 Mini Review
Mini Review
Should We Repeat Imaging If Clinical Suspicion is High in Axial Spondyloarthritis, A Case Report.
Anupama Nandagudi1, Krisztina Szabo-Kocsis2 and Michael Dare3*
1Anupama Consultant Rheumatologist Basildon University Hospital
2Krisztina Consultant Rheumatologist Connect Health
3Michael Advanced Practice Physiotherapist Connect Health
Dare Michael, Michael Advanced Practice Physiotherapist Connect Health, UK.
Received Date: October 03, 2020; Published Date: October 30, 2020
Abstract
Currently there is an average delay to diagnosis of eight and a half years in axial spondyloarthritis (AxSpA) in the United Kingdom often leading to detrimental consequences for patients. The 2009 ASAS criteria for the diagnosis of Axial Spondyloarthritis support the use of Magnetic resonance imaging of the spine and sacroiliac joints in early diagnosis and are said to enhance diagnostic accuracy [1]. At times in clinic we are presented with patients who have strong features of Inflammatory back pain (IBP) that may have normal inflammatory markers and a normal MRI which pose diagnostic and treatment confusion.
We present a case of a 28-year-old female who presented to the community rheumatology service with a three-year history of inflammatory back pain and widespread arthralgia and fatigue. She was subsequently found to be HLA-B27 negative and her CRP was 1. Initial conventional radiographs of the sacroiliac joints were normal and initial whole spine and sacrolliac MRI showed no romanus lesions in the spine and only subtle right anterior bony oedema which was thought not to be of clinical significance. Initially the BASDAI score was 3.4. The patient continued to have strong symptoms of Axial Spondyloarthritis despite a largely negative imaging and normal CRP. We planned to treat her with Arcoxia, Proton pump inhibitors and yoga/Stretching exercises and repeat the MRI after 6 months .Repeat imaging demonstrated moderate bilateral sacroilliatis with both sacral and illium anterior bony oedema without any romanus lesions in the spine. BASDAI improved to 2.4 with the use of Etoricoxib and regular stretching exercises.
The case suggests that in the right clinical setting with strong features of Axial Spondyloarthritis repeat scanning may be beneficial to diagnosis and treatment which is currently suggested in the NICE guidelines.
Introduction
Dear Editor Axial Spondyloarthritis (AxSpA) has a prevalence of 1 in 200 in the United Kingdon and according to Morgan et al [2] is increasing. The increasing prevalence may be a reflection of improvements in diagnosis. Currently according to all parliamentary national review there is an average delay to diagnosis of eight and a half years for axial spondyloarthritis in the United Kingdom. These statistics when compared to other European Countries are concerning for patients with Axial Spondyloarthritis.
Axial Spondyloarthritis is a subtype of a family of diseases known as Spondyloarthritis (SpA) characterized by inflammation and new bone formation Furst et al [3]. Axial Spondyloarthritis encompasses two spectrums of disease namely Ankylosing Spondylitis which presents with Radiographic evidence of ankylosing of the sacroilliac joints and secondly non radiographic axial spondyloarthritis which shows no conventional radiographic evidence of ankylosing but demonstrates inflammatory changes on Magnetic Resonance Imaging. There is much debate currently if the non-radiographic cohort are a pre-radiographic stage, but more evidence Is emerging for a true non-radiograhic AxSpA whom may never develop conventional radiographic changes.
According to Slobodin et al [4], whom retrospectively reviewed a cohort of 151 patients diagnosed with axial spondyloarthritis found the contributing factors in delay to diagnosis to be multifactorial. Male cohorts generally presented with more inflammatory back pain while female patients generally presented with widespread pain and enthesopathy which interestingly often doubled delay to diagnosis. Similar findings were cited by Lapane et al 2020 who suggest delay to diagnosis was multifactorial often complicated by the slow progression of AxSpA and normal radiographs of the spine and sacroilliac joints. The emergence and acceptance of a true non radiographic cohort of axial spondyloarthritis patients who may never develop MRI or Radiograph changes further complicates diagnosis and management Ortega et al [5]
We present a case of a female previously thought to have widespread pain syndrome with normal radiographs later found to have axial spondyloarthritis. This case supports the concepts summarized above in the literature that delays to diagnosis are complex and multifactorial and often female cohorts face longer delays due to widespread pain presentations.
Case Report
A 28-year-old female was referred to a Rheumatology service with a diagnosis of chronic widespread pain, arthralgia and fatigue for three years in duration. There was no peripheral arthritis, inflammatory back pain and generalized early morning stiffness for 60 minutes. There was no personal or family history of psoriasis, inflammatory bowel disease, enthesitis or dactylitis. There was also no family history of spondyloarthritis.
On clinical examination there was no peripheral arthritis, modified Schobers was 7cm, Leeds Enthesitis score was 0/6, initial BASDAI score was 3.4. Initial investigations demonstrated a normal full blood count, CRP within normal limits and the patient was found to be HLA-B27 negative. Initial plain radiographs Figure 1. Demonstrated normal sacroiliac joints. The patient was prescribed Etoricoxib for three-month duration and reported a significant improvement in her symptoms and her BASDAI reduced to 2.4 (Figure 1).
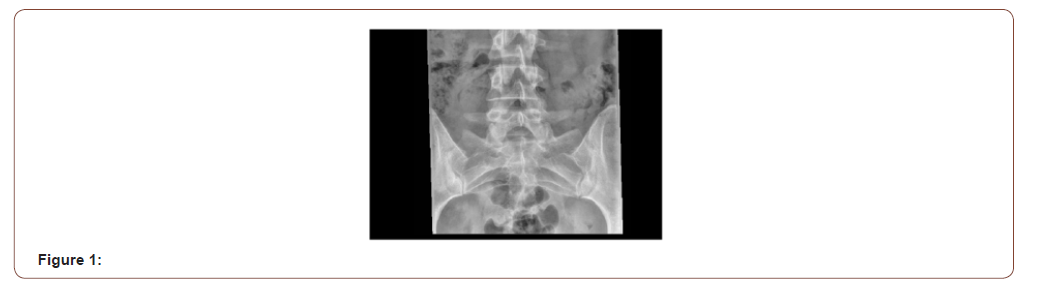
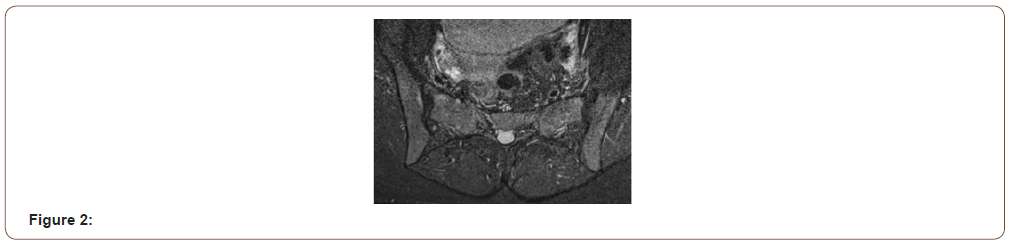
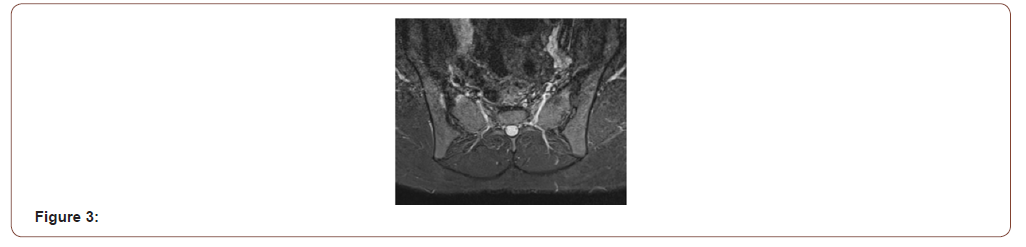
The patients initial Magnetic Resonance Imaging (MRI) in Figure 2 of the whole spine and sacroiliac joints including fat supressed sequences demonstrated minimal right anterior sacroiliac joint bony oedema while the left sacroiliac joint was normal. After a Multidisciplinary discussion it was suggested the imaging be repeat after a six-month duration. The repeat images Figure 3 demonstrated right anterior iliac and sacral bony oedema as well as left anterior sacral oedema both on two consecutive slices highly suggestive of active sacroilliatis and the case meets the ASAS criteria for a diagnosis of axial spondyloarthritis (Figure 2,3).
This case illustrates the many challenges clinicians face in the assessment, work-up and diagnosis of axial spondyloarthritis. Of note, in this case difficulties in diagnosis are complicated by widespread presentations often found in female patients and those with normal inflammatory makers and conventional radiographs. Currently NICE guidelines suggest that if a diagnosis of Axial Spondyloarthritis cannot be made, follow up imaging could be considered if clinical suspicion is high, this case supports that notion [6].
Main message points: The diagnosis of axial spondyloarthritis is often complex and factors such as female sex, normal blood tests and conventional radiographs should not discourage further clinical investigation in the correct clinical setting.
Acknowledgement
None.
Conflicts of Interest
No conflicts of interest.
References
- Khmelinskii, N, Regel A, Baraliakos, X (2018) The Role of Imaging in Diagnosing Axial Spondyloarthritis. Frontiers in medicine 5: 106.
- Morgan C, White A, Tomlinson M, Scott A, Tian H (2020) O16 Incidence, prevalence and associated comorbidity of axSpA within the UK: a retrospective database analysis. Rheumatology, 59(Supplement_2).
- Furst D, Louie J (2019) Targeting inflammatory pathways in axial spondyloarthritis. Arthritis Research & Therapy 21(1): 135.
- Slobodin G, Reyhan I, Avshovich N, Balbir-Gurman A, Boulman N, et al. (2011) Recently diagnosed axial spondyloarthritis: gender differences and factors related to delay in diagnosis. Clinical Rheumatology 30(8): 1075-1080.
- Lapane K, Khan S, Shridharmurthy D, Beccia A, Dube C, et al. (2020) Primary care physician perspectives on barriers to diagnosing axial Spondyloarthritis: a qualitative study. BMC Family Practice 21(1): 204.
- Michelena X, Lopez-Medina C, Marzo-Ortega H (2020) Non-radiographic versus radiographic axSpA: what’s in a name?. Rheumatology 59(Supplement_4): 18-24.
-
Nandagudi, Szabo-Kocsis, Dare Michael. Should We Repeat Imaging If Clinical Suspicion is High in Axial Spondyloarthritis, A Case Report. Glob J Ortho Res. 2(5): 2020. GJOR.MS.ID.000548.
-
ASAS criteria, Axial Spondyloarthritis, Spondyloarthritis, Rheumatology, Bilateral sacroilliatis, Yoga, Stretching, Illium anterior bony, Radiographic
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






