 Case Report
Case Report
Rapidly Progressive Bilateral Metabolic Cataract in an Adolescent with Type 1 Diabetes Mellitus: A Case Report
Diana Simões1*, Sara Rolim2, Natacha Moreno3, Rita Gentil3, Goreti Lobarinhas2
1 1Department of Pediatrics, Local Health Unit of São João, Portugal
2 2Department of Pediatrics, Local Health Unit of Barcelos and Esposende, Portugal
3Department of Ophthalmology, Local Health Unit of Barcelos and Esposende, Portugal
Diana Simões, Department of Pediatrics, Local Health Unit of São João, Alameda Prof. Hernâni Monteiro, Porto, Portugal.
Received Date:November 12, 2025; Published Date:November 18, 2025
Abstract
Metabolic cataract is an uncommon but clinically significant ocular complication of type 1 diabetes mellitus (T1DM), particularly in pediatric
patients with sustained hyperglycemia or delayed disease recognition.
We describe the case of a 14-year-old female with newly diagnosed T1DM who initially presented without ocular abnormalities. Despite followup,
glycemic control remained inconsistent, with significant time above the recommended glucose range. Within ten months of diagnosis, she
developed unilateral visual impairment, which progressed to near-complete bilateral visual loss in two weeks. Ophthalmologic evaluation confirmed
bilateral metabolic cataract, without evidence of retinopathy or other microvascular complications. absence of diabetic retinopathy. She underwent
bilateral phacoemulsification with intraocular lens implantation, resulting in full restoration of visual function.
This case underscores the need for heightened clinical awareness of early cataract formation in adolescents with suboptimal glycemic control
and highlights the importance of prompt ophthalmologic evaluation in the presence of visual symptoms, even during the initial years following
T1DM diagnosis. Early recognition and timely surgical intervention are essential to prevent long-term visual morbidity.
Keywords: Type 1 diabetes mellitus, Metabolic cataract, Pediatric age
Introduction
Although advances in diabetes management have markedly improved prognosis and quality of life, inadequate glycemic control continues to pose a substantial risk for both acute metabolic disturbances and chronic microvascular complications. Among these, ocular involvement is particularly concerning, as it may lead to significant and potentially irreversible visual impairment if not recognized and managed promptly [1,2].
While diabetic retinopathy is the most commonly highlighted ocular complication of type 1 diabetes mellitus (T1DM), cataract formation represents an important yet often underrecognized manifestation. Metabolic cataracts in pediatric age are uncommon; however, they can be among the earliest clinical signs of undiagnosed diabetes or may develop within the first months following diagnosis, especially in cases of delayed recognition or persistently poor glycemic control [2-4].
Case Presentation
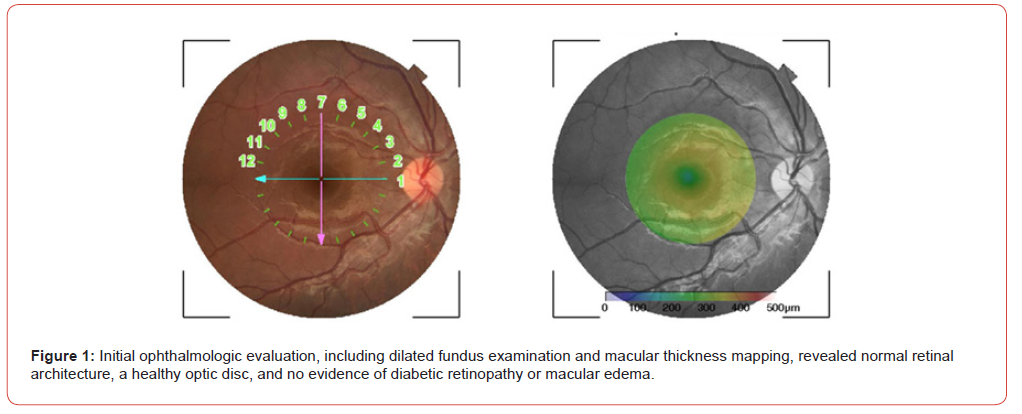
A 14-year-old female presented to the emergency department with an history of polyuria, polydipsia, polyphagia, and unintentional weight loss. Initial laboratory evaluation confirmed new-onset T1DM without ketoacidosis. Hemoglobin A1c (HbA1c) was >14%, and autoimmune screening revealed positive anti-GAD65 antibodies (141.7 UI/ml) and anti-islet cell antibodies (14.71 UI/ml). Screening for associated autoimmune comorbidities, including celiac disease, pernicious anemia, and autoimmune thyroid disease, was negative. Baseline evaluation for diabetes-related complications, including retinopathy or metabolic cataract (figure 1), nephropathy, neuropathy, dyslipidemia, and hypertension, showed no abnormalities.
She remained under outpatient follow-up in pediatric endocrinology but adherence to insulin therapy and glycemic monitoring was inconsistent. During follow-up, her HbA1c was 7.8%, with 39% of glycemic readings above the target range and 3% below.
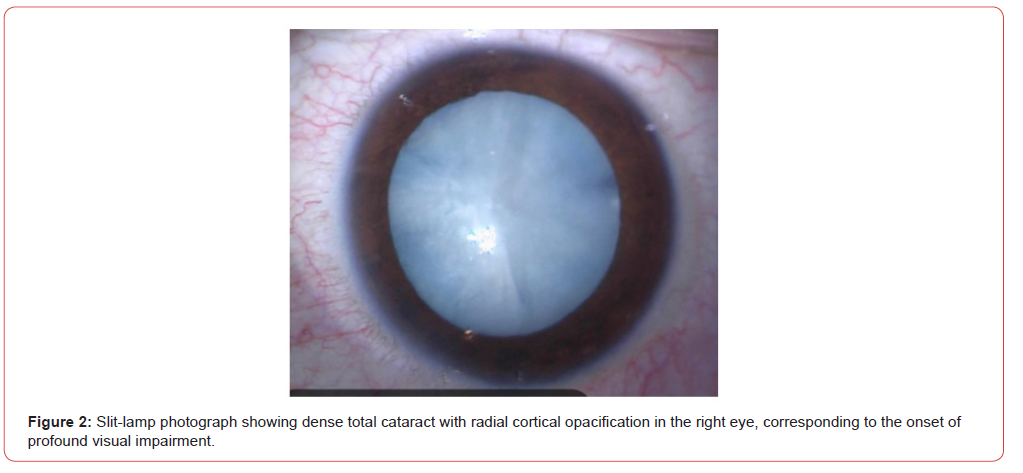
Ten months after diagnosis of T1DM, the patient returned to the emergency department reporting rapidly progressive unilateral visual impairment in the right eye over the preceding week, without history of ocular trauma. Ophthalmologic examination revealed lens opacity in the right eye, consistent with metabolic cataract, with no evidence of microvascular retinopathy or other ocular abnormalities (figure 2). She was scheduled for outpatient ophthalmology consultation and surgical planning. However, within 15 days, the cataract progressed rapidly, involving the contralateral eye and resulting in near-complete bilateral visual loss.
The patient underwent bilateral phacoemulsification with intraocular lens implantation. The postoperative course was favorable, with resolution of visual symptoms and restoration of functional vision.
Discussion
Metabolic cataract is a rare but clinically relevant complication of T1DM, particularly in pediatric and adolescent populations. In contrast to diabetic retinopathy, which typically develops only after prolonged periods of chronic hyperglycemia, metabolic cataracts may occur early in the disease course and can even constitute the first clinical indicator of undiagnosed T1DM [2-4].
The pathophysiology of metabolic cataract is primarily linked to activation of the polyol pathway. In chronic hyperglycemia, excess glucose is converted to sorbitol by aldose reductase, and because sorbitol diffuses poorly across cell membranes, it accumulates within the lens. This leads to increased osmotic pressure, water influx, lens fiber swelling, and loss of transparency. Oxidative stress and non-enzymatic glycation of lens proteins may further destabilize lens architecture [5-7].
Clinically, metabolic cataract may present with rapidly progressive visual impairment, blurred vision, and, in severe cases, marked loss of visual function [4,8]. The risk is higher in patients with prolonged hyperglycemia, markedly elevated HbA1c levels, and a long symptomatic period preceding the diagnosis of diabetes [3,8].
Adolescents with T1DM may be particularly vulnerable to metabolic cataract due to lifestyle-related challenges influencing treatment adherence, including psychosocial stressors, transition of responsibility for self-care, and difficulties maintaining consistent glucose monitoring and insulin administration [9,10]. In the present case, glycemic patterns reflected substantial time above target range despite a seemingly acceptable HbA1c, suggesting significant glycemic variability. Such fluctuations are increasingly recognized as independent contributors to diabetes-related complications, even in the absence of extreme hyperglycemia [11,12].
Although guidelines vary slightly among organizations, early ophthalmologic surveillance is essential. American Diabetes Association recommend initiating routine screening 3–5 years after the diagnosis of T1DM, provided the child is at least 11 years of age or has entered puberty (whichever occurs first), with follow-up every 2-year thereafter [13]. However, ophthalmologic assessment should be performed earlier in the presence of visual symptoms, poor glycemic control, or clinical suspicion of ocular complications [3,2,13].
Prompt recognition is critical, as early intervention can prevent long-term visual impairment [14]. Surgical management with phacoemulsification and intraocular lens implantation generally offers favorable outcomes, as observed in this patient, who experienced complete recovery of visual function following bilateral surgery [9,15].
Conclusion
This case reinforces the importance of maintaining optimal glycemic control from the earliest stages of disease and highlights the need for multidisciplinary care involving pediatric endocrinology, ophthalmology, and psychosocial support services. Improving adherence strategies—through continuous glucose monitoring systems, structured diabetes education, family support, and psychological intervention when appropriate—may help reduce the risk of early metabolic complications such as cataract.
Conflict of Interest
The authors declare that there were no conflicts of interest in carrying out this work.
References
- Lu Wen-Li, Shen Po-Chih, Lee Chen-Hao, Su Yu-Tsun, Chen Li-Min (2020) High Risk of Early Cataracts in Young Type 1 Diabetes Group: A Nationwide Cohort Study, International Journal of Endocrinology 2020: 8160256.
- Šimunović M, Paradžik M, Škrabić R, Unić I, Bućan K, et al. (2018) Cataract as Early Ocular Complication in Children and Adolescents with Type 1 Diabetes Mellitus. Int J Endocrinol 2018: 6763586.
- Reiter UM, Eckert AJ, Dunstheimer D, Bechtold-Dalla Pozza S, Lüllwitz C, et al. (2022) Cataract in children and adolescents with type 1 diabetes. Insights from the German/Austrian DPV registry. Pediatr Diabetes 23(3): 362-369.
- Cook E, Stratton E, Thornton MD (2020) Acute Cataract Development in a Pediatric Patient With Type 1 Diabetes. J Emerg Med 58(4): e207-e209.
- Ghahramani M, Shahsavani MB, Simon S, Saboury AA, Yousefi R (2025) Recent insights into the pathomechanisms of cataract development in diabetic patients. Exp Eye Res 261: 110630.
- Thorne CA, Grey AC, Lim JC, Donaldson PJ (2024) The Synergistic Effects of Polyol Pathway-Induced Oxidative and Osmotic Stress in the Aetiology of Diabetic Cataracts. Int J Mol Sci 25(16): 9042.
- Mrugacz M, Pony-Uram M, Bryl A, Zorena K (2023) Current Approach to the Pathogenesis of Diabetic Cataracts. Int J Mol Sci 24(7): 6317.
- Iafusco D, Prisco F, Romano MR, Dell'omo R, Libondi T, et al. (2011) Acute juvenile cataract in newly diagnosed type 1 diabetic patients: a description of six cases. Pediatr Diabetes 12(7): 642-648.
- Chiang JL, Maahs DM, Garvey KC, Hood KK, Laffel LM, et al. (2018) Type 1 Diabetes in Children and Adolescents: A Position Statement by the American Diabetes Association. Diabetes Care 41(9): 2026-2044.
- Azar S, Maroun Abou Jaoude N, Kędzia A, Niechciał E (2024) Barriers to Type 1 Diabetes Adherence in Adolescents. J Clin Med 13(19): 5669.
- Valente T, Arbex AK (2021) Glycemic Variability, Oxidative Stress, and Impact on Complications Related to Type 2 Diabetes Mellitus. Curr Diabetes Rev 17(7): e071620183816.
- Ceriello A, Monnier L, Owens D (2019) Glycaemic variability in diabetes: clinical and therapeutic implications. Lancet Diabetes Endocrinol 7(3): 221-230.
- American Diabetes Association Professional Practice Committee (2024) 14. Children and Adolescents: Standards of Care in Diabetes-2024. Diabetes Care 47(Suppl 1): S258-S281.
- Medsinge A, Nischal KK (2015) Pediatric cataract: challenges and future directions. Clin Ophthalmol 9: 77-90.
- Repka MX, Dean TW, Kraker RT, Zhuokai Li, Kimberly G Yen, et al. (2022) Visual Acuity and Ophthalmic Outcomes 5 Years After Cataract Surgery Among Children Younger Than 13 Years. JAMA Ophthalmol 140(3): 269-276.
-
Diana Simões*, Sara Rolim, Natacha Moreno, Rita Gentil, Goreti Lobarinhas. Rapidly Progressive Bilateral Metabolic Cataract in an Adolescent with Type 1 Diabetes Mellitus: A Case Report. Glob J of Ped & Neonatol Car. 5(5): 2025. GJPNC. MS.ID.000624..
Type 1 diabetes mellitus, Metabolic cataract, Pediatric age, Polyuria, Pediatric Endocrinology, Disease, Child
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






