 Case Report
Case Report
Tracheobronchial Laceration in a Paediatric Patient: A Case Report
Kartulev Nikola*
Paediatric Surgery Department, University Multiprofile Hospital for Active Treatment and Emergency Medicine (UMHATEM) “N.I. Pirogov”, Sofia, Bulgаria
Kartulev Nikola, Paediatric Surgery Department, University Multiprofile Hospital for Active Treatment and Emergency Medicine (UMHATEM) “N.I. Pirogov”, Sofia, Bulgаria
Received Date: February 09, 2026; Published Date: February 17, 2026
Introduction
Tracheobronchial injuries (TBI) are relatively rare yet potentially life-threatening conditions. The incidence of hospitalized patients who have sustained chest trauma accounts for approximately 10– 15% of all trauma patients [2]. Tracheobronchial injuries occur in 1.5–3% of patients with thoracic and cervical trauma [1,3]. According to the mechanism of injury, TBIs can be classified as resulting from penetrating or blunt trauma, as well as iatrogenic or inhalational etiologies [1]. Approximately 76% of tracheobronchial injuries resulting from blunt trauma involve the main bronchi within 1 cm of the carina [7]. The right mainstem bronchus is most frequently affected (27%), followed by the distal trachea (22%), the left mainstem bronchus (17%), the lobar bronchial orifices (16%), and the cervical trachea (4%).
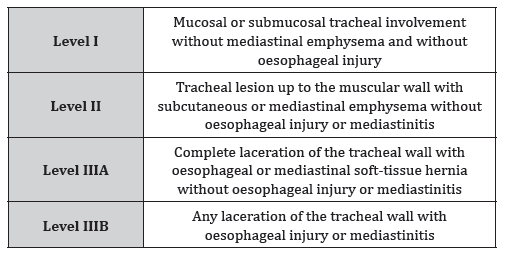
Combined tracheal and bronchial injuries have been reported in approximately 8% of cases [4]. Diagnosis is often challenging due to nonspecific clinical manifestations. Patients may present with a range of nonspecific findings, including subcutaneous emphysema, pneumothorax, pneumomediastinum, hemoptysis, respiratory distress syndrome, and, less commonly, pneumoperitoneum [4- 6]. Bronchoscopy represents the gold standard for the diagnosis and assessment of tracheobronchial injuries. The currently available classification is based on bronchoscopic evaluation of tracheobronchial injuries related to intubation trauma (Table 1) [8]. In the present case, we report a 15-year-old girl patient who sustained polytrauma following a pedestrian road traffic accident, namely thoracic trauma with tracheal and right main bronchial laceration and abdominal trauma with liver contusion.
Table 1: Bronchoscopic classification of tracheobronchial injuries.
Case Presentation
A 15-year-old previously healthy girl with normal development was admitted to the emergency department following a road traffic accident, in which she was struck by a vehicle while crossing the street. She complained of retrosternal chest pain. The patient did not clearly recall the incident and denied vomiting.
On admission, the patient was conscious with a Glasgow Coma Scale score of 15. Physical examination revealed extensive subcutaneous emphysema, palpable from the lower third of the sternum posteriorly to the anterior border of the trapezius muscle and superiorly to the mandible. Mild asymmetry of chest expansion was noted, with slight delay of the right hemithorax during respiration. Bilateral vesicular breath sounds were present, with mildly decreased breath sounds at the right lung base. Oxygen saturation on room air was 90%, improving to 99% with supplemental oxygen delivered via face mask at 4 L/min. Hemodynamic assessment revealed a blood pressure of 90/50 mmHg and a heart rate of 79 beats per minute.
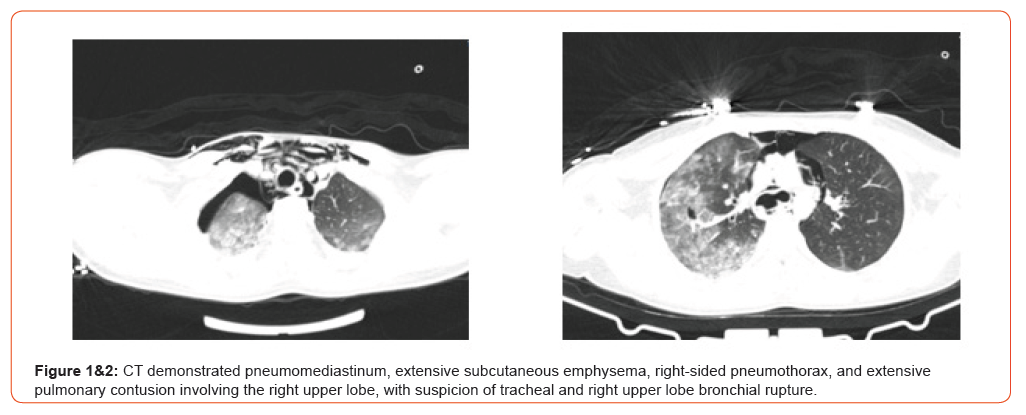
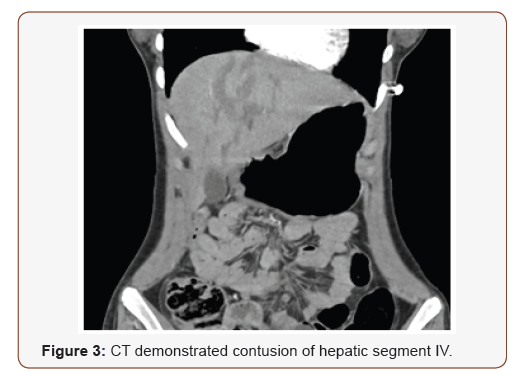
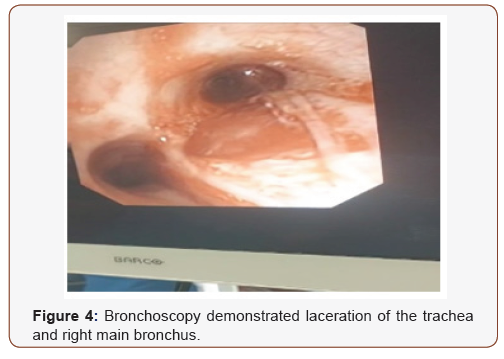
Abdominal examination demonstrated superficial skin excoriations in the right lower quadrant, with soft abdominal wall and spontaneous as well as palpation-induced pain in the epigastric region. Chest radiography revealed a right-sided apical pneumothorax and a fracture of the seventh rib. A whole-body computed tomography demonstrated pneumomediastinum, extensive subcutaneous emphysema, right-sided pneumothorax, and extensive pulmonary contusion involving the right upper lobe, with suspicion of tracheal and right upper lobe bronchial rupture. In addition, findings were consistent with a contusion of hepatic segment IV (Figures 1,2,3). Subsequently, bronchoscopy was performed under endotracheal anaesthesia, revealing a laceration of the membranous portion of the trachea located approximately 1 cm from the carina, extending into the right main bronchus up to 1 cm from the orifice of the right upper lobe bronchus (Figure 4).
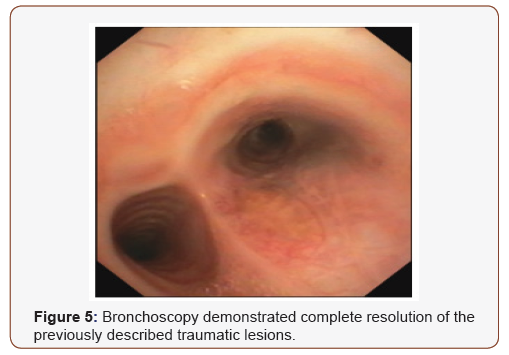
A right-sided chest tube was inserted, and mediastinal drainage was performed via jugulotomy with placement of two mediastinal drains. Given the patient’s stable clinical condition and the location of the injury, a decision was made to proceed with extubating. The early post-interventional period was spent in the paediatric intensive care unit, during which a course of broad-spectrum antibiotics was administered for prevention of mediastinitis. During follow-up, the patient remained hemodynamically stable, with no signs of respiratory distress, progressive resolution of the subcutaneous emphysema, and no evidence of recurrent pneumothorax. Serial abdominal ultrasonography demonstrated a gradual reduction in the extent of hepatic contusion. On postprocedural day 7, follow-up bronchoscopy revealed a reduction in the extent of the previously described tracheal and right main bronchial lesions. On the same day, the left mediastinal drain was removed, and the patient was transferred to the paediatric thoracic surgery ward. On day 8, following a control chest radiograph, the thoracic drain was removed. The right mediastinal drain was removed on day 10. The patient was discharged on day 15 in good clinical condition, with complete resolution of subcutaneous emphysema and no residual symptoms. One month after the injury, follow-up bronchoscopy demonstrated complete resolution of the previously described traumatic lesions (Figure 5).
Discussion
Tracheobronchial injuries are rare conditions, particularly in the paediatric population, with blunt trauma accounting for up to 94% of reported cases [9]. Tracheobronchial ruptures (TBR) most commonly result from high-energy mechanisms of injury. Tracheal damage typically occurs as a consequence of high-energy blunt thoracic trauma against a closed glottis or due to direct impact to the neck during flexion or hyperextension. Injuries most frequently involve the membranous portion of the trachea, as it represents the structurally weakest component of the laryngotracheal complex. In all patients who sustain high-energy trauma to the neck and/ or thorax, the possibility of tracheobronchial injury should be considered [10]. Timely diagnosis plays a pivotal role in guiding subsequent management and overall prognosis. In the setting of high-energy trauma accompanied by clinical signs suggestive of tracheobronchial injury, further diagnostic evaluation is mandatory, with airway stabilization taking priority whenever indicated. Initial chest radiography most commonly reveals findings such as pneumothorax, pneumomediastinum, or subcutaneous emphysema. In clinically stable patients, further evaluation with computed tomography is recommended. Owing to the mechanism of injury in our patient, a contrast-enhanced whole-body CT scan was performed, which raised suspicion for injury to the trachea and right main bronchus and additionally identified an associated hepatic injury.
Flexible bronchoscopy represents the gold standard for the diagnosis of tracheobronchial injuries, as it allows accurate assessment of the exact location, extent, and depth of the lesion. When bronchoscopy is performed in intubated patients, the endotracheal tube should be gradually withdrawn to the level of the vocal cords to enable proper visualization and precise evaluation of the level of injury, as well as to exclude the presence of additional lesions. If necessary, the endotracheal tube may subsequently be repositioned under direct visual control distal to the level of the injury [1,7,11,12]. The bronchoscopic classification presented in Table 1 provides a framework for selecting patients suitable for conservative management. Patients with Level I and Level II injuries who are clinically stable, breathing spontaneously or requiring minimal ventilatory support, with lesions measuring less than 2 cm, no associated esophageal injury, and non-progressive subcutaneous emphysema or pneumomediastinum, are suitable for non- operative management.
However, despite an initial preference for conservative management, it is essential to promptly recognize surgical complications indicating the need for operative intervention, including worsening subcutaneous emphysema, progressive pneumomediastinum, pneumothorax with persistent air leak, or pneumothorax with failure of lung re-expansion despite adequate chest tube placement [12]. Non-operative treatment approaches reported in the literature include airway stenting, application of fibrin glue, administration of corticosteroids, and prophylactic antibiotic therapy. In the present case, a history of road traffic trauma, extensive subcutaneous emphysema, and careful physical examination were crucial in guiding subsequent clinical decisionmaking. The case highlights the importance of timely diagnosis, underscoring the role of computed tomography and bronchoscopy. Placement of thoracic and mediastinal drains provided effective decompression, allowing spontaneous healing of the lesion under conservative management. In addition, the absence of significant comorbidities played a crucial role in the patient’s favourable clinical course and overall prognosis.
Conclusion
Tracheobronchial injuries are relatively rare but potentially lifethreatening conditions. Timely diagnosis, along with the presence or absence of associated comorbidities, is of critical importance for the final treatment outcome. Conservative management options should not be underestimated; however, each patient must be evaluated individually, and the decision for non-operative treatment should be guided by the patient’s clinical presentation.
Acknowledgement
None.
Conflict of Interest
No conflict of Interest.
References
- Antonescu I, Mani VR, Agarwal S (2022) Traumati injuries to the trachea and bronchi: a narrative review. Mediastinum 6: 22.
- Abubeker EY, SY Mustofa, Amare H/kiros Gebregzi, Habtu AA (2021) Mortality rate and factors associated with death in traumatic chest injury patients: A retrospective study. I J Surg Open 37: 100420.
- Goh SH, Tan SM, Chui P, Low BY (1995) Traumatic bronchial rupture--a case report. Ann Acad Med Singap 24(6): 883-886.
- Verkoulen KCHA, van Roozendaal LM, Daemen JHT, Franssen AJPM, Meesters B, et al. (2023) Management of tracheobronchial ruptures in blunt chest trauma: pushing the boundaries towards a minimally invasive surgical approach. AME Case Rep 7: 21.
- Grewal HS, Dangayach NS, Ahmad U, Ghosh S, Gildea T, et al. (2019) Treatment of Tracheobronchial Injuries: A Contemporary Review. Chest 155 (3): 595-604.
- Hong SB, Lee JY, Lee J, Choi KB, Suh JH (2018) Right Main Bronchus Rupture Presenting with Pneumoperitoneum. Korean J Thorac Cardiovasc Surg 51(3): 216-219.
- Welter S, Essaleh W (2020) Management of tracheobronchial injuries. J Thorac Dis 12(10): 6143-6151.
- Giuseppe C, Luigi C, Francesco C, Sandro B, Raffaelle DJ, et al. (2010) Tracheal lacerations after endotracheal intubation: a proposed morphological classification to guide non-surgical treatment. Eur J Cardio Thorac Surg 37(3): 581-587.
- Loroch A, Curran JF, Wynne DM (2021) Paediatric Longitudinal Tracheal Laceration From Blunt Force Trauma: A Case Report. Cureus 13(11): e19867.
- Kuhne CA, Kaiser GM, Flohe S, Beiderlinden M, Kuehl H, et al. (2005) Nonoperative management of tracheobronchial injuries in severely injured patients. Surg Today 35(7): 518-523.
- Altinok T, Can A (2014) Management of tracheobronchial injuries. Eurasian J Med 46(3): 209-215.
- Grewal HS, Dangayach NS, Ahmad U, Ghosh S, Gildea T, et al. (2019) Treatment of Tracheobronchial Injuries: A Contemporary Review. Chest 155(3): 595-604.
-
Kartulev Nikola*. Tracheobronchial Laceration in a Paediatric Patient: A Case Report. 5(1): 2026. ACCS.MS.ID.000601.
-
Tracheobronchial laceration; trauma; pneumoperitoneum; chest radiography; anesthesia; iris publishers; iris publisher’s group
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






