Research Article
Research Article
Impact of the Covid-19 Pandemic on the Prevalence of Wheeze In Children in Hong Kong
Jacqueline Hung1*, Ka Ka Siu2, Shuk Kuen Chau3 and So Lun Lee4
1 Duchess of Kent Children’s Hospital, Hong Kong Special Administrative Region
2 University of Hong Kong, Hong Kong Special Administrative Region
3 Duchess of Kent Children’s Hospital, Hong Kong Special Administrative Region
4 Queen Mary Hospital, Hong Kong Special Administrative Region
Jacqueline Hung, Department of Paediatrics and Adolescent Medicine, Queen Mary Hospital Room 115, 1/F, New Clinical Building, 102 Pokfulam Road, Hong Kong.
Received Date:October 23, 2024; Published Date:May 12, 2025
Abstract
Background
During the COVID-19 pandemic, children in Hong Kong experienced a zero-COVID policy, prolonged school closure and a mandatory maskwearing
requirement. They had significantly less exposure to microbes and represented a more naïve immune system. We explored the prevalence
of wheeze in previously healthy children in Hong Kong during the pandemic. We postulated that the reduced viral load of other respiratory viruses
during this time would affect their immune response and predispose them to allergic diseases, such as asthma.
Methods
Children admitted for the first episode of wheeze from January 2017 to December 2022 were included. They were divided into pre-COVID and
during COVID, spanning from January 2017 to December 2019 and January 2020 to December 2022 respectively. Patients older than 18 years old,
with a history of asthma or a known anatomic abnormality causing chronic bronchial obstruction were excluded. Patient demographics including
age on admission, respiratory virus identified, duration of hospital stay, the need for oxygen, respiratory support and intensive care unit [ICU]
admission were collected.
Results
During the pandemic, there was a 38.4% decrease in hospitalization for wheeze, with 190 admissions pre-COVID compared to 117 admissions
during COVID. The children requiring admission during COVID were younger, with mean age of 3.0 ± 2.5 years compared to 4.0 ± 2.9 years pre-COVID
[p = 0.002]. They also had more severe disease, with a higher prevalence of children requiring oxygen [p = 0.025] and ICU admission [p = 0.001].
Conclusion
We explored the prevalence of wheeze in healthy children during COVID and found that hospitalisation was decreased compared to pre-COVID.
Those hospitalised during COVID had more severe disease. We postulate that this paediatric population could represent a specific “post-COVID”
phenotype. Longitudinal studies focusing on the prevalence of asthma in this cohort is needed.
Keywords:Wheeze; Asthma; COVID-19
Abbreviations:COVID-19: coronavirus disease 2019
WHO: World Health Organisation
ACE2: angiotensin-converting enzyme 2
ICU: intensive care unit
HHHFNC: heated humidified high-flow nasal cannula
NIV: non-invasive ventilation
Introduction
In December 2019, China reported the first case of COVID-19. By spring of 2020, World Health Organisation [WHO] had declared COVID-19 a global pandemic with more than 100 countries affected. After three years with over 770 million reported cases worldwide, the WHO declared an official end to the pandemic in May 2023. During this time, many countries implemented drastic infection control measures as an attempt to reduce disease transmission, morbidity, and mortality. These included wearing surgical masks, hand hygiene, school lockdowns and restriction on social gatherings.
Studies showed that children, who make up approximately 0.1% of all COVID-19 mortality [1], were less symptomatic and had lower risk of severe disease during COVID-19 infection [2]. While there was initial concern that COVID-19 would trigger asthma exacerbations [3], available data so far have suggested otherwise [4,5]. In the United States, there was a 76% decrease in asthmarelated emergency department utilization in children compared to pre-COVID era [6]. Similarly, a retrospective study in Hong Kong showed a third reduction in paediatric asthma hospitalizations [7]. This could be attributed to reduced exposure to outdoor aeroallergens, reduced air pollution and reduced infection of other respiratory viruses [3]. Moscovich et al reported a 17% decrease in respiratory admissions during the pandemic, which was related to a decrease in the detection of respiratory syncytial virus and influenza [8]. Asthma appears to play a protective role in COVID-19 infection in atopic children, as the angiotensin-converting enzyme 2 (ACE2) receptor required for coronavirus attachment to the nasal epithelium and the lungs is under-expressed in this population [9].
While infection control policies remained stringent to protect children from COVID-19 infection, there was a costly detriment to their emotional and mental wellbeing. Children lost access to faceto- face education, faced more domestic violence [10], and social interactions were reduced to the bare minimum. This resulted in higher stress levels and increased depressive and anxiety symptoms [11]. There were also physical health issues, such as reduced physical activity leading to an increase in obese children [12]. If the hygiene hypothesis were to be true, the reduced viral load of other respiratory viruses during the pandemic would affect the immune response in children, shifting them towards a T helper 2 (Th2) phenotype and predisposing them to allergic diseases such as asthma [13].
This is particularly relevant to our locality in Hong Kong, where there was nearly 450 days of school closure, a zero-COVID policy and a mandatory mask-wearing requirement of nearly three years from July 2020 to March 2023. The local paediatric population experienced a much longer period of social distancing compared to western countries. With school resumption, lifting of travel restrictions and seasonal weather changes, the prevalence of respiratory viruses was expected to increase. While studies have focused on the impact of COVID-19 on asthma control in preschool wheezers or children with known asthma [5–7,14], we hope to explore on how the COVID-19 pandemic has affected the prevalence and severity of wheeze in previously healthy children in Hong Kong.
Materials and methods
Participants
This was a single centre retrospective observational study. All children admitted to the Department of Paediatric and Adolescent Medicine at Queen Mary Hospital from January 2017 to December 2022 with physician-diagnosed wheeze were recruited. They were identified from the Clinical Data Analysis and Reporting System (CDARS) using the keywords “wheeze”, “wheezing”, “dyspnoea”, “asthma”, “acute bronchitis” and “acute bronchiolitis”. Only those admitted for the first episode of wheeze were included. Patients older than 18 years old or with a history of wheeze or asthma or a known anatomic abnormality causing chronic bronchial obstruction were excluded.
Study design
Patient demographics were obtained from the Hospital Authority clinical management system, a computerized database that captures all clinical information. Demographics including sex, age during hospitalization, primary diagnosis, respiratory virus identified, use of oxygen or respiratory support, need for admission into intensive care unit (ICU) and duration of hospitalization, were collected.
Children were diagnosed with bronchiolitis or bronchitis based on history and physical examination. Children below 2 years of age with a history of viral prodrome followed by increased respiratory effort, supported with physical findings of tachypnoea, intercostal and/or subcostal retractions, wheeze and crepitations, were diagnosed to have bronchiolitis [15]. Children 2 years of age or above with a history of increased respiratory effort or wheeze, which may be preceded by upper respiratory tract symptoms, and confirmed to have wheeze on physical examination were diagnosed with bronchitis. Respiratory viruses were detected by polymerase chain reaction (PCR) from nasopharyngeal swab or aspirate. Respiratory support was defined as the use of any respiratory support, including heated high-flow nasal cannula (HHHFNC), noninvasive ventilation (NIV) and invasive ventilation. Children were divided into pre-COVID group and during COVID group, of which 36 months of data was collected for each. Pre-COVID data was collected from January 2017 to December 2019, and during COVID data was collected from January 2020 to December 2022.
Statistical analysis
SPSS version 27 was used for data analysis. Descriptive statistics were calculated for subject demographics. Continuous data were reported as mean (SD)or median (IQR) as appropriate. Categorical data was reported as frequency (%). Categorical data between the two groups was compared using the chi-square test. Statistical significance was achieved when p-value ≤ 0.05.
Results
Subject demographics
We identified 862 admissions pre-COVID and 423 admissions during COVID (figure 1). Of these, 672 and 306 admissions respectively were excluded as the patient had a previous history of wheeze, had a known anatomic abnormality causing chronic bronchial obstruction or the admission was not related to wheeze. As a result, a total of 307 children were included in this study (table 1). During COVID, there was a 38.4% decrease in hospital admissions for first episode of wheeze, with 190 admissions pre-COVID compared to 117 admissions during COVID. Children requiring hospitalisation during COVID were predominantly male (p = 0.017) and younger, with mean age of 3.0 ± 2.5 years on admission compared to 4.0 ± 2.9 years pre-COVID (p = 0.002).
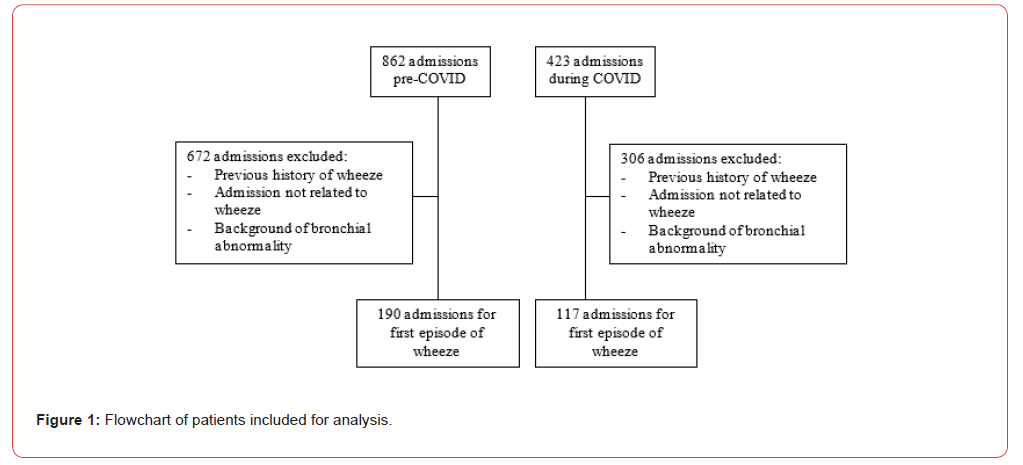
Table 1: Demographics of patients hospitalised for first episode of wheeze pre-COVID and during COVID
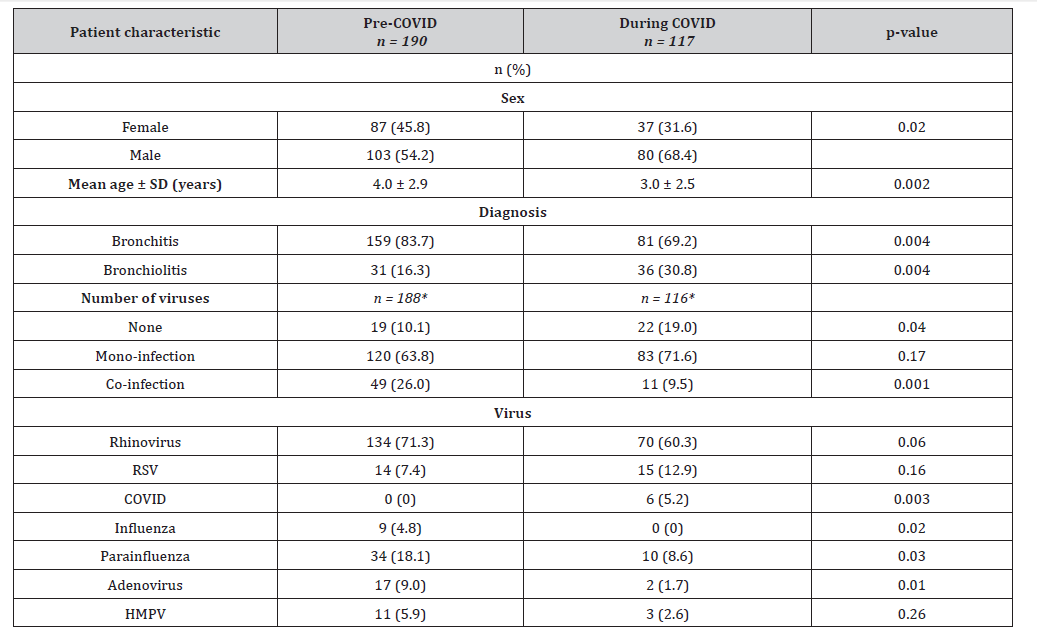
*Nasopharyngeal swab was not performed for two children and one child pre-COVID and during COVID respectively.
Primary diagnosis and virus identified
Bronchitis was the primary diagnosis in more than 50% of hospital admissions in both groups (83.7% pre-COVID and 69.2% during COVID, p = 0.004). Nonetheless, there was a higher proportion of bronchiolitis requiring hospitalisation during COVID (p = 0.004).
Two children in the pre-COVID group (n = 188) and 1 child in the during COVID group (n = 116) did not have nasopharyngeal swab (NPS) performed. Co-infection of respiratory viruses was less frequently seen during COVID, with 11 (9.5%) children having co-infections during COVID compared to 49 (26%) children pre- COVID (p = 0.001). In both groups, rhinovirus was the leading cause of wheeze, making up 71.3% of admissions pre-COVID and 60.3% of admissions during COVID (p = 0.059). COVID was identified in 6 (5.2%) children during COVID (p = 0.003). During COVID, the prevalence of parainfluenza virus (p = 0.028), adenovirus (p = 0.013) and influenza virus (p = 0.015) resulting in wheeze and hospitalisation were significantly reduced.
Seasonal variation
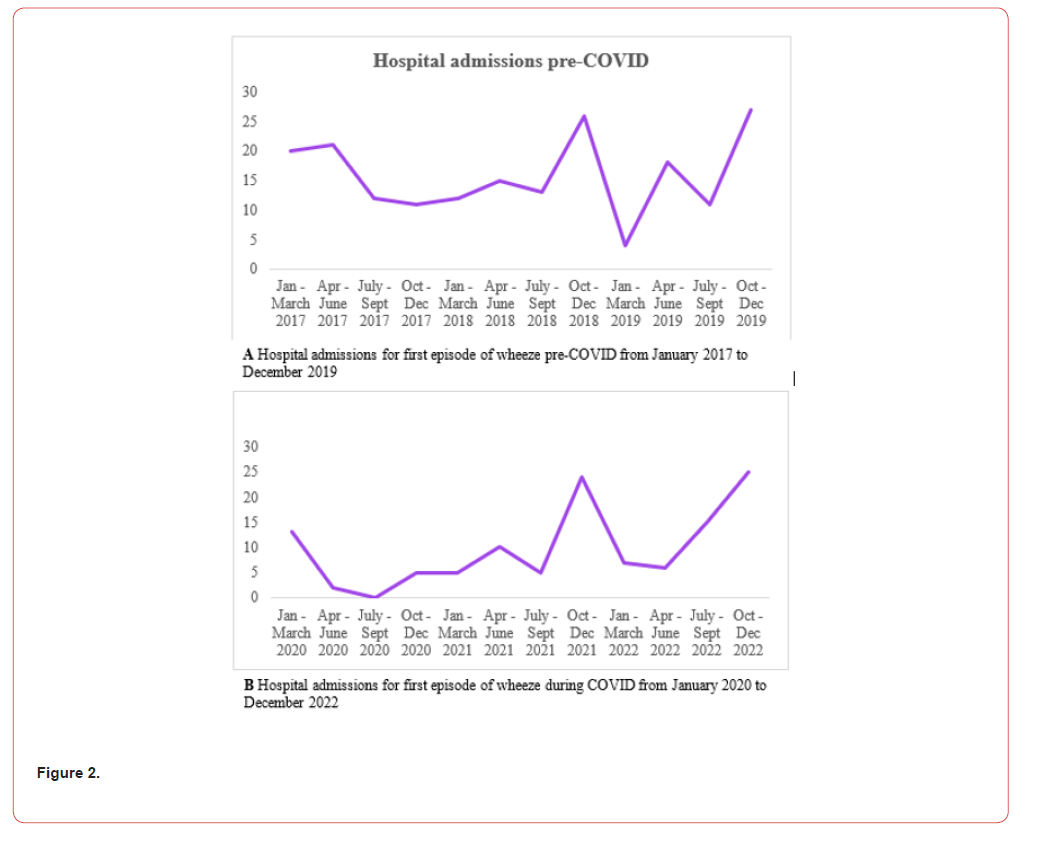
During COVID from January 2020 to September 2021, there was an extended period of city-wide school closure, during which we observed a reduction in hospital admissions compared to pre- COVID from 2017 to 2018 (figure 2). Following the resumption of in-person teaching in September 2021, hospitalisations increased from October to December 2021 and was comparable to pre-COVID. There was another decrease in hospital admissions from April to June 2022, which corresponded to the re-implementation of social restrictions, such as prohibition of group gatherings and temporary suspension of dining services. Following the relaxation of social restrictions in July 2022, there was a sharp rise in hospitalisations that matched pre-COVID times.
Disease severity
During COVID, there was a higher prevalence of children requiring oxygen while hospitalised compared to pre-COVID (table 2), with 41 (35%) children and 44 (23.2%) children requiring oxygen respectively (p = 0.025). There was also a higher prevalence of ICU admissions during COVID, with 7 (6%) patients requiring ICU admission, whereas none of the patients from pre-COVID group required ICU admission (p = 0.001). All patients admitted to ICU required respiratory support. Of these, 6 (85.7%) children required heated HHHFNC and 1 (14.3%) child required NIV. None required invasive ventilation. There was no difference in duration of hospitalisation among the two groups, although this was not statistically significant (p = 0.120).
Table 2: Disease severity of patients hospitalised for first episode of wheeze pre-COVID and during COVID
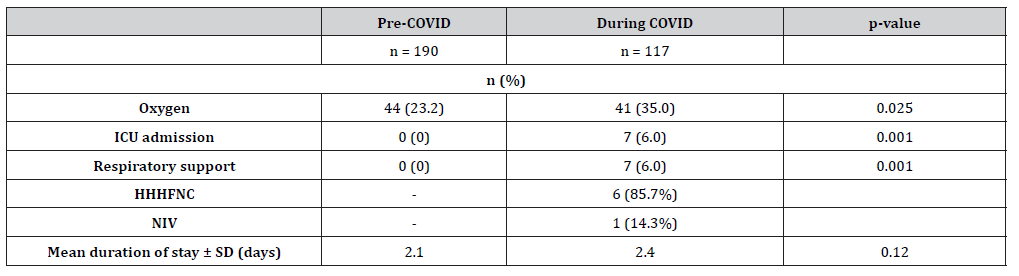
ICU = intensive care unit
HHHFNC = heated humidified high-flow nasal cannula
NIV = non-invasive ventilation.
Discussion
Our study showed a 38.4% reduction in hospital admissions for first episode of wheeze in children during COVID, which was consistent with reports of reduced emergency visits [6] and asthma hospitalisations in the paediatric population [5,7,16]. This was particularly evident from January 2020 to September 2021, when social restrictions and school lockdown were implemented in Hong Kong, and was likely the result of reduced load of respiratory viruses secondary to the use of non-pharmaceutical interventions [7,17], such as hand hygiene and mask wearing. The increase in hospitalisations from October to December 2021 and from July 2022 onwards coincided with the time that social restrictions were eased, which was similar to that observed in the western population [18].
Whilst there was a decrease in prevalence in most respiratory viruses during COVID, rhinovirus remained the leading viral cause of wheeze. Similar findings were reported in Japan, Finland and the United Kingdom [16,18,19] and could be explained by its non-enveloped nature that makes it resistant to alcohol hand rub. Our finding of no influenza-induced wheeze during COVID was in keeping with the observation from Leung et al that surgical face masks significantly reduced detection of influenza virus RNA in respiratory droplets [20].
Interestingly, there was a higher prevalence of bronchiolitis requiring hospitalisation during COVID, making up 36 (30.8%) admissions during COVID compared to 31 (16.3%) admissions pre- COVID. The children hospitalised during COVID were also younger. While this could have been partly due to the higher prevalence of RSV infection during COVID, parallel to that observed in a 3-year Chinese study [21], we postulated that it was also the result of an altered immune response. With bronchiolitis affecting children under the age of 2, these young children grew up during the COVID-19 pandemic, a time where various social restrictions were implemented. If the hygiene hypothesis were true, they would have had substantially less exposure to microbes and aeroallergens, causing their immune response to shift towards a T-helper 2 cell phenotype and resulting in an exaggerated response to viral infections [13]. Our observation that the children hospitalised during COVID had more severe disease compared to pre-COVID, as evidenced by the increased rate of ICU admission and the increased number of children requiring respiratory support, also supported this hypothesis.
An explanation for the reduction in hospital admissions and more severe clinical disease that we observed during COVID was that many parents had hospital phobia due to concerns of nosocomial COVID infection [22] and sought medical attention later than usual and when the child was more severely ill. Despite this, they likely had a lower threshold to seek medical attention for younger children, explaining for the higher prevalence of bronchiolitis during COVID.
A strength of our study is that it is the first to evaluate how the COVID-19 pandemic has affected the prevalence of wheeze in previously healthy children, unlike other paediatric studies that have focused on its impact on asthma control [4,6,7,14]. Additionally, our local paediatric population is unique in that the children had significantly reduced social interaction compared to western countries due to extensive periods of school closure and constant mask-wearing, therefore representing a much more naïve immune system than usual. The COVID effect on the development of wheeze in healthy children, if any, would be amplified in this cohort.
We also have to address our limitations. Being a single-centre study, our data is not representative of the entire paediatric population in Hong Kong. By looking at hospitalised children only, we overlook milder cases of wheeze that were managed at the outpatient clinic or primary healthcare setting. However, 71% of hospitalisations in 2021 pertained to hospitals under the Hospital Authority (HA) [23], which meant that we were able to capture the majority of children requiring hospitalisation in our area. While we are the first to evaluate how the COVID-19 pandemic has affected the development of wheeze in children, whether this translates to an increased prevalence of childhood asthma remains to be seen. Longitudinal studies focusing on the prevalence of physiciandiagnosed asthma and subsequent asthma control in this cohort is needed.
Conclusion
In this study, we found a reduction in hospitalization for wheeze in previously healthy children during the COVID-19 pandemic. Despite various non-pharmaceutical measures, rhinovirus remained the leading viral cause of wheeze. The children requiring admission were younger and had more severe disease, some of whom required ICU admission and respiratory support. It would be of value to study the prevalence of childhood asthma in this paediatric population and to ascertain if they represent a specific “post-COVID” phenotype.
Acknowledgement
Dr Jacqueline Hung conceptualized and designed the study,
collected data, carried out initial analyses, drafted the initial
manuscript and revised the manuscript.
Drs Ka Ka Siu, Shuk Kuen Chau and So Lun Lee critically
reviewed and revised the manuscript.
All authors approved the final manuscript as submitted and
agree to be accountable for all aspects of the work.
We thank Eunice L Y Chan for her assistance in data analysis.
Conflicts of interest
The authors have no conflicts of interest relevant to this article to disclose.
References
- CDC: COVID data tracker [Internet].
- Dong Y, Mo X, Hu Y, Qi X, Jiang F, et al. (2020) Epidemiology of COVID-19 Among Children in China. Pediatrics 145(6): e20200702.
- Abrams E, Sinha I, Fernandes R, Hawcutt D (2020) Pediatric asthma and COVID‐19: The known, the unknown, and the controversial. Pediatric Pulmonology 55(12): 3573-357
- Hazan G, Fox C, Eiden E, Anderson N, Friger M, et al. (2022) Effect of the COVID-19 Lockdown on Asthma Biological Rhythms. J Biol Rhythms 37(2): 152-163.
- Ullmann N, Allegorico A, Bush A, Porcaro F, Negro V, et al. (2021) Effects of the COVID‐19 pandemic and lockdown on symptom control in preschool children with recurrent wheezing. Pediatric Pulmonology 56(7): 1946-1950.
- Kenyon C, Hill D, Henrickson S, Bryant-Stephens T, Zorc J (2020) Initial Effects of the COVID-19 Pandemic on Pediatric Asthma Emergency Department Utilization. The Journal of Allergy and Clinical Immunology 8(8): 2774-2776.e1.
- Wong K, Wong WHS, Yau Y, Lee S, Chiu SSS (2022) Asthma admission among children in Hong Kong during the first year of the COVID-19 pandemic. Pediatr Pulmonol 57(12): 3104-3110.
- Moscovich DP, Averbuch D, Kerem E, Cohen-Cymberknoh M, Berkun Y, et al. (2023) Pediatric respiratory admissions and related viral infections during the COVID-19 pandemic. Pediatric Pulmonology 58(7): 2076-2084.
- Jackson D, Busse W, Kattan M, O’Connor G, Wood R, et al. (2020) Association of Respiratory Allergy, Asthma and Expression of the SARS-CoV-2 Receptor, ACE2. Journal of Allergy and Clinical Immunology 146(1):203-206.e3.
- (2020) Policy Brief: The Impact of COVID-19 on children [Internet].
- Zhao SZ, Wong JYH, Luk TT, Wai AKC, Lam TH, et al. (2020) Mental health crisis under COVID-19 pandemic in Hong Kong, China. International Journal of Infectious Diseases 100: 431-433.
- Daniels NF, Burrin C, Chan T, Fusco F (2022) A Systematic Review of the Impact of the First Year of COVID-19 on Obesity Risk Factors: A Pandemic Fueling a Pandemic? Current Developments in Nutrition 6(4): nzac011.
- Okada H, Kuhn C, Feillet H, Bach JF (2010) The ‘hygiene hypothesis’ for autoimmune and allergic diseases: An update. Clinical and experimental immunology 160(1): 1-9.
- Ruano F, Álvarez M, Haroun-Díaz E, Torrem M, González P, et al. (2020) Impact of the Covid-19 Pandemic in Children with Allergic Asthma. The Journal of Allergy and Clinical Immunology: In Practice 8(9): 3172-3174.e1.
- Subcommittee on Diagnosis and Management of Bronchiolitis (2006) Diagnosis and Management of Bronchiolitis. Pediatrics 118(4): 1774-1793.
- Teo KW, Patel D, Sisodia S, Roland D, Gaillard EA, et al. (2022) Rhinovirus persistence during the COVID-19 pandemic-Impact on pediatric acute wheezing presentations. Journal of Medical Virology 94(11): 5547-5552.
- Chiu S, Cowling B, Peiris JS, Chan E, Wong W, et al. (2022) Effects of Nonpharmaceutical COVID-19 Interventions on Pediatric Hospitalizations for Other Respiratory Virus Infections, Hong Kong. Emerging infectious diseases 28(1): 62-68.
- Kuitunen I, Artama M, Haapanen M, Renko M (2021) Rhinovirus spread in children during the COVID‐19 pandemic despite social restrictions—A nationwide register study in Finland. Journal of Medical Virology 93(10): 6063-6067.
- Takashita E, Kawakami C, Momoki T, Saikusa M, Shimizu K, et al. (2021) Increased risk of rhinovirus infection in children during the coronavirus disease-19 pandemic. Influenza and Other Respiratory Viruses 15(4): 488-494.
- Leung NHL, Chu DKW, Shiu EYC, Chan KH, McDevitt JJ, et al. (2020) Respiratory virus shedding in exhaled breath and efficacy of face masks. Nature Medicine 26(5): 676-680.
- Qiu W, Zheng C, Huang S, Zhang Y, Chen Z (2022) Epidemiological Trend of RSV Infection Before and During COVID-19 Pandemic: A Three-Year Consecutive Study in China. Infection and Drug Resistance 15: 6829-6837.
- WongLaura E, HawkinsJessica E, Langness Simone, Murrell Karen L, Iris Patricia, et al. (2020) Where Are All the Patients? Addressing Covid-19 Fear to Encourage Sick Patients to Seek Emergency Care.
- Health Status of Hong Kong Residents [Internet]. Census and Statistics Department Hong Kong Special Administrative Region.
-
Jacqueline Hung*, Ka Ka Siu, Shuk Kuen Chau and So Lun Lee. Impact of the Covid-19 Pandemic on the Prevalence of Wheeze In Children in Hong Kong. Archives in Respiratory & Pulmonary Medicine. 1(4): 2024. ARPM.MS.ID.000516.
-
COVID-19; Children; Mask-wearing; Microbes; Naïve immune system; Respiratory viruses; Allergic diseases; Asthma; Chronic bronchial obstruction; Oxygen; Intensive care unit (ICU); Wheeze; Dyspnoea; Polymerase chain reaction (PCR)
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.