 Research Article
Research Article
Diagnosis and Surgical Treatment of Orbital Tumors of Various Localizations and Histostructures
OI Lystratenko1*, AM Kardash2, DO Lystratenko3, AV Vashchenko4 and OF Smyrnova5
1Neurosurgeon of Donetsk Clinical Medical Association (DoKTMO), Ukraine
2Head of the Department of Neurosurgery, Donetsk National Medical University (DoNNMU), Ukraine
3Neurosurgeon of Donetsk Clinical Medical Association, Ukraine
4Department of Neurosurgery, Neurosurgeon, Ukraine
5Doctor of Medical Sciences, Ophthalmological clinic, Ukraine
OI Lystratenko, Neurosurgeon of Donetsk Clinical Medical Association (DoKTMO), Donetsk National Medical University, DoKTMO, Donetsk, Ukraine.
Received Date: January 27, 2020; Published Date: February 07, 2020
Abstract
Introduction: The article reviews and analyzes the results of treatment of 32 patients with orbital tumors operated in the clinic, neurosurgery until the period from 2015 till September 2019.
Goals and objectives: coverage of clinical signs and symptoms, histology, diagnostic methods and treatment of patients operated on with orbital tumors during the period 2015-2019. Determination of optimal surgical approach to the tumors with different localization for performing the radical organ-preserving surgery, with maximal saving of visual functions, minimization of oculomotor disorders, patient disability.
Materials and methods: we analyzed the clinical cases of 32 patients undergoing treatment in DOKTMO with orbital tumors for the period from 2015 till September 2019.
Results: Patients were operated on with various approaches - transcutaneous, subconjunctive (without orbitotomy), fronto-orbito-zygomatic, pterional, subfrontal (neurosurgical approaches), transmaxillary, transethmoidal (ENT approaches). The choice of surgical approaches were individual. In 2 cases we become a backset of tumor growth: one patient with aggressive adenocarcinoma, after 18 months, leading to orbital exentration and the child, 9 years old with rhabdomyosarcoma after non-radical removal of tumors of subconjunctival approach. In all other cases, relapses were not detected, operation were organ-preserving oriented.
Conclusion: the results of treatment of patients with tumors directly depend on the choice of radicality tumor removal, which is associated with the choice of surgical approach, chemical, radiation treatment in postoperative period depending on the histological response. From our point of view, the most universal method for tumor removal with various localizations and sizes is fronto-orbito-zygomatic approach which provides the performance of radical organ-preserving operation with maximal vision saving, minimizing oculomotor disorders, disability of the patient, despite its technical complexity for ophthalmologist surgeons. In this regard, surgery of orbital tumors is subject to the competence of doctors of related specialties.
Keywords: Orbital tumor; Ptosis; Fronto-orbito-zygomatic approach; Subconjuctive approach; Rhabdomyosarcoma
Introduction
Tumors of the orbit is a common disease among ophthalmic pathology - up to 4%. As it turned out, their diagnosis is a big problem not only for the ophthalmologist. Due to the anatomical proximity of the orbit to the cranial cavities and paranasal sinuses tumors of the orbit are very diverse, as they can arise from different anatomical structures of the orbit. In this regard not only oculists, but also ENT- doctors, maxillofacial surgeons and neurosurgeons can be involved in the diagnosis establishing and delivery of the surgical care of patients with orbital tumors.
The detection of orbital tumors in the Donetsk region since January 2015 has become much higher due to the use of the following examination algorithm:
examination by an ophthalmologist, ENT specialist, neurologist;
Ultrasound of the eye as a screening study;
CT scan with intravenous contrast, MRI to clarify the abundance of the process.
In the article we examined the results of the treatment of 32 patients operated on by us and performed the analysis of the surgical approaches depending on the localization and the nature of the process. We have proposed a scheme for determining the choice of surgical access, affecting on the radical removal of the tumor while maintaining all eye functions.
Materials and Methods
For the period from 2015 till September 2019, in Donetsk Neurosurgergical Clinic, we operated on 32 patients with tumors of the orbit of various localization and histostructure. Among the patients, 15 men (46.9%) and 17 (53.1%) women aged 2 to 79 years. Among them 7 (21.9%) children - 3 boys and 4 girls.
The main symptoms of orbital tumors are: unilateral ptosis, exophthalm, diplopia, progressive decrease in vision in one eye, eye pain.
All patients were examined according to the algorithm above.
According to histological analysis, we distributed the clinical cases in the table (Table 1):
Table 1:
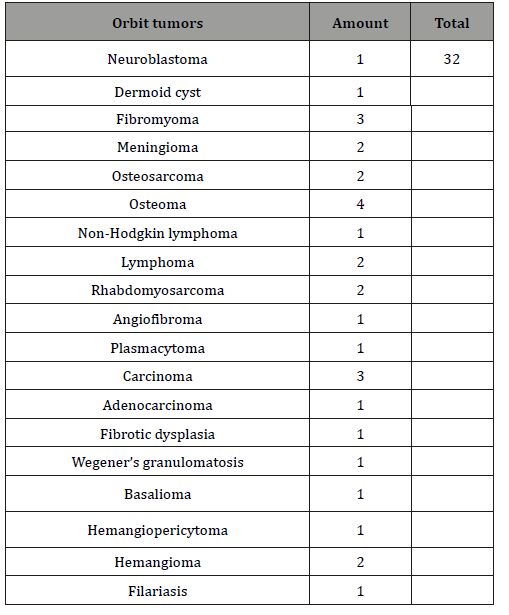
Orbital tumors are various according location:
o associated with the apical part of the orbit;
o not associated with the apical part of the orbit;
o with intracranial growth,
o with growth in the paranasal sinuses.
Depending on the location of the tumor, different surgical approaches should be preferred, which is displayed in a pie chart (Diagram 1):

We pay special attention to the selection of the optimal surgical approach to minimize the damage of the orbit structures during performance of organ-sparing surgery.
The types of surgical approaches we conditionally divided into 3 fundamentally different directions:
I. extracranial approaches:
-lateral orbitotomy,
-transmaxillary orbitotomy,
-transetmoidal and transsphenoidal orbitotomy.
III. approaches without orbitotomy:
-transcutaneous
-transconjuctive.
Transcutaneous tumor removal, without orbitotomy, is the most often used by us when the tumor is located on the lower and lower medial edge of the orbit. The most often these are vascular tumors. We must not forget about filariasis, which can be regarded as a tumor of the orbit.
Clinical case. Woman 64 years old. The disease was taking place about 3 months when a painful swelling appeared on the right lower eyelid. Recurrent course with periodic edema, redness of the lower eyelid. On CT - soft tissue formation along the lower edge of the orbit. Intraoperatively was detected helminth in a fibrous capsule (Figure 1).

Results

Clinical case (Figure 2,3 & 4). Child 10 years old. The diagnosis is cavernous angioma of the lower edge of the left orbit. The main complaint is pain in the left eye during its movement, limitation of the eyeball mobility. There was performed the operation - transcutaneous removal of the tumor. The histological response is cavernous angioma (Figure 2,3 & 4).
Lateral orbitotomy is used in a limited number of cases, more often when the tumor process is in the lateral, upper lateral region of the orbit, it is a minimally invasive orbitotomy. However, it requires fixation of the bone flap with titanium bridges. It is performed by cantotomy.
Clinical case (Figure 5,6). The patient is 57 years old. The diagnosis is plasmacytoma with damage of the frontal bone, upper lateral walls of the orbit. The main complaint is the restriction of the eyeball mobility and pain in the eye. The operation was performed - lateral orbitotomy with resection of the portion of the lateral wall of the orbit and the part of the frontal bone affected by the tumor. After the operation the pain syndrome regressed and the mobility of the eyeball was restored.
The histological response is plasmacytoma. She underwent specific treatment with an oncohematologist (Figure 5,6).
Subconjunctival approach by cantotomy. It is a less traumatic modern approach, without orbitotomy. It is used to remove the orbital tumors of the lower medial and lower lateral location. Not effective for the location of the orbital tumors in the area of the intramuscular funnel, can be used for open biopsy of a diffuse tumor.




Clinical case (Figure 7,8,9). This child is 6 years old. The girl was operated on in one of the ophthalmological clinics of Ukraine for a tumor of the left orbit with subconjunctival access. The histological response is rhabdomyosarcoma (Figure 7. Photo -15 days after operation). Due to lightning-fast relapse, severe pain, exophthalmos, progressive visual impairment, the child was reoperated in the neurosurgery clinic of DoKTMO. In order to radically remove the tumor there was chosen the fronto-orbito-zygomatic approach. (Figure 8. CT scan on the left before operation, on the right - after). After the operation regress of exophthalmos and pain, movements of the eyeball are full. The histological response is rhabdomyosarcoma. The child received a course of chemotherapy (Figure 9. Photo after combined treatment on the 30th day). No metastasis in the internal organs (Figure 7,8,9).


Front-orbit-zygomatic access from our point of view is ideal, universal for removing orbital tumors with various localization: the optic nerve channel, intermuscular funnel, lacrimal gland tumors, lateral, lower lateral orbit regions, large diffuse tumors with intracranial spread.
Clinical case. Patient 62 years old. Diplopia, pain, exophthalmos, visual impairment. Symptoms increased in the indicated sequence within 1 year. Patient was operated on with fronto-orbito-zygomatic approach. In the postoperative period - regression of the described symptoms. The histological response is angiofibroma (Figure 10,11,12 & 13).


Separately, we provide the tactics of managing patients with tumors of the optic nerve. As a rule, these are patients of early childhood. In the treatment of such patients we were guided by literature data, the experience of foreign colleagues and a little of our own experience.
• Conservative treatment may be warranted because only 21% of these patients have tumor progression.
• Surgical treatment only by patients with progressive ptosis, blind eye, severe pain syndrome or when the expansion of the intracranial part of the optic nerve threatens chiasm, there exists fears of tumor expansion into the hypothalamus, 3rd ventricle. Fronto-orbito-zygomatic or pterional approach is used.
• Surgery includes resection of the optic nerve from the eyeball, within 2 mm of the chiasm. A puncture biopsy of the orbital component of the tumor is used to confirm the diagnosis if there occurs a progressive loss of vision or significant tumor growth.
• Radiation therapy with using of linear accelerator (50 Gy) is the treatment of choice for chiasmal gliomas.
• Radiation therapy does not affect the outcome of the disease, even when the tumor involves the hypothalamus and the third ventricle in the process (mortality rate: 28%). You can become serious complications from the central nervous system.
Here are a few clinical cases:
-Clinical case (Figure 14) A child of 3 years. Lightning-fast development of the disease - pain, exophthalmos, vision loss, hypothalamic disorders.



An inoperable tumor of the right optic nerve with involving of the eyeball, chiasm and later the thalamic structures of the brain. A biopsy was not performed due to the severity of the child’s condition — the transience of the process, the addition of hypothalamic disorders — most likely glioblastoma. Chemotherapy. The prognosis for life is not favorable (Figure 14).
Clinical case (Figure 15) A child of 8 months – there exists a glioma of the right optic nerve. The main complaint of parents is exophthalmos. Chemotherapy, positive dynamics. Currently, the child is 2 years 8 months old. Exophthalmos is regressed, vision on the affected eye is preserved. The child is under dynamic MRI supervision (Figure 15).


Conclusion
1. Tumors of the orbit are common diseases. The main symptoms of the orbital tumors are - unilateral ptosis, exophthalmos, diplopia, pain syndrome, progressive visual impairment. With the exclusion of endocrine pathology, a diagnostic algorithm should be performed to identify or exclude the tumors:
o Ultrasound of the eye, as a screening study;
o CT with intravenous contrast, MRI, to clarify the prevalence of the process;
o CT with intravenous contrast, MRI, to clarify the prevalence of the process;
2. The results of the treatment of patients with orbital tumors directly depend on the radicalism of the neoplasm removal, which is associated with the choice of surgical approach, the use of chemo-, radiation therapy in the postoperative period, depending on the histological response. In our opinion, the most universal method for removing orbital tumors of various localization and sizes is fronto-orbito-zygomatic approach which provides the implementation of radical organ-preserving surgery, with the maximum preservation of visual function, minimizing oculomotor disturbances, and patient disability, despite its technical complexity for surgeons ophthalmologists. In this regard, surgery of orbital tumors is a subject to the competence of doctors of related specialties.
Acknowledgement
None.
Conflict of Interest
No conflict of interest.
References
- Shields CL, Shields JA, HonavarSG, Demirci H (2001) Clinical spectrum ofprimary ophthalmic rhabdomyo-sarcoma. Ophthalmology 108: 2284-2292.
- Konovalov AN (2004) Surgery of tumors of the base of the skull. In: AN Konovalov, VA Cherekaev, AV Kozlov, AG Vinokurov (Eds.), p. 371.
- Bouguila H, Malek I, Nacef L, Marrakchi S, Dagfous F, Ayed S (1999) Intraorbital dermoid cyst. Apropos of a case. J Fr Ophtalmol 22: 438-441.
- Cherekaev VA (1995) Surgery of tumors of the base of the skull extending into the orbit and paranasal sinuses: autorefer. diss. honey. Sciences: 31.
- Gloor B, Kalman A (1992) Neoplasticspace-occupying lesions of the orbit.I. Review hemangioma, lymphangiomaand embryonal rhabdomyosarcoma. Klin Monatsbl Augenheilkd 201(5): 291-301.
- Balabanov Ch, Parashkevova B, Murgova S, Iordanov I (2005) Tumors of theeye and adnexa. Bulgarian Review of Ophthalmology 49: 12-20.
- Weisman RA, Kikkawa D, MoeKS, Osguthorpe JD (2001) Orbital tumors. Otolaryngol Clin North Am 34: 1157-1174.
- Krivoshiiska E, Nedkova B, Balabanov Ch, Iordanov I, Karaivanov M, et al. (2006) Langerhans cell histiocytosis - aclinical case. In: Tumors of the eye and the eyes adnexa. Pleven: 147-153.
- Hejazi N, Hassler W, Farghaly F (1999) Transconjunctival microsurgical approach to the orbit: a retrospective preliminary review and analysis of experience with the first 15 operative cases. Neurosurg Quart 9: 197-220.
- Gunalp I, Gunduz K (1995) Pediatric orbital tumors in Turkey. Ophthal Plast Reconstr Surg 11: 193-199.
- Turbin RE, Pokorny K (2004) Diagnosis and treatment of orbital optic nerve sheath meningioma. Cancer Control 11: 334-341.
- De Jesús O, Toledo MM (2001) Surgical management of meningioma en plaque of the sphenoid ridge. Surg Neurol 55: 265-269.
- Konovalov AN (1998) Surgery of the base of the skull. In: AN Konovalov, UB Makhmudov, BA Kadashev (Eds.), Zh Q. neurohir them NN Burdenko, pp. 4.-S. 3-9.
- Savinykh VI (1983) Transcranial access for retrobulbar tumors. In: VI Savinykh, AA Lutsik, VF Barykina (Eds.), Ophthalmol journal 1: 21-23.
- Cherekaev VA (1984) Tumors of the optic nerve, diagnosis and surgical treatment: Dis. Cand honey Sciences, p. 186.
- Bejjani GK (2001) A reappraisal of surgery for orbital tumors. Part 1: extraorbital approaches. In: GK Bejjani, KP Cockerham, JS Kennerdell (Eds.), Neurosurg focus 10(2): E2
- Chang CW (2007) Orbitozygomatic approach for excisions of orbital tumors with 1 piece of craniotomy bone flap: 2 case reports. In: CW Chang, LC Wang (Eds.), Surg neurol 68: 56-59.
- Fahmy P (2003) Metastases in the ophthalmic region in Denmark 1969-1998. A histopathological study. In: P Fahmy, S Heegaard, OA Jensen (Eds.), Acta opthalm scand 81(1): 47-50.
- Housepian EM (1969) Surgical treatment of unilateral optic nerve gliomas. In: EM Housepian (Ed.), J neurosurg 31: 604-607.
- Rohde V (1995) The combined pterional and orbitozygomatic approach to extensive tumors of the lateral and laterobasal orbit and orbital apex. In: V Rohde, K Schaller, W Hassler (Eds.), Acta neurochir 132: 127-130.
- Borisova IA (2002) Surgical treatment of gliomas of the optic nerve growing into the eyeball. In: IA Borisova (Ed.), Thesis. reports of the III Congress of Neurosurgeons of Russia. St. Petersburg, pp. 83-84.
- Zozulya Yu (1979) A Surgical treatment of meningiomas of the wings of the main bone. In: Yu A Zozulya, SA Romodanov (Eds.), Neurosurgery 12: 2633.
- Goldberg SH, Cantore WA (1997) Tumors of the orbit. Curr Opin Ophthalmol 8(5): 51-60.
- Mareeva TG (1974) About radical removal of gliomas of the optic nerve of cranioorbital distribution. In: TG Mareeva VI Rostotskaya, ON Sokolova, Yu N Volynskaya (Eds.), Questions of neurosurgery 2: 3-7.
-
OI Lystratenko, AM Kardash, DO Lystratenko, AV Vashchenko, OF Smyrnova. Diagnosis and Surgical Treatment of Orbital Tumors of Various Localizations and Histostructures. Arch Neurol & Neurosci. 7(1): 2020. ANN.MS.ID.000652.
-
Orbital tumor, Ptosis, Fronto-orbito-zygomatic approach, Subconjuctive approach, Rhabdomyosarcoma.
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






