 Case Report
Case Report
Deficiency of Vitamin E and Dehydration as a Cause of Deep Venous Thrombosis in a Child with Cystic Fibrosis
Melpomeni Bizhga1 and Virtut Velmishi2*
1Service of Pediatric Pulmonology, Mother Teresa Hospital, Albania
2Service of Pediatric Gastroenterology, Mother Teresa Hospital, Albania
Virtut Velmishi, Pediatric Department, UHC Mother Teresa, Dibra Street nr 372, Tirana-Albania.
Received Date: December 04, 2020; Published Date: January 08, 2021
Abstract
Deep vein thrombosis (DVT) is caused by a blood clot that occurs in the deep venous system. DVTs are rare in healthy children but may occur more commonly in children that are hospitalized or have chronic diseases. Children with cystic fibrosis have a higher risk to develop deep vein thrombosis. Signs and symptoms of DVT include swelling, pain, and changes in skin color of the affected limb. Diagnosis of DVT is usually confirmed with an imaging test such as an ultrasound. Treatment for DVT includes waiting and watching to see what happens, medication, thrombolysis, or surgery. We describe a child with cystic fibrosis who presented a deep vein thrombosis of left leg as a cause of dehydration and vitamin E deficiency
Keywords:Deep vein thrombosis; Cystic fibrosis; Vitamin E
Introduction
Venous thromboembolism is increasing in the pediatric population, especially in children with cystic fibrosis. Due to central venous catheters, acquired thrombophilia due to chronic inflammation, deficiency of anticoagulant proteins due to vitamin K deficiency or liver dysfunction [1]. Vitamin E supplements are given to children with fat malabsorption such as in cystic fibrosis and cholestatic liver disease [2].
Case Presentation
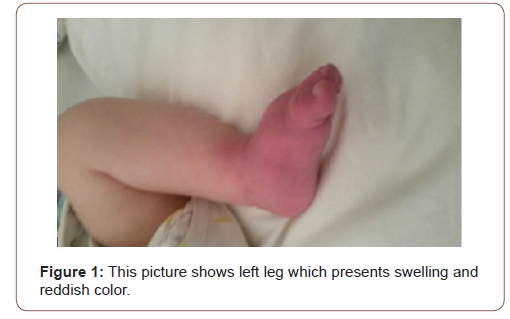
Our patient is the first child of an Albanian couple without consanguinity. Birth weight was 2400g Pregnancy and delivery were normal. This child was breastfed, but his mother noticed poor weight gain and several episodes of diarrhea. He was sent at our center at the age of 4 months. He presented failure to thrive and sweat test resulted 130 mmol/L confirming cystic fibrosis. No history of important disease in family. The rest of examination was quite normal except mild hypoalbuminemia and hyponatremia. After two albumin infusions and regulation of electrolyte disbalance this child was discharged at home with Creon, vitamin ADK supplement every day and vitamin E 100 mg/day in alternate days . A month later this child is returned to our service because of dehydration, poor feeding and developed swelling and tenderness of left leg . Skin over the affected area was turned reddish (Figure 1). He presented pain during leg movements associated with warm skin over affected zone . According to his mother treatment was not administrated properly because of frequent vomiting and child refusal.
Hemorrhage and coagulation test showed: hemorrhage time 2 min; coagulation time 3 min 30 sek; PT 89.5%; APTT C 27 sek.; D dimer was positive. Testing for secondary infections showed: CRP negative. Tests for viral and bacterial agents: negative. Other tests: Homocysteine 6.8 micro mol/l; Protein C 61% (N 70-110%); Protein S 67% (N 65-58%). Level of E vitamin was 0.8 mcg/mL (3- 18.4 μg/dL). We excluded antiphospholipid antibodies (aPLs), FV Leiden and antithrombin deficiency. Doppler ultrasound of the leg showed a blood clot at distal part of posterior tibial vein, but overall flow of the blood is not being constrained or restricted. We started immediately rehydration 3 l/m2 correcting hyponatremia. At the same time, we restarted creon, vitamin A,D,K and vitamin E 50 mg per day making sure a proper administration. We used antibiotics to prevent infection. Blood clot dissolved and leg took normal color 4 days later. During follow up this boy didn’t show any thrombosis phenomenon.
Discussion
The incidence of venous thromboembolism is increasing in pediatric population especially in hospitalized children [3]. Children with cystic fibrosis have an increased risk of thrombosis due to central venous catheters, as well as acquired thrombophilia secondary to inflammation or deficiencies of anticoagulant proteins due to vitamin K deficiency and liver dysfunction [4]. In our case we excluded these etiologies because our patient had not a central vein, he had a normal PCR excluding a severe inflammation. According to normal INR we logically can say that is excluded deficit of vitamin K Liver function was also normal. Most of our tests regarding thrombophilia resulted negative. It is well known that dehydration remains a serious cause of deep vein thrombosis such as in our case [5]. The second point which is not frequently described in literature is the deficiency of vitamin E as a cause of thrombosis. Vitamin E is all the following eight compounds alpha, beta ,gamma, and deltatocopherol and alpha, beta , gamma , and delta-tocotrienol. Alpha - tocopherol is the only compound of eight that are known to meet human dietary needs. All of the vitamin E forms are absorbed in small intestine, and then liver metabolizes only alpha-tocopherol. The liver then removes and excretes the remaining vitamin E forms [6-9]. Vitamin E is a lipid soluble nutrient. Patient with cystic fibrosis fail to secrete pancreatic enzymes to absorb vitamins A,D,E and K. Vitamin E inhibits platelet adhesion by preventing oxidative changes to LDLs and inhibition of platelet aggregation by reducing prostaglandin E2 [10]. In our patient we found a level of vitamin E 0.8 μg/dL [11-13]. In infants a level of vitamin E lower than 3 μg/dL is considered as deficiency. In this context we started immediately a prompt administration of vitamin E 100 mg per day for 7 days and later 50 mg per day continuously. We didn’t start thrombolytic agents because of small age of our patient and lack of experience. Preferring a strategy wait and see the outcome of conservative treatment including aggressive rehydration, creon and vitamin supplements resulted very efficient.
Conclusion
Indications of Alfa Tocopherol Acetate (Vitamin E) in cystic fibrosis are well designed. Vitamin E is given by mouth 50mg/ once day adjusted as necessary in children 1 month to 1 years old with cystic fibrosis. Deficiency of vitamin E associated with other risk factor such as dehydration in our case may lead to deep vein thrombosis. A prompt treatment can avoid serious complications. Other studies should be done to confirm our findings.
Acknowledgement
None.
Conflict of Interest
The authors declare that they don’t have conflict of interest.
References
- Askegard-Giesmann JR, O` Brien SH, Wang W, Kenney BD (2012) Increased use of enoxyparine in pediatric trauma patients. J Pediatr Surg 47(5): 980-983.
- Sapiejka E, Krzyzanowska-Janowska P, Wenska- Chuzy E, Szczepanik M, Walkowiak D, et al. (2018) Vitamin E status and its determinants in patients with cystic fibrosis. Adv Med Sci 63(2): 341-346.
- Raffini LJ, Raybagkar D, Blumenstein MS, Rubenstein RC, Manno CS (2006) Cystic fibrosis as a risk factor for recurrent venous thrombosis at a pediatric tertiary care hospital. J Pediatr 148(5): 659-664.
- Clifford M Takemoto (2012) Venous thromboembolism in Cystic fibrosis. Pediatric pulmonology 47(2): 105-112.
- Ishola T, Kirk Se, Guffey D, Voigt K, Shah MD, et al. (2016) Risk factors and co-morbidities in adolescent thromboembolism are different than those in younger children. Thromb Res May 141: 178-182.
- Kim HK, Han SN (2019) Vitamin E: Regulatory role on gene and protein expression and metabolomics profiles. IUBMB Life. 71(4): 442-455.
- Suzuki H, Kume A, Herbas MS (2018) Potential of Vitamin E Deficiency, Induced by Inhibition of α-Tocopherol Efflux, in Murine Malaria Infection. Int J Mol Sci 20(1): 64.
- Jilani T, Iqbal MP (2018) Vitamin E deficiency in South Asian population and the therapeutic use of alpha-tocopherol (Vitamin E) for correction of anemia. Pak J Med Sci 34(6): 1571-1575.
- Khadangi F, Azzi A (2019) Vitamin E - The Next 100 Years. IUBMB Life 71(4): 411-415.
- Tyler R Kemnic, Meghan Coleman (2020) Vitamin E deficiency. Stat Pearls Publishing.
- Burtis CA, Ashwood ER, Burns DE (2006) Tietz Textbook of Clinical Chemistry and Molecular Diagnostics. 4th St. Louis: Elsevier Saunders, USA.
- McPherson RA, Pincus MR (2011) Henry's Clinical Diagnosis and Management by Laboratory Methods. 22nd Philadelphia: Elsevier Saunders, USA.
- Wallach J (1996) Interpretation of Diagnostic Tests. 6th New York: Little, Brown.
-
Melpomeni Bizhga, Virtut Velmishi. Deficiency of Vitamin E and Dehydration as a Cause of Deep Venous Thrombosis in a Child with Cystic Fibrosis. Glob J of Ped & Neonatol Car. 3(2): 2021. GJPNC.MS.ID.000556.
Deep vein thrombosis, Cystic fibrosis, Vitamin E, Children, Deficiency, Child, Blood clot, Dehydration
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






