 Research Article
Research Article
Dyspnea In Children with Diagnosed Asthma and Undiagnosed Asthma, A Cross- Sectional Study
Melpomeni Bizhga MD1* and Anita Pollozhani MD2
1 University Hospital Nene Tereza, Pediatric Hospital, Pulmonology Service, Tirane, Albania
2 University Hospital Nene Tereza, Pediatric Hospital, Pulmonology Service, Tirane, Albania
Melpomeni Bizhga, University Hospital Nene Tereza, Pediatric Hospital, Pulmonology Service, Tirane, Albania
Received Date: August 19, 2025; Published Date:September 17, 2025
Abstract
Back ground: Asthma is a prevalent chronic respiratory condition that significantly affects pediatric populations globally. This study aims to
describe the subjective perception of dyspnea in asthma crisis in children with diagnosed asthma and not diagnosed asthma.
Methods: This study employs a cross-sectional observational design aimed to evaluate the subjective perception of dyspnea in two distinct
pediatric groups. The study involved a cohort of 38 children, in Hospital Mother Teresa, Tirane. Box plot comparing and Pearson s correlation
coefficient were used to compare values of Borg scale in both groups, at admission and after 6 hours.
Results: Children in the previously diagnosed asthma, DA group, demonstrated a more severe baseline level of dyspnea, as indicated by higher
Borg scale scores, with an average initial score of 5.04. Following the reintroduction of treatment, this group experienced a substantial reduction
in symptoms, with Borg scale scores decreasing to an average of 1.95, representing a significant improvement of 3.1 points. In contrast, children in
the newly diagnosed asthma, NDA group, exhibited milder symptoms at the outset, with an average initial Borg scale score of 4.06. Post treatment,
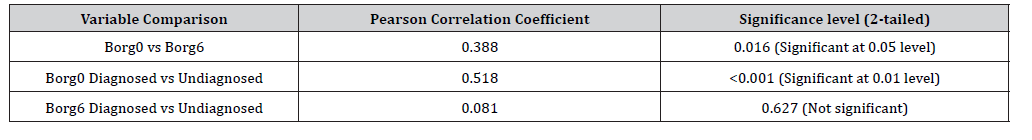
their scores improved to an average of 1.82, marking an improvement of 2.2 points. Pearson s coefficient correlation in Borg at admission and after
6 hours (0.016) showed a significant improvement in dyspnea scale. Pearson s coefficient at admission was significant (<0.001) in both diagnosed
and not diagnosed patients. Pearson s coefficient was not significant (0.627) in both diagnosed and not diagnosed children with asthma after 6 hours
of treatment.
Conclusion: The greater improvement in the Borg scale for the DA group suggests that previously diagnosed children, despite presenting with
more severe symptoms initially, experience more substantial benefits from treatment reintroduction. This highlights the potential impact of earlier
treatment interruptions on symptom severity and suggests that continuous treatment can lead to better outcomes.
Keywords: Asthma, Children, Borg scale
Back Ground
Asthma is a prevalent chronic respiratory condition that significantly affects pediatric populations globally. This study aims to describe the subjective perception of dyspnea in asthma crisis in children with diagnosed asthma and not diagnosed asthma. In pediatric and adult populations asthma has consequences in public health related to high morbidity and in extreme cases, mortality. It is estimated that approximately 300 million individuals globally have asthma [1].
Asthma-related fatalities occur in low- to middle-income countries. Patient education, particularly related the understanding and reporting of dyspnea, is very important when an acute attack happens. The incidence of severe asthma in children who have asthma can reach up to 5% of the affected population [1].
Objectives/ Hypothesis
Children with undiagnosed asthma have a poor perception of dyspnea, postponing the report of symptoms and treatment.
Methods
This observational, cross-sectional, one center study is based on a preset questionnaire. This was filled from the doctor on duty in emergency service in tertiary care center Mother Tereza, Tirane, where is managed the acute attack of asthma in children. The study utilized the Borg scale as a simple numerical scale to assess the subjective perception of dyspnea among children experiencing an asthma crisis./p>
Setting and population
The aim of this study is to compare the perception of dyspnea in two distinct groups of children with asthma crisis, in children who had experienced dyspnea before due to asthma crisis and children that had no previous crisis and diagnosed as having asthma.
Characteristics of participants
Children 5-14 years old that had a asthma crisis that is resolved completely in hours and days during this hospitalization. Children with asthma crisis that were presented to emergency service during fall (October-January) 2023 in Emergency department of UHC Mother Teresa were subject to this study.
Inclusion criteria:
44 children who had either ceased or not initiated prophylactic asthma treatment and presented to the pediatric emergency department. They were divided in two distinct categories: Prior Diagnosed Asthma (DA) or Non diagnosed Asthma (NDA) Children aged five years and above are included, so that participants could reliably communicate their dyspnea perceptions, in order to comply with the study’s procedural requirements.
Interventions
Response to Salbutamol
Initial salbutamol aerosol treatment were administered and 6 children had complete resolution of symptoms, therefore were excluded from the study.
For the remaining participants, the effectiveness of salbutamol inhalation was a critical criterion for study inclusion. This effectiveness was defined quantitatively as an increase in Forced Expiratory Volume in 1 second (FEV1) of at least 12% from the baseline measurement at the end of the first hour after salbutamol administration, as a criterion for asthma definition In children.
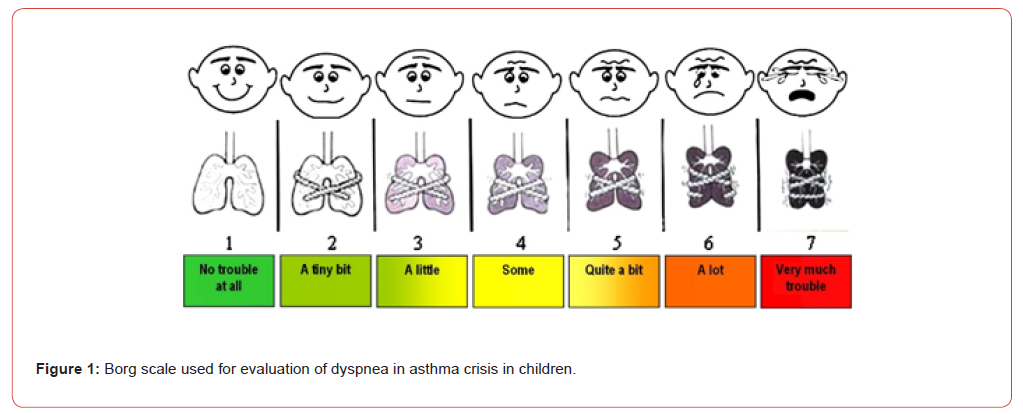
17 children without a prior asthma diagnosis were included in NDA group (Non Diagnosed Asthma) DA (Prior Diagnosed Asthma) group consisted of 21 children with a history of diagnosed asthma who had not adhered to prophylactic treatment. The objective of this group was to investigate the influence of asthma diagnosis awareness on the perception of dyspnea and the manifestation of respiratory distress during an asthma attack. The study utilized the Borg scale as a simple numerical scale to assess the subjective perception of dyspnea among children experiencing an asthma crisis. This scale is a self-reported measure that allows individuals to rate the intensity of their breathlessness on a numerical scale, typically ranging from 0 (no breathlessness at all) to 7 (maximum breathlessness).
The study’s children were shown and explained the scale and asked to place themselves there to rate their difficulty breathing both at the initial presentation during the asthma crisis and again after a period of 6 hours. This approach is designed to capture the immediate subjective experience of respiratory discomfort as well as any changes in perception following the onset of the crisis or after the administration of any interventions.
Exclusion Criteria
Children who showed complete alleviation of symptoms immediately following the initial salbutamol aerosol treatment were excluded (6 children).
Data analyses and Processing
SPSS 16.0 software was used to analyze the data received. Histograms, box plots, and correlations were used (Pearson s correlation) Diagnostic value of analysis results in translation of a subjective measure as dyspnea in numbers in order to be more alert to not diagnosed children with dyspnea that are in greater risk for deterioration.
Results
Table 1:Results of correlation analysis Borg at admission versus Borg after 6 hours in diagnosed and undiagnosed children with asthma crises.
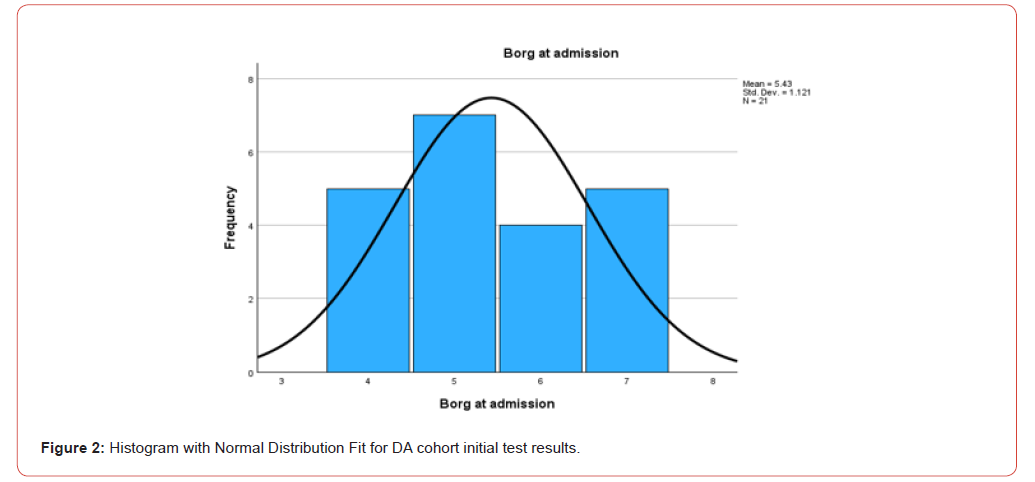
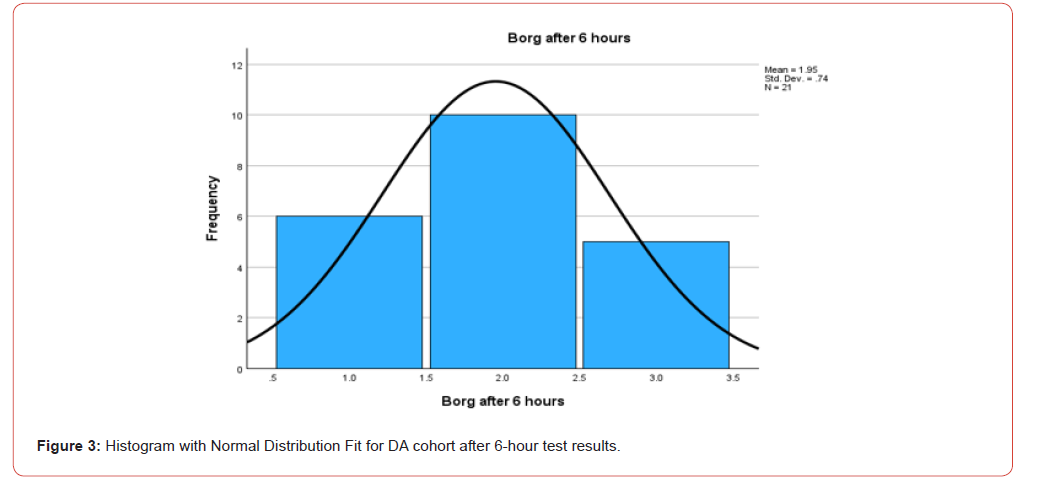
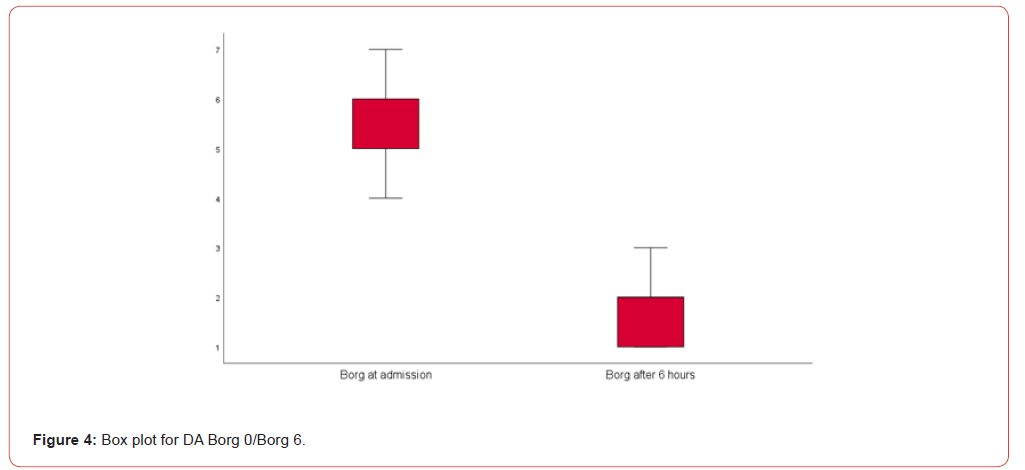
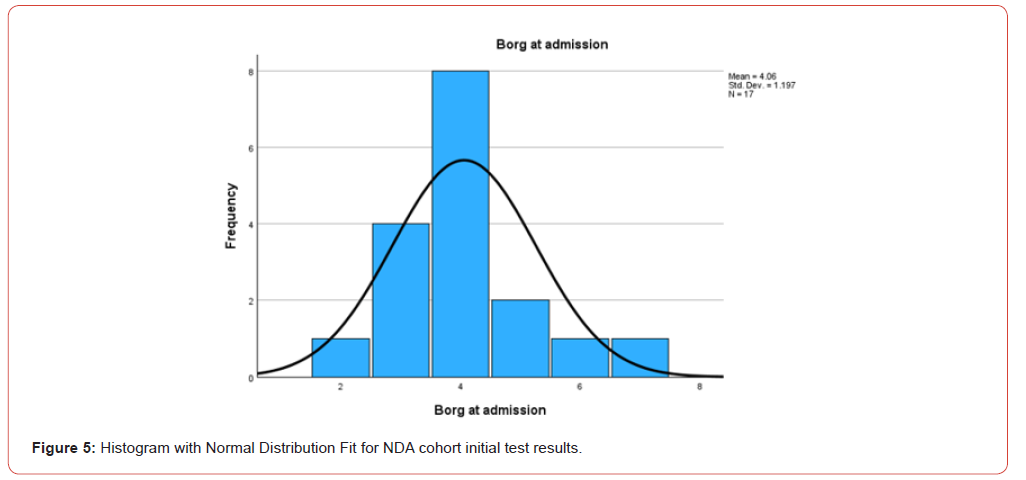
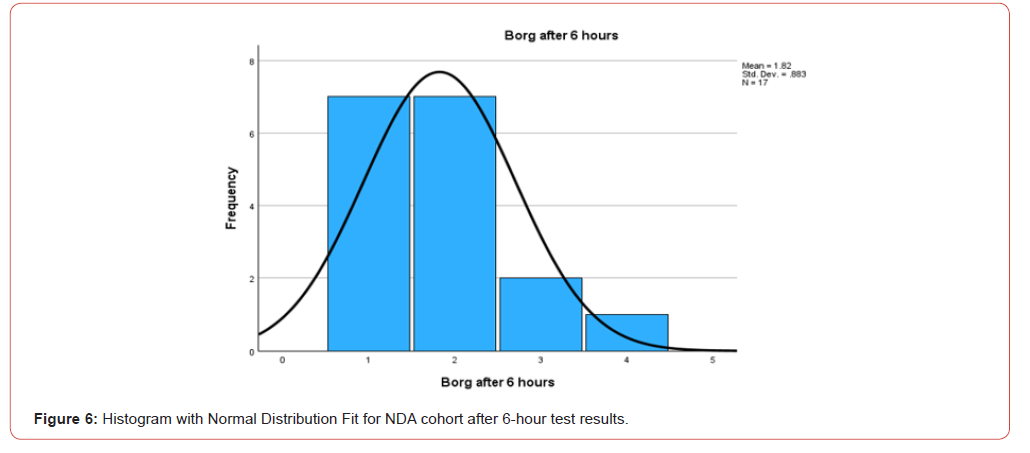
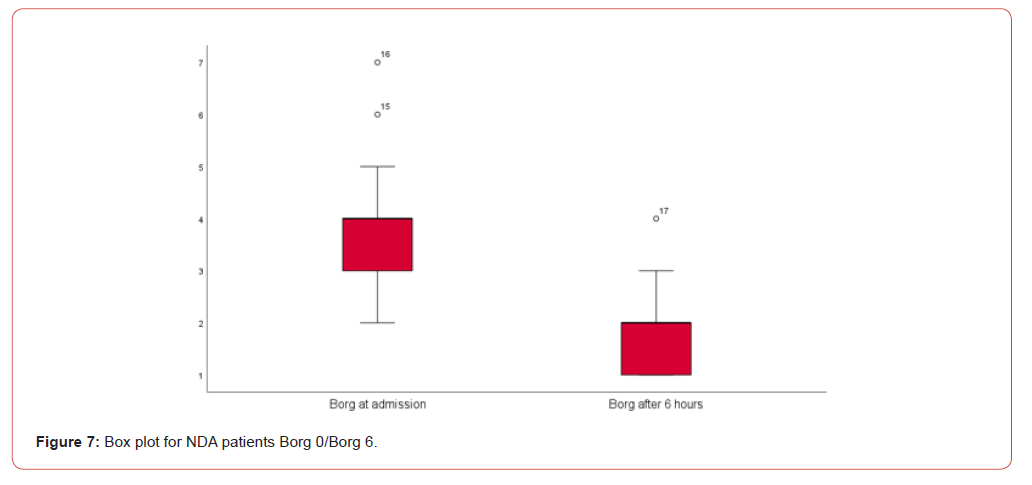
Children in the DA group demonstrated a more severe baseline level of dyspnea, as indicated by higher Borg scale scores, with an average initial score of 5.04. Following the reintroduction of treatment, this group experienced a substantial reduction in symptoms, with Borg scale scores decreasing to an average of 1.95, representing a significant improvement of 3.1 points. In contrast, children in the NDA group exhibited milder symptoms at the outset, with an average initial Borg scale score of 4.06. Post-treatment, their scores improved to an average of 1.82, marking an improvement of 2.2 points.
The greater improvement in the Borg scale for the DA group suggests that previously diagnosed children, despite presenting with more severe symptoms initially, experience more substantial benefits from treatment reintroduction. This highlights the potential impact of earlier treatment interruptions on symptom severity and suggests that continuous treatment can lead to better outcomes.
This faster alleviation of symptoms could be attributed to the body’s previous adaptation to asthma medications, which may facilitate a more rapid therapeutic response upon re-exposure. This observation suggests that children with a history of asthma treatment may benefit from a kind of ‘therapeutic memory’ that allows their bodies to respond more quickly to reintroduced medications.
The data indicates that children in the DA group, who had a higher baseline severity of dyspnea as shown by higher initial Borg scale scores, experienced more substantial improvements after treatment compared to those in the NDA group.
Discussion
Understanding of the pathophysiological mechanisms underlying dyspnea is still evolving. No specific receptors for dyspnea have been identified, and the absence of a clear initiation point for sensory nerve transduction pathways complicates understanding its neurophysiology. Unlike well-defined sensory systems such as vision, hearing, or pain, the neural pathways for the sensation of dyspnea need to be delineated. Nevertheless, F. I. Fukushi et al. [2] determined that sensory information from the respiratory system is conveyed via intact afferent pathways to the cerebral cortex, interpreted as the subjective experience of breathlessness.
The Motor Command Theory, as explained by R. M. Schwartzstein et al. [3], posits that the sensation of dyspnea arises when the effort to breathe, as commanded by the brain, is perceived as excessive. This makes it a crucial study area in conditions like asthma, where airway obstruction is prevalent. According to this theory, the sensory cortex receives signals commensurate with the effort required to overcome bronchoconstriction, translating into the subjective experience of breathlessness.
In contrast, the Mismatch Theory, articulated by E. L. De Vito [4], suggests that dyspnea results from a dissonance between the brain’s respiratory commands and the mechanical responses of the lungs and chest wall. In the current study, children experiencing an asthma crisis may perceive severe dyspnea if their respiratory effort (to overcome increased airway resistance and decreased lung compliance) does not suffice to achieve adequate ventilation, as reflected in their subjective Borg scale assessments and objective measures such as PEFR.
In contrast, the Mismatch Theory, articulated by E. L. De Vito [4], suggests that dyspnea results from a dissonance between the brain’s respiratory commands and the mechanical responses of the lungs and chest wall. In the current study, children experiencing an asthma crisis may perceive severe dyspnea if their respiratory effort (to overcome increased airway resistance and decreased lung compliance) does not suffice to achieve adequate ventilation, as reflected in their subjective Borg scale assessments and objective measures such as PEFR.
The Mismatch Theory elucidates the observations where, despite similar treatments, the subjective experience of dyspnea (Borg scores) differs markedly between NDA and DA groups, which could stem from varying degrees of airway responsiveness and mechanical efficiency between newly diagnosed versus previously treated children. The Integrated Model helps in understanding the multifaceted nature of dyspnea in asthma, where not just the airway mechanics but also inflammatory and possibly chemoreceptive changes play roles, as evidenced by the variability in Borg scores.
The impact of dyspnea on verbal expression varies with its severity, a point noted by M. J. Johnson et al. [6]. A child without dyspnea can speak in entire sentences without interruption. With moderate dyspnea, speech becomes broken into phrases, often interrupted by breaths. In cases of severe dyspnea, the child may be able to utter only a few words at a time or might altogether refrain from speaking and eating due to the effort involved.
The use of accessory muscles also correlates with the intensity of the respiratory crisis. In mild episodes, the intercostal muscles are not noticeable. As the crisis intensifies to a moderate level, the intercostal muscles moderately retract, and the sternocleidomastoid muscle is involved. In severe cases, pronounced retraction can be observed in the sternocostal and tracheosternal areas, and significant nasal flaring during inspiration indicates substantial respiratory distress.
In exploring methodologies to assess the severity of shortness of breath in asthma, researchers have employed the Borg Dyspnea Scale and developed and recommended additional tools. The Numerical Rating Scale (NRS) and the modified Borg scale (mBorg) are prominent among these.
Furthermore, P. T. Pianosi’s [7] work introduced the Dalhousie Dyspnea and Perceived Exertion Scales, providing a new pictorial method for assessing dyspnea and perceived exertion during physical activities. This innovation was particularly validated in healthy adults and individuals with pulmonary disorders, comparing the outcomes with those obtained from the Borg scale. The Dalhousie scales are an intuitive alternative for evaluating perceived exertion and breathlessness. They offer advantages for populations that may find traditional scales challenging.
These advancements and alternatives to the Borg scale are significant as they offer diverse methods to assess the subjective experience of breathlessness, accommodating different patient needs and research contexts.
As O. Lagiou et al. [8] have indicated, the Borg scale is a wellestablished tool for quantifying perceived exertion and assessing functional limitations in respiratory conditions. It has traditionally found its primary applications within the context of chronic respiratory diseases, including asthma in children. However, the scope of the Borg scale’s utilization has expanded significantly beyond merely measuring exercise tolerance or functional impairment.
Research in this field has been pivoting towards a more dynamic application of the Borg scale, particularly in evaluating the severity of acute asthmatic events. This shift underscores the scale’s versatility and adaptability as the medical practice evolves to meet the pressing need for quick and accurate assessments during asthmatic crises.
While the Borg scale is undoubtedly well-suited for monitoring functional capacity, the emerging perspective within current studies suggests a promising approach to using the scale in crisis scenarios. This expanded application involves tracking how asthma interferes with daily activities and how it manifests during an emergency. The capability of the Borg scale to provide immediate, patientreported insights into breathlessness can significantly enhance the management of acute asthma exacerbations.
Adopting the Borg scale in this broader capacity could improve patient outcomes by facilitating more precise and timely interventions. This expanded use aligns with ongoing efforts to optimize asthma management protocols, ensuring that they are comprehensive and tailored to meet patients’ acute needs. The potential of the Borg scale to contribute to acute asthma care highlights its importance as a versatile tool that goes beyond traditional boundaries, offering both reliability and critical insights into patient health during moments of medical urgency.
There was no clear correlation between the severity of objective symptoms and the subjective perception of wheezing during exacerbation of asthma in children. Douros, K. et al. [9], in their work, noted that the correlation between objective measures of respiratory distress and subjective awareness of dyspnea is weak
Due to adaptation, children with undiagnosed asthma are associated with frequent bronchoconstriction and may be tolerant to some of bronchoconstriction.
Delayed and/or underdiagnosis and undertreatment of asthma in children that have a poor perception of dyspnea of asthma attack, results at risk of severe, even life-threatening asthma attacks. Those who do not perceive dyspnea may not be motivated to comply with prophylaxis. They tend to seek medical help only late in their flareups. Despite suffering from asthma they are not diagnosed and treated.
In this context, the lack of prophylactic treatment combined with poor vigilance may result in the first clear presentation of their disease as a severe and possibly life-threatening acute attack. Parents and caregivers appear to be even less accurate in detecting their child’s symptoms. This underscores the critical need for better education and awareness among both children with asthma and their caregivers to ensure timely and effective management of the condition.
The value of the Borg scale in acute asthma management lies in its ability to provide a direct, quantifiable assessment of the patient’s subjective experience of breathlessness. This subjective evaluation complements objective measures, such as lung function tests and oxygen saturation levels, to better understand the patient’s respiratory status. By incorporating the Borg scale into the clinical workflow, healthcare providers can gain valuable insights into the patient’s perceived symptom severity, which can inform tailored treatment strategies and guide real-time decision-making during acute asthmatic episodes.
Furthermore, longitudinal use of the Borg scale throughout an asthma exacerbation can offer insights into the patient’s response to various interventions. Tracking the changes in Borg scores before and after administering bronchodilators or other treatments can help healthcare providers evaluate the effectiveness of the management plan and make timely adjustments as needed.
Conclusion
Children in the DA group demonstrated a more severe baseline level of dyspnea, as indicated by higher Borg scale scores, with an average initial score of 5.04. Following the reintroduction of treatment, this group experienced a substantial reduction in symptoms, with Borg scale scores decreasing to an average of 1.95, representing a significant improvement of 3.1 points. In contrast, children in the NDA group exhibited milder symptoms at the outset, with an average initial Borg scale score of 4.06. Post-treatment, their scores improved to an average of 1.82, marking an improvement of 2.2 points.
The greater improvement in the Borg scale for the DA group suggests that previously diagnosed children, despite presenting with more severe symptoms initially, experience more substantial benefits from treatment reintroduction. This highlights the potential impact of earlier treatment interruptions on symptom severity and suggests that continuous treatment can lead to better outcomes.
The data indicates that children in the DA group, who had a higher baseline severity of dyspnea as shown by higher initial Borg scale scores, experienced more substantial improvements after treatment compared to those in the NDA group.
Ethics Approval and Consent to Participate
WMA declaration of Helsinki
This study adhered to Ethical Principles for medical Research involving human participants is applied. Informed consent for study participation is applied. 44 consent forms from parents were retrieved in order to get information for the scale of dyspnea.
Aknowlegment
NO FUNDING was placed for this study.
Conflict of Interst
None.
References
- Ohwada A, Sato K (2019) Heterogeneity of perception of symptoms in patients with asthma. Journal of Thoracic Disease 11(12): 5218-5227.
- Fukushi I, Pokorski M, Okada Y (2021) Mechanisms underlying the sensation of dyspnea. Respiratory Investigation 59(1): 66-80.
- Schwartzstein R M, Sturley R (2023) Dyspnea and mechanical ventilation: applying physiology to guide therapy. Transactions of the American Clinical and Climatological Association 133: 162-180.
- De Vito E L (2023) Series on Dyspnea. Part 3. Mechanisms, efferent copy or corollary discharge. Revista americana de medicina respiratoria 23(4): 362-368.
- Ibsen S, Laursen B S, Christensen E F, Weinreich U M, Mikkelsen S, et al. (2022) How Patients Who Are Transported by Ambulance Experience Dyspnea and the Use of a Dyspnea Scale: A Qualitative Study. In Healthcare 10(7): 1208.
- Johnson M J, Close L, Gillon S C, Molassiotis A, Lee P H, et al. (2016) Use of the modified Borg scale and numerical rating scale to measure chronic breathlessness: a pooled data analysis. European Respiratory Journal 47(6): 1861-1864.
- Pianosi P T, Zhang Z, Hernandez P, Huebner M (2016) Measuring dyspnea and perceived exertion in healthy adults and with respiratory disease: new pictorial scales. Sports medicine-open 2: 17.
- Lagiou O, Fouzas S, Lykouras D, Sinopidis X, Karatza A, et al. (2022) Exercise limitation in children and adolescents with mild-to-moderate asthma. Journal of asthma and allergy 15: 89-98.
- Douros K, Boutopoulou B, Papadopoulos M, Fouzas S (2015) Perception of dyspnea in children with asthma. Frontiers in bioscience (Elite edition) 7(3): 469-477.
-
Melpomeni Bizhga MD* and Anita Pollozhani MD. Dyspnea In Children with Diagnosed Asthma and Undiagnosed Asthma, A Cross- Sectional Study. Glob J of Ped & Neonatol Car. 5(5): 2025. GJPNC.MS.ID.000621..
Asthma, Children, Borg scale, Adult populations, Public health, Hypothesis, DA group, Respiratory, Diagnosed children
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






