 Research article
Research article
Frequency of Rh Incompatibility among Neonates Presenting with Jaundice at Children Hospital, Multan, Pakistan
Maria Hassan1*, Syed M Dur E Sabih Haider2, Tuba Qaisar3M, Jam Ali Haider4, Rushan Hassan5, Bushra Urooj6
1 Fellow Paediatric Hematology and Oncology, The Children Hospital and Institute of Child Health Multan
2 Medical Officer Paediatric Medicine, The Children Hospital and Institute of Child Health Multan
3 Woman Medical Officer Paediatric Nephrology, The Children Hospital and Institute of Child Health Multan
4 Medical Officer Paediatric Medicine, The Children Hospital and Institute of Child Health Multan
5 Consultant Paediatrician, Paediatric Medicine, DHQ Hosital Chakwal
6 Postgraduate Resident Emergency Medicine, Mayo Hospital Lahore
Maria Hassan, Fellow Paediatric Hematology and Oncology, The Children Hospital and Institute of Child Health Multan.
Received Date: April 21, 2025; Published Date:May 02, 2025
Abstract
Objective: To determine the frequency of Rh incompatibility among neonates presenting with jaundice.
Methods: This cross-sectional study was conducted at the department of pediatrics, Children Hospital, Multan Pakistan during January 2024
to June 2024. A total of 169 full-term neonates with birth weight ≥ 2500 grams, and presenting with jaundice (serum bilirubin levels > 12mg/dl),12
within 2 days of life were analyzed. Demographic neonatal and maternal characteristics were noted, and relevant laboratory investigations were
done. Rh incompatibility was defined as Rh –ve mother, Rh +ve baby and detectible antibodies in baby’s blood by direct coombs test. Chi-square test
(for qualitative data), and Mann-Whiteny U test (for numeric data) were employed taking p<0.05 as significant.
Results: Among the total of 169 neonates, 89 (52.7%) were male, and the median (IQR) gestational age was 38 (37-40) weeks. There were 87
(51.5%) neonates who were admitted within 24-hours of life. Rh incompatibility was identified in 16 (9.5%) cases. A relatively higher proportion of
neonates with Rh incompatibility were admitted on day 2 of life compared to those without Rh incompatibility (68.8% vs 46.4%), but the difference
did not reach statistical significance (p=0.089). Among maternal characteristics, 19 of 169 (11.2%) mothers were Rh-negative, all of whom had
neonates with Rh incompatibility (100% vs 2.0%, p<0.001). Neonates with Rh incompatibility had significantly higher median (IQR) total serum
bilirubin levels (21.30 [15.45-23.02] mg/dL vs 14.20 [13.00-19.35] mg/dL, p<0.001), and reticulocyte count (4.50 [3.90-5.35] % vs 3.60 [3.00-4.70]
%; p=0.010).
Conclusion: This study found that 9.5% of neonates presenting with jaundice had Rh incompatibility. Rh-incompatible neonates had significantly
higher bilirubin levels compared to their counterparts, reinforcing the need for early screening and intervention.
Keywords: Gestational age, Jaundice, Reticulocyte count, Rh incompatibility, Serum bilirubin.
Introduction
For centuries, neonatal jaundice (icterus neonatorum) has been observed in newborns. As early as 1724, Juncker, in the Conspectus Medicinae Theoreticopraticae, began distinguishing between true jaundice and the icteric tinge which may be observed in infants, immediately after birth. In 1875, Orth noticed during autopsies the presence of bilirubin in the basal ganglia of infants who had severe jaundice, which was labeled kernicterus by Schmorl in 1903 [1]. In 1958, however, a nurse in the nursery of the General Hospital in Rothford, Essex, Great Britain, reported an apparent fading away of the yellow pigmentation in the skin of the jaundiced babies when they had been a short time in sunlight [2].
Neonatal jaundice is defined as yellowish discoloration of skin, sclera of eye balls and mucous membranes caused by deposition of bile salts in tissues [3]. Depending upon the cause, the jaundice may present at birth or anytime during neonatal period. Jaundice due to either direct (conjugated) or indirect (unconjugated) bilirubin in the first 24 hours of life should be taken seriously [4]. Globally, around 60-80% term or late-term healthy newborns are estimated to develop some degree of jaundice [5]. Early identification and proper management is needed to prevent the serious neurological complications associated with it. The most common cause of neonatal jaundice during first 24 hours of life is rhesus hemolytic disease [6].
Worldwide, the prevalence of Rh incompatibility is estimated to affect around 276 per 100,000 live-births [7]. According to a study, the frequency of Rh-D negative phenotype was 4.1% in Guinea, and 2.4% in Cameroon [8,9]. The injection of anti D gamma globulin (RhoGAM) to the mother immediately after the delivery of each Rh positive infant has been a successful strategy to reduce hemolytic disease [10].
Not much local data is available regarding the magnitude Rh incompatibility in neonatal jaundice but it is suspected that the burden could be high which (if left untreated) may result in life threatening complications like kernicterus (a brain destroying condition). The Rh incompatibility can also be prevented in subsequent pregnancies by giving Anti-D to the mothers within 72 hours after delivery. The purpose of this study is to determine the frequency of Rh incompatibility among neonates presenting with jaundice.
Methodology
This cross-sectional study was conducted at the department of pediatrics, Children Hospital, Multan Pakistan during January 2024 to June 2024. Sample size of169 was calculated using online Open EPI sample size calculator taking the proportion of Rh incompatibility in neonatal jaundice as 12.5% [11], with 95% confidence level and 5% margin of error. Non-probability consecutive sampling technique was used. Approval from Institutional Ethical Committee was obtained. Written and informed consents were sought from parents/guardians of all study participants. Inclusion criteria were full-term neonates of either gender, birth weight ≥ 2500 grams, and presenting with jaundice (serum bilirubin levels > 12mg/dl), [12] within 2 days of life. Term neonate was defined as a baby born between 37 and 42 weeks of gestation. Exclusion criteria were preterm neonates, birthweight < 2500 grams, or dysmorphic neonates.
Participants fulfilling the eligibility criteria were included and analyzed. Demographic neonatal and maternal characteristics were noted, and relevant laboratory investigationswere done. All laboratory investigations were done from central laboratory of Children Hospital Multan, free of cost. The element of bias was minimized as all the tests were performed from same laboratory. Confounding variables (like physiological jaundice) were controlled by strict following of inclusion and exclusion criteria. Rh incompatibility was defined as Rh –ve mother, Rh +ve baby and detectible antibodies in baby’s blood by direct coombs test [13]. A special proforma was designed to record study data.
Data were entered and analyzed using IBM-SPSS, version 26.0. Median and interquartile range were calculated for numeric data as the distribution of these variables were non normal. Frequency and percentages were shown for qualitative data. For the comparison of qualitative data, chi-square test was applied. Mann-Whiteny U test was employed to compare numeric data. For all inferential statistics, p<0.05 was considered as significant.
Results
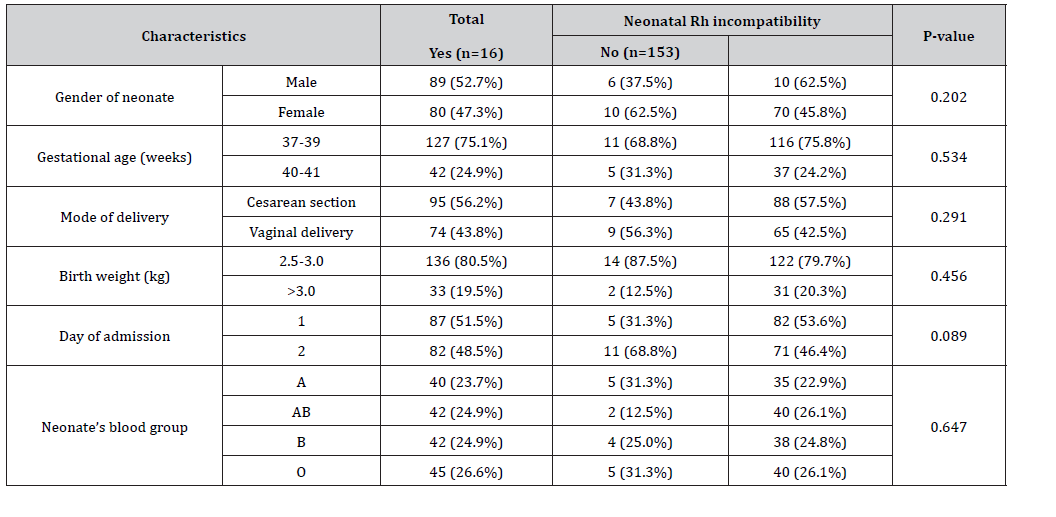
Among the total of 169 neonates, 89 (52.7%) were male, and the median (IQR) gestational age was 38 (37-40) weeks. Mode of delivery was cesarean section among 95 (56.2%) cases. The median birth weight was 2.90 (2.65-3.00) kg. There were 87 (51.5%) neonates who were admitted within 24-hours of life. The most common blood group among neonates was O, noted in 45 (26.6%) cases. Rh incompatibility was identified in 16 (9.5%) cases. Rh incompatibility was more common in female neonates (62.5% vs 45.8%, p=0.202), and among those born via vaginal delivery (56.3% vs 42.5%, p=0.291). There was no significant association between birth weight and Rh incompatibility (p=0.456). A relatively higher proportion of neonates with Rh incompatibility were admitted on day 2 of life compared to those without Rh incompatibility (68.8% vs 46.4%), but the difference did not reach statistical significance (p=0.089).
Table 1:Association of Rh incompatibility with neonatal characteristics (N=169).
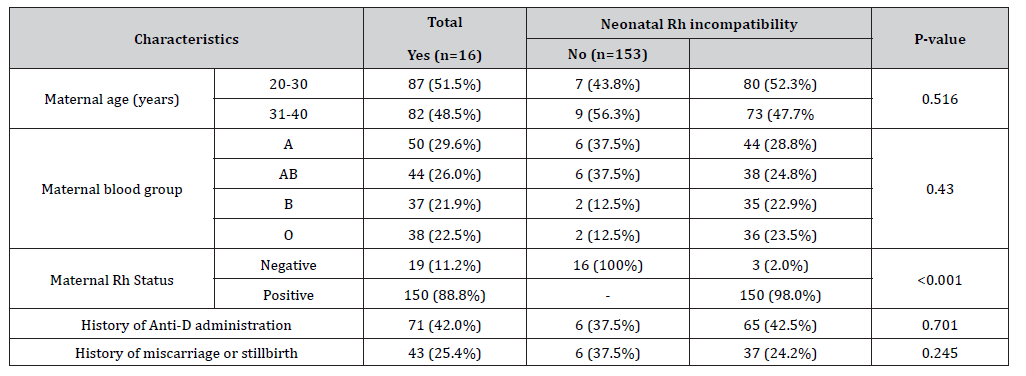
Among maternal characteristics, 19 of 169 (11.2%) mothers were Rh-negative, all of whom had neonates with Rh incompatibility (100% vs 2.0%, p<0.001). The distribution of maternal blood groups among Rh-incompatible neonates was 6 (37.5%) with type A, 6 (37.5%) with AB, 2 (12.5%) with B, and 2 (12.5%) with O (P = 0.430). Anti-D immunoglobulin was administered in 6 37.5% Rh-incompatible cases compared to 42.5% Rh-compatible cases (p=0.701). History of miscarriage or stillbirth was reported in 37.5% mothers of Rh-incompatible neonates vs 24.2% in Rhcompatible neonates (p=0.245) (Table 2).
Table 2:Association of Rh incompatibility with maternal characteristics (N=169).
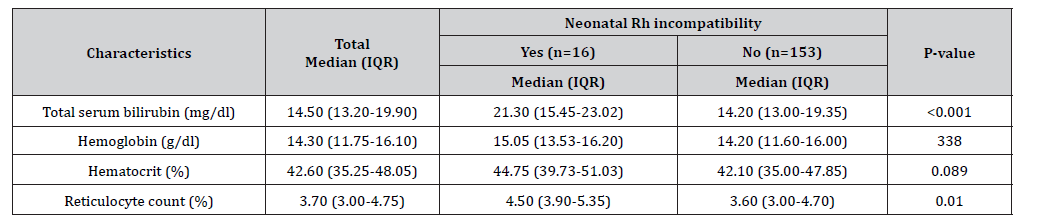
Neonates with Rh incompatibility had significantly higher median (IQR) total serum bilirubin levels than those without (21.30 [15.45-23.02] mg/dL vs 14.20 [13.00-19.35] mg/dL, p<0.001). The median (IQR) hemoglobin level was similar between Rh-incompatible and Rh-compatible neonates (15.05 [13.53- 16.20] g/dL vs 14.20 [11.60-16.00] g/dL; p=0.338). Hematocrit levels were slightly higher in Rh-incompatible neonates (median [IQR] 44.75 [39.73-51.03] % vs 42.10 [35.00-47.85] %; p=0.089). The median (IQR) reticulocyte count was significantly elevated in Rh-incompatible neonates compared to those without (4.50 [3.90- 5.35] % vs 3.60 [3.00-4.70] %; p=0.010) (Table 3).
Table 3:Association of Rh incompatibility with laboratory parameters (N=169).
Discussion
In this study among neonates with jaundice, 9.5% had Rh incompatibility. The frequency of Rh incompatibility in jaundiced neonates varies in literature, with Irshad et al. [11], reporting a 12.5% prevalence, which is slightly higher than the present study, while Patel et al. [14], found it to be 1.37% in their cohort. Alkhotani et al. [15], documented the prevalence of Rh incompatibility in neonatal jaundice as 2.6%. Zelelew et al from Ethiopia revealed the prevalence of Rh incompatibility among neonatal jaundice as8.8% which is very close to what this study revealed.6These variations can be attributed to differences in sample sizes, study designs, and regional variations in maternal Rh-negative status. This study also found a relatively higher prevalence of Rh incompatibility among female neonates (62.5%), a pattern also reported by Patel et al. [14], who found that Rh-incompatible neonates had a higher risk of requiring treatment compared to ABO-incompatible neonates (65% vs 56%). However, unlike Irshad et al. [11], who found 70% of jaundiced neonates to be male, this study had a more balanced gender distribution (52.7% male). This difference could be due to random variation or gender-based referral biases in different hospital settings.
A key laboratory finding in this study was that neonates with Rh incompatibility had significantly higher serum bilirubin levels compared to those without Rh incompatibility (21.30 mg/dL vs 14.20 mg/dL, p<0.001). This is consistent with findings from Singh et al. [16], who reported that Rh incompatibility leads to more severe hyperbilirubinemia requiring intervention compared to ABO incompatibility. Patel et al. [14], found that 10% of Rhincompatible neonates developed kernicterus, whereas only 0.5% of ABO-incompatible neonates developed kernicterus, highlighting the greater clinical significance of Rh isoimmunization.
Despite the well-documented role of Anti-D immunoglobulin in preventing Rh incompatibility, this study found that 37.5% of mothers of Rh-incompatible neonates had received Anti-D prophylaxis, a proportion comparable to findings in Girish et al. [17], who noted that jaundice was 3.97 times more likely in Rh +ve neonates born to multiparous Rh-negative mothers who had not received Anti-D. The persistence of Rh incompatibility despite prophylaxis could be due to suboptimal dosing, delayed administration, or alloimmunization in previous pregnancies [18,19].
The finding that Rh-incompatible neonates had higher bilirubin levels than their counterparts is expected, given that Rh isoimmunization leads to significant hemolysis and unconjugated hyperbilirubinemia [20,21]. This study found only a slight increase in hemoglobin and hematocrit levels in Rh-incompatible neonates, unlike Routray et al. [22], who reported a strong correlation between hemoglobin levels and DAT positivity.
The findings of this study have several important clinical implications. The identification of Rh incompatibility in 9.5% of neonates presenting with jaundice underscores the continued need for routine antenatal Rh screening and timely administration of Anti-D immunoglobulin. Despite the availability of Anti-D prophylaxis, a considerable proportion of neonates still develop Rh isoimmunization, suggesting the need for better maternal education and improved compliance with prophylaxis protocols. The significantly higher bilirubin levels in Rh-incompatible neonates reinforce the need for early bilirubin monitoring in Rhnegative mothers to prevent severe complications like kernicterus [23]. The lack of a significant association between birth weight and Rh incompatibility suggests that all Rh-negative pregnancies should be treated as high-risk regardless of neonatal birth weight [24]. The observed trend of Rh-incompatible neonates being admitted later than their Rh-compatible counterparts (68.8% on day 2 vs 46.4%) suggests that early postnatal bilirubin screening is essential in Rhnegative pregnancies, even if the neonate appears clinically well at birth.
This study has several limitations. The study was conducted at a single tertiary care hospital, which may limit the generalizability of findings to other settings, particularly rural areas where antenatal care practices may differ. This study did not assess maternal antibody titers or neonatal hemolysis markers (e.g., lactate dehydrogenase, bilirubin/albumin ratio), which could have provided additional insight into disease severity. The sample size was relatively modest, which may have limited the power to detect subtle associations between Rh incompatibility and neonatal characteristics. The lack of follow-up data precludes conclusions about long-term neurodevelopmental outcomes in affected neonates.
Conclusion
This study found that 9.5% of neonates presenting with jaundice had Rh incompatibility, with female neonates and vaginal deliveries being slightly more common. Rh-incompatible neonates had significantly higher bilirubin levels compared to their counterparts, reinforcing the need for early screening and intervention. Despite widespread use of Anti-D immunoglobulin, a considerable proportion of mothers of Rh-incompatible neonates had received prophylaxis, suggesting the need for improved implementation of preventive strategies. These findings highlight the ongoing importance of Rh screening, timely prophylaxis, and neonatal bilirubin monitoring to prevent severe hyperbilirubinemia and its complications. Future research with larger multicenter studies and longer follow-up is needed to further assess the long-term outcomes of Rh-incompatible neonates and optimize prevention strategies.
Acknowledgement
None.
Conflicts of Interest
None.
References
- Lauer BJ, Spector ND (2011) Hyperbilirubinemia in the newborn. Pediatr Rev 32(8): 341-9.
- Horn D, Ehret D, Suresh G, Soll R (2021) Sunlight for the prevention and treatment of hyperbilirubinemia in term and late preterm neonates. Cochrane Database Syst Rev 7(7): CD013277.
- Wang J, Guo G, Li A, Cai WQ, Wang X (2021) Challenges of phototherapy for neonatal hyperbilirubinemia (Review). Exp Ther Med 21(3): 231.
- Jaundice in newborn babies under 28 days. London: National Institute for Health and Care Excellence (NICE); 2023 Oct 31. (NICE Guideline, No. 98.).
- Anne RP, Rahiman EA, Dudeja S, Kumar A (2023) Diagnostic Accuracy of Cord Bilirubin to Predict the Need for Phototherapy in Healthy Neonates >35-Week Gestational Age: A Systematic Review and Meta-Analysis. J Clin Exp Hepatol 13(4): 666-681.
- Zelelew AM, Tafere TZ, Jemberie SM, Belay GM (2024) Prevalence and Associated Factors of Jaundice Among Neonates Admitted to Neonatal Intensive Care Units at Public Specialized Hospitals in Bahir Dar City, Northwest Ethiopia. Glob Pediatr Health 11: 2333794X241286739.
- Bhutani VK, Zipursky A, Blencowe H, Khanna R, Sgro M, et al. (2013) Neonatal hyperbilirubinemia and Rhesus disease of the newborn: incidence and impairment estimates for 2010 at regional and global levels. Pediatr Res 74 Suppl 1(Suppl 1): 86-100.
- Loua A, Lamah MR, Haba NY, Camara M (2007) Fréquence des groupessanguins ABO et rhésus D dans la population guinéenne [Frequency of blood groups ABO and rhesus D in the Guinean population]. Transfus Clin Biol 14(5):435-9.
- Bergström S, Pereira C, Hagström U, Säfwenberg J (1994) Obstetric implications of rhesus antigen distribution in Mozambican and Swedish women. GynecolObstet Invest 38(2):82-6.
- Jackson ME, Baker JM (2021) Hemolytic Disease of the Fetus and Newborn: Historical and Current State. Clin Lab Med 41(1): 133-151.
- Irshad M, Ameer M, Mohammaed H, Behram K, Nusrat A (2011) Prevalence of Rhesus type & ABO incompatibility in jaundicedneonates. J Postgrad Med Inst 25(3): 233-239.
- Usatin D, Liljestrand P, Kuzniewicz MW, Escobar GJ, Newman TB (2010) Effect of neonatal jaundice and phototherapy on the frequency of first-year outpatient visits. Pediatrics 125(4): 729-34.
- Neamţu SD, Novac MB, Neamţu AV, Stanca ID, Boldeanu MV, et al. (2022) Fetal-maternal incompatibility in the Rh system. Rh isoimmunization associated with hereditary spherocytosis: case presentation and review of the literature. Rom J MorpholEmbryol 63(1):229-235.
- Patel AS, Desai DA, Patel RA (2017) Association of ABO and Rh incompatibility with neonatal hyperbilirubinaemia. Int J Reprod Contracept ObstetGynecol 6(4): 1368-1375.
- Alkhotani A, Eldin EE, Zaghloul A, Mujahid S (2014) Evaluation of neonatal jaundice in the Makkah region. Sci Rep 4: 4802.
- Singh SK, Manu K, Simlai S (2020) Clinical Severity of Neonatal Jaundice Especially in ABO and Rh Incompatibility in Northern India. Ann Int Med Dent Res 6(5):PE07-PE10.
- Girsh N, Santosh S, Keshavamurthy SR (2013) Evolving trends: hyperbilirubinemia among newborns delivered to rh negative mothers in southern India. J Clin Diagn Res 7(11): 2508-610.
- Hamel C, Esmaeilisaraji L, Thuku M, Michaud A, Sikora L, et al. (2020) Antenatal and postpartum prevention of Rh alloimmunization: A systematic review and GRADE analysis. PLoS One 15(9): e0238844.
- Saha SC, Rai R, Bagga R, Jain A, Mukhopadhyay K, et al. (2021) Pregnancy Outcome of Rh D Alloimmunized Pregnancies: A Tertiary Care Institute Experience of a Developing Country. J Obstet Gynaecol India 71(6): 583-590.
- Agrawal A, Hussain KS, Kumar A (2020) Minor blood group incompatibility due to blood groups other than Rh(D) leading to hemolytic disease of fetus and newborn: a need for routine antibody screening during pregnancy. Intractable Rare Dis Res 9(1): 43-47.
- Haider M, Memon S, Tariq F, Fatima S, Hameed A (2020) Rhesus Isoimmunization: Late-onset Hemolytic Disease of the Newborn Without Jaundice. Cureus 12(1): e6559.
- Routray SS, Behera R, Mallick B, Acharya D, Sahoo JP, et al. (2021) The Spectrum of Hemolytic Disease of the Newborn: Evaluating the Etiology of Unconjugated Hyperbilirubinemia Among Neonates Pertinent to Immunohematological Workup. Cureus 13(8): e16940.
- Naeem H, Ullah K, Ochani S, Naeem K, Ahmad HB, et al. (2023) The need for neonatal jaundice screening awareness in the Pakistani population: short communication. Ann Med Surg (Lond) 85(8): 4187-4189.
- Aliyo A, Ashenafi G, Abduselam M (2023) Rhesus Negativity Prevalence and Neonatal Outcomes among Pregnant Women Delivered at Bule Hora University Teaching Hospital, West Guji Zone, South Ethiopia. Clin Med Insights Pediatr 17: 11795565221145598.
-
Maria Hassan*, Syed M Dur E Sabih Haider, Tuba Qaisar, Jam Ali Haider, Rushan Hassan, Bushra Urooj. Frequency of Rh Incompatibility among Neonates Presenting with Jaundice at Children Hospital, Multan, Pakistan. Glob J of Ped & Neonatol Car. 5(4): 2025. GJPNC.MS.ID.000616.
Gestational age, Janundice, Reticulocyte count, Rh incompatibility, Serum bilirubin, Hemolytic disease, Pediatrics, Children
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






