likewise, the medical doctors’ advice was the main source of information in further questions. On the other hand, there is a contradiction between Table 3 and Table 6, as notably higher rate of people thought, it was important to notify their physician or pharmacist about the utilized complementary medicine than the rate of those patients, who truly asked their healthcare provider about the applied supplements, functional foods, etc. The explanation to this discrepancy maybe people thought the first case is only about a short disclosure, while the second case is about a longer conversation. On the other hand, it was a remarkably low rate of people, who were educated about the importance of these components from the public education. All in all, physicians have a remarkable role in the education of the patients, hence oncologists have critical part in the life of cancerpatients.
In the case of vitamin- and mineral-containing products, patients used mostly the internet but not alone. As for the mushroom- and herb-containing products the internet was the main source of information. It should be highlighted, that information on the internet (especially in the social media) can become markedly pessimistic, without counterpoint [20]. One of the most well-known examples is the spreading of anti-vaccination campaigns [21]. Internet is also a main source of obtaining these supplements. The illegal, uncontrolled websites without professional supervisions are serious threat to the patients, as Fittler et al. (2018) highlighted [22].
From Table 5 it is also visible, that vast majority of patients are not familiar with the regulation and advices of medicines, supplements and foods. A critical point is that many participants believed that food-supplements are produced in a same controlled environment like pharmaceutical products. On the other hand, food-supplements are in the class of foods, hence a lower quality assurance is enough to produce them.
Furthermore, more than quarter of the patients believed, the utilized food supplements cannot be harmful with medicines. It can be a serious problem, as patients may consume foods or supplements, that cause interactions. For example, in our study a patient used grapefruit and garlic. Not to mention, grapefruit and garlic based food-supplements are widely available in stores. Furthermore, the most utilized agent, the vitamin C also has side effects. On the other hand, food-supplement producing firms are not urged to inform patients about the side effect profile of this agent. Also, vitamin C may cause interaction with chemotherapeutic agents [23].
On the other hand, food-supplements and functional foods, etc. products are purchased mainly from pharmacies. It is a noteworthy opportunity for pharmacists, to revise possible and serious interactions, or notice side effects. Pharmacists knowledge is better than (for example) health food store employees about complementary and alternative therapies, it seems to be a safer opportunity for these patients [24]. For that, community pharmacies can be a useful tool in the management of over the counter drug, food-supplement and other food consumption. Furthermore, internationally available monographies and guidelines are necessary to maintain an up-to-date knowledge about these products [16,17].
In summary, complementary and alternative therapies are widely available, and used by cancer-patients. Hence, the main question in this situation is not whether they use these therapies, but whether they have a good guidance. In this case not only a good patient-medic relationship is necessary, but a good patient-medicpharmacist- other healthcare professional relationship.
Conclusion
In the Semmelweis University Oncology Center, most of the patients consumed some kind of food-supplements, certain medical formulations that meet special needs and other foods or over the counter drugs as complementary or alternative therapies. These agents (because of their long-term consumption) may alter the health-status of patients or the therapeutic effect or toxicities of medications. On the other hand, physicians, pharmacists and other healthcare professionals are essential as a primary source of information about these products. These consultations can provide an opportunity for a safer complementary and alternative therapy. While our study may have limitations, the findings should not be overlooked, hence the good communication between patients, physicians, pharmacists and other healthcare providers should be the base of the future cancer therapies.
Funding
We would like to thank for the „Together for the Local Communities” application, provided by Hungaropharma Zrt.
Acknowledgement
We would like to thank Hungaropharma Zrt. for its support in the “Together for Local Communities” application. Furthermore, to dr. Dorina Ali, to dr. Szonja Bóta and to dr. Diána Simon for the help provided at the questionnaires.
Conflict of Interest
The authors declare that they have no conflict of interest.
References
- Richardson MA, Sanders T, Palmer JL, Greisinger A, Singletary SE (2000) Complementary/alternative medicine use in a comprehensive cancer center and the implications for oncology. J Clin Oncol 18(13): 2505-2514.
- Luo Q, Asher GN (2017) Complementary and alternative medicine use at a comprehensive cancer center. Integr Cancer Ther 16(1): 104-109.
- Zörgő S, Olivas Hernández OL (2018) Patient journeys of nonintegration in Hungary: A qualitative study of possible reasons for considering medical modalities as mutually exclusive. Integr Cancer Ther 17(4): 1270-1284.
- Buckner CA, Lafrenie RM, Dénommée JA, Caswell JM, Want DA (2018) Complementary and alternative medicine use in patients before and after a cancer diagnosis. Curr Oncol 25(4): e275-e281.
- Lugasi A, Horacsek M, Martos É (2010) Food supplements on the domestic market in Hungary. Nutritional assessment of the ingredients, risks and benefits, the role of food supplements in human nutrition. Orv Hetil 151(48): 1964-1975.
- Dietary supplements (2021).
- Budai KA, Hankó B, Antal I, Zelkó R (2015) Introduction of functional foods-types, manufacturing methods and quality assurance. Acta Pharm Hung 85(3): 97-110.
- Fittler A, Bősze G, Botz Lajos (2010) Attitude of patients and customers regarding online drug purchase – a Hungarian community pharmacy survey. Orv Hetil 151(48): 1983-1990.
- Végh A, Lankó E, Fittler A, Vida RG, Miseta I, et al. (2014) Identification and evaluation of drug-supplement interactions in Hungarian hospital patients. Int J Clin Pharm 36(2): 451-459.
- Larsson J (2019) eulerr: Area-Proportional Euler and Venn Diagrams with Ellipses.
- Faria A, Monteiro R, Azevedo I, Calhau C (2007) Pomegranate juice effects on cytochrome P450S expression: in vivo J Med Food 10(4): 643-649.
- Woodbury A, Sniecinski R (2016) Garlic-induced surgical bleeding: How much is too much? A A Case Rep 7(12): 266-269.
- Fan Y, Adam TJ, McEwan R, Pakhomov SV, Melton GB, et al. (2017) Detecting signals of interactions between warfarin and dietary supplements in electronic health records. Stud Health Technol Inform 245: 370-374.
- Holmberg MT, Tornio A, Hyvärinen H, Neuvonen M, Neuvonen PJ, et al. (2015) Effect of grapefruit juice on the bioactivation of prasugrel. Br J Clin Pharmacol 80(1): 139-145.
- Ginter E, Simko V (2013) False claims about so called vitamin B 17. Bratisl Lek Listy 114(4): 241.
- (2021) CAM Cancer.
- (2021) About Herbs, Botanicals & Other Products.
- Davis EL, Oh B, Butow PN, Mullan BA, Clarke S (2012) Cancer patient disclosure and patient-doctor communication of complementary and alternative medicine use: a systematic review. Oncologist 17(11): 1475-1481.
- Shelley BM, Sussman AL, Williams RL, Segal AR, Crabtree BF, et al. (2009) 'They don't ask me so I don't tell them': patient-clinician communication about traditional, complementary, and alternative medicine. Ann Fam Med 7(2): 139-147.
- Freedman RA, Viswanath K, Vaz-Luis I, Keating NL (2016) Learning from social media: utilizing advanced data extraction techniques to understand barriers to breast cancer treatment. Breast Cancer Res Treat 158(2): 395-405.
- Hussain A, Ali S, Ahmed M, Hussain S (2018) The Anti-vaccination movement: A regression in modern medicine. Cureus 10(7): e2919.
- Fittler A, Vida RGy, Káplár M, Botz L (2018) Consumers turning to the internet pharmacy market: Cross-sectional study on the frequency and attitudes of Hungarian patients purchasing medications online. J Med Internet Res 20(8): e11115.
- Heaney ML, Gardner JR, Karasavvas N, Golde DW, Scheinberg DA, et al. (2008) Vitamin C antagonizes the cytotoxic effects of antineoplastic drugs. Cancer Res 68(19): 8031-8038.
- Coon SA, Stevens VW, Brown JE, Wolff SE, Wrobel MJ (2003) Comparison of dietary supplement product knowledge and confidence between pharmacists and health food store employees. J Am Pharm Assoc 55(2): 161-168.
-
Balázs Hankó, István Horváth, Dénes Kleiner, Magdolna Dank, Hegyi Gabriella, Mária Matuz. Dietary Supplements and Supplemented Diets. On J Complement & Alt Med. 6(5): 2021. OJCAM.MS.ID.000648.
-
Dietary Supplements, Supplemented Diets, Oncology, Negative effects, Complementary medicine, Numerous foods, Antitumor therapy, Supplementary foods, Functional foods, Beneficial effects
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






