 Review Article
Review Article
A Rare Case of Cysticercosis Involving the Spinal Canal
Irakli Gakhokidze1,2*, Ketevan Tavadze1, Mirza Khinikadze1,2,3 and Nikoloz Sainishvili3
1Aversi Clinic, Tbilisi, Georgia
2NewVision University, Tbilisi, Georgia
3Caucasus Medical Centre, Tbilisi, Georgia
Irakli Gakhokidze, Radiologist, NewVision University, Tbilisi, Georgia.
Received Date: May 20,2023; Published Date: June 08, 2023
Abstract
A Rare Case of Cysticercosis Involving the Spinal Canal cover: 55-year-old male presented to the radiology department (of his own accord) with a 9-year history of lumbar, spinal pain and a weakness of both lower limbs. He had no bladder or bowel involvement. According to the patient an MRI of the spine with contrast and been performed in 2014. Ependymoma was suggested as a possible cause, however the patient did not seek any treatment. Due to the worsening of the symptoms during the last few months, the patient underwent an MRI imaging of the spine. The MRI study performed in 2022 and the radiologically expressed progression of the disease, specifically the similar changes arising in the cervical segments, put to question the presence of Ependymoma. Patient underwent a surgical resection of the lesion from the lumbar segment for further histological examination. Pathology: A histological examination of a postoperative sample showed the presence of a cyst like structure, containing larvae and consisting of a double layer eosinophilic membrane. The Histomorphology is consistent with cysticercosis. Histopathological images are consistent with tapeworm parasites.
Keywords:Spinal MRI; Spinal neurocysticercosis; Arachnoiditis; Intradural spinal mass lesion
Clinical Information
Age and gender: 55 year old man. Clinical history & presentation: 55-year-old male presented to the radiology department (of his own accord) with a 9-year history of lumbar, spinal pain and a weakness of both lower limbs. He had no bladder or bowel involvement. According to the patient an MRI of the spine with contrast and been performed in 2014. Ependymoma was suggested as a possible cause, however the patient did not seek any treatment. Due to the worsening of the symptoms during the last few months, the patient underwent an MRI imaging of the spine. The MRI study performed in 2022 and the radiologically expressed progression of the disease, specifically the similar changes arising in the cervical segments, put to question the presence of Ependymoma. Patient underwent a surgical resection of the lesion from the lumbar segment for further histological examination (Figure 1 to Figure 7).
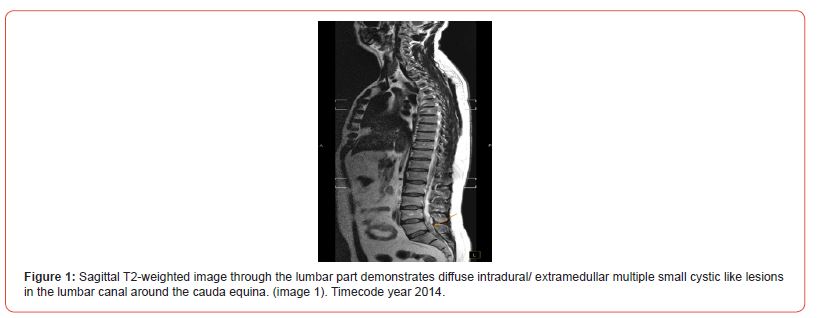
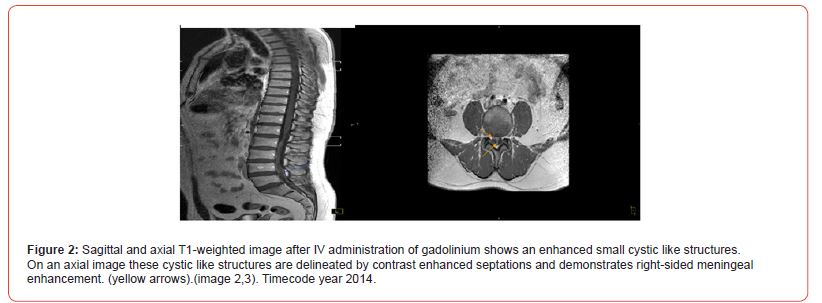
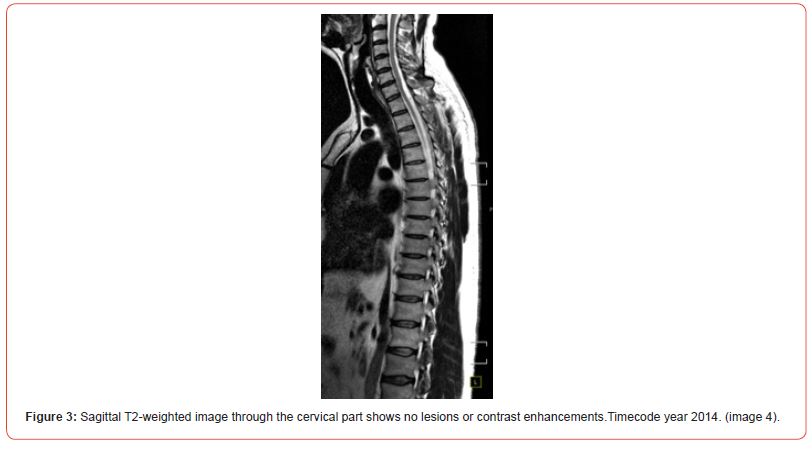
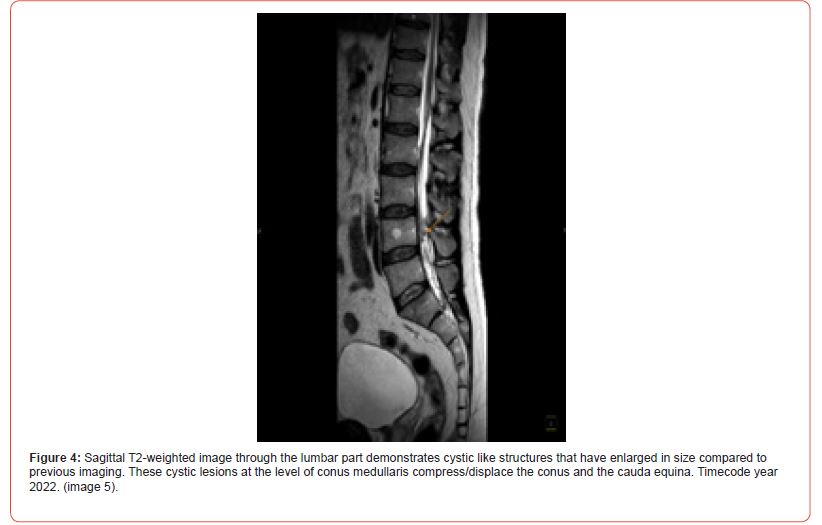

Pathology: A histological examination of a postoperative sample showed the presence of a cyst like structure, containing larvae and consisting of a double layer eosinophilic membrane. The Histomorphology is consistent with cysticercosis. Histopathological images are consistent with tapeworm parasites. Other diagnostic testing: elevated eosinophils (Eosinophilia). Laboratory results were positive for Taenia solium antibodies.
Diagnosis
A. Final diagnosis: Spinal neurocysticercosis.
B. Differential diagnoses: myxopapillary ependymoma: myxopapillary ependymomas are usually more circumscribed and have more homogenous enhancement.
spinal leptomeningeal carcinomatosis: is usually more nodular enhancing foci along the nerve roots of the cauda equina; are not characterized by small cystic like structures. Leptomeningeal carcinomatosis enhancement is more homogenous.
Discussion
Clinical presentation & general epidemiology: Cysticercosis is an infection caused by Cysticercus cellulosae, the larvae of the tapeworm Taenia solium, which infects humans mainly by accidental ingestion of eggs containing infective oncospheres. CNS cysticercosis effects men and women equally. The peak incidence is between the third and fourth decades of life. Intraspinal forms of neurocysticercosis are rare with the incidence varying from 1% to 3%. Isolated spinal cysticercosis, like this case, is extremely rare.
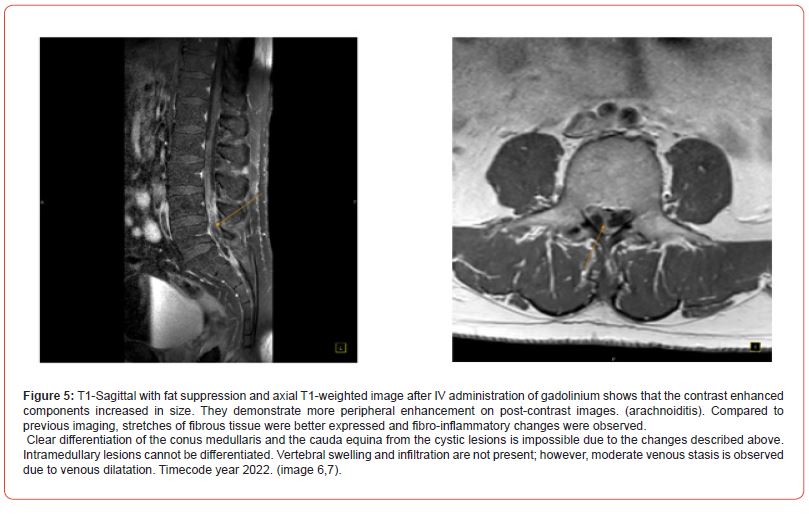
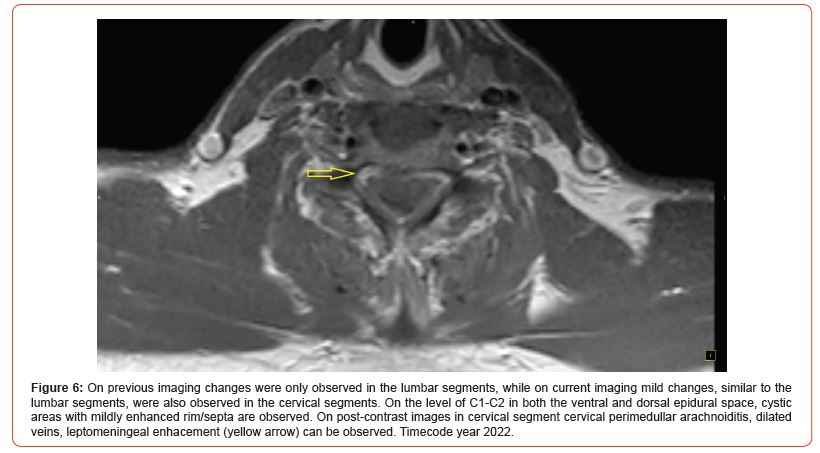
Imaging features: spinal cysticercosis manifests as a nodular or cystic lesion. Within the lesion the scolex of the tapeworm can be observed. The scolex appears as a mural nodule with isointensity on T1 and iso- to hyperintensity on T2. However, the scolex can’t always be visualized in every case. After the administration of contrast medium, the cysticercosis lesions show no enhancement or dot-like enhancement in the scolex, while peripheral ring-like enhancement can be noted in some cases. MRI features include cystic, diffuse arachnoiditis or both. Arachnoiditis is most likely caused by an inflammatory reaction due to the rupture of the cysticercosis cyst into subarachnoid space. Lesions are diffuse with heterogeneous or minor enhancement on post-contrast images.
Prognosis, treatment or therapeutic options: typically, medical treatment is antiparasitic drugs, with dexamethasone to attenuate treatment-associated inflammatory reactions, however, if the extensive lesions shows progressive neurological deficit and no response to medical treatment, then it is managed surgically. Postoperatively patient shows improvement in signs and symptoms with no complications. Postoperative follow up and monitoring response to treatment is essential.
Acknowledgement
None.
Conflict of Interest
No Conflict of interest.
References
- Barrie U, Badejo O, Aoun SG, Adeyemo E, Moler N, et al. (2020) Systematic Review and Meta-Analysis of Management Strategies and Outcomes in Adult Spinal Neurocysticercosis. World Neurosurg 138: 504-511 e8.
- Agale SV, Bhavsar S, Choudhury B, Manohar V (2012) Isolated intramedullary spinal cord cysticercosis. Asian J Neurosurg 7(2): 90–92.
- Kim M, Rhim SC, Khang SK (2014) Intramedullary spinal cysticercosis: a case report and review of literature. Korean J Spine 11(2): 81–84.
- Cantey PT, Coyle CM, Sorvillo FJ, Wilkins PP, Starr MC, et al. (2014) Neglected parasitic infections in the United States: cysticercosis. Am J Trop Med Hyg 90(5): 805-809.
-
Irakli Gakhokidze* and Ketevan Tavadze. A Rare Case of Cysticercosis Involving the Spinal Canal. Arch Neurol & Neurosci. 15(3): 2023. ANN.MS.ID.000864.
-
Decompression Surgery, Neurosurgery, Anesthesiology, Medical Science, Bupivacaine, Pain relief, Lumbar decompression surgery, Neural complications, Nerve tissue.
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






